Atopic dermatitis (eczema)
Overview
Atopic dermatitis (eczema) is a condition that causes dry, itchy and inflamed skin. It's common in young children but can occur at any age. Atopic dermatitis is long lasting (chronic) and tends to flare sometimes. It can be irritating but it's not contagious.
People with atopic dermatitis are at risk of developing food allergies, hay fever and asthma.
Moisturizing regularly and following other skin care habits can relieve itching and prevent new outbreaks (flares). Treatment may also include medicated ointments or creams.
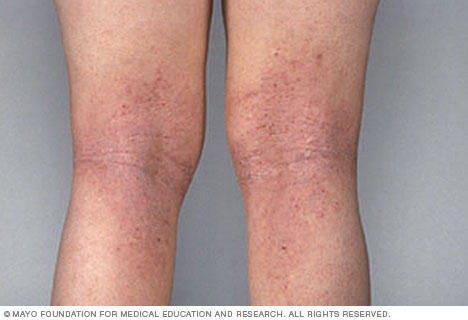
Atopic dermatitis can cause a very itchy rash. Atopic dermatitis most often occurs where the skin flexes — inside the elbows, behind the knees and in front of the neck.
Symptoms
Atopic dermatitis (eczema) symptoms can appear anywhere on the body and vary widely from person to person. They may include:
- Dry, cracked skin
- Itchiness (pruritus)
- Rash on swollen skin that varies in color depending on your skin color
- Small, raised bumps, on brown or Black skin
- Oozing and crusting
- Thickened skin
- Darkening of the skin around the eyes
- Raw, sensitive skin from scratching
Atopic dermatitis often begins before age 5 and may continue into the teen and adult years. For some people, it flares and then clears up for a time, even for several years.
When to see a doctor
Talk with a health care provider if you or your child:
- Has symptoms of atopic dermatitis
- Is so uncomfortable that the condition is affecting sleep and daily activities
- Has a skin infection — look for new streaks, pus, yellow scabs
- Has symptoms even after trying self-care steps
Seek immediate medical attention if you or your child has a fever and the rash looks infected.
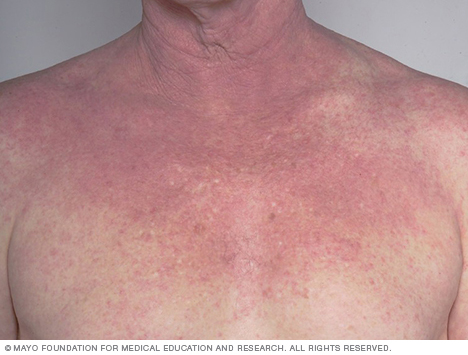
Inflammation caused by atopic dermatitis can cover large areas of the body, such as the chest, or be limited to a few small spots.
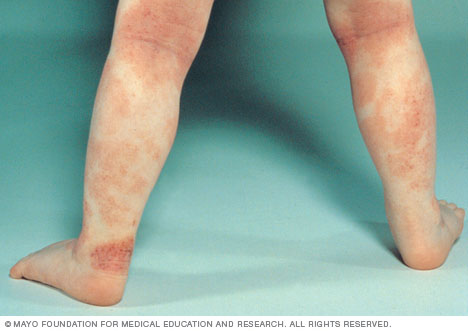
Atopic dermatitis in infants (infantile eczema) appears here as red, itchy patches on very dry skin.
Causes
In some people, atopic dermatitis is related to a gene variation that affects the skin's ability to provide protection. With a weak barrier function, the skin is less able to retain moisture and protect against bacteria, irritants, allergens and environmental factors — such as tobacco smoke.
In other people, atopic dermatitis is caused by too much of the bacteria Staphylococcus aureus on the skin. This displaces helpful bacteria and disrupts the skin's barrier function.
A weak skin barrier function might also trigger an immune system response that causes the inflamed skin and other symptoms.
Atopic dermatitis (eczema) is one of several types of dermatitis. Other common types are contact dermatitis and seborrheic dermatitis (dandruff). Dermatitis isn't contagious.
Risk factors
The main risk factor for atopic dermatitis is having had eczema, allergies, hay fever or asthma in the past. Having family members with these conditions also increases your risk.
Complications
Complications of atopic dermatitis (eczema) may include:
- Asthma and hay fever. Many people with atopic dermatitis develop asthma and hay fever. This can happen before or after developing atopic dermatitis.
- Food allergies. People with atopic dermatitis often develop food allergies. One of the main symptoms of this condition is hives (urticaria).
