Ruptured eardrum (perforated eardrum)
Overview
A ruptured eardrum (tympanic membrane perforation) is a hole or tear in the thin tissue that separates the ear canal from the middle ear (eardrum).
A ruptured eardrum can result in hearing loss. It can also make the middle ear vulnerable to infections.
A ruptured eardrum usually heals within a few weeks without treatment. But sometimes it requires a patch or surgical repair to heal.
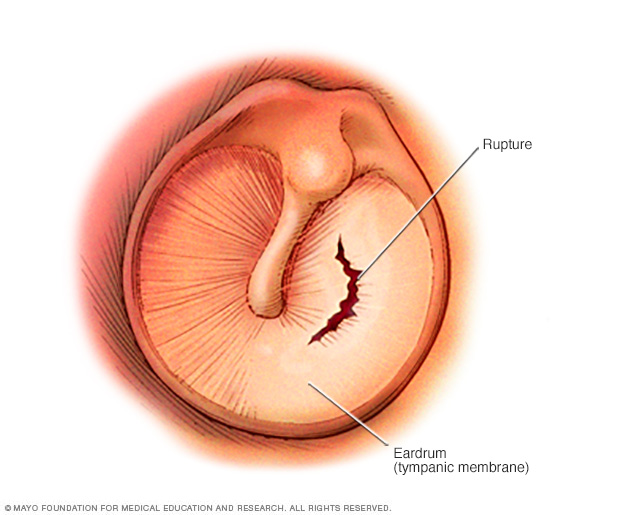
A ruptured (perforated) eardrum prevents the proper transmission of sound waves to the middle ear and leaves the middle ear vulnerable to infectious agents, water and other foreign substances.
Symptoms
Signs and symptoms of a ruptured eardrum may include:
- Ear pain that may subside quickly
- Mucuslike, pus-filled or bloody drainage from the ear
- Hearing loss
- Ringing in the ear (tinnitus)
- Spinning sensation (vertigo)
- Nausea or vomiting that can result from vertigo
When to see a doctor
Call your health care provider if you have signs or symptoms of a ruptured eardrum. The middle and inner ears are made up of delicate structures that are sensitive to injury or disease. It is important to try to figure out the cause of ear symptoms and determine whether a ruptured eardrum has occurred.
Causes
Causes of a ruptured (perforated) eardrum may include:
- Middle ear infection (otitis media). A middle ear infection often results in the accumulation of fluids in the middle ear. Pressure from these fluids can cause the eardrum to rupture.
-
Barotrauma. Barotrauma is stress exerted on the eardrum when the air pressure in the middle ear and the air pressure in the environment are out of balance. If the pressure is severe, the eardrum can rupture. Barotrauma is most often caused by air pressure changes associated with air travel.
Other events that can cause sudden changes in pressure — and possibly a ruptured eardrum — include scuba diving and a direct blow to the ear, such as the impact of an automobile air bag.
- Loud sounds or blasts (acoustic trauma). A loud sound or blast, as from an explosion or gunshot — essentially an overpowering sound wave — can rarely cause a tear in the eardrum.
- Foreign objects in your ear. Small objects, such as a cotton swab or hairpin, can puncture or tear the eardrum.
- Severe head trauma. Severe injury, such as a skull base fracture, may cause the dislocation of or damage to middle and inner ear structures, including the eardrum.
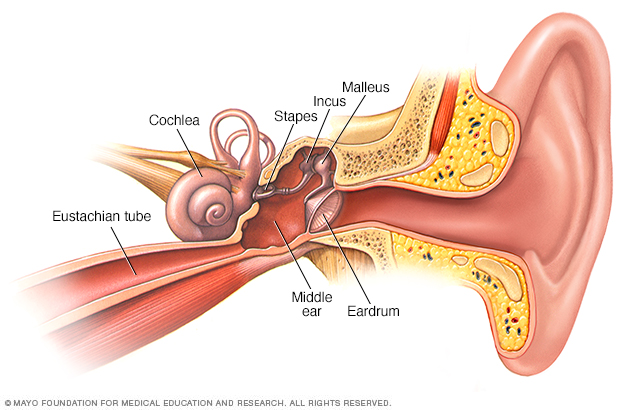
The middle ear includes three small bones. They are the hammer, called the malleus; the anvil, known as the incus; and the stirrup, known as the stapes. The eardrum lies between the middle ear and outer ear. The middle ear connects to the back of the nose and throat by a narrow area called the eustachian tube. The snail-shaped cochlea is part of the inner ear.
