Impacted wisdom teeth
Overview
Wisdom teeth, the third molars at the back of the mouth, are the last adult teeth to come in. Most people have four wisdom teeth — two on the top and two on the bottom. When wisdom teeth become impacted, they don't have enough room to emerge or develop in the usual way.
Impacted wisdom teeth can cause pain, damage other teeth and lead to other dental problems. Sometimes they don't cause any problems. But because wisdom teeth are hard to clean, they may be more prone to tooth decay and gum disease than other teeth.
Impacted wisdom teeth that cause pain or other dental problems usually are taken out. Some dentists and oral surgeons also recommend taking out impacted wisdom teeth that don't cause symptoms to prevent future problems.
