Chronic sinusitis
Overview
Chronic sinusitis causes the spaces inside the nose and head, called sinuses, to become inflamed and swollen. The condition lasts 12 weeks or longer, even with treatment.
This common condition keeps mucus from draining. It makes the nose stuffy. Breathing through the nose might be hard. The area around the eyes might feel swollen or tender.
Infection, growths in the sinuses, called nasal polyps, and swelling of the lining of the sinuses might all be part of chronic sinusitis. Chronic sinusitis is also called chronic rhinosinusitis. The condition affects adults and children.
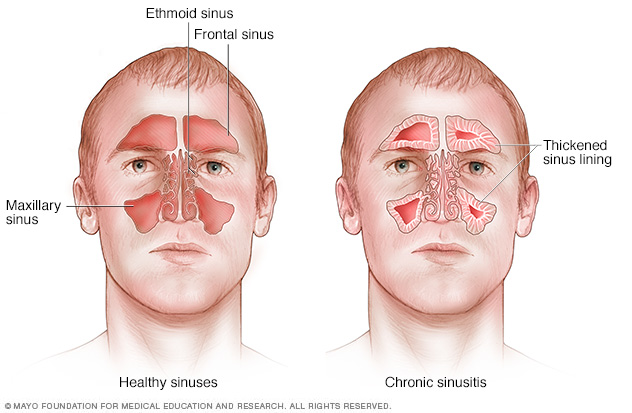
An infection, growths in the sinuses, called nasal polyps, or swelling of the lining of the sinuses can cause chronic sinusitis. Symptoms might include a blocked or stuffy nose that makes it hard to breathe through the nose and pain and swelling around the eyes, cheeks, nose or forehead.
Symptoms
Common symptoms of chronic sinusitis include:
- Thick, discolored mucus from the nose, known as a runny nose.
- Mucus down the back of the throat, known as postnasal drip.
- Blocked or stuffy nose, known as congestion. This makes it hard to breathe through the nose.
- Pain, tenderness and swelling around the eyes, cheeks, nose or forehead.
- Reduced sense of smell and taste.
Other symptoms can include:
- Ear pain.
- Headache.
- Aching in the teeth.
- Cough.
- Sore throat.
- Bad breath.
- Tiredness.
Chronic sinusitis and acute sinusitis have similar symptoms. But acute sinusitis is a short-lived infection of the sinuses often linked to a cold.
The symptoms of chronic sinusitis last at least 12 weeks. There might be many bouts of acute sinusitis before it becomes chronic sinusitis. Fever isn't common with chronic sinusitis. But fever might be part of acute sinusitis.
When to see a doctor
Schedule an appointment with your health care provider for:
- Repeated sinusitis, and if the condition doesn't get better with treatment.
- Sinusitis symptoms that last more than 10 days.
See a health care provider right away if you have symptoms that could mean a serious infection:
- Fever.
- Swelling or redness around the eyes.
- Bad headache.
- Forehead swelling.
- Confusion.
- Double vision or other vision changes.
- Stiff neck.
Causes
The cause of chronic sinusitis usually is not known. Some medical conditions, including cystic fibrosis, can cause chronic sinusitis in children and teens.
Some conditions can make chronic sinusitis worse. These include:
- A common cold or other infection that affects the sinuses. Viruses or bacteria can cause these infections.
- A problem inside the nose, such as a deviated nasal septum, nasal polyps or tumors.
