Impetigo
Overview
Impetigo (im-puh-TIE-go) is a common and highly contagious skin infection that mainly affects infants and young children. It usually appears as reddish sores on the face, especially around the nose and mouth and on the hands and feet. Over about a week, the sores burst and develop honey-colored crusts.
Treatment with antibiotics can limit the spread of impetigo to others. Keep children home from school or day care until they're no longer contagious — usually 24 hours after beginning antibiotic treatment.
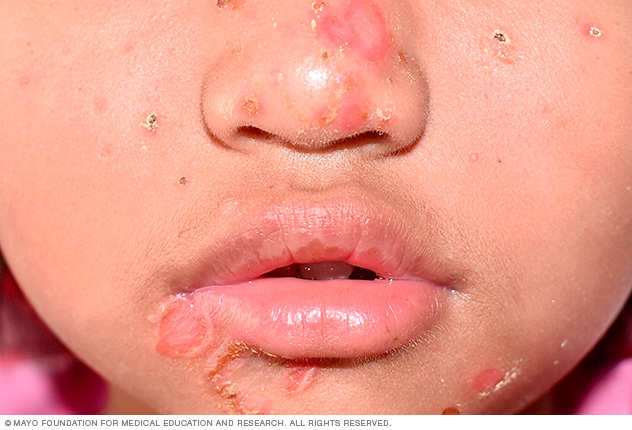
Impetigo starts as a reddish sore that ruptures, oozes for a few days and then forms a honey-colored crust. Sores mainly occur around the nose and mouth in infants and children.
Symptoms
The main symptom of impetigo is reddish sores, often around the nose and mouth. The sores quickly rupture, ooze for a few days and then form a honey-colored crust. Sores can spread to other areas of the body through touch, clothing and towels. Itching and soreness are generally mild.
A less common form of the condition called bullous impetigo causes larger blisters on the trunk of infants and young children. Ecthyma is a serious form of impetigo that causes painful fluid- or pus-filled sores.
When to see a doctor
If you suspect that you or your child has impetigo, consult your family doctor, your child's pediatrician or a dermatologist.
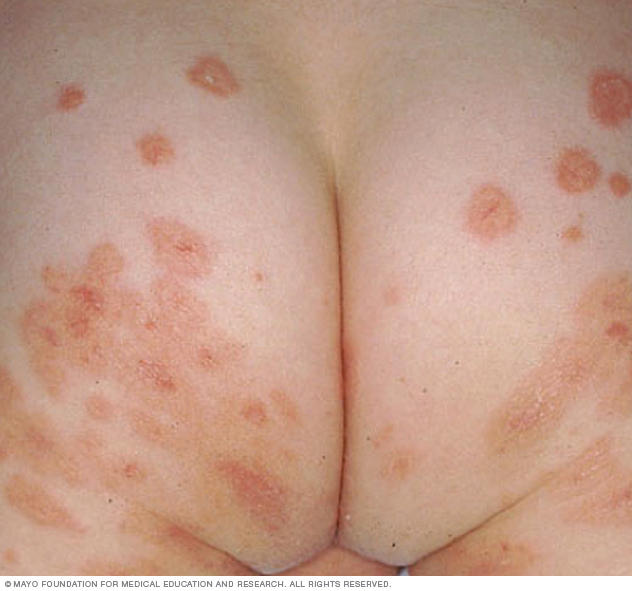
Bullous impetigo causes fluid-filled blisters — often on the trunk, arms and legs of infants and children younger than 2 years.
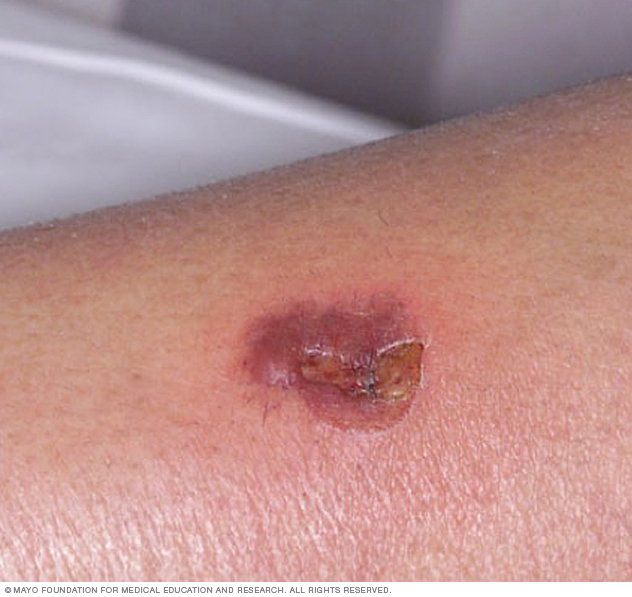
A more serious form of impetigo, called ecthyma, penetrates deeper into the skin — causing painful fluid- or pus-filled sores that turn into deep ulcers.
