Hypercalcemia
Overview
Hypercalcemia is a condition in which the calcium level in the blood becomes too high. Too much calcium in the blood can weaken bones and create kidney stones. It also can affect the heart and brain.
Most often, hypercalcemia happens after one or more of the parathyroid glands make too much hormone. These four tiny glands are in the neck, near the thyroid gland. Other causes of hypercalcemia include cancer, certain other medical conditions and some medicines. Taking too much of calcium and vitamin D supplements also can cause hypercalcemia.
Some people have no symptoms of this condition. Others have symptoms that range from mild to serious. Treatment depends on the cause.
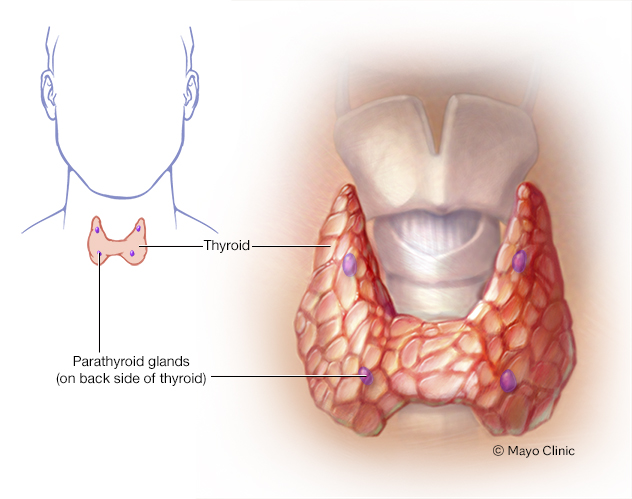
The four tiny parathyroid glands, which lie near the thyroid, make the parathyroid hormone. The hormone plays a role in controlling levels of the minerals calcium and phosphorus in the body.
Symptoms
You might not have any symptoms if your hypercalcemia is mild. If it's more serious, your symptoms are related to the parts of your body affected by high blood calcium levels. Examples include:
- Kidneys. Excess calcium makes the kidneys work harder to filter it. This can cause serious thirst and frequent urination.
- Digestive system. Hypercalcemia can cause stomach upset or pain, vomiting, and constipation.
- Bones and muscles. Most often, the extra calcium in the blood is leached from the bones. This weakens the bones. It can cause bone pain and muscle weakness.
- Brain. Hypercalcemia can affect how the brain works. That can lead to trouble focusing, confusion, drowsiness and fatigue. It also can cause depression.
- Heart. Rarely, serious hypercalcemia can affect the heart. It can cause feelings of a fast-beating, fluttering or pounding heart. It also can cause the heart to beat out of rhythm. It's linked with other heart-related conditions as well.
When to see a doctor
Call your healthcare professional if you think you have any symptoms of hypercalcemia. These can include extreme thirst, frequent urination and pain in the stomach area.
Causes
Calcium helps build strong bones and teeth. It also helps muscles contract and nerves send signals. When the parathyroid glands work right, they release hormones that help maintain the right balance of calcium in the blood. Parathyroid hormones trigger:
- Bones to release calcium into the blood.
- The digestive tract to absorb more calcium.
- The kidneys to release less calcium and activate more vitamin D. Vitamin D plays a key role in the body's ability to absorb calcium.
This delicate balance between too little calcium in the blood and hypercalcemia can be affected by various factors. Hypercalcemia can be caused by:
- Overactive parathyroid glands. This also is called hyperparathyroidism. It's the most common cause of hypercalcemia. Overactive parathyroid glands make too much parathyroid hormone. The condition can stem from a small tumor that isn't cancer. It also can stem from one or more of the four parathyroid glands becoming larger.
- Cancer. Lung cancer, breast cancer and some blood cancers can raise the risk of hypercalcemia. Cancer that spreads to the bones also raises the risk.
- Other diseases. Conditions such as tuberculosis and sarcoidosis can raise blood levels of vitamin D. That in turn spurs the digestive tract to absorb more calcium.
- Genetic factors. A rare genetic condition called familial hypocalciuric hypercalcemia causes an increase of calcium in the blood. This condition doesn't cause symptoms or complications of hypercalcemia.
- Little or no movement. People who have a condition that causes them to spend a lot of time sitting or lying down can get hypercalcemia. Over time, bones that don't bear weight release calcium into the blood.
- Serious dehydration. This is a common cause of mild or short-term hypercalcemia. Having less fluid in the blood causes a rise in calcium.