- Chronic itchy, scaly skin. A skin condition called neurodermatitis (lichen simplex chronicus) starts with a patch of itchy skin. You scratch the area, which provides only temporary relief. Scratching actually makes the skin itchier because it activates the nerve fibers in your skin. Over time, you may scratch out of habit. This condition can cause the affected skin to become discolored, thick and leathery.
- Patches of skin that's darker or lighter than the surrounding area. This complication after the rash has healed is called post-inflammatory hyperpigmentation or hypopigmentation. It's more common in people with brown or Black skin. It might take several months for the discoloration to fade.
- Skin infections. Repeated scratching that breaks the skin can cause open sores and cracks. These increase the risk of infection from bacteria and viruses. These skin infections can spread and become life-threatening.
- Irritant hand dermatitis. This especially affects people whose hands are often wet and exposed to harsh soaps, detergents and disinfectant at work.
- Allergic contact dermatitis. This condition is common in people with atopic dermatitis. Allergic contact dermatitis is an itchy rash caused by touching substances you're allergic to. The color of the rash varies depending on your skin color.
- Sleep problems. The itchiness of atopic dermatitis can interfere with sleep.
- Mental health conditions. Atopic dermatitis is associated with depression and anxiety. This may be related to the constant itching and sleep problems common among people with atopic dermatitis.
Prevention
Developing a basic skin care routine may help prevent eczema flares. The following tips may help reduce the drying effects of bathing:
-
Moisturize your skin at least twice a day. Creams, ointments, shea butter and lotions seal in moisture. Choose a product or products that work well for you. Ideally, the best one for you will be safe, effective, affordable and unscented.
Using petroleum jelly on your baby's skin may help prevent development of atopic dermatitis.
- Take a daily bath or shower. Use warm, rather than hot, water and limit your bath or shower to about 10 minutes.
- Use a gentle, nonsoap cleanser. Choose a cleanser that's free of dyes, alcohols and fragrance. For young children, you usually need only warm water to get them clean — no soap or bubble bath needed. Soap can be especially irritating to the skin of young children. For people of any age, deodorant soaps and antibacterial soaps can remove too much of the skin's natural oils and dry the skin. Don't scrub the skin with a washcloth or loofah.
- Pat dry. After bathing, gently pat the skin with a soft towel. Apply moisturizer while your skin is still damp (within three minutes).
The triggers for atopic dermatitis vary widely from person to person. Try to identify and avoid irritants that trigger your eczema. In general, avoid anything that causes an itch because scratching often triggers a flare.
Common triggers for atopic dermatitis include:
- Rough wool fabric
- Dry skin
- Skin infection
- Heat and sweat
- Stress
- Cleaning products
- Dust mites and pet dander
- Mold
- Pollen
- Smoke from tobacco
- Cold and dry air
- Fragrances
- Other irritating chemicals
Infants and children may have flares triggered by eating certain foods, such as eggs and cow's milk. Talk with your child's health care provider about identifying potential food allergies.
Once you understand what triggers your eczema, talk with your health care provider about how to manage your symptoms and prevent flares.
Diagnosis
To diagnose atopic dermatitis, your health care provider will likely talk with you about your symptoms, examine your skin and review your medical history. You may need tests to identify allergies and rule out other skin diseases.
If you think a certain food caused your child's rash, ask your health care provider about potential food allergies.
Patch testing
Your doctor may recommend patch testing on your skin. In this test, small amounts of different substances are applied to your skin and then covered. During visits over the next few days, the doctor looks at your skin for signs of a reaction. Patch testing can help diagnose specific types of allergies causing your dermatitis.
Treatment
Treatment of atopic dermatitis may start with regular moisturizing and other self-care habits. If these don't help, your health care provider might suggest medicated creams that control itching and help repair skin. These are sometimes combined with other treatments.
Atopic dermatitis can be persistent. You may need to try various treatments over months or years to control it. And even if treatment is successful, symptoms may return (flare).
Medications
-
Medicated products applied to the skin. Many options are available to help control itching and repair the skin. Products are available in various strengths and as creams, gels and ointments. Talk with your health care provider about the options and your preferences. Whatever you use, apply it as directed (often twice a day), before you moisturize. Overuse of a corticosteroid product applied to the skin may cause side effects, such as thinning skin.
Creams or ointments with a calcineurin inhibitor might be a good option for those over age 2. Examples include tacrolimus (Protopic) and pimecrolimus (Elidel). Apply it as directed, before you moisturize. Avoid strong sunlight when using these products.