Complications
The eardrum (tympanic membrane) has two primary roles:
- Hearing. When sound waves strike it, the eardrum vibrates — the first step by which structures of the middle and inner ears translate sound waves into nerve impulses.
- Protection. The eardrum also acts as a barrier, protecting the middle ear from water, bacteria and other foreign substances.
If the eardrum ruptures, uncommon problems can occur, especially if it fails to self-heal after three to six months. Possible complications include:
- Hearing loss. Usually, hearing loss is temporary, lasting only until the tear or hole in the eardrum has healed. The size and location of the tear can affect the degree of hearing loss.
- Middle ear infection (otitis media). A ruptured (perforated) eardrum can allow bacteria to enter the ear. If a perforated eardrum doesn't heal, a small number of people may be vulnerable to ongoing (recurrent or chronic) infections. In this small group, chronic drainage and hearing loss can occur.
Middle ear cyst (cholesteatoma). Although very rare, this cyst, which is composed of skin cells and other debris, can develop in the middle ear as a long-term result of eardrum rupture.
Ear canal debris normally travels to the outer ear with the help of ear-protecting earwax. If the eardrum is ruptured, the skin debris can pass into the middle ear and form a cyst.
A cyst in the middle ear provides a friendly environment for bacteria and contains proteins that can damage the bones of the middle ear.
Prevention
Follow these tips to avoid a ruptured (perforated) eardrum:
- Get treatment for middle ear infections. Be aware of the signs and symptoms of middle ear infection, including earache, fever, nasal congestion and reduced hearing. Children with middle ear infections often are fussy and may refuse to eat. Seek prompt evaluation from your provider to prevent potential damage to the eardrum.
Protect your ears during flight. If possible, don't fly if you have a cold or an active allergy that causes nasal or ear congestion. During takeoffs and landings, keep ears clear with pressure-equalizing earplugs, yawning or chewing gum.
Or use the Valsalva maneuver — gently pushing air into the nose, as if blowing your nose, while pinching the nostrils and keeping the mouth closed. Don't sleep during ascents and descents.
- Keep your ears free of foreign objects. Never attempt to dig out excess or hardened earwax with items such as a cotton swab, paper clip or hairpin. These items can easily tear or puncture the eardrum. Teach your children about the damage that can be done by putting foreign objects in their ears.
- Guard against explosive noise. Avoid activities that expose the ears to explosions. If your hobbies or work involves planned activities that produce explosive noise, protect your ears from unnecessary damage by wearing protective earplugs or earmuffs.
Diagnosis
Your provider or an ENT specialist can often determine if you have a ruptured (perforated) eardrum with a visual inspection using a lighted instrument (otoscope or microscope).
Your provider may conduct or order additional tests to determine the cause of your ear symptoms or to detect the presence of any hearing loss. These tests include:
- Laboratory tests. If there's discharge from the ear, your provider may order a laboratory test or culture to detect a bacterial infection of the middle ear.
-
Tuning fork evaluation. Tuning forks are two-pronged, metal instruments that produce sounds when struck. Simple tests with tuning forks can help your provider detect hearing loss.
A tuning fork evaluation may also reveal whether hearing loss is caused by damage to the vibrating parts of the middle ear (including the eardrum), damage to sensors or nerves of the inner ear, or damage to both.
- Tympanometry. A tympanometer uses a device inserted into the ear canal that measures the response of the eardrum to slight changes in air pressure. Certain patterns of response can indicate a perforated eardrum.
- Audiology exam. This is a series of tests that measure how well you hear sounds at different volumes and pitches. The tests are conducted in a soundproof booth.
Treatment
Most ruptured (perforated) eardrums heal without treatment within a few weeks. Your provider may prescribe antibiotic drops if there's evidence of infection. If the tear or hole in the eardrum doesn't heal by itself, treatment will likely involve procedures to close the tear or hole. These may include:
-
Eardrum patch. If the tear or hole in the eardrum doesn't close on its own, an ENT specialist may seal it with a paper patch (or a patch made of other material).
