Baker cyst
Overview
A Baker cyst is a fluid-filled growth behind the knee. It causes a bulge and a feeling of tightness. Also called a popliteal (pop-luh-TEE-ul) cyst, a Baker cyst sometime causes pain. The pain can get worse when with activity or when fully straightening or bending the knee.
A Baker cyst is usually the result of a problem with the knee joint, such as arthritis or a cartilage tear. Both conditions can cause the knee to produce too much fluid.
Although a Baker cyst may cause swelling and discomfort, treating the underlying problem that is causing it usually provides relief.
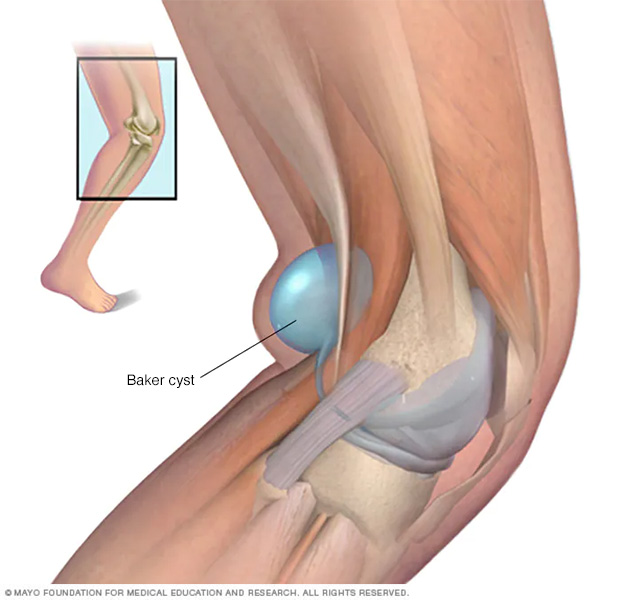
Swelling on the back of one knee may be a Baker cyst. This can form when joint-lubricating fluid fills a cushioning pouch (bursa) at the back of the knee.
Symptoms
In some cases, a Baker cyst causes no pain, and you may not notice it. If you do have symptoms, they might include:
- Swelling behind the knee, and sometimes in the leg
- Knee pain
- Stiffness and inability to fully flex the knee
The symptoms may be worse after you've been active or if you've been standing for a long time.
When to see a doctor
Seek medical attention if you have pain and swelling behind your knee. Though unlikely, these symptoms may be a sign of a blood clot in a leg vein.
Causes
A lubricating fluid called synovial (sih-NO-vee-ul) fluid helps the leg swing smoothly and reduces friction between the moving parts of the knee.
But sometimes underlying conditions can cause the knee to produce too much synovial fluid. When this happens, fluid can build up in the back of the knee, leading to a Baker cyst.
This can be caused by:
- Inflammation of the knee joint, which can occur with various types of arthritis
- A knee injury, such as a cartilage tear
Complications
Rarely, a Baker cyst bursts and synovial fluid leaks into the calf region, causing:
- Sharp pain in the knee
- Swelling in the calf
- Sometimes, redness of the calf or a feeling of water running down the calf
Diagnosis
A Baker cyst can often be diagnosed during a physical exam. However, some of the symptoms of a Baker cyst are similar to the symptoms of more-serious conditions, such as a blood clot, aneurysm or tumor. To get more information, your health care provider may order imaging tests, including:
- Ultrasound
- X-ray
- Magnetic resonance imaging (MRI)
Treatment
Sometimes a Baker cyst will disappear on its own. Mild symptoms can often be controlled by avoiding activities that trigger them.
However, if the cyst is large and causes pain, you may need treatment.
Medications
A nonprescription pain reliever, such as acetaminophen (Tylenol, others) or ibuprofen (Advil, Motrin IB, others) can reduce pain and inflammation.
An injection of steroid medication, such as cortisone, into the knee can reduce inflammation. This may reduce the size of the cyst and relieve pain, but it doesn't always stop the cyst from coming back.
Therapies
Gentle exercises that improve range of motion and strengthen the muscles around the knee may help it feel better and preserve knee function.
Surgery or other procedures
To reduce the size of the cyst, your care provider may drain the fluid from the cyst using a needle. This is called needle aspiration and is often performed with ultrasound guidance.
If a joint problem is causing the cyst, arthroscopic surgery may be performed to repair the problem. For example, if a cartilage tear is causing synovial fluid to collect in the knee, the surgeon removes or repairs the torn cartilage. At the same time, the surgeon can also remove fluid from the cyst.
Rarely, surgery is needed to remove the cyst. This approach is typically used only after other treatment options haven't helped the pain and the ability to walk or perform other activities is still limited.
Lifestyle and home remedies
If arthritis is causing the cyst, your health care provider may advise you to take some or all of the following steps:
- Follow the R.I.C.E. principles. These letters stand for rest, ice, compression and elevation. Rest your leg. Ice your knee. Compress your knee with a wrap, sleeve or brace. And elevate your leg when possible, especially at night.
- Try over-the-counter pain-relieving medications. Drugs such as ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve, others), acetaminophen (Tylenol, others) and aspirin can help relieve pain. Follow the dosing instructions on the package. Don't take more than the recommend dosage.
- Reduce your physical activity. Doing so will reduce irritation of your knee joint. Your health care provider can offer you guidance on how long you need to reduce your activity levels. Your provider may be able to suggest alternative forms of exercise you can do in the meantime.
Preparing for an appointment
Here's some information to help you prepare for your appointment.
What you can do
- Write down symptoms you have, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Write down key personal information, including recent life changes.
- List all medications, vitamins and supplements you're taking.
- Write down questions to ask your health care provider.
Your time with your care provider may be limited, so preparing a list of questions can help you make the most of your time together. For a Baker cyst, some basic questions to ask include:
- What caused this cyst to develop?
- What tests do I need? Do these tests require special preparation?
- Is a Baker cyst temporary or long lasting?
- What treatments are available, and which do you recommend?
- What side effects can I expect from treatment?
- What steps can I take on my own that might help?
- Do I need to limit my activity? If so, how much and for how long?
- I have other health conditions. How can I best manage these conditions together?
Don't hesitate to ask other questions.
What to expect from your doctor
Your health care provider is likely to ask you a number of questions, such as:
- When did your symptoms begin?
- Do you feel pain or stiffness all the time, or does the pain come and go with activity?
- Does your knee swell, feel unstable or lock?
- How severe are your symptoms?
- Does anything seem to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Last Updated Sep 27, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




