Lynch syndrome
Overview
Lynch syndrome is a condition that increases the risk of many kinds of cancer. This condition is passed from parents to children.
Families that have Lynch syndrome have more instances of cancer than expected. This might include colon cancer, endometrial cancer and other types of cancer. Lynch syndrome also causes cancers to happen at an earlier age.
People with Lynch syndrome may need careful testing to look for cancer when it's small. Treatment is more likely to be successful when the cancer is caught early. Some people with Lynch syndrome might consider treatments to prevent cancer.
Lynch syndrome used to be called hereditary nonpolyposis colorectal cancer (HNPCC). HNPCC is a term used to describe families with a strong history of colon cancer. Lynch syndrome is the term used when doctors find a gene that runs in the family and causes cancer.
Symptoms
People with Lynch syndrome may experience:
- Colon cancer before age 50
- Cancer of the inside lining of the uterus (endometrial cancer) before age 50
- A personal history of more than one type of cancer
- A family history of cancer before age 50
- A family history of other cancers caused by Lynch syndrome, including stomach cancer, ovarian cancer, pancreatic cancer, kidney cancer, bladder cancer, ureteral cancer, brain cancer, small intestine cancer, gallbladder cancer, bile duct cancer and skin cancer
When to see a doctor
If a family member has Lynch syndrome, tell your health care provider. Ask your provider to help set up an appointment with a professional trained in genetics, such as a genetic counselor. This person can help you understand Lynch syndrome, what causes it and whether genetic testing is right for you.
Causes
Lynch syndrome is caused by genes that are passed from parents to children.
Genes are pieces of DNA. DNA is like a set of instructions for every chemical process that happens in the body.
As cells grow and make new cells as part of their lifecycle, they make copies of their DNA. Sometimes the copies have errors. The body has a set of genes that hold the instructions for finding the errors and fixing them. Doctors call these genes mismatch repair genes.
People with Lynch syndrome have mismatch repair genes that don't work as expected. If an error happens in the DNA, it might not get fixed. This could cause cells that grow out of control and become cancer cells.
Lynch syndrome runs in families in an autosomal dominant inheritance pattern. This means that if one parent has genes that cause Lynch syndrome, there's a 50% chance that each child will have the genes that cause Lynch syndrome. Which parent carries the gene doesn't affect the risk.
Complications
Knowing that you have Lynch syndrome can raise concerns about your health. It may also raise some concerns about other parts of your life. These might include:
- Your privacy. You may have questions about what could happen if others find out you have Lynch syndrome. For instance, you might be concerned that your job or insurance companies might find out. A genetics professional can explain the laws that may protect you.
- Your children. If you have Lynch syndrome, your children have a risk of inheriting it from you. A genetics professional can help you come up with a plan for talking about this with your children. The plan might include how and when to tell them and when they should consider testing.
- Your extended family. Having Lynch syndrome has implications for your entire family. Other blood relatives may have a chance of having Lynch syndrome. A genetics professional can help you come up with the best way to tell family members.
Diagnosis
Diagnosing Lynch syndrome might start with a review of your family history of cancer. Your health care provider will want to know whether you or anyone in your family has had colon cancer, endometrial cancer and other cancers. This may lead to other tests and procedures to diagnose Lynch syndrome.
Family history
Your provider may want you to consider genetic testing for Lynch syndrome if your family history has one or more of the following:
- Multiple relatives with any Lynch-associated cancers, including colon cancer and endometrial cancer. Other cancers caused by Lynch syndrome include those that happen in the stomach, ovaries, pancreas, kidneys, bladder, ureters, brain, gallbladder, bile ducts, small intestine and skin.
- One or more family members who had cancer before age 50.
- One or more family members who have had more than one type of cancer.
- More than one generation of family with the same type of cancer.
Testing cancer cells
If you or someone in your family has had cancer, a sample of the cancer cells might be tested.
Tests on cancer cells include:
- Immunohistochemistry (IHC) testing. IHC testing uses special dyes to stain tissue samples. The presence or absence of staining shows whether the tissue has certain proteins. Missing proteins might help determine if the genes related to Lynch syndrome caused the cancer.
- Microsatellite instability (MSI) testing. Microsatellites are pieces of DNA. In people with Lynch syndrome, there may be errors or instability in these pieces.
Positive IHC or MSI test results can show that the cancer cells have genetic changes that are connected to Lynch syndrome. But the results can't say for certain whether you have Lynch syndrome. Some people have these genetic changes only in their cancer cells. This means the genetic changes weren't inherited.
People with Lynch syndrome have the genes that cause Lynch syndrome in all the cells in their bodies. Genetic testing is needed to see if all the cells have these genes.
