Adenomyosis
Overview
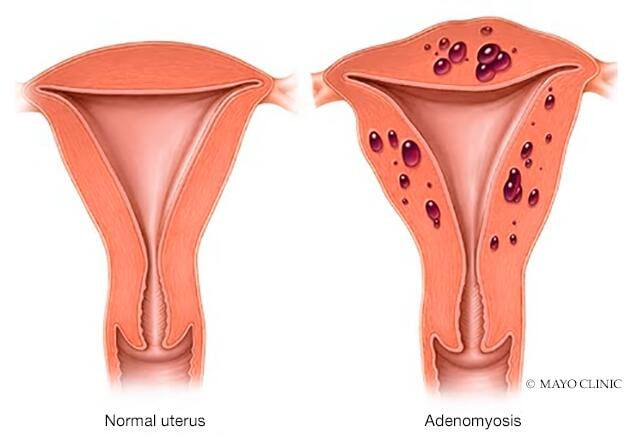
Adenomyosis (ad-uh-no-my-O-sis) occurs when the tissue that normally lines the uterus (endometrial tissue) grows into the muscular wall of the uterus. The displaced tissue continues to act normally — thickening, breaking down and bleeding — during each menstrual cycle. An enlarged uterus and painful, heavy periods can result.
Doctors aren't sure what causes adenomyosis, but the disease usually resolves after menopause. For women who have severe discomfort from adenomyosis, hormonal treatments can help. Removal of the uterus (hysterectomy) cures adenomyosis
Symptoms
Sometimes, adenomyosis causes no signs or symptoms or only mild discomfort. However, adenomyosis can cause:
- Heavy or prolonged menstrual bleeding
- Severe cramping or sharp, knifelike pelvic pain during menstruation (dysmenorrhea)
- Chronic pelvic pain
- Painful intercourse (dyspareunia)
Your uterus might get bigger. Although you might not know if your uterus is bigger, you may notice tenderness or pressure in your lower abdomen.
When to see a doctor
If you have prolonged, heavy bleeding or severe cramping during your periods that interferes with your regular activities, make an appointment to see your doctor.
Causes
The cause of adenomyosis isn't known. There have been many theories, including:
- Invasive tissue growth. Some experts believe that endometrial cells from the lining of the uterus invade the muscle that forms the uterine walls. Uterine incisions made during an operation such as a cesarean section (C-section) might promote the direct invasion of the endometrial cells into the wall of the uterus.
- Developmental origins. Other experts suspect that endometrial tissue is deposited in the uterine muscle when the uterus is first formed in the fetus.
- Uterine inflammation related to childbirth. Another theory suggests a link between adenomyosis and childbirth. Inflammation of the uterine lining during the postpartum period might cause a break in the normal boundary of cells that line the uterus.
- Stem cell origins. A recent theory proposes that bone marrow stem cells might invade the uterine muscle, causing adenomyosis.
Regardless of how adenomyosis develops, its growth depends on the body's circulating estrogen.
Risk factors
Risk factors for adenomyosis include:
- Prior uterine surgery, such as C-section, fibroid removal, or dilatation and curettage (D&C)
- Childbirth
- Middle age
Most cases of adenomyosis — which depends on estrogen — are found in women in their 40s and 50s. Adenomyosis in these women could relate to longer exposure to estrogen compared with that of younger women. However, current research suggests that the condition might also be common in younger women.
Complications
If you often have prolonged, heavy bleeding during your periods, you can develop chronic anemia, which causes fatigue and other health problems.
Although not harmful, the pain and excessive bleeding associated with adenomyosis can disrupt your lifestyle. You might avoid activities you've enjoyed in the past because you're in pain or you worry that you might start bleeding.
Diagnosis
Some other uterine conditions can cause signs and symptoms similar to those of adenomyosis, making adenomyosis difficult to diagnose. These conditions include fibroid tumors (leiomyomas), uterine cells growing outside the uterus (endometriosis) and growths in the uterine lining (endometrial polyps).
Your doctor might conclude that you have adenomyosis only after ruling out other possible causes for your signs and symptoms.
Your doctor may suspect adenomyosis based on:
- Signs and symptoms
- A pelvic exam that reveals an enlarged, tender uterus
- Ultrasound imaging of the uterus
- Magnetic resonance imaging (MRI) of the uterus
In some instances, your doctor might collect a sample of uterine tissue for testing (endometrial biopsy) to make sure you don't have a more serious condition. But an endometrial biopsy won't help your doctor confirm a diagnosis of adenomyosis.
Pelvic imaging such as ultrasound and MRI can detect signs of adenomyosis, but the only way to confirm it is to examine the uterus after hysterectomy.
Treatment
Adenomyosis often goes away after menopause, so treatment might depend on how close you are to that stage of life.
Treatment options for adenomyosis include:
- Anti-inflammatory drugs. Your doctor might recommend anti-inflammatory medications, such as ibuprofen (Advil, Motrin IB, others), to control the pain. By starting an anti-inflammatory medicine one to two days before your period begins and taking it during your period, you can reduce menstrual blood flow and help relieve pain.
- Hormone medications. Combined estrogen-progestin birth control pills or hormone-containing patches or vaginal rings might lessen heavy bleeding and pain associated with adenomyosis. Progestin-only contraception, such as an intrauterine device, or continuous-use birth control pills often cause amenorrhea — the absence of your menstrual periods — which might provide some relief.
- Hysterectomy. If your pain is severe and no other treatments have worked, your doctor might suggest surgery to remove your uterus. Removing your ovaries isn't necessary to control adenomyosis.
Self care
To ease pelvic pain and cramping related to adenomyosis, try these tips:
- Soak in a warm bath.
- Use a heating pad on your abdomen.
- Take an over-the-counter anti-inflammatory medication, such as ibuprofen (Advil, Motrin IB, others).
Preparing for your appointment
Your first appointment will be with either your primary care provider or your gynecologist.
What you can do
Make a list of:
- Your signs and symptoms, and when they began
- All medications, vitamins and other supplements you take, including dosages
- Medical information, including menstrual and childbirth history
- Questions to ask your doctor
For adenomyosis, basic questions to ask your doctor include:
- Are there medications I can take to improve my symptoms?
- Under what circumstances do you recommend surgery?
- Could my condition affect my ability to become pregnant?
Don't hesitate to ask other questions.
What to expect from your doctor
Your doctor might ask you:
- When do symptoms typically occur?
- How severe are your symptoms?
- When was your last period?
- Could you be pregnant?
- Are you using a birth control method? If so, which one?
- Do your symptoms seem to be related to your menstrual cycle?
- Does anything seem to improve your symptoms?
- Does anything make your symptoms worse?
Last Updated Apr 6, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use