Croup
Overview
Croup refers to an infection of the upper airway, which becomes narrow, making it harder to breathe. Croup also causes a cough that sounds like barking.
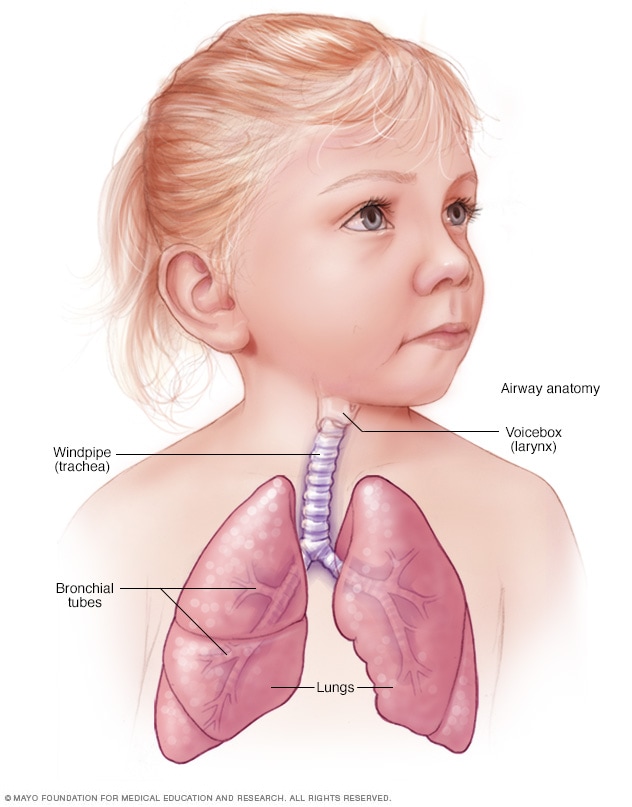
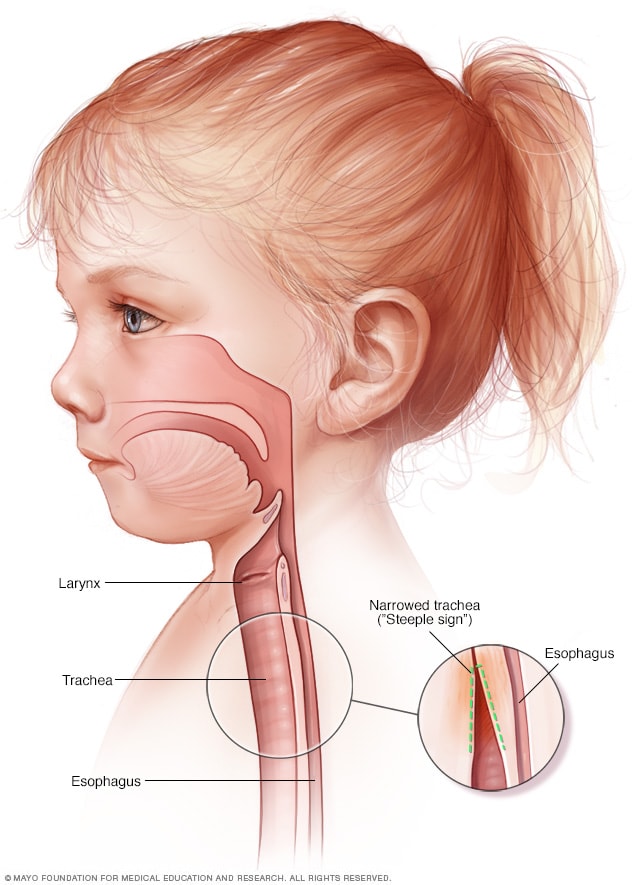
The cough and other signs and symptoms of croup are the result of swelling and irritation around the voice box (larynx), windpipe (trachea) and bronchial tubes (bronchi). When a cough forces air through this narrowed passageway, the swollen vocal cords produce a noise like a seal barking. Taking a breath often produces a high-pitched whistling sound called stridor.
Croup most often occurs in younger children. It usually isn't serious. Most children can be treated for croup at home.
Symptoms
Croup often begins as an ordinary cold. If there's enough swelling, irritation and coughing, a child can develop:
- Loud barking cough that's made worse by crying and coughing, as well as anxiety and distress, setting up a cycle of worsening symptoms.
- Fever.
- Hoarse voice.
- Noisy or labored breathing.
Symptoms of croup are often worse at night and usually last for 3 to 5 days.
When to see a doctor
Contact your child's health care provider if symptoms are severe, worsen, last longer than 3 to 5 days or aren't responding to home treatment.
Seek immediate medical attention if your child:
- Makes noisy, high-pitched breathing sounds when breathing both in and out.
- Makes high-pitched breathing sounds when not crying or upset.
- Begins drooling or has problems swallowing.
- Seems anxious, upset and restless or extra tired and has no energy.
- Breathes at a faster rate than usual.
- Struggles to breathe.
- Develops a blue or gray tint around the nose, in or around the mouth, or on the fingernails.
Causes
Croup is usually caused by a viral infection, most often a parainfluenza virus.
Your child may get a virus by breathing infected respiratory droplets coughed or sneezed into the air. Virus particles in these droplets may also survive on toys and other surfaces. If your child touches a surface with a virus on it, and then touches the eyes, nose or mouth, an infection may follow.
