Glaucoma
Overview
Glaucoma is a group of eye conditions that damage the optic nerve. The optic nerve sends visual information from your eye to your brain and is vital for good vision. Damage to the optic nerve is often related to high pressure in your eye. But glaucoma can happen even with normal eye pressure.
Glaucoma can occur at any age but is more common in older adults. It is one of the leading causes of blindness for people over the age of 60.
Many forms of glaucoma have no warning signs. The effect is so gradual that you may not notice a change in vision until the condition is in its later stages.
It's important to have regular eye exams that include measurements of your eye pressure. If glaucoma is recognized early, vision loss can be slowed or prevented. If you have glaucoma, you'll need treatment or monitoring for the rest of your life.
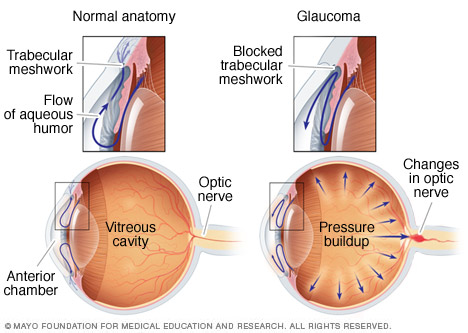
Usually, fluid (aqueous humor) in the eye flows freely through the anterior chamber and exits through the drainage system (trabecular meshwork). If that system is blocked or isn't functioning well, the pressure inside the eye (intraocular pressure) builds, which in turn damages the optic nerve. With the most common type of glaucoma, this results in gradual vision loss.
Symptoms
The symptoms of glaucoma depend on the type and stage of your condition.
Open-angle glaucoma
- No symptoms in early stages
- Gradually, patchy blind spots in your side vision. Side vision also is known as peripheral vision
- In later stages, difficulty seeing things in your central vision
Acute angle-closure glaucoma
- Severe headache
- Severe eye pain
- Nausea or vomiting
- Blurred vision
- Halos or colored rings around lights
- Eye redness
Normal-tension glaucoma
- No symptoms in early stages
- Gradually, blurred vision
- In later stages, loss of side vision
Glaucoma in children
- A dull or cloudy eye (infants)
- Increased blinking (infants)
- Tears without crying (infants)
- Blurred vision
- Nearsightedness that gets worse
- Headache
Pigmentary glaucoma
- Halos around lights
- Blurred vision with exercise
- Gradual loss of side vision
When to see a doctor
If you experience symptoms that come on suddenly, you may have acute angle-closure glaucoma. Symptoms include severe headache and severe eye pain. You need treatment as soon as possible. Go to an emergency room or call an eye doctor's (ophthalmologist's) office immediately.
Causes
Glaucoma develops when the optic nerve becomes damaged. As this nerve gradually deteriorates, blind spots develop in your vision. For reasons that doctors don't fully understand, this nerve damage is usually related to increased pressure in the eye.
Elevated eye pressure happens as the result of a buildup of fluid that flows throughout the inside of the eye. This fluid also is known as the aqueous humor. It usually drains through a tissue located at the angle where the iris and cornea meet. This tissue also is called the trabecular meshwork. The cornea is important to vision because it lets light into the eye. When the eye makes too much fluid or the drainage system doesn't work properly, eye pressure may increase.
Open-angle glaucoma
This is the most common form of glaucoma. The drainage angle formed by the iris and cornea remains open. But other parts of the drainage system don't drain properly. This may lead to a slow, gradual increase in eye pressure.
Angle-closure glaucoma
This form of glaucoma occurs when the iris bulges. The bulging iris partially or completely blocks the drainage angle. As a result, fluid can't circulate through the eye and pressure increases. Angle-closure glaucoma may occur suddenly or gradually.
Normal-tension glaucoma
No one knows the exact reason why the optic nerve becomes damaged when eye pressure is normal. The optic nerve may be sensitive or experience less blood flow. This limited blood flow may be caused by the buildup of fatty deposits in the arteries or other conditions that damage circulation. The buildup of fatty deposits in the arteries also is known as atherosclerosis.
Glaucoma in children
A child may be born with glaucoma or develop it in the first few years of life. Blocked drainage, injury or an underlying medical condition may cause optic nerve damage.
Pigmentary glaucoma
In pigmentary glaucoma, small pigment granules flake off from the iris and block or slow fluid drainage from the eye. Activities such as jogging sometimes stir up the pigment granules. That leads to a deposit of pigment granules on tissue located at the angle where the iris and cornea meet. The granule deposits cause an increase in pressure.
Glaucoma tends to run in families. In some people, scientists have identified genes related to high eye pressure and optic nerve damage.
Risk factors
Glaucoma can damage vision before you notice any symptoms. So be aware of these risk factors:
- High internal eye pressure, also known as intraocular pressure
- Age over 55
- Black, Asian or Hispanic heritage
- Family history of glaucoma
- Certain medical conditions, such as diabetes, migraines, high blood pressure and sickle cell anemia
- Corneas that are thin in the center
- Extreme nearsightedness or farsightedness
- Eye injury or certain types of eye surgery
- Taking corticosteroid medicines, especially eye drops, for a long time
Some people have narrow drainage angles, putting them at increased risk of angle-closure glaucoma.
