Eye floaters
Overview
Eye floaters are spots in your vision. They may look to you like black or gray specks, strings, or cobwebs. They may drift about when you move your eyes. Floaters appear to dart away when you try to look at them directly.
Most eye floaters are caused by age-related changes that occur as the jelly-like substance (vitreous) inside your eyes liquifies and contracts. Scattered clumps of collagen fibers form within the vitreous and can cast tiny shadows on your retina. The shadows you see are called floaters.
If you notice a sudden increase in eye floaters, contact an eye specialist immediately — especially if you also see light flashes or lose your vision. These can be symptoms of an emergency that requires prompt attention.
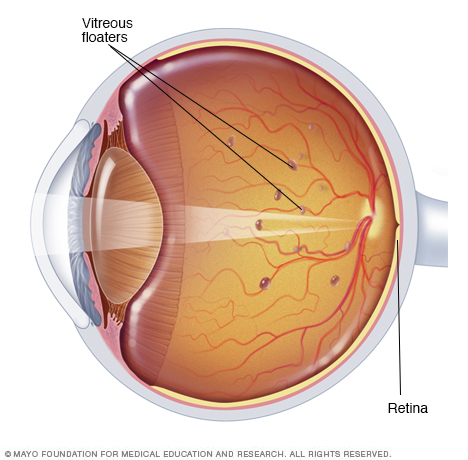
As you age, the vitreous — a jelly-like material inside your eyes — liquifies and contracts. When this happens, microscopic collagen fibers in the vitreous tend to clump together. These scattered pieces cast tiny shadows onto your retina. The shadows you see are called floaters.
Symptoms
Symptoms of eye floaters may include:
- Small shapes in your vision that appear as dark specks or knobby, transparent strings of floating material
- Spots that move when you move your eyes, so when you try to look at them, they move quickly out of your line of vision
- Spots that are most noticeable when you look at a plain bright background, such as a blue sky or a white wall
- Small shapes or strings that eventually settle down and drift out of the line of vision
When to see a doctor
Contact an eye specialist immediately if you notice:
- Many more eye floaters than usual
- A sudden onset of new floaters
- Flashes of light in the same eye as the floaters
- A gray curtain or blurry area that blocks part of your vision
- Darkness on a side or sides of your vision (peripheral vision loss)
These painless symptoms could be caused by a retinal tear, with or without a retinal detachment. This is a sight-threatening condition that requires immediate attention.
Causes
Eye floaters may be caused by vitreous changes related to aging or from other diseases or conditions:
-
Age-related eye changes. The vitreous is a jelly-like substance made primarily of water, collagen (a type of protein) and hyaluronan (a type of carbohydrate). The vitreous fills the space in your eye between the lens and retina and helps the eye maintain its round shape.
As you age, the vitreous changes. Over time, it liquifies and contracts — a process that causes it to pull away from the eyeball's inside surface.
As the vitreous changes, collagen fibers within the vitreous form clumps and strings. These scattered pieces block some of the light passing through the eye. This casts tiny shadows on your retina that are seen as floaters.
- Inflammation in the back of the eye. Uveitis is inflammation in the middle layer of tissue in the eye wall (uvea). Posterior uveitis affects the back of the eye, which includes the retina and an eye layer called the choroid. The inflammation causes floaters in the vitreous. Causes of posterior uveitis include infection, autoimmune disorders and inflammatory diseases.
- Bleeding in the eye. Bleeding into the vitreous can have many causes, including retinal tears and detachments, diabetes, high blood pressure (hypertension), blocked blood vessels, and injury. Blood cells are seen as floaters.
- Torn retina. Retinal tears can happen when a contracting vitreous tugs on the retina with enough force to tear it. Without treatment, a retinal tear may lead to retinal detachment. If fluid leaks behind the tear, it can cause the retina to separate from the back of your eye. Untreated retinal detachment can cause permanent vision loss.
- Eye surgeries and eye medications. Certain medications that are injected into the vitreous can cause air bubbles to form. These bubbles are seen as shadows until your eye absorbs them. Silicone oil bubbles added during certain surgeries on the vitreous and retina also can be seen as floaters.