Risk factors
Children between 6 months and 3 years of age have the highest risk of getting croup. Because children have small airways, they're likely to have more symptoms with croup. Croup rarely occurs in children older than 6 years of age.
Complications
Most cases of croup are mild. In a small number of children, the airway swells enough to cause problems with breathing. Rarely, a bacterial infection of the windpipe can occur in addition to the viral infection. This can result in trouble breathing and requires emergency medical care.
Only a small number of children seen in the emergency room for croup require a stay in the hospital.
Prevention
To prevent croup, take the same steps you use to prevent colds and flu.
- Frequent hand-washing with soap and water for at least 20 seconds is the most important step.
- Keep your child away from anyone who's sick.
- Encourage your child to cough or sneeze into the elbow.
- Clean frequently touched surfaces.
To prevent more-serious infections that may cause croup, keep your child's vaccinations up to date. The diphtheria and Haemophilus influenzae type b (Hib) vaccines offer protection from some of the rarest — but most dangerous — upper airway infections. There isn't a vaccine yet that protects against parainfluenza viruses.
Diagnosis
Croup is usually diagnosed by a health care provider. The provider:
- Observes your child's breathing.
- Listens to your child's chest with a stethoscope.
- Examines your child's throat.
Sometimes X-rays or other tests are used to rule out other possible illnesses.
Treatment
Most children with croup can be treated at home. Still, croup can be scary, especially if your child needs a visit to the health care provider's office, emergency room or hospital. Treatment is usually based on how severe the symptoms are.
Comfort measures
It's important to comfort and calm your child because crying and distress can worsen airway swelling, making it harder to breathe. Hold your child, sing lullabies or read quiet stories. Offer a favorite blanket or toy. Speak in a soothing voice.
Also, make sure that your child drinks plenty of fluids to stay hydrated.
Medicines
Your child's health care provider may prescribe these medicines:
- Corticosteroid. A corticosteroid — such as dexamethasone — may be given to reduce swelling in the airway. Symptoms will usually start to improve within a few hours. Your child may take pills over several days. Or your child may get a single dose of dexamethasone as a shot because of its long-lasting effects.
- Epinephrine. Epinephrine is effective in reducing airway swelling with more-severe symptoms. The medicine may be given in an inhaled form using a nebulizer. It's fast acting, but its effects wear off quickly. Your child likely will need to be observed in the emergency room for several hours to see if a second dose is needed before going home.
A stay in the hospital
For severe croup, your child may need to spend time in a hospital to be monitored and receive more treatments.
Self care
Croup often runs its course within 3 to 5 days. In the meantime, keep your child comfortable with a few simple measures:
- Stay calm. Comfort or distract your child — cuddle, read a book or play a quiet game. Crying makes breathing more difficult.
- Provide humidified or cool air. Although there's no evidence of benefit from these practices, many parents believe that humid air or cool air helps a child's breathing. For moist air, you can use a humidifier. You can also sit with the child in a bathroom filled with steam created by running hot water from the shower. If it's cool outside, you can open a window for your child to breathe the cool air.
- Hold your child in a comfortable upright position. Hold your child on your lap, or place your child in a favorite chair or infant seat. Sitting upright may make breathing easier.
- Offer fluids. For babies, breast milk or formula is fine. For older children, soup or frozen fruit pops may be soothing.
- Encourage rest. Sleep can help your child fight the infection.
-
Try a fever reducer. For treatment of fever or pain, consider giving your child infants' or children's over-the-counter fever and pain medicines such as acetaminophen (Tylenol, others) or ibuprofen (Advil, Motrin, others) as a safer alternative to aspirin. Read the directions carefully for dosing. Ask your health care provider about the right dose if you're not sure.
Use caution when giving aspirin to children or teenagers. Though aspirin is approved for use in children older than age 3, children and teenagers recovering from chickenpox or flu-like symptoms should never take aspirin. This is because aspirin has been linked to Reye's syndrome, a rare but potentially life-threatening condition, in such children.
- Skip the cold medicines. Cold preparations available without a prescription aren't recommended for children of any age. And they can be harmful in children under than 2 years old. Plus, nonprescription cough medicines won't help croup.
Your child's cough may improve during the day, but don't be surprised if it returns at night. You may want to sleep near your child or even in the same room so that you can take quick action if symptoms worsen.
Preparing for your appointment
In most cases of croup, your child won't need to see a health care provider. However, if symptoms are severe or aren't responding to home treatment, you should call your provider.
What you can do
Before your appointment, make a list of:
- Your child's symptoms, including how long they have been occurring and what, if anything, makes them better or worse.
- Any medicine your child is taking, including over-the-counter medicines, vitamins, herbs and other supplements, and their doses.
- Questions to ask your child's health care provider.
What to expect from your doctor
Your child's health care provider will likely ask a number of questions to help determine the best course of treatment:
- What are your child's symptoms?
- Has your child had a fever or difficulty swallowing?
- How long has your child been experiencing symptoms?
- Has your child's cough become worse over time? If so, how rapidly?
- Have you noticed a pattern to your child's cough? For instance, does it get worse at night?
- Has your child had croup in the past?
- Has your child recently been exposed to other sick children?
- Does your child have any other medical conditions?
- Are your child's vaccinations up to date?
Your health care provider will ask other questions based on your answers and your child's symptoms and needs. Preparing and anticipating questions will help you make the most of your time with the provider.
Last Updated Dec 3, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use