Granuloma annulare
Overview
Granuloma annulare (gran-u-LOW-muh an-u-LAR-e) is a skin condition that causes a raised rash or bumps in a ring pattern. The most common type affects young adults, usually on the hands and feet.
Minor skin injuries and some medicines might trigger the condition. It's not contagious and usually not painful, but it can make you feel self-conscious. And if it becomes a long-term condition, it can cause emotional distress.
Treatment might clear the skin gradually, but the bumps tend to come back. Untreated, the condition might last from a few weeks to decades.
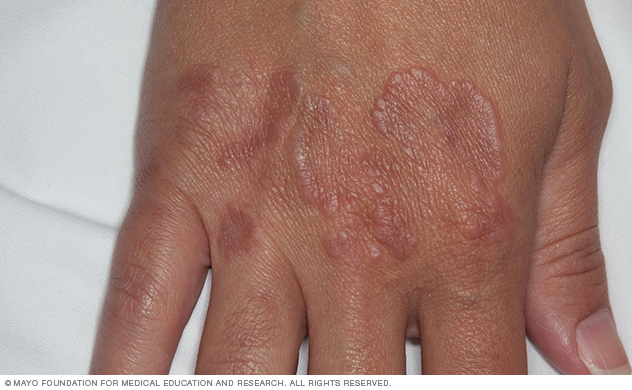
Granuloma annulare is a skin condition that causes a raised rash or bumps in a ring pattern, usually on the hands and feet.
Symptoms
The signs and symptoms of granuloma annulare can vary, depending on the type:
- Localized. This is the most common type of granuloma annulare. The rash borders are circular or semicircular, with a diameter up to 2 inches (5 centimeters). The rash occurs most commonly on the hands, feet, wrists and ankles of young adults.
- Generalized. This type is uncommon and usually affects adults. It causes bumps that form a rash on most of the body, including the trunk, arms and legs. The rash might cause discomfort or itchiness.
- Under the skin. A type that usually affects young children is called subcutaneous granuloma annulare. It produces small, firm lumps under the skin, instead of a rash. The lumps form on the hands, shins and scalp.
When to see a doctor
Call your health care provider if you develop a rash or bumps in ring pattern that don't go away within a few weeks.
Causes
It's not clear what causes granuloma annulare. Sometimes it's triggered by:
- Animal or insect bites
- Infections, such as hepatitis
- Tuberculin skin tests
- Vaccinations
- Sun exposure
- Minor skin injuries
- Medicines
Granuloma annulare is not contagious.
Risk factors
Granuloma annulare can be related to diabetes or thyroid disease, most often when you have many bumps all over the body. It may, rarely, be related to cancer, especially in older people whose granuloma annulare is severe, doesn't respond to treatment or returns after cancer treatment.
Diagnosis
Your health care provider may diagnose granuloma annulare by looking at the affected skin and taking a small skin sample (biopsy) to examine under a microscope.
Treatment
Granuloma annulare can clear on its own over time. Treatment might help clear the skin faster than if left untreated, but the condition often returns. The bumps that return after treatment tend to appear at the same spots, and 80% of those usually clear within two years.
Untreated, the condition might last a few weeks or decades.
Treatment options include:
- Corticosteroid creams or ointments. Prescription-strength products may help clear the skin faster. Your health care provider may direct you to cover the cream with bandages or an adhesive patch, to help the medicine work better.
- Corticosteroid injections. If the skin isn't clearing up with a medicated cream or ointment, your health care provider may suggest a corticosteroid injection. Repeat injections may be needed every 6 to 8 weeks until the condition clears up.
- Freezing. Applying liquid nitrogen to the affected area may help remove the bumps.
- Light therapy. Exposing the affected skin to certain types of light, including lasers, is sometimes helpful.
- Oral medicines. When the condition is widespread, your health care provider might prescribe medicine taken by mouth, such as antibiotics or antimalarials.
Coping and support
These coping methods might help ease the distress of living with granuloma annulare long term:
- Routinely reach out to friends and family members.
- Join a local or reputable internet-based support group.
Preparing for an appointment
You're likely to start by seeing your primary care provider, who may then refer you to a specialist in skin conditions (dermatologist).
What you can do
Before your appointment, you might want to list answers to the following questions:
- Have you recently traveled to a new area or spent much time outdoors?
- Do you have pets, or have you recently had contact with new animals?
- Are any family members or friends having similar symptoms?
- What medicines or supplements do you take regularly?
What to expect from your doctor
Your health care provider is likely to ask you a number of questions, such as those listed below. Being ready to answer them may reserve time to go over any points you want to spend more time on.
- When did your skin condition first appear?
- Does your rash cause any discomfort? Does it itch?
- Have your symptoms become worse or stayed the same over time?
- Have you been treating your skin condition with any medicines or creams?
- Does anything seem to improve — or worsen — your symptoms?
- Do you have any other health conditions, such as diabetes or thyroid problems?
Last Updated Jan 20, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