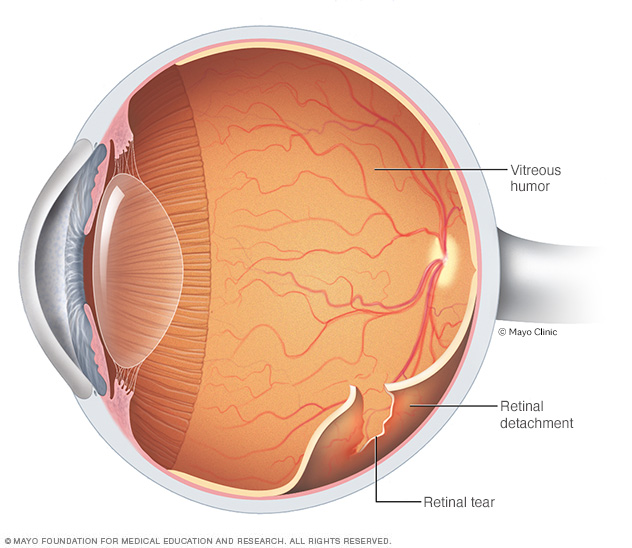
Retinal detachment describes an emergency situation in which a thin layer of tissue (the retina) at the back of the eye pulls away from the layer of blood vessels that provides it with oxygen and nutrients. Retinal detachment is often accompanied by flashes and floaters in your vision.
Risk factors
Factors that can increase your risk of eye floaters include:
- Age over 50 years
- Nearsightedness
- Eye injury
- Complications from cataract surgery
- Diabetes complication that causes damage to the blood vessels of the retina (diabetic retinopathy)
- Eye inflammation
Diagnosis
Your eye care specialist conducts a complete eye exam to determine the cause of your eye floaters. Your exam usually includes eye dilation. Eye drops widen (dilate) the dark center of your eye. This allows your specialist to better see the back of your eyes and the vitreous.
Treatment
Most eye floaters don't require treatment. However, any medical condition that is the cause of eye floaters, such as bleeding from diabetes or inflammation, should be treated.
Eye floaters can be frustrating and adjusting to them can take time. Once you know the floaters will not cause any more problems, over time you may be able to ignore them or notice them less often.
If your eye floaters get in the way of your vision, which happens rarely, you and your eye care specialist may consider treatment. Options may include surgery to remove the vitreous or a laser to disrupt the floaters, although both procedures are rarely done.
- Surgery to remove the vitreous. An ophthalmologist who is a specialist in retina and vitreous surgery removes the vitreous through a small incision (vitrectomy). The vitreous is replaced with a solution to help your eye maintain its shape. Surgery may not remove all the floaters, and new floaters can develop after surgery. Risks of a vitrectomy include infection, bleeding and retinal tears.
- Using a laser to disrupt the floaters. An ophthalmologist aims a special laser at the floaters in the vitreous (vitreolysis). This may break up the floaters and make them less noticeable. Some people who have this treatment report improved vision; others notice little or no difference. Risks of laser therapy include damage to your retina if the laser is aimed incorrectly.
Preparing for an appointment
If you're concerned about eye floaters, make an appointment with a specialist in eye disorders (optometrist or ophthalmologist) for an eye exam. If you have complications that require treatment, you'll need to see an ophthalmologist. Here's some information to help you get ready for your appointment.
What you can do
Before your appointment, make a list of:
- Your symptoms, including situations that increase eye floaters you see or times when you see fewer eye floaters
- All medications, vitamins, herbs and other supplements you take, and the dosages
- Questions to ask your eye care specialist to help you make the most of your appointment
For eye floaters, some basic questions to ask include:
- Why do I see these eye floaters?
- Will they always be there?
- What can I do to prevent more from occurring?
- Are there treatments available?
- Are there brochures or other printed material that I can take? What websites do you recommend?
- Do I need a follow-up appointment, and, if so, when?
What to expect from your doctor
Your eye care specialist is likely to ask you a number of questions, such as:
- When did your eye floaters begin?
- Which eye has the floaters?
- Have your symptoms been continuous or occasional?
- Have you recently noticed an increase in the number of floaters?
- Have you seen light flashes?
- Does anything seem to improve or worsen your symptoms?
- Have you ever had eye surgery?
- Do you have any medical conditions, such as diabetes or high blood pressure?
Last Updated Jul 2, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use