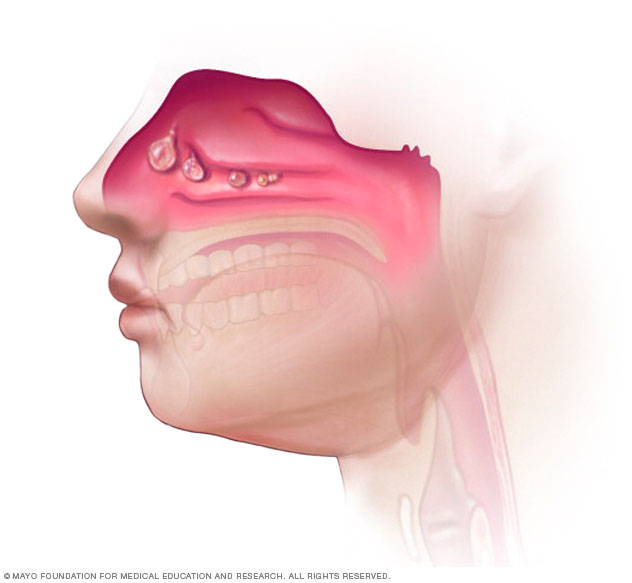
Nasal polyps are soft growths on the lining of the nose or the spaces inside the nose, known as sinuses. Nasal polyps aren't cancer. Nasal polyps often occur in groups, like grapes on a stem.
Risk factors
The following factors raise the risk of getting chronic sinusitis:
- A dental infection.
- A fungal infection.
- Regularly being around cigarette smoke or other pollutants.
Complications
Serious complications of chronic sinusitis are rare. They can include:
- Vision problems. If a sinus infection spreads to an eye socket, it can reduce vision or possibly cause blindness.
- Infections. It's not common. But a serious sinus infection can spread to the membranes and fluid around the brain and spinal cord. The infection is called meningitis. Other serious infections can spread to the bones, called osteomyelitis, or to skin, called cellulitis.
Prevention
Take these steps to lower the risk of getting chronic sinusitis:
- Protect your health. Try to stay away from people who have colds or other infections. Wash your hands often with soap and water, especially before meals.
- Manage allergies. Work with your health care provider to keep symptoms under control. Stay away from things you're allergic to when possible.
- Avoid cigarette smoke and polluted air. Tobacco smoke and other pollutants can irritate the lungs and inside the nose, called the nasal passages.
- Use a humidifier. If the air in your home is dry, adding moisture to the air with a humidifier may help prevent sinusitis. Be sure the humidifier stays clean and free of mold with regular, complete cleaning.
Diagnosis
A health care provider might ask about symptoms and do an exam. The exam might include feeling for tenderness in the nose and face and looking inside the nose.
Other ways to diagnose chronic sinusitis and rule out other conditions include:
- Nasal endoscopy. A health care provider inserts a thin, flexible tube, known as an endoscope, into the nose. A light on the tube allows a care provider to see inside the sinuses.
- Imaging tests. CT or MRI scans can show details of the sinuses and nasal area. These images might pinpoint the cause of chronic sinusitis.
- Nasal and sinus samples. Lab tests aren't often used to diagnose chronic sinusitis. But, if the condition doesn't get better with treatment or gets worse, tissue samples from the nose or sinuses might help find the cause.
- An allergy test. If allergies might be causing chronic sinusitis, an allergy skin test might show the cause.
Treatment
Treatments for chronic sinusitis include:
- Nasal corticosteroids. These nasal sprays help prevent and treat swelling. Some are available without a prescription. Examples include fluticasone (Flonase Allergy Relief, Xhance), budesonide (Rhinocort Allergy), mometasone (Nasonex 24HR Allergy) and beclomethasone (Beconase AQ, Qnasl, others).
- Saline nasal rinses. Use a specially designed squeeze bottle (NeilMed Sinus Rinse, others) or neti pot. This home remedy, called nasal lavage, can help clear sinuses. Saline nasal sprays also are available.
- Corticosteroids shots or pills. These medicines ease severe sinusitis, especially for those who have nasal polyps. The shots and pills can cause serious side effects when used long term. So they're used only to treat severe symptoms.
- Allergy medicines. Using allergy medicines might lessen allergy symptoms of sinusitis caused by allergies.
- Aspirin desensitization treatment. This is for people who react to aspirin and the reaction causes sinusitis and nasal polyps. Under medical supervision, people receive larger and larger doses of aspirin to increase their ability to take it.
