Cystic fibrosis
Overview
Cystic fibrosis (CF) is an inherited disorder that causes severe damage to the lungs, digestive system and other organs in the body.
Cystic fibrosis affects the cells that produce mucus, sweat and digestive juices. These secreted fluids are normally thin and slippery. But in people with CF, a defective gene causes the secretions to become sticky and thick. Instead of acting as lubricants, the secretions plug up tubes, ducts and passageways, especially in the lungs and pancreas.
Although cystic fibrosis is progressive and requires daily care, people with CF are usually able to attend school and work. They often have a better quality of life than people with CF had in previous decades. Improvements in screening and treatments mean that people with CF now may live into their mid- to late 30s or 40s, and some are living into their 50s.
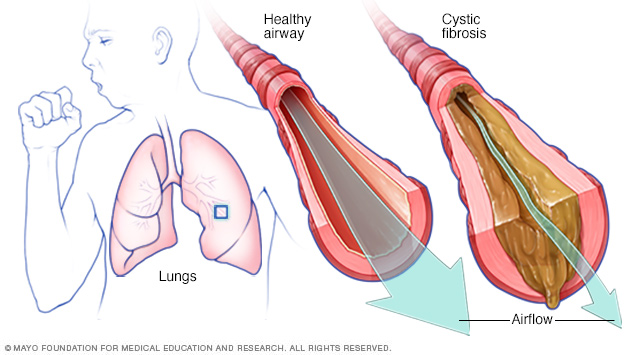
In cystic fibrosis, the airways fill with thick, sticky mucus, making it difficult to breathe. The thick mucus is also an ideal breeding ground for bacteria and fungi.
Symptoms
In the U.S., because of newborn screening, cystic fibrosis can be diagnosed within the first month of life, before symptoms develop. But people born before newborn screening became available may not be diagnosed until the signs and symptoms of CF show up.
Cystic fibrosis signs and symptoms vary, depending on the severity of the disease. Even in the same person, symptoms may worsen or improve as time passes. Some people may not experience symptoms until their teenage years or adulthood. People who are not diagnosed until adulthood usually have milder disease and are more likely to have atypical symptoms, such as recurring bouts of an inflamed pancreas (pancreatitis), infertility and recurring pneumonia.
People with cystic fibrosis have a higher than normal level of salt in their sweat. Parents often can taste the salt when they kiss their children. Most of the other signs and symptoms of CF affect the respiratory system and digestive system.
Respiratory signs and symptoms
The thick and sticky mucus associated with cystic fibrosis clogs the tubes that carry air in and out of your lungs. This can cause signs and symptoms such as:
- A persistent cough that produces thick mucus (sputum)
- Wheezing
- Exercise intolerance
- Repeated lung infections
- Inflamed nasal passages or a stuffy nose
- Recurrent sinusitis
Digestive signs and symptoms
The thick mucus can also block tubes that carry digestive enzymes from your pancreas to your small intestine. Without these digestive enzymes, your intestines aren't able to completely absorb the nutrients in the food you eat. The result is often:
- Foul-smelling, greasy stools
- Poor weight gain and growth
- Intestinal blockage, particularly in newborns (meconium ileus)
- Chronic or severe constipation, which may include frequent straining while trying to pass stool, eventually causing part of the rectum to protrude outside the anus (rectal prolapse)
When to see a doctor
If you or your child has symptoms of cystic fibrosis — or if someone in your family has CF — talk with your doctor about testing for the disease. Consult a physician who is knowledgeable about CF.
Cystic fibrosis requires consistent, regular follow-up with your doctor, at least every three months. Contact you doctor if you experience new or worsening symptoms, such as more mucus than usual or a change in the mucus color, lack of energy, weight loss, or severe constipation.
Seek immediate medical care if you're coughing up blood, have chest pain or difficulty breathing, or have severe stomach pain and distention.