With this office procedure, your ENT doctor may apply a chemical to the edges of the tear, which can promote ear drum healing, and then apply a patch over the hole. The procedure may need to be repeated more than once before the hole closes.
-
Surgery. If a patch doesn't result in proper healing or your ENT doctor determines that the tear isn't likely to heal with a patch, he or she may recommend surgery.
The most common surgical procedure is called tympanoplasty. Your surgeon grafts a patch of your own tissue to close the hole in the eardrum. This procedure is done on an outpatient basis. In an outpatient procedure, you can usually go home the same day unless medical anesthesia conditions require a longer hospital stay.
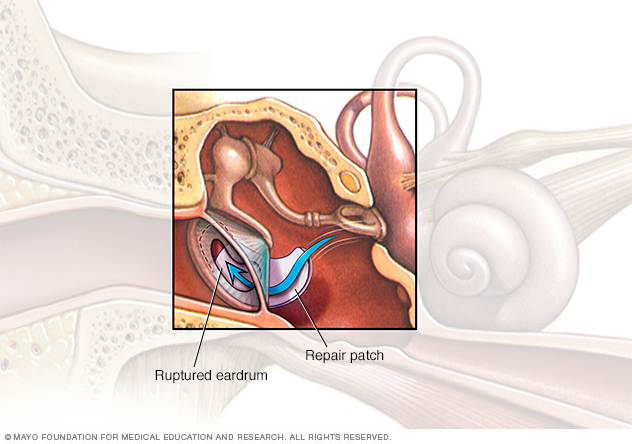
In some cases, your surgeon treats a ruptured eardrum with a procedure called tympanoplasty. Your surgeon grafts a tiny patch of your own tissue to close the hole in the eardrum.
Lifestyle and home remedies
A ruptured (perforated) eardrum usually heals on its own within weeks. In some cases, healing takes months. Until your provider tells you that your ear is healed, protect it by:
- Keeping the ear dry. Place a waterproof silicone earplug or cotton ball coated with petroleum jelly in the ear when showering or bathing.
- Refraining from cleaning the ears. Give the eardrum time to heal completely.
- Avoiding blowing your nose. The pressure created when blowing your nose can damage the healing eardrum.
Preparing for an appointment
If you have signs or symptoms of a perforated eardrum, you're likely to start by seeing your provider. However, your provider may refer you to a specialist in ear, nose and throat (ENT) disorders (otolaryngologist).
Here's some information to help you prepare for your appointment.
What you can do
Make a list ahead of time that you can share with your provider. Your list should include:
- Symptoms you're experiencing, including any that may seem unrelated to hearing loss, fluid discharge or other ear-related symptoms
- Relevant events that may be related to your ear problems, such as a history of ear infections, recent ear injuries or head traumas, or recent air travel
- Medications, including any vitamins or supplements you're taking
- Questions for your provider
If you think you have signs or symptoms of a ruptured eardrum, you may want to ask your provider some of the following questions.
- Do I have a ruptured eardrum?
- What else could be causing my hearing loss and other symptoms?
- If I have a ruptured eardrum, what do I need to do to protect my ear during the healing process?
- What type of follow-up appointments will I need?
- At what point do we need to consider other treatments?
Don't hesitate to ask other questions you have.
What to expect from your doctor
Your provider is likely to ask you a number of questions, including:
- When did you first experience symptoms?
- Did you have symptoms such as pain or vertigo that cleared up?
- Have you had ear infections?
- Have you been exposed to loud sounds?
- Have you been swimming or diving recently?
- Have you recently flown?
- Have you had head injuries?
- Do you put anything in your ear to clean it?
What you can do in the meantime
If you think that you have a ruptured eardrum, be careful to keep your ears dry to prevent infection.
Don't go swimming until your condition has been evaluated and discussed with your provider. To keep water out of the ear when showering or bathing, use a moldable, waterproof silicone earplug or put a cotton ball coated with petroleum jelly in the outer ear.
Don't put medication drops in the ear unless your provider prescribes them specifically for infection related to the perforated eardrum.
Last Updated Jan 18, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