Genetic testing
Genetic testing looks for changes in the genes that cause Lynch syndrome. You may give a sample of your blood for this test.
If a family member has Lynch syndrome, your test might look only for the gene that runs in your family. If you're the first person in your family to be tested for Lynch syndrome, your test might examine many genes that can run in families. A genetics professional can help decide which test is best for you.
Genetic testing may show:
-
A positive genetic test result. A positive result means that a genetic change that causes Lynch syndrome was found in your cells. It doesn't mean you'll get cancer. But it does mean that your risk of certain cancers is higher than people who don't have Lynch syndrome.
Your personal risk of cancer depends on which genes run in your family. You can lower your risk with tests to look for signs of cancer. Some treatments can help lower your risk of certain cancers. A genetics professional can explain your individual risk to you based on your results.
- A negative genetic test result. A negative result means gene changes that cause Lynch syndrome weren't found in your cells. It means you probably don't have Lynch syndrome. But you could still have an increased risk of cancer. That's because people with a strong family history of cancer may have an increased risk of the disease.
- A gene variation of unknown significance. Genetic tests don't always give you a yes or no answer. Sometimes genetic testing finds a gene that doctors aren't sure about. A genetics professional can tell you what this means for your health.
Treatment
There's no cure for Lynch syndrome. People with Lynch syndrome often have tests to look for early signs of cancer. If cancer is found when it's small, treatment is more likely to be successful.
Sometimes cancer can be prevented with operations to remove some organs before they can develop cancer. Talk with your health care provider about your options.
Cancer screening for people with Lynch syndrome
Cancer screening tests are tests that look for signs of cancer in people who don't have any cancer symptoms. Which cancer tests you need depends on your situation. Your health care provider will consider which Lynch syndrome gene you carry. Your provider also considers what cancers run in your family.
You might have tests to look for:
- Colon cancer. A colonoscopy is a procedure that uses a long flexible tube to look at the inside of your colon. This exam can find precancerous growths and areas of cancer. People with Lynch syndrome may begin colonoscopy screening every year or two starting in their 20s or 30s.
- Endometrial cancer. Endometrial cancer is cancer that starts in the inside lining of the uterus. The lining is called the endometrium. To look for this cancer, you might have ultrasound imaging of the uterus. A sample of endometrium might be removed. The sample is tested for signs of cancer. This procedure is called an endometrial biopsy.
- Ovarian cancer. Your provider may suggest an ultrasound and blood test to look for signs of cancer in the ovaries.
- Stomach cancer and small intestine cancer. Your provider might suggest a procedure to look at the inside of your esophagus, stomach and small intestine. This procedure is called an endoscopy. It involves passing a long, thin tube with a camera on the end down your throat. You might also have a test to look for a bacteria that increases the risk of stomach cancer.
- Urinary system cancer. Your provider may suggest testing a sample of your urine to look for signs of urinary system cancers. This includes cancer in the kidneys, bladder and the ureters. The ureters are tubes that connect the kidneys to the bladder.
- Pancreatic cancer. Your provider might suggest an imaging test to look for cancer in the pancreas. This is usually with an MRI.
- Brain cancer. Your provider might suggest a neurological exam. This exam involves testing your vision, hearing, balance, coordination and reflexes. This test looks for signs that a brain cancer is pressing on your brain tissue or nerves.
- Skin cancer. Your provider might suggest a skin exam. This involves looking at your whole body for signs of skin cancer.
You might need other tests if your family has a history of other types of cancer. Ask your provider about which tests are best for you.
Aspirin for cancer prevention
Some research suggests that taking a daily aspirin may lower the risk of cancer in people with Lynch syndrome. More research is needed to understand how much aspirin is needed to get the most benefit. Discuss the potential benefits and risks of aspirin therapy with your provider. Together you can decide whether this might be right for you.
Treatments to prevent cancers caused by Lynch syndrome
In certain situations, you might consider surgery or treatments to prevent cancer. Discuss the benefits and risks with your health care provider.
Treatments may be available for:
- Endometrial cancer prevention. Surgery to remove the uterus is called hysterectomy. It prevents endometrial cancer. Another option may be a procedure to place a contraceptive device in the uterus. The device, called an intrauterine device (IUD), emits a hormone that lowers the risk of endometrial cancer. It also prevents you from getting pregnant.
- Ovarian cancer prevention. Surgery to remove the ovaries is called oophorectomy. It greatly reduces the risk of ovarian cancer. Another option might be oral contraceptive pills, which are also called birth control pills. Research suggests taking oral contraceptive pills for at least 5 years lowers the risk of ovarian cancer.