Causes
Impetigo is caused by bacteria, usually staphylococci organisms.
You might be exposed to the bacteria that cause impetigo when you come into contact with the sores of someone who's infected or with items they've touched — such as clothing, bed linen, towels and even toys.
Risk factors
Factors that increase the risk of impetigo include:
- Age. Impetigo occurs most commonly in children ages 2 to 5.
- Close contact. Impetigo spreads easily within families, in crowded settings, such as schools and child care facilities, and from participating in sports that involve skin-to-skin contact.
- Warm, humid weather. Impetigo infections are more common in warm, humid weather.
- Broken skin. The bacteria that cause impetigo often enter the skin through a small cut, insect bite or rash.
- Other health conditions. Children with other skin conditions, such as atopic dermatitis (eczema), are more likely to develop impetigo. Older adults, people with diabetes or people with a weakened immune system are also more likely to get it.
Complications
Impetigo typically isn't dangerous. And the sores in mild forms of the infection generally heal without scarring.
Rarely, complications of impetigo include:
- Cellulitis. This potentially life-threatening infection affects the tissues underlying the skin and eventually may spread to the lymph nodes and bloodstream.
- Kidney problems. One of the types of bacteria that cause impetigo can also damage the kidneys.
- Scarring. The sores associated with ecthyma can leave scars.
Prevention
Keeping skin clean is the best way to keep it healthy. It's important to wash cuts, scrapes, insect bites and other wounds right away.
To help prevent impetigo from spreading to others:
- Gently wash the affected areas with mild soap and running water and then cover lightly with gauze.
- Wash an infected person's clothes, linens and towels every day with hot water and don't share them with anyone else in your family.
- Wear gloves when applying antibiotic ointment and wash your hands thoroughly afterward.
- Cut an infected child's nails short to prevent damage from scratching.
- Encourage regular and thorough handwashing and good hygiene in general.
- Keep your child with impetigo home until your doctor says they aren't contagious.
Diagnosis
To diagnose impetigo, your doctor might look for sores on your face or body. Lab tests generally aren't needed.
If the sores don't clear, even with antibiotic treatment, your doctor might take a sample of the liquid produced by a sore and test it to see what types of antibiotics would work best on it. Some types of the bacteria that cause impetigo have become resistant to certain antibiotics.
Treatment
Impetigo is treated with prescription mupirocin antibiotic ointment or cream applied directly to the sores two to three times a day for five to 10 days.
Before applying the medicine, soak the area in warm water or apply a wet cloth compress for a few minutes. Then pat dry and gently remove any scabs so the antibiotic can get into the skin. Place a nonstick bandage over the area to help prevent the sores from spreading.
For ecthyma or if more than just a few impetigo sores are present, your doctor might prescribe antibiotics taken by mouth. Be sure to finish the entire course of medication even if the sores are healed.
Lifestyle and home remedies
For minor infections that haven't spread to other areas, you could try treating the sores with an over-the-counter antibiotic cream or ointment. Placing a nonstick bandage over the area can help prevent the sores from spreading. Avoid sharing personal items, such as towels or athletic equipment, while contagious.
Preparing for an appointment
When you call your family doctor or child's pediatrician to make an appointment, ask if you need to do anything to prevent infecting others in the waiting room.
Here's some information to help you get ready for your appointment.
What you can do
Make a list of the following in preparation for your appointment:
- Symptoms you or your child is experiencing
- All medications, vitamins and supplements that your or your child is taking
- Key medical information, including other conditions
- Questions to ask your doctor
Questions to ask your doctor
- What might be causing the sores?
- Are tests needed to confirm the diagnosis?
- What is the best course of action?
- What can I do to prevent the infection from spreading?
- What skin care routines do you recommend while the condition heals?
In addition to the questions that you've prepared to ask your doctor, don't hesitate to ask other questions during your appointment.
What to expect from your doctor
Your doctor is likely to ask you a number of questions, such as:
- When did the sores start?
- What did the sores look like when they started?
- Have you had any recent cuts, scrapes or insect bites to the affected area?
- Are the sores painful or itchy?
- What, if anything, makes the sores better or worse?
- Does someone in your family already have impetigo?
- Has this problem occurred in the past?
Last Updated Apr 8, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