Causes
In cystic fibrosis, a defect (mutation) in a gene — the cystic fibrosis transmembrane conductance regulator (CFTR) gene — changes a protein that regulates the movement of salt in and out of cells. The result is thick, sticky mucus in the respiratory, digestive and reproductive systems, as well as increased salt in sweat.
Many different defects can occur in the gene. The type of gene mutation is associated with the severity of the condition.
Children need to inherit one copy of the gene from each parent in order to have the disease. If children inherit only one copy, they won't develop cystic fibrosis. However, they will be carriers and could pass the gene to their own children.
Risk factors
Because cystic fibrosis is an inherited disorder, it runs in families, so family history is a risk factor. Although CF occurs in all races, it's most common in white people of Northern European ancestry.
Complications
Complications of cystic fibrosis can affect the respiratory, digestive and reproductive systems, as well as other organs.
Respiratory system complications
- Damaged airways (bronchiectasis). Cystic fibrosis is one of the leading causes of bronchiectasis, a chronic lung condition with abnormal widening and scarring of the airways (bronchial tubes). This makes it harder to move air in and out of the lungs and clear mucus from the bronchial tubes.
- Chronic infections. Thick mucus in the lungs and sinuses provides an ideal breeding ground for bacteria and fungi. People with cystic fibrosis may often have sinus infections, bronchitis or pneumonia. Infection with bacteria that is resistant to antibiotics and difficult to treat is common.
- Growths in the nose (nasal polyps). Because the lining inside the nose is inflamed and swollen, it can develop soft, fleshy growths (polyps).
- Coughing up blood (hemoptysis). Bronchiectasis can occur next to blood vessels in the lungs. The combination of airway damage and infection can result in coughing up blood. Often this is only a small amount of blood, but it can also be life-threatening.
- Pneumothorax. In this condition, air leaks into the space that separates the lungs from the chest wall, and part or all of a lung collapses. This is more common in adults with cystic fibrosis. Pneumothorax can cause sudden chest pain and breathlessness. People often feel a bubbling sensation in the chest.
- Respiratory failure. Over time, cystic fibrosis can damage lung tissue so badly that it no longer works. Lung function usually worsens gradually, and it eventually can become life-threatening. Respiratory failure is the most common cause of death.
- Acute exacerbations. People with cystic fibrosis may experience worsening of their respiratory symptoms, such as coughing with more mucus and shortness of breath. This is called an acute exacerbation and requires treatment with antibiotics. Sometimes treatment can be provided at home, but hospitalization may be needed. Decreased energy and weight loss also are common during exacerbations.
Digestive system complications
- Nutritional deficiencies. Thick mucus can block the tubes that carry digestive enzymes from your pancreas to your intestines. Without these enzymes, your body can't absorb protein, fats or fat-soluble vitamins, so you can't get enough nutrients. This can result in delayed growth, weight loss or inflammation of the pancreas.
- Diabetes. The pancreas produces insulin, which your body needs to use sugar. Cystic fibrosis increases the risk of diabetes. About 20% of teenagers and 40% to 50% of adults with CF develop diabetes.
- Liver disease. The tube that carries bile from your liver and gallbladder to your small intestine may become blocked and inflamed. This can lead to liver problems, such as jaundice, fatty liver disease and cirrhosis — and sometimes gallstones.
- Intestinal obstruction. Intestinal blockage can happen to people with cystic fibrosis at all ages. Intussusception, a condition in which a segment of the intestine slides inside an adjacent section of the intestine like a collapsible telescope, also can occur.
- Distal intestinal obstruction syndrome (DIOS). DIOS is partial or complete obstruction where the small intestine meets the large intestine. DIOS requires urgent treatment.
Reproductive system complications
- Infertility in men. Almost all men with cystic fibrosis are infertile because the tube that connects the testes and prostate gland (vas deferens) is either blocked with mucus or missing entirely. Certain fertility treatments and surgical procedures sometimes make it possible for men with CF to become biological fathers.
