Episiotomy: When it's needed, when it's not
An episiotomy is a cut (incision) made in the tissue between the vaginal opening and the anus during childbirth. This area is called the perineum.
Although an episiotomy was once a routine part of childbirth, that's no longer the case. If you're planning a vaginal delivery, here's what you need to know about episiotomy and childbirth.
The episiotomy tradition
For years, an episiotomy was thought to help prevent larger vaginal tears during childbirth. Experts believed an incision would heal better than a natural tear. The procedure was also thought to help preserve the muscles and connective tissue that support the pelvic floor.
Today, however, research suggests that routine episiotomies don't prevent these problems after all.
The new approach
Routine episiotomies are no longer recommended. Still, the procedure is sometimes needed. An incision might be recommended if a baby needs to be quickly delivered because:
- The baby's shoulder is stuck behind the pelvic bone
- The baby has an unusual heart rate pattern during delivery
- Forceps or vacuum extraction is needed during a vaginal delivery
How it works
If you need an episiotomy, you typically won't feel the incision or the repair. If you haven't had anesthesia or if the anesthesia has worn off, you'll likely receive an injection of a local anesthetic to numb the tissue.
Your health care provider will discuss different techniques for improving your comfort as you heal.
There are two types of episiotomy incisions:
- Midline incision. A midline incision is done vertically. A midline incision is easier to repair. But it has a higher risk of extending into the anal area.
- Mediolateral incision. A mediolateral incision is done at an angle. A mediolateral incision is less likely to result in an extended tear into the anal area. However, this incision is often more painful and more difficult to repair.
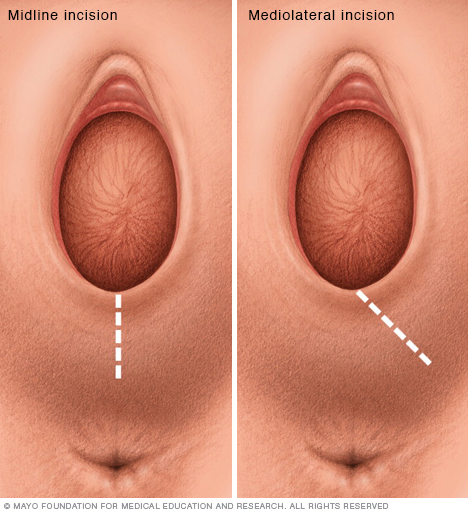
An episiotomy is an incision made in the perineum — the tissue between the vaginal opening and the anus — during childbirth. A midline (median) incision (shown at left) is done vertically. A mediolateral incision (shown at right) is done at an angle. A midline incision is easier to repair, but it has a higher risk of extending into the anal area. A mediolateral incision offers the best protection from an extended tear affecting the anal area, but it is often more painful and is more difficult to repair.
Episiotomy risks
Episiotomy recovery is uncomfortable. Sometimes the incision is more extensive than a natural tear would have been. Infection is possible. For some, an episiotomy causes pain during sex in the months after delivery.
A midline episiotomy puts you at risk of fourth-degree vaginal tearing. This type of tearing extends through the anal sphincter and into the mucous membrane that lines the rectum. Fecal incontinence could result.
Healing from an episiotomy
Any stitches used to repair the episiotomy are usually absorbed on their own. You might take prescription medications or use a nonprescription pain reliever or stool softener. However, pain-relieving creams or ointments haven't been found to be effective for episiotomy wounds.
While you're healing, expect the discomfort to improve over time. Contact your health care provider if the pain gets worse. Also call your provider if you develop a fever or if the wound produces pus. These could be symptoms of an infection.
Accept some uncertainty
Share your thoughts about episiotomy with your health care provider during your prenatal visits and when labor begins. Remember, though, to go into labor with an open mind. It'll take time for the baby to stretch the vaginal tissues to allow delivery. But sometimes the baby needs to be delivered before the vaginal tissues can stretch on their own.
Count on your health care provider to respect your wishes about episiotomy — and to let you know when it's the safest option for you and your baby.
Last Updated Aug 2, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use