Dermatitis
Overview
Dermatitis is a common condition that causes swelling and irritation of the skin. It has many causes and forms and often involves itchy, dry skin or a rash. Or it might cause the skin to blister, ooze, crust or flake. Three common types of this condition are atopic dermatitis, contact dermatitis and seborrheic dermatitis. Atopic dermatitis is also known as eczema.
Dermatitis isn't contagious, but it can be very uncomfortable. Moisturizing regularly helps control the symptoms. Treatment also may include medicated ointments, creams and shampoos.
Symptoms
Each type of dermatitis tends to occur on a different part of the body. Symptoms may include:
- Itchiness that can be painful.
- Dry, cracked, scaly skin, more typical on white skin.
- Rash on swollen skin that varies in color depending on skin color.
- Blisters, perhaps with oozing and crusting.
- Dandruff.
- Thickened skin.
- Small, raised bumps, more typical on brown or Black skin.
When to see a doctor
See your doctor if:
- You're so uncomfortable that the condition is affecting sleep and daily activities.
- Your skin is painful.
- You have a skin infection — look for new streaks, pus, yellow scabs.
- You have symptoms even after trying self-care steps.
Seek immediate medical attention if you have a fever and the rash looks infected.
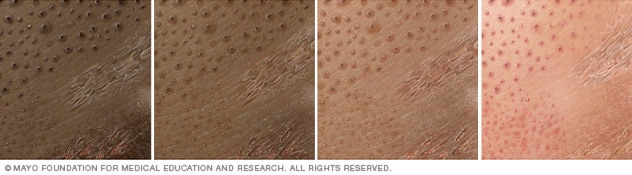
Illustration of contact dermatitis on different skin colors. Contact dermatitis can appear as an itchy rash.
Causes
A common cause of dermatitis is contact with something that irritates your skin or triggers an allergic reaction. Examples of such things are poison ivy, perfume, lotion and jewelry containing nickel. Other causes of dermatitis include dry skin, a viral infection, bacteria, stress, genetic makeup and a problem with the immune system.
Risk factors
Common risk factors for dermatitis include:
- Age. Dermatitis can occur at any age, but atopic dermatitis is more common in children than adults. It often begins in infancy.
- Allergies, atopic dermatitis and asthma. People who have a personal or family history of atopic dermatitis, allergies, hay fever or asthma are more likely to develop atopic dermatitis.
- Occupation. Jobs that put you in contact with certain metals, solvents or cleaning supplies increase your risk of contact dermatitis. Being a health care worker is linked to hand eczema.
- Other health conditions. Health conditions that put you at increased risk of seborrheic dermatitis include Parkinson's disease, immunodeficiency and HIV/AIDS.
Complications
Repeated scratching that breaks the skin can cause open sores and cracks. These increase the risk of infection from bacteria and fungi. These skin infections can spread and become life-threatening, though this is rare.
In people with brown and Black skin, dermatitis might cause the affected skin to darken or lighten. These conditions are called post-inflammatory hyperpigmentation and post-inflammatory hypopigmentation. It might take months or years for the skin to return to its usual color.
Prevention
Wear protective clothing if you're doing a task that involves irritants or caustic chemicals.
Developing a basic skin care routine also may help prevent dermatitis. The following habits can help reduce the drying effects of bathing:
- Take shorter baths and showers. Limit your bath or shower to about 10 minutes. Use lukewarm, not hot, water. Bath oil also may be helpful.
- Use a mild soap or a soapless cleanser. Choose a cleanser that has no dyes, alcohols and fragrance. Some soaps can dry the skin. For young children, you usually need only warm water to get them clean — no soap or bubble bath needed. Don't scrub the skin with a washcloth or loofah.
- Pat dry. After bathing, gently pat the skin with a soft towel. Avoid aggressive rubbing.
-
Moisturize all the skin. While the skin is still damp, seal in moisture with an oil, cream or lotion. Moisturize throughout the day as needed.
Many moisturizers are sold. Try different products to find one that works for you. The ideal moisturizer is safe, unscented, effective, affordable and one that you like to use regularly. Examples include Vanicream, Eucerin, CeraVe and Cetaphil.
Diagnosis
To diagnose dermatitis, your doctor will likely look at your skin and talk with you about your symptoms and medical history. You may need to have a small piece of skin removed for study in a lab, which helps rule out other conditions. This procedure is called a skin biopsy.
Patch testing
Your doctor may suggest a patch test to identify the cause of your symptoms. In this test, small amounts of potential allergens are put on sticky patches. Then the patches are placed on your skin. They stay on your skin for 2 to 3 days. During this time, you'll need to keep your back dry. Then your health care provider checks for skin reactions under the patches and determines whether further testing is needed.
Treatment
The treatment for dermatitis varies, depending on the cause and your symptoms. If home care steps don't ease your symptoms, your doctor may prescribe medicine. Possible treatments include:
- Applying to the rash a prescription-strength corticosteroid cream, gel or ointment.
- Applying to the rash a cream or ointment with a calcineurin inhibitor. This is a medicine that affects the immune system. You'll need a prescription from your doctor for it.