- Reduced fertility in women. Although women with cystic fibrosis may be less fertile than other women, it's possible for them to conceive and to have successful pregnancies. Still, pregnancy can worsen the signs and symptoms of CF, so be sure to discuss the possible risks with your doctor.
Other complications
- Thinning of the bones (osteoporosis). People with cystic fibrosis are at higher risk of developing a dangerous thinning of bones. They may also experience joint pain, arthritis and muscle pain.
- Electrolyte imbalances and dehydration. Because people with cystic fibrosis have saltier sweat, the balance of minerals in their blood may be upset. This makes them prone to dehydration, especially with exercise or in hot weather. Signs and symptoms include increased heart rate, fatigue, weakness and low blood pressure.
- Mental health problems. Dealing with a chronic illness that has no cure may cause fear, depression and anxiety.
Prevention
If you or your partner has close relatives with cystic fibrosis, you both may choose to have genetic testing before having children. The test, which is performed in a lab on a sample of blood, can help determine your risk of having a child with CF.
If you're already pregnant and the genetic test shows that your baby may be at risk of cystic fibrosis, your doctor can conduct additional tests on your developing child.
Genetic testing isn't for everyone. Before you decide to be tested, you should talk to a genetic counselor about the psychological impact the test results might carry.
Diagnosis
To diagnose cystic fibrosis, doctors typically do a physical exam, review your symptoms and conduct several tests.
Newborn screening and diagnosis
Every state in the U.S. now routinely screens newborns for cystic fibrosis. Early diagnosis means that treatment can begin immediately.
In one screening test, a blood sample is checked for higher than normal levels of a chemical called immunoreactive trypsinogen (IRT), which is released by the pancreas. A newborn's IRT levels may be high because of premature birth or a stressful delivery. For that reason, other tests may be needed to confirm a diagnosis of cystic fibrosis.
To evaluate if an infant has cystic fibrosis, doctors may also conduct a sweat test once the infant is at least 2 weeks old. A sweat-producing chemical is applied to a small area of skin. Then the sweat is collected to test it and see if it's saltier than normal. Testing done at a care center accredited by the Cystic Fibrosis Foundation helps ensure reliable results.
Doctors may also recommend genetic tests for specific defects on the gene responsible for cystic fibrosis. Genetic tests may be used in addition to checking the IRT levels to confirm the diagnosis.
Testing of older children and adults
Cystic fibrosis tests may be recommended for older children and adults who weren't screened at birth. Your doctor may suggest genetic and sweat tests for CF if you have recurring bouts of an inflamed pancreas, nasal polyps, chronic sinus or lung infections, bronchiectasis, or male infertility.
Treatment
There is no cure for cystic fibrosis, but treatment can ease symptoms, reduce complications and improve quality of life. Close monitoring and early, aggressive intervention is recommended to slow the progression of CF, which can lead to a longer life.
Managing cystic fibrosis is complex, so consider getting treatment at a center with a multispecialty team of doctors and medical professionals trained in CF to evaluate and treat your condition.
The goals of treatment include:
- Preventing and controlling infections that occur in the lungs
- Removing and loosening mucus from the lungs
- Treating and preventing intestinal blockage
- Providing adequate nutrition
Medications
Options include:
- Medications that target gene mutations, including a new medication that combines three drugs to treat the most common genetic mutation causing CF and is considered a major achievement in treatment
- Antibiotics to treat and prevent lung infections
- Anti-inflammatory medications to lessen swelling in the airways in your lungs
- Mucus-thinning drugs, such as hypertonic saline, to help you cough up the mucus, which can improve lung function
- Inhaled medications called bronchodilators that can help keep your airways open by relaxing the muscles around your bronchial tubes
- Oral pancreatic enzymes to help your digestive tract absorb nutrients
- Stool softeners to prevent constipation or bowel obstruction
- Acid-reducing medications to help pancreatic enzymes work better
- Specific drugs for diabetes or liver disease, when appropriate
Medications that target genes
For those with cystic fibrosis who have certain gene mutations, doctors may recommend cystic fibrosis transmembrane conductance regulator (CFTR) modulators. These newer medications help improve the function of the faulty CFTR protein. They may improve lung function and weight, and reduce the amount of salt in sweat.
