Genital herpes
Overview
Genital herpes is a common sexually transmitted infection (STI). The herpes simplex virus (HSV) causes genital herpes. Genital herpes can often be spread by skin-to-skin contact during sexual activity.
Some people infected with the virus may have very mild symptoms or no symptoms. They can still able to spread the virus. Other people have pain, itching and sores around the genitals, anus or mouth.
There is no cure for genital herpes. Symptoms often show up again after the first outbreak. Medicine can ease symptoms. It also lowers the risk of infecting others. Condoms can help prevent the spread of a genital herpes infection.
Symptoms
Most people infected with HSV don't know they have it. They may have no symptoms or have very mild symptoms.
Symptoms start about 2 to 12 days after exposure to the virus. They may include:
- Pain or itching around the genitals
- Small bumps or blisters around the genitals, anus or mouth
- Painful ulcers that form when blisters rupture and ooze or bleed
- Scabs that form as the ulcers heal
- Painful urination
- Discharge from the urethra, the tube that releases urine from the body
- Discharge from the vagina
During the first outbreak, you may commonly have flu-like symptoms such as:
- Fever
- Headache
- Body aches
- Swollen lymph nodes in the groin
Differences in symptom location
Sores appear where the infection enters the body. You can spread the infection by touching a sore and then rubbing or scratching another area of your body. That includes your fingers or eyes.
Sore can develop on or in the:
- Buttocks
- Thighs
- Rectum
- Anus
- Mouth
- Urethra
- Vulva
- Vagina
- Cervix
- Penis
- Scrotum
Repeat outbreaks
After the first outbreak of genital herpes, symptoms often appear again. These are called recurrent outbreaks or recurrent episodes.
How often recurrent outbreaks happen varies widely. You'll usually have the most outbreaks the first year after infection. They may appear less often over time. Your symptoms during recurrent outbreaks usually don't last as long and aren't as severe as the first.
You may have warning signs a few hours or days before a new outbreak starts. These are called prodromal symptoms. They include:
- Genital pain
- Tingling or shooting pain in the legs, hips or buttocks
When to see a doctor
If you suspect you have genital herpes, or any other STI, see your health care provider.
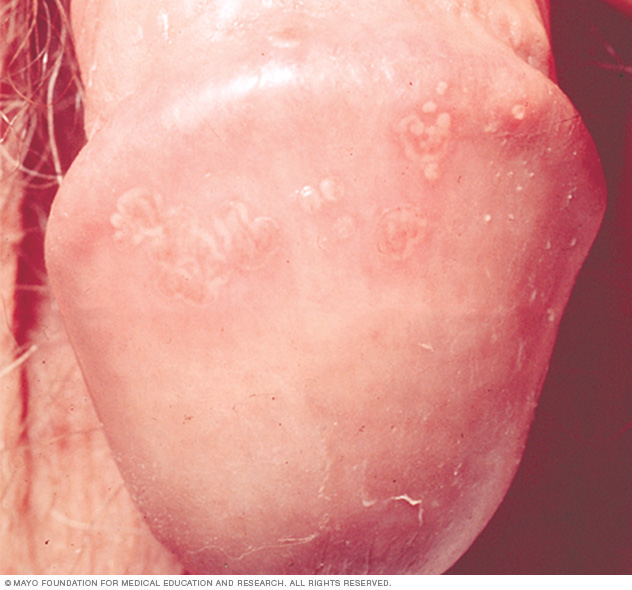
Sores associated with genital herpes can be small bumps, blisters or open sores. Scabs eventually form and the sores heal, but they tend to recur.
Causes
Genital herpes is caused by two types of herpes simplex virus. These types include herpes simplex virus type 2 (HSV-2) and herpes simplex virus type 1 (HSV-1). People with HSV infections can pass along the virus even when they have no visible symptoms.
HSV-2
HSV-2 is the most common cause of genital herpes. The virus can be present:
- On blisters and ulcers or the fluid from ulcers
- The moist lining or fluids of the mouth
- The moist lining or fluids of the vagina or rectum
The virus moves from one person to another during sexual activity.
HSV-1
HSV-1 is a version of the virus that causes cold sores or fever blisters. People may be exposed to HSV-1 as children due to close skin-to-skin contact with someone infected.
A person with HSV-1 in tissues of the mouth can pass the virus to the genitals of a sexual partner during oral sex. The newly caught infection is a genital herpes infection.
Recurrent outbreaks of genital herpes caused by HSV-1 are often less frequent than outbreaks caused by HSV-2.
Neither HSV-1 nor HSV-2 survives well at room temperature. So the virus is not likely to spread through surfaces, such as a faucet handle or a towel. But kissing or sharing a drinking glass or silverware might spread the virus.
Risk factors
A higher risk of getting genital herpes is linked to:
- Contact with genitals through oral, vaginal or anal sex. Having sexual contact without using a barrier increases your risk of genital herpes. Barriers include condoms and condom-like protectors called dental dams used during oral sex. Women are at higher risk of getting genital herpes. The virus can spread more easily from men to women than from women to men.