- Exposing the rash to controlled amounts of natural or artificial light. This method is called light therapy or phototherapy.
- Using prescription-strength pills or injected medicine, for more-severe disease. Examples are oral corticosteroids or an injectable biologic called dupilumab.
- Using wet dressings, a medical treatment for severe atopic dermatitis. It involves applying a corticosteroid ointment, wrapping it with wet bandages and topping that with a layer of dry gauze.
Lifestyle and home remedies
These self-care habits can help you manage dermatitis and feel better:
- Apply an anti-itch cream or ointment. Try 1% hydrocortisone cream or ointment (Cortizone 10, others). This is a product you can buy at a store without a prescription. Use it 1 to 2 times a day for a few days. Try cooling it in the refrigerator before applying.
- Moisturize your skin. Apply a moisturizer once or twice a day, as a top layer over any medicated cream you're using. Ointments and creams tend to protect skin better than do lotions with high water content. Choose a product that has no dyes, alcohols, fragrances and other ingredients that might irritate the skin. Allow the moisturizer to absorb into the skin before getting dressed.
- Apply a cool, wet cloth. Place a cool, wet cloth over the rash for 15 to 30 minutes several times a day. This may help soothe your skin.
- Take a warm bath. Sprinkle your bathwater with finely ground oatmeal that's made for the bathtub. You might see this in the store labeled as colloidal oatmeal (Aveeno, others). Soak for less than 10 minutes, then pat dry. Apply moisturizer while the skin is still damp. A lotion with 12% ammonium lactate helps with flaky, dry skin.
- Use medicated shampoos. For dandruff, first try nonprescription shampoos containing selenium sulfide, zinc pyrithione, coal tar or ketoconazole. If that doesn't help, talk with your doctor about a stronger shampoo, such as those available only with a prescription.
-
Take a bleach bath. This may help people with severe atopic dermatitis by decreasing the bacteria on the skin. For a dilute bleach bath, add 1/2 cup (118 milliliters) of household bleach, not concentrated bleach, to a 40-gallon (151-liter) bathtub filled with warm water. Measures are for a U.S. standard-sized tub filled to the overflow drainage holes. Soak from the neck down or just the affected areas for 5 to 10 minutes. Don't put the head under water. Rinse with tap water, then pat dry. Take a bleach bath 2 to 3 times a week.
Many people have had success using a dilute vinegar bath rather than a bleach bath. Add 1 cup (236 milliliters) of vinegar to a bathtub filled with warm water.
Talk with your doctor about whether either of these approaches is a good idea for you.
- Protect your skin. Avoid rubbing and scratching. Cover the itchy area with a dressing if you can't keep from scratching it. Trim your nails and wear gloves at night. While your skin heals, stay out of the sun or use other sun protection measures.
- Avoid known irritants or allergens. Avoid rough and scratchy clothing. And try to identify and remove allergens and other things in your environment that irritate your skin. Fragrances used in skin care products are one of the common allergens. Avoid using perfumes, colognes and scented soaps, deodorants and laundry detergents. Choose unscented options. Avoid using fabric softeners in the washer or dryer.
- Manage your stress. Emotional stress can cause some types of dermatitis to flare. Being aware of stress and anxiety and taking steps to improve your emotional health may help your skin too.
Alternative medicine
Many alternative therapies, including those listed below, have helped some people manage their dermatitis.
- Taking dietary supplements, such as vitamin D and probiotics, for atopic dermatitis.
- Applying rice bran broth to the skin, for atopic dermatitis.
- Using 5% tea tree oil shampoo, for dandruff.
- Applying an aloe product to the skin, for seborrheic dermatitis.
- Taking Chinese herbal therapy.
The evidence for whether these approaches work is mixed. And sometimes herbal and traditional remedies cause irritation or an allergic reaction.
Alternative therapies are sometimes called integrative medicine. If you're considering dietary supplements or other integrative medicine approaches, talk with your doctor about their pros and cons.
Preparing for an appointment
You may first bring your concerns to the attention of your primary care provider. Or you may see a doctor who specializes in the diagnosis and treatment of skin conditions (dermatologist) or allergies (allergist).
Here's some information to help you get ready for your appointment.
What you can do
- List your symptoms, when they occurred and how long they lasted. Also, it may help to list factors that triggered or worsened your symptoms — such as soaps or detergents, tobacco smoke, sweating, or long, hot showers.
- Make a list of all the medicines, vitamins, supplements and herbs you're taking. Even better, take the original bottles and a list of the dosages and directions.
- List questions to ask your health care provider. Ask questions when you want something clarified.
What to expect from your doctor
Your doctor is likely to ask you a few questions. Being ready to answer them may free up time to go over any points you want to spend more time on. Your doctor might ask:
- Do your symptoms come and go, or are they fairly constant?
- How often do you shower or bathe?
- What products do you use on your skin, including soaps, lotions and cosmetics?
- What household cleaning products do you use?
- Are you exposed to any possible irritants from your job or hobbies?
- Have you been under any unusual stress or depressed lately?
- How much do your symptoms affect your quality of life, including your ability to sleep?
- What treatments have you tried so far? Has anything helped?
Last Updated Sep 8, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