The FDA has approved these medications for treating CF in people with one or more mutations in the CFTR gene:
- The newest combination medication containing elexacaftor, ivacaftor and tezacaftor (Trikafta) is approved for people age 12 years and older and considered a breakthrough by many experts.
- The combination medication containing tezacaftor and ivacaftor (Symdeko) is approved for people age 6 years and older.
- The combination medication containing lumacaftor and ivacaftor (Orkambi) is approved for people who are age 2 years and older.
- Ivacaftor (Kalydeco) has been approved for people who are 6 months and older.
Doctors may conduct liver function tests and eye exams before prescribing these medications. While taking these drugs, testing on a regular basis is needed to check for side effects such as liver function abnormalities and cataracts. Ask your doctor and pharmacist for information on possible side effects and what to watch for.
Keep regular follow-up appointments so your doctor can monitor you while taking these medications. Talk to your doctor about any side effects that you experience.
Airway clearance techniques
Airway clearance techniques — also called chest physical therapy (CPT) — can relieve mucus obstruction and help to reduce infection and inflammation in the airways. These techniques loosen the thick mucus in the lungs, making it easier to cough up.
Airway clearing techniques are usually done several times a day. Different types of CPT can be used to loosen and remove mucus, and a combination of techniques may be recommended.
- A common technique is clapping with cupped hands on the front and back of the chest.
- Certain breathing and coughing techniques also may be used to help loosen the mucus.
- Mechanical devices can help loosen lung mucus. Devices include a tube that you blow into and a machine that pulses air into the lungs (vibrating vest). Vigorous exercise also may be used to clear mucus.
Your doctor will instruct you on the type and frequency of chest physical therapy that's best for you.
Pulmonary rehabilitation
Your doctor may recommend a long-term program that may improve your lung function and overall well-being. Pulmonary rehabilitation is usually done on an outpatient basis and may include:
- Physical exercise that may improve your condition
- Breathing techniques that may help loosen mucus and improve breathing
- Nutritional counseling
- Counseling and support
- Education about your condition
Surgical and other procedures
Options for certain conditions caused by cystic fibrosis include:
- Nasal and sinus surgery. Your doctor may recommend surgery to remove nasal polyps that obstruct breathing. Sinus surgery may be done to treat recurrent or chronic sinusitis.
- Oxygen therapy. If your blood oxygen level declines, your doctor may recommend that you breathe pure oxygen to prevent high blood pressure in the lungs (pulmonary hypertension).
- Noninvasive ventilation. Typically used while sleeping, noninvasive ventilation uses a nose or mouth mask to provide positive pressure in the airway and lungs when you breathe in. It's often used in combination with oxygen therapy. Noninvasive ventilation can increase air exchange in the lungs and decrease the work of breathing. The treatment may also help with airway clearance.
- Feeding tube. Cystic fibrosis interferes with digestion, so you can't absorb nutrients from food very well. Your doctor may suggest using a feeding tube to deliver extra nutrition. This tube may be a temporary tube inserted into your nose and guided to your stomach, or the tube may be surgically implanted in the abdomen. The tube can be used to give extra calories during the day or night and does not prevent eating by mouth.
- Bowel surgery. If a blockage develops in your bowel, you may need surgery to remove it. Intussusception, where a segment of intestine has telescoped inside an adjacent section of intestine, also may require surgical repair.
-
Lung transplant. If you have severe breathing problems, life-threatening lung complications or increasing resistance to antibiotics for lung infections, lung transplantation may be an option. Because bacteria line the airways in diseases that cause permanent widening of the large airways (bronchiectasis), such as cystic fibrosis, both lungs need to be replaced.
Cystic fibrosis does not recur in transplanted lungs. However, other complications associated with CF — such as sinus infections, diabetes, pancreas conditions and osteoporosis — can still occur after a lung transplant.