- Colon cancer prevention. Surgery to remove most or all of your colon is called colectomy. It lowers your risk of colon cancer. This operation might be an option in certain situations. For example, it might be an option if you've had colon cancer. Removing your colon would prevent you from getting colon cancer again.
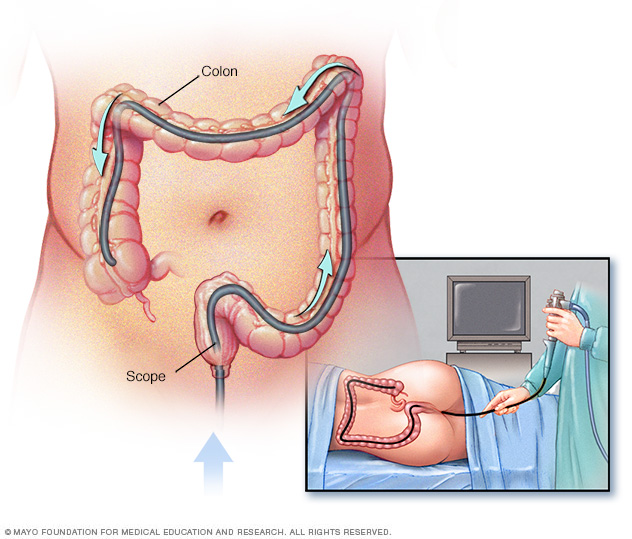
During a colonoscopy, the healthcare professional puts a colonoscope into the rectum to check the entire colon.
Coping and support
Having Lynch syndrome can be stressful. Knowing that you have an increased risk of cancer can make you feel worried about your future. In time, you'll find ways to cope with the stress and worry. Until then, you might find it helpful to:
- Find out all you can about Lynch syndrome. Make a list of questions about Lynch syndrome and ask them at your next appointment. Ask your health care team for further sources of information. Learning about Lynch syndrome can help you feel more confident when making decisions about your health.
- Take care of yourself. Knowing that you have an increased risk of cancer can make you feel as if you can't control your health. Make healthy choices for the parts of your health you can control. For instance, choose a healthy diet. Exercise most days of the week. Maintain a healthy weight. Get enough sleep so that you wake feeling rested. Go to all your scheduled medical appointments, including your cancer-screening exams.
- Connect with others. Find friends and family with whom you can discuss your fears. Connect with other people with Lynch syndrome through advocacy groups. Examples include Lynch Syndrome International and Facing Our Risk of Cancer Empowered (FORCE). Find other trusted people you can talk with, such as clergy members. Ask for a referral to a therapist who can help you understand your feelings.
Preparing for an appointment
If your health care provider thinks you could have Lynch syndrome, they may suggest that you meet with a genetics professional, such as a genetic counselor.
A genetics professional can help you decide whether genetic testing would be useful for you. If you choose to have the test, they can help you understand your results.
What you can do
To prepare for your meeting with the genetics professional:
- Gather your medical records. If you've had cancer, bring your medical records to your appointment.
- Ask family members who've had cancer for information. If your family members have had cancer, ask for information about their diagnoses. Write down the types of cancer, types of treatments and ages at diagnosis.
- Consider taking a family member or friend along. Sometimes it can be hard to remember all the information provided during an appointment. Someone who comes with you may remember something that you missed or forgot.
- Write down questions to ask.
Questions to ask
Prepare a list of questions to ask. Questions could include:
- What causes Lynch syndrome?
- How is Lynch syndrome passed through families?
- If I have a family member with Lynch syndrome, what is the chance that I have it, too?
- What types of tests are involved in genetic testing?
- What will the results of genetic testing tell me?
- How long can I expect to wait for my results?
- If my genetic test result is positive, what is the chance that I will get cancer?
- What types of tests can detect Lynch-related cancers at an early stage?
- If my genetic test result is negative, does that mean I won't get cancer?
- Are genetic testing results ever wrong or not clear?
- What will my genetic test results mean for my family?
- How much does genetic testing cost?
- Will my insurance company pay for genetic testing?
- What laws protect me from discrimination if my genetic test result is positive?
- Is it OK to decide against genetic testing?
- If I choose to not have genetic testing, what does that mean for my future health?
- Are there brochures or other printed material that I can take with me? What websites do you suggest?
In addition to the questions that you've prepared, ask any other questions that you think of during your appointment.
What to expect
The genetics professional will likely ask questions about your health history and the health history of your family members. Questions may include:
- Have you ever had cancer?
- Have members of your family had cancer?
- At what age was each family member with cancer diagnosed?
- Have any family members ever had genetic testing?
Last Updated Jul 15, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