The Food and Drug Administration requires that these products have a black box warning about the risk of lymphoma. This warning is based on rare cases of lymphoma among people using topical calcineurin inhibitors. After 10 years of study, no causal relationship between these products and lymphoma and no increased risk of cancer have been found.
- Drugs to fight infection. Your health care provider may prescribe antibiotic pills to treat an infection.
- Pills that control inflammation. For more-severe eczema, your health care provider may prescribe pills to help control your symptoms. Options might include cyclosporine, methotrexate, prednisone, mycophenolate and azathioprine. These pills are effective but can't be used long term because of potential serious side effects.
- Other options for severe eczema. The injectable biologics (monoclonal antibodies) dupilumab (Dupixent) and tralokinumab (Adbry) might be options for people with moderate to severe disease who don't respond well to other treatment. Studies show that it's safe and effective in easing the symptoms of atopic dermatitis. Dupilumab is for people over age 6. Tralokinumab is for adults.
Therapies
- Wet dressings. An effective, intensive treatment for severe eczema involves applying a corticosteroid ointment and sealing in the medication with a wrap of wet gauze topped with a layer of dry gauze. Sometimes this is done in a hospital for people with widespread lesions because it's labor intensive and requires nursing expertise. Or ask your health care provider about learning how to use this technique at home safely.
-
Light therapy. This treatment is used for people who either don't get better with topical treatments or rapidly flare again after treatment. The simplest form of light therapy (phototherapy) involves exposing the affected area to controlled amounts of natural sunlight. Other forms use artificial ultraviolet A (UVA) and narrow band ultraviolet B (UVB) alone or with drugs.
Though effective, long-term light therapy has harmful effects, including premature skin aging, changes in skin color (hyperpigmentation) and an increased risk of skin cancer. For these reasons, phototherapy is less commonly used in young children and is not given to infants. Talk with your health care provider about the pros and cons of light therapy.
- Counseling. If you're embarrassed or frustrated by your skin condition, it can help to talk with a therapist or other counselor.
- Relaxation, behavior modification and biofeedback. These approaches may help people who scratch out of habit.
Baby eczema
Treatment for eczema in babies (infantile eczema) includes:
- Identifying and avoiding skin irritants
- Avoiding extreme temperatures
- Giving your baby a short bath in warm water and applying a cream or ointment while the skin is still damp
See your baby's health care provider if these steps don't improve the rash or it looks infected. Your baby might need a prescription medication to control the rash or treat an infection. Your health care provider might also recommend an oral antihistamine to help lessen the itch and cause drowsiness, which may be helpful for nighttime itching and discomfort. The type of antihistamine that causes drowsiness may negatively affect the school performance of some children.
Lifestyle and home remedies
Taking care of sensitive skin is the first step in treating atopic dermatitis and preventing flares. To help reduce itching and soothe inflamed skin, try these self-care measures:
- Moisturize your skin at least twice a day. Find a product or combination of products that works for you. You might try bath oils, creams, lotions, shea butter, ointments or sprays. For a child, the twice-a-day regimen might be an ointment before bedtime and a cream before school. Ointments are greasier and may sting less when applied. Choose products that are free of dyes, alcohols, fragrances and other ingredients that might irritate the skin. Allow the moisturizer to absorb into the skin before getting dressed.
- Apply an anti-itch cream to the affected area. A nonprescription cream containing at least 1% hydrocortisone can temporarily relieve the itch. Apply it no more than twice a day to the affected area before moisturizing. Once your reaction has improved, you may use this type of cream less often to prevent flares.
- Take an oral allergy or anti-itch medication. Options include nonprescription allergy medicines (antihistamines) — such as cetirizine (Zyrtec Allergy) or fexofenadine (Allegra Allergy). Also, diphenhydramine (Benadryl, others) may be helpful if itching is severe. But it causes drowsiness, so it's better for bedtime. The type of antihistamine that causes drowsiness may negatively affect the school performance of some children.
- Don't scratch. Rather than scratching when you itch, try pressing on or patting the skin. Cover the itchy area if you can't keep from scratching it. Keep your nails trimmed. For children, it might help to trim their nails and have them wear socks or gloves at night.
- Take a daily bath or shower. Use warm, rather than hot, water. If you're taking a bath, sprinkle the water with colloidal oatmeal, which is finely ground oatmeal made for bathing (Aveeno, others). Soak for less than 10 minutes, then pat dry. Apply moisturizer while the skin is still damp (within three minutes).