Prevention
These steps may help detect and manage glaucoma in its early stages. That may help to prevent vision loss or slow its progress.
Get regular eye examinations. Regular comprehensive eye exams can help detect glaucoma in its early stages, before significant damage occurs. As a general rule, the American Academy of Ophthalmology recommends a comprehensive eye exam every 5 to 10 years if you're under 40 years old; every 2 to 4 years if you're 40 to 54 years old; every 1 to 3 years if you're 55 to 64 years old; and every 1 to 2 years if you're older than 65.
If you're at risk of glaucoma, you'll need more frequent screening. Ask your health care provider to recommend the right screening schedule for you.
- Know your family's eye health history. Glaucoma tends to run in families. If you're at increased risk, you may need more frequent screening.
- Wear eye protection. Serious eye injuries can lead to glaucoma. Wear eye protection when using power tools or playing sports.
- Take prescribed eye drops regularly. Glaucoma eye drops can significantly reduce the risk that high eye pressure will progress to glaucoma. Use eye drops as prescribed by your health care provider even if you have no symptoms.
Diagnosis
Your health care provider will review your medical history and conduct a comprehensive eye examination. Your provider may perform several tests, including:
- Measuring intraocular pressure, also called tonometry
- Testing for optic nerve damage with a dilated eye examination and imaging tests
- Checking for areas of vision loss, also known as a visual field test
- Measuring corneal thickness with an exam called pachymetry
- Inspecting the drainage angle, also known as gonioscopy
Treatment
The damage caused by glaucoma can't be reversed. But treatment and regular checkups can help slow or prevent vision loss, especially if you catch the disease in its early stages.
Glaucoma is treated by lowering intraocular pressure. Treatment options include prescription eye drops, oral medicines, laser treatment, surgery or a combination of approaches.
Eyedrops
Glaucoma treatment often starts with prescription eye drops. Some may decrease eye pressure by improving how fluid drains from your eye. Others decrease the amount of fluid your eye makes. Depending on how low your eye pressure needs to be, you may be prescribed more than one eye drop.
Prescription eye drop medicines include:
Prostaglandins. These increase the outflow of the fluid in your eye, helping to reduce eye pressure. Medicines in this category include latanoprost (Xalatan), travoprost (Travatan Z), tafluprost (Zioptan), bimatoprost (Lumigan) and latanoprostene bunod (Vyzulta).
Possible side effects include mild reddening and stinging of the eyes, darkening of the iris, darkening of the pigment of the eyelashes or eyelid skin, and blurred vision. This class of drug is prescribed for once-a-day use.
Beta blockers. These reduce the production of fluid in your eye, helping to lower eye pressure. Examples include timolol (Betimol, Istalol, Timoptic) and betaxolol (Betoptic S).
Possible side effects include difficulty breathing, slowed heart rate, lower blood pressure, impotence and fatigue. This class of drug can be prescribed for once- or twice-daily use depending on your condition.
Alpha-adrenergic agonists. These reduce the production of the fluid that flows throughout the inside of your eye. They also increase the outflow of fluid in your eye. Examples include apraclonidine (Iopidine) and brimonidine (Alphagan P, Qoliana).
Possible side effects include irregular heart rate, high blood pressure, fatigue, red, itchy or swollen eyes, and dry mouth. This class of drug is usually prescribed for twice-daily use but sometimes can be prescribed for use three times a day.
- Carbonic anhydrase inhibitors. These medicines reduce the production of fluid in your eye. Examples include dorzolamide and brinzolamide (Azopt). Possible side effects include a metallic taste, frequent urination, and tingling in the fingers and toes. This class of drug is usually prescribed for twice-daily use but sometimes can be prescribed for use three times a day.
- Rho kinase inhibitor. This medicine lowers eye pressure by suppressing the rho kinase enzymes responsible for fluid increase. It is available as netarsudil (Rhopressa) and is prescribed for once-a-day use. Possible side effects include eye redness and eye discomfort.
- Miotic or cholinergic agents. These increase the outflow of fluid from your eye. An example is pilocarpine (Isopto Carpine). Side effects include headache, eye ache, smaller pupils, possible blurred or dim vision, and nearsightedness. This class of medicine is usually prescribed to be used up to four times a day. Because of potential side effects and the need for frequent daily use, these medicines are not prescribed very often anymore.
Because some of the eye drop medicine is absorbed into your bloodstream, you may experience some side effects unrelated to your eyes. To minimize this absorption, close your eyes for 1 to 2 minutes after putting the drops in. You also may press lightly at the corner of your eyes near your nose to close the tear duct for 1 or 2 minutes. Wipe off any unused drops from your eyelid.
You may have been prescribed multiple eye drops or need to use artificial tears. Make sure you wait at least five minutes in between using different drops.
Oral medications
Eye drops alone may not bring your eye pressure down to the desired level. So your eye doctor may also prescribe oral medicine. This medicine is usually a carbonic anhydrase inhibitor. Possible side effects include frequent urination, tingling in the fingers and toes, depression, stomach upset, and kidney stones.