- Having sex with multiple partners. The number of people you have sex with is a strong risk factor. Contact with genitals through sex or sexual activity puts you at higher risk. Most people with genital herpes do not know they have it.
- Having a partner who has the disease but is not taking medicine to treat it. There is no cure for genital herpes, but medicine can help limit outbreaks.
- Certain groups within the population. Women, people with a history of sexually transmitted diseases, older people, Black people in in the United States and men who have sex with men diagnosed with genital herpes at a higher than average rate. People in groups at higher risk may choose to talk to a health care provider about their personal risk.
Complications
Complications associated with genital herpes may include:
- Other sexually transmitted infections. Having genital sores raises your risk of giving or getting other STIs, including HIV/AIDS.
- Newborn infection. A baby can be infected with HSV during delivery. Less often, the virus is passed during pregnancy or by close contact after delivery. Newborns with HSV often have infections of internal organs or the nervous system. Even with treatment, these newborns have a high risk of developmental or physical problems and a risk of death.
- Internal inflammatory disease. HSV infection can cause swelling and inflammation within the organs associated with sexual activity and urination. These include the ureter, rectum, vagina, cervix and uterus.
- Finger infection. An HSV infection can spread to a finger through a break in the skin causing discoloration, swelling and sores. The infections are called herpetic whitlow.
- Eye infection. HSV infection of the eye can cause pain, sores, blurred vision and blindness.
- Swelling of the brain. Rarely, HSV infection leads to inflammation and swelling of the brain, also called encephalitis.
- Infection of internal organs. Rarely, HSV in the bloodstream can cause infections of internal organs.
Prevention
Prevention of genital herpes is the same as preventing other sexually transmitted infections.
- Have one long-term sexual partner who has been tested for STIs and isn't infected.
- Use a condom or dental dam during sexual activity. These reduce the risk of disease, but they don't prevent all skin-to-skin contact during sex.
- Don't have sex when a partner with genital herpes has symptoms.
Pregnancy precautions
If you are pregnant and know you have genital herpes, tell your health care provider. If you think you might have genital herpes, ask your provider if you can be tested for it.
Your provider may recommend that you take herpes antiviral medicines late in pregnancy. This is to try to prevent an outbreak around the time of delivery. If you have an outbreak when you go into labor, your provider may suggest a cesarean section. That is a surgery to remove the baby from your uterus. It lowers the risk of passing the virus to your baby.
Diagnosis
Your health care provider can usually make a diagnosis of genital herpes based on a physical exam and a history of your sexual activity.
To confirm a diagnosis, your provider will likely take a sample from an active sore. One or more tests of these samples are used to see if you have herpes simplex virus (HSV), infection and show whether the infection is HSV-1 or HSV-2.
Less often, a lab test of your blood may be used for confirming a diagnosis or ruling out other infections.
Your care provider will likely recommend that you get tested for other STIs. Your partner should also be tested for genital herpes and other STIs.
Treatment
There's no cure for genital herpes. Treatment with prescription antiviral pills may be used for the following:
- Help sores heal during a first outbreak
- Lower the frequency of recurrent outbreaks
- Lessen the severity and duration of symptoms in recurrent outbreaks
- Reduce the chance of passing the herpes virus to a partner
Commonly prescribed medicines used for genital herpes include:
- Acyclovir (Zovirax)
- Famciclovir
- Valacyclovir (Valtrex)
Your health care provider will talk to you about the right treatment for you. Treatment depends on the severity of disease, the type of HSV, your sexual activity and other medical factors. The dose will vary depending on whether you currently have symptoms. Long-term use of the antiviral drugs is considered safe.
Coping and support
A diagnosis of genital herpes may cause embarrassment, shame, anger or other strong emotions. You may be suspicious or resentful of your partner. Or you might be worried about rejection by your current partner or future partners.
Healthy ways to cope with having genital herpes include the following:
- Communicate with your partner. Be open and honest about your feelings. Trust your partner and believe what your partner tells you.
- Educate yourself. Talk with your health care provider or a counselor. They can help you learn how to live with the condition. They can also help you lessen the chance of infecting others. Learn about your treatment options and how to manage outbreaks.
- Join a support group. Look for a group in your area or online. Talk about your feelings and learn from others' experiences.
Preparing for an appointment
If you think you have genital herpes or another STI, make an appointment to see your health care provider.
Be prepared to answer the following questions:
- What are your symptoms? When did they start?
- Do you have sores or unusual discharge?
- Do you have pelvic pain?
- Do you have pain while urinating?
- Do you have a new sexual partner or multiple partners?
- Have you ever been diagnosed with a sexually transmitted infection?
- Do you regularly use condoms?
- What medications or supplements do you take regularly?
Last Updated Nov 22, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