- Use a gentle, nonsoap cleanser. Choose one without dyes, alcohols or fragrances. Harsh soaps can wash away your skin's natural oils. Be sure to rinse off the cleanser completely.
-
Take a bleach bath. The American Academy of Dermatology recommends a bleach bath for relief from severe or frequent flares. Talk with your health care provider about whether this is a good option for you.
A diluted-bleach bath decreases bacteria on the skin and related infections. Add 1/2 cup (118 milliliters) of household bleach, not concentrated bleach, to a 40-gallon (151-liter) bathtub filled with warm water. Measurements are for a U.S.-standard-sized tub filled to the overflow drainage holes.
Soak from the neck down or just the affected areas for 5 to10 minutes. Don't put the head under water. Rinse off the bleach water with tap water. Take a bleach bath 2 to 3 times a week.
- Use a humidifier. Hot, dry indoor air can parch sensitive skin and worsen itching and flaking. A portable home humidifier or a humidifier attached to your furnace adds moisture to the air inside your home.
- Wear cool, smooth-textured clothing. Avoiding clothing that's rough, tight or scratchy. Also, in hot weather or while exercising, choose lightweight clothing that lets your skin breathe. When washing your clothing, avoid harsh detergents and fabric softeners added during the drying cycle.
- Treat stress and anxiety. Stress and other emotional disorders can worsen atopic dermatitis. Being aware of stress and anxiety and taking steps to improve your emotional health may help your skin too.
Alternative medicine
Many people with atopic dermatitis have tried alternative (integrative) medicine approaches to easing their symptoms. Some approaches are supported by clinical studies.
- Cannabinoids. When applied to skin, creams containing cannabinoids have been shown to ease itching and skin thickening. Several studies over more than 10 years showed some benefit.
- Natural oils. When added to bathwater, natural oils might help improve dry skin. Examples of such oils are soybean oil and mineral oil. Use caution with oils in a bathtub as they can make the tub slippery.
- Manuka honey. When applied to the skin, manuka honey has been shown to calm reactions on the skin. It has been used for centuries as an antimicrobial. Don't use in it on children under 1 year of age, as it carries the risk of infantile botulism.
- Acupuncture and acupressure. Several studies show that acupuncture and acupressure can reduce the itchiness of atopic dermatitis.
If you're considering alternative therapies, talk with your health care provider about their pros and cons.
Coping and support
Atopic dermatitis can make you feel uncomfortable and self-conscious. It can be especially stressful, frustrating or embarrassing for adolescents and young adults. It can disrupt their sleep and even lead to depression.
Some people may find it helpful to talk with a therapist or other counselor, a family member, or a friend. Or it can be helpful to find a support group for people with eczema, who know what it's like to live with the condition.
Preparing for an appointment
You're likely to start by seeing your primary care provider. Or you may see a doctor who specializes in the diagnosis and treatment of skin conditions (dermatologist) or allergies (allergist).
Here's some information to help you get ready for your appointment.
What you can do
- List your symptoms, when they occurred and how long they lasted. Also, it may help to list factors that triggered or worsened your symptoms — such as soaps or detergents, tobacco smoke, sweating, or long, hot showers.
- Make a list of all the medications, vitamins, supplements and herbs you're taking. Even better, take the original bottles and a list of the dosages and directions.
- List questions to ask your health care provider. Ask questions when you want something clarified.
For atopic dermatitis, some basic questions you might ask your health care provider include:
- What might be causing my symptoms?
- Are tests needed to confirm the diagnosis?
- What treatment do you recommend, if any?
- Is this condition temporary or chronic?
- Can I wait to see if the condition goes away on its own?
- What are the alternatives to the approach you're suggesting?
- What skin care routines do you recommend to improve my symptoms?
What to expect from your doctor
Your health care provider is likely to ask you a few questions. Being ready to answer them may free up time to go over any points you want to spend more time on. Your health care provider might ask:
- What are your symptoms and when did they start?
- Does anything seem to trigger your symptoms?
- Do you or any family members have allergies or asthma?
- Are you exposed to any possible irritants from your job or hobbies?
- Have you felt depressed or been under any unusual stress lately?
- Do you come in direct contact with pets or other animals?
- What products do you use on your skin, including soaps, lotions and cosmetics?
- What household cleaning products do you use?
- How much do your symptoms affect your quality of life, including your ability to sleep?
- What treatments have you tried so far? Has anything helped?
- How often do you shower or bathe?
Last Updated May 15, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