Surgery and other therapies
Other treatment options include laser therapy and surgery. The following techniques may help to drain fluid within the eye and lower eye pressure:
- Laser therapy. Laser trabeculoplasty (truh-BEK-u-low-plas-tee) is an option if you can't tolerate eye drops. It also may be used if medicine hasn't slowed the progression of your disease. Your eye doctor also may recommend laser surgery before using eye drops. It's done in your eye doctor's office. Your eye doctor uses a small laser to improve the drainage of the tissue located at the angle where the iris and cornea meet. It may take a few weeks before the full effect of this procedure becomes apparent.
- Filtering surgery. This is a surgical procedure called a trabeculectomy (truh-bek-u-LEK-tuh-me). The eye surgeon creates an opening in the white of the eye, which also is known as the sclera. The surgery creates another space for fluid to leave the eye.
- Drainage tubes. In this procedure, the eye surgeon inserts a small tube in your eye to drain excess fluid to lower eye pressure.
- Minimally invasive glaucoma surgery (MIGS). Your eye doctor may suggest a MIGS procedure to lower your eye pressure. These procedures generally require less immediate postoperative care and have less risk than trabeculectomy or using a drainage device. They are often combined with cataract surgery. There are a number of MIGS techniques available, and your eye doctor will discuss which procedure may be right for you.
After your procedure, you'll need to see your eye doctor for follow-up exams. And you may eventually need to undergo additional procedures if your eye pressure begins to rise or other changes occur in your eye.
Treating acute angle-closure glaucoma
Acute angle-closure glaucoma is a medical emergency. If you're diagnosed with this condition, you'll need urgent treatment to reduce the pressure in your eye. This generally will require treatment with medicine and laser or surgical procedures.
You may have a procedure called a laser peripheral iridotomy. The doctor creates a small hole in your iris using a laser. This allows fluid to flow through the iris. This helps to open the drainage angle of the eye and relieves eye pressure.
Lifestyle and home remedies
These tips may help you control high eye pressure or promote eye health.
- Eat a healthy diet. Eating a healthy diet can help you maintain your health, but it won't prevent glaucoma from worsening. Several vitamins and nutrients are important to eye health, including zinc, copper, selenium and antioxidant vitamins C, E and A.
- Exercise safely. Regular exercise may reduce eye pressure. Talk to your health care provider about an appropriate exercise program.
- Limit your caffeine. Drinking beverages with large amounts of caffeine may increase your eye pressure.
- Sip fluids carefully. Drink moderate amounts of fluids. Drinking a quart or more of any liquid within a short time may temporarily increase eye pressure.
- Take prescribed medicine. Using your eye drops or other medicines as prescribed can help you get the best possible result from your treatment. Be sure to use the drops exactly as prescribed. Otherwise, your optic nerve damage could get worse.
Alternative medicine
Some alternative medicine approaches may help your overall health, but none is an effective glaucoma remedy. Talk with your doctor about their possible benefits and risks.
- Herbal remedies. Some herbal supplements, such as bilberry extract, have been advertised as glaucoma remedies. But further study is needed to prove their effectiveness. Don't use herbal supplements in place of proven therapies.
- Relaxation techniques. Stress may trigger an attack of acute angle-closure glaucoma. Try to find healthy ways to cope with stress. Meditation and other techniques may help.
- Marijuana. Research shows that marijuana lowers eye pressure in people with glaucoma, but only for 3 to 4 hours. Other, standard treatments are more effective. The American Academy of Ophthalmology doesn't recommend marijuana for treating glaucoma.
Coping and support
When you receive a diagnosis of glaucoma, you're potentially facing lifelong treatment, regular checkups and the possibility of progressive vision loss.
Meeting and talking with other people with glaucoma can be very helpful, and many support groups exist. Check with hospitals and eye care centers in your area to find local groups and meeting times. Look for online resources, including support groups.
Preparing for an appointment
You may start by seeing your primary health care provider. Or you may be referred immediately to an eye specialist (ophthalmologist).
Here's some information to help you get ready for your appointment.
What you can do
When you make the appointment, ask if there's anything you need to do in advance, such as fasting before having a specific test. Make a list of:
- Your symptoms, including any that seem unrelated to the reason for your appointment
- Key personal information, including major stresses, recent life changes and family medical history
- All medications, vitamins or other supplements you take, including the doses
- Questions to ask your doctor
Take a family or friend along, if possible, to help you remember the information you're given.
For glaucoma, some basic questions to ask include:
- What's likely causing my symptoms?
- Other than the most likely cause, what are other possible causes for my symptoms?
- What tests do I need?
- Is my condition likely temporary or chronic?
- What's the best course of action?
- What are the alternatives to the primary approach you're suggesting?
- I have these other health conditions. How can I best manage them together?
- Are there restrictions I need to follow?
- What other self-care measures might help me?
- What is the long-term outlook in my case?
- Should I see a specialist?
- Are there brochures or other printed material I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your doctor is likely to ask you several questions, such as:
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
What you can do in the meantime
Avoid doing anything that seems to worsen your symptoms.
Last Updated Sep 30, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use