Dyshidrosis
Overview
Dyshidrosis is a skin condition that causes small, fluid-filled blisters to form on the palms of the hands and sides of the fingers. Sometimes the bottoms of the feet are affected too.
The itchy blisters last a few weeks and often come back.
Treatment for dyshidrosis most often includes prescription steroid skin creams or ointments. Your doctor or other health care provider may suggest a different treatment, such as light therapy or medicine taken by mouth or injection. The right treatment depends on how severe your symptoms are.
Dyshidrosis is also called dyshidrotic eczema and pompholyx.
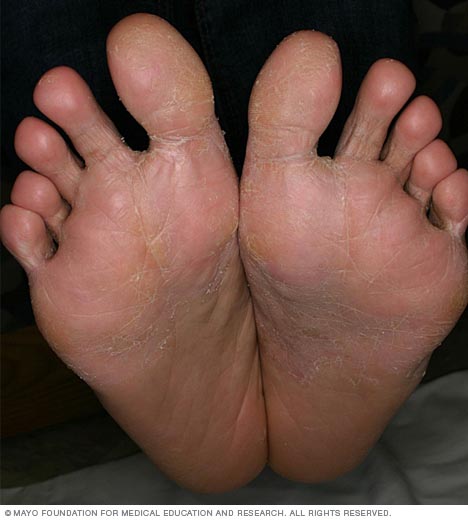
Dyshidrosis causes small, fluid-filled blisters to form on the soles of the feet, the palms of the hands or sides of the fingers.
Symptoms
Dyshidrosis symptoms include painful, itchy and fluid-filled blisters on the sides of the fingers, the palms of the hands and the bottoms of the feet. The blisters are small — about the width of a standard pencil lead. They are grouped in clusters and can look like tapioca.
With severe disease, the small blisters can merge to form larger blisters. Skin affected by dyshidrosis can be painful and very itchy. After a few weeks, the blisters dry and flake off.
Dyshidrosis tends to come back regularly for months or years.
When to see a doctor
Call your doctor if you have a rash on your hands or feet that's severe, doesn't go away, or spreads beyond the hands and feet.
Causes
The cause of dyshidrosis isn't known. It tends to happen in people who have a skin condition called atopic dermatitis (eczema) and allergic conditions, such as hay fever or glove allergy. Dyshidrosis isn't contagious.
Risk factors
Risk factors for dyshidrosis include:
- Stress. Dyshidrosis appears to be more common during times of emotional or physical stress.
- Exposure to certain metals. These include cobalt and nickel — often in an industrial setting.
- Sensitive skin. People who develop a rash after contact with certain irritants are more likely to form the blisters of dyshidrosis.
- Atopic dermatitis. Some people with atopic dermatitis may have dyshidrosis.
Complications
For most people with dyshidrosis, it's just an itchy inconvenience. For others, the pain and itching may limit the use of their hands or feet. Intense scratching can increase the risk of a bacterial infection of the affected skin.
After healing, you may notice skin color changes in the affected area. This is called postinflammatory hyperpigmentation. It's more likely to occur in people with brown or Black skin. This complication most often goes away in time without treatment.
Prevention
There's no way to prevent dyshidrosis. It may help to manage stress and avoid exposure to metal salts, such as cobalt and nickel.
Good skin care practices may help protect the skin as well. These include:
- Using mild, nonsoap cleansers and lukewarm water to wash your hands.
- Drying your hands well.
- Applying moisturizer at least twice a day.
- Wearing gloves. But if you notice that wearing gloves worsens the rash, you may be sensitive to gloves. Let your doctor know about this. Try cotton gloves to prevent irritation. For wet activities, you might try wearing cotton gloves under waterproof gloves.
Diagnosis
To diagnosis dyshidrosis, your doctor will likely talk with you about your medical history and look at the affected skin. You might need other tests to rule out conditions that can cause symptoms similar to those of dyshidrosis. For example, a scraping of the skin can be tested for the type of fungus that causes athlete's foot. Or you might have a patch test. With this test, the skin is exposed to a small amount of suspected allergen and watched for a reaction.
Treatment
Dyshidrosis treatment might involve:
-
Corticosteroids. Your doctor may prescribe a corticosteroid cream or ointment to help clear up the blisters. Covering the treated area in plastic wrap or a moist bandage helps the skin absorb the medicine. Long-term use of steroids can cause side effects, such as spider veins and thinning of skin.
In severe cases, your doctor may prescribe a brief course of oral steroids, such as prednisone, as a bridge to other treatments.
- Phototherapy. If other treatments aren't effective, your doctor may recommend light therapy. In this treatment, a UV light called narrowband UVB is directed at the affected skin.
- Immune-suppressing ointments. The calcineurin inhibitor tacrolimus (Protopic) may be helpful for people who want to limit their exposure to steroids. Do not combine this treatment with phototherapy.
- Controlling sweating. Heavy sweating of the palms and soles may contribute to dyshidrosis. Your doctor might suggest anti-perspirants or injection with botulinum toxin A. This treatment may help reduce sweating and improve the skin.
Lifestyle and home remedies
Home treatment might include:
- Applying a moist cloth. A wet, cool cloth may help reduce itching.
- Taking anti-itch drugs. Antihistamine medicine that you can get at a store without a prescription may help relieve itching. Examples are diphenhydramine and loratadine (Alavert, Claritin).
Preparing for an appointment
You're likely to start by seeing your primary care provider. You may be referred to a doctor who specializes in skin disorders (dermatologist). Here's some information to help you get ready for your appointment.
What you can do
Before your appointment, list answers to the following questions:
- Have you experienced this problem in the past?
- Do you have an allergy, such as to rubber, glue, fragrances or nickel?
- Have you been under extra stress lately?
- What medicines and supplements do you take?
- Are you exposed to certain metals or chemicals at work or during other activities?
What to expect from your doctor
Your doctor is likely to ask you questions, such as:
- When did you first notice your symptoms?
- Are your symptoms present all the time or only once in a while?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Last Updated Jun 27, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