- Medicine to treat nasal polyps and chronic sinusitis. If you have nasal polyps and chronic sinusitis, a shot of dupilumab (Dupixent), omalizumab (Xolair) or mepolizumab (Nucala) might reduce the size of the nasal polyps and lessen stuffiness.
Antibiotics
Antibiotics are sometimes needed to treat sinusitis caused by bacteria. A possible bacterial infection might need to be treated with an antibiotic and sometimes with other medicines.
Immunotherapy
For sinusitis caused or made worse by allergies, allergy shots might help. This is known as immunotherapy.
Surgery
For chronic sinusitis that doesn't clear up with treatment, endoscopic sinus surgery might be an option. In this procedure, a health care provider uses a thin, flexible tube with an attached light, called an endoscope, and tiny cutting tools to remove the tissue that's causing the problem.
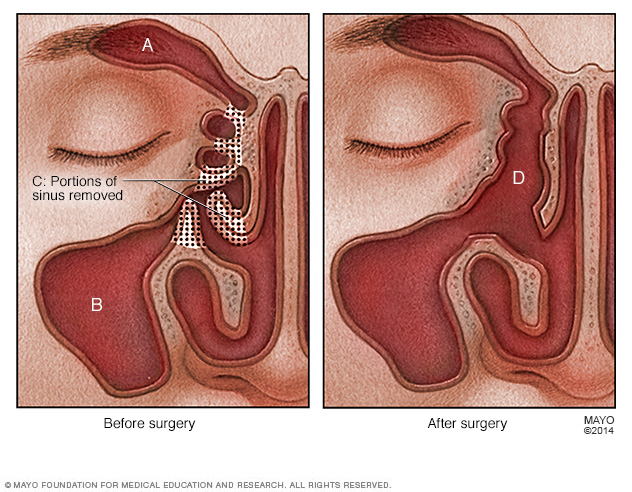
The left picture shows the frontal (A) and maxillary (B) sinuses. It also shows the channel between the sinuses, also known as the ostiomeatal complex (C). The right picture shows the results of endoscopic sinus surgery. A surgeon uses a lighted tube and tiny cutting tools to open the blocked passage and let the sinuses drain. (D).
Lifestyle and home remedies
These self-help steps can help ease sinusitis symptoms:
- Rest. Rest helps the body fight infection and speed recovery.
- Drink fluids. Keep drinking plenty of fluids.
- Use a warm compress. A warm compress on the nose and forehead might help ease pressure in the sinuses.
- Keep sinuses moist. Put a towel over your head while breathing in the vapor from a bowl of hot water. Or take a hot shower, breathing in the warm, moist air. This will help ease pain and help mucus drain.

A neti pot is a container designed to rinse the nasal cavity.
Preparing for an appointment
You'll likely see your primary care provider for symptoms of sinusitis. If you've had many bouts of acute sinusitis or you have symptoms of chronic sinusitis, your provider might refer you to an allergist or an ear, nose and throat specialist.
Here's information to help you get ready for your appointment.
What you can do
Make a list of:
- Your symptoms, including any that seem unrelated to the reason for your appointment, and when they began.
- Key personal information, including whether you have allergies or asthma, and family medical history.
- All medicines, vitamins or other supplements you take, including doses.
- Questions to ask your health care provider.
For chronic sinusitis, questions to ask your provider include:
- What's the most likely cause of my symptoms?
- What tests do I need?
- Is my condition likely to go away or be long lasting?
- What treatments do you suggest for me?
- I have these other health conditions. How can I best manage these conditions together?
- Should I see a specialist?
- Are there brochures or other printed material I can have? What websites do you suggest?
Be sure to ask all the questions you have.
What to expect from your doctor
Your care provider is likely to ask you questions, such as:
- Do you have symptoms all the time or sometimes?
- How bad are your symptoms?
- What, if anything, seems to make your symptoms better?
- What, if anything, appears to make your symptoms worse?
- Do you smoke or are you around smoke or other pollutants?
Last Updated Sep 19, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use