- Some medicines. Medicines such as lithium and thiazide diuretics might cause more parathyroid hormone to be released.
- Supplements. Taking too much calcium or vitamin D supplements over time can raise calcium levels in the blood.
Complications
Hypercalcemia can lead to medical conditions that include:
- Osteoporosis. This condition involves thinning bones. It could develop if the bones keep releasing calcium into the blood. Osteoporosis can lead to broken bones, curving of the spinal column and loss of height.
- Kidney stones. If the urine contains too much calcium, crystals might form in the kidneys. Over time, the crystals can combine to form kidney stones. Passing a stone can be very painful.
- Kidney failure. This condition limits the kidneys' ability to clean the blood and get rid of extra fluid. It can develop over time as hypercalcemia damages the kidneys.
- Nervous system conditions. Serious hypercalcemia can lead to confusion, dementia and coma. Coma can be fatal.
- Irregular heart rhythm. This also is called arrhythmia. Hypercalcemia can affect the electrical signals that control the heartbeat. That can cause the heart to beat out of rhythm.
Diagnosis
Hypercalcemia can cause few or no symptoms. So, you might not know you have it until routine blood tests show a high level of calcium. Blood tests also can show whether your parathyroid hormone level is high, which could be a sign of hyperparathyroidism.
If you have hypercalcemia, your healthcare professional looks for its cause. You might need imaging tests of your bones or lungs. This helps find out if the cause is a disease such as cancer or sarcoidosis.
Treatment
If your hypercalcemia is mild, you might not need treatment right away. You and your healthcare professional may wait to see if symptoms start or become worse. Your bones and kidneys might be checked over time to be sure they stay healthy.
For hypercalcemia that is more serious, your healthcare professional might recommend medicines or treatment of the underlying disease. Sometimes, treatment includes surgery.
Medications
For some people, medicines such as these may be recommended:
- Calcitonin (Miacalcin). This hormone from salmon controls calcium levels in the blood. Mild upset stomach can be a side effect.
- Calcimimetics. This type of medicine can help control overactive parathyroid glands. Cinacalcet (Sensipar) has been approved to manage hypercalcemia.
- Bisphosphonates. These osteoporosis medicines can quickly lower calcium levels when given through a vein (IV). Often, they're used to treat hypercalcemia due to cancer. Risks linked with this treatment include thigh fractures as well as breakdown of the jaw, called osteonecrosis.
- Denosumab (Prolia, Xgeva). This medicine often is used to treat people with hypercalcemia caused by cancer who don't respond well to bisphosphonates.
- Prednisone. Short-term use of steroid pills such as prednisone can help against hypercalcemia caused by high vitamin D levels.
- IV fluids and loop diuretics. Very high calcium levels can be a medical emergency. You might need treatment with IV fluids in the hospital to quickly lower your calcium level. This helps prevent heart rhythm problems or damage to the nervous system. You also might need medicines called loop diuretics if your calcium level stays high. Or you might need them if too much fluid builds up in your body.
Surgical and other procedures
Conditions linked with overactive parathyroid glands often can be cured by surgery to remove the tissue that's causing the problem. In many people, only one of the four parathyroid glands is affected. Before surgery, a special scanning test involves getting a shot with a small amount of radioactive material. The material helps pinpoint the affected gland or glands.
Preparing for an appointment
You might start by seeing your primary healthcare professional. Then you'll likely be referred to a doctor called an endocrinologist, who treats hormonal conditions.
Here's some information to help you get ready for your appointment.
What you can do
Before your appointment, make a list of:
- Your symptoms. Include any that don't seem related to the reason for your checkup. Note when they began.
- Key personal information. Include major stresses or recent life changes, your medical history, and your family's medical history.
- All medicines, vitamins and other supplements you take. Include the amounts you take, called the doses.
- Questions to ask your healthcare professional.
Take a family member or friend along if you can. That person can help you remember the information you're given.
For hypercalcemia, basic questions to ask your healthcare team include:
- What's the most likely cause of my symptoms?
- What tests do I need?
- What treatments are available, and which do you recommend?
- What side effects can I expect from treatment?
- Are there treatment options other than the one that you're suggesting?
- I have other health conditions. How can I best manage them together?
What to expect from your doctor
Your healthcare professional likely will ask you questions such as:
- Does anything improve your symptoms?
- What, if anything, makes your symptoms worse?
- Have you had kidney stones, bone fractures or osteoporosis?
- Do you have bone pain?
- Do you have unexplained weight loss?
- Have family members had hypercalcemia or kidney stones?
Last Updated Mar 8, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use