- Liver transplant. For severe cystic fibrosis-related liver disease, such as cirrhosis, liver transplant may be an option. In some people, a liver transplant may be combined with lung or pancreas transplants.
Lifestyle and home remedies
You can manage your condition and minimize complications in several ways.
Prevention
Pay attention to nutrition and fluid intake
Cystic fibrosis can cause malnourishment because the enzymes needed for digestion can't reach your small intestine, preventing food from being absorbed. People with CF may need a much higher number of calories daily than do people without the condition.
A healthy diet is important to growth and development and to maintain good lung function. It's also important to drink lots of fluids, which can help thin the mucus in your lungs. You may work with a dietitian to develop a nutrition plan.
Your doctor may recommend:
- Pancreatic enzyme capsules with every meal and snack
- Medications to suppress acid production
- Supplemental high-calorie nutrition
- Special fat-soluble vitamins
- Extra fiber to prevent intestinal blockage
- Extra salt, especially during hot weather or before exercising
- Adequate water intake, especially during hot weather
Keep vaccinations up to date
In addition to receiving other usual childhood vaccines, people with cystic fibrosis should have the annual flu vaccine and any other vaccines their doctors recommend, such as the vaccine to prevent pneumonia. CF doesn't affect the immune system, but children with CF are more likely to develop complications when they become sick.
Exercise
Regular exercise helps loosen mucus in your airways and strengthens your heart. Because people with cystic fibrosis are living longer, maintaining good cardiovascular fitness for a healthy life is important. Anything that gets you moving, including walking and biking, can help.
Eliminate smoke
Don't smoke, and don't allow other people to smoke around you or your child. Secondhand smoke is harmful for everyone, but especially for people with cystic fibrosis, as is air pollution.
Encourage hand-washing
Teach all the members of your family to wash their hands thoroughly before eating, after using the bathroom, when coming home from work or school, and after being around a person who is sick. Hand-washing is the best way to protect against infection.
Attend medical appointments
You'll have ongoing care from your doctor and other medical professionals.
- Make sure to attend your regular follow-up appointments.
- Take your medications as prescribed and follow therapies as instructed.
- Talk to your doctor about how to manage symptoms and the warning signs of serious complications.
Coping and support
If you or someone you love has cystic fibrosis, you may experience strong emotions such as depression, anxiety, anger or fear. These issues may be especially common in teens. These tips may help.
- Find support. Talking openly about how you feel can help. It also may help to talk with others who are dealing with the same issues. That might mean joining a support group for yourself, or finding a support group for parents of children with cystic fibrosis. Older children with CF may want to join a CF group to meet and talk with others who have the disorder.
- Seek professional help. If you or your child is depressed or anxious, it may help to meet with a mental health professional. He or she can talk with you about feelings and coping strategies, and may suggest medications or other treatments as well.
- Spend time with friends and family. Having their support can help you manage stress and reduce anxiety. Ask your friends or family for help if you need it.
- Take time to learn about cystic fibrosis. If your child has cystic fibrosis, encourage him or her to learn about CF. Find out how medical care is managed for children with CF as they grow older and reach adulthood. Talk with your doctor if you have questions about care.
Preparing for an appointment
Make an appointment with your doctor if you or your child has signs or symptoms common to cystic fibrosis. After the initial evaluation, you may be referred to a doctor trained in evaluating and treating CF.
Here's some information to help you prepare for your appointment, as well as what to expect from your doctor.
What you can do
You may want to prepare answers to these questions:
- What symptoms are you or your child experiencing?
- When did the symptoms start?
- Does anything make the symptoms better or worse?
- Has anyone in your family ever had cystic fibrosis?
- Has growth been normal and weight been stable?
What to expect from your doctor
After getting detailed information about the symptoms and your family's medical history, your doctor may order tests to help with diagnosis and plan treatment.
Last Updated Nov 23, 2021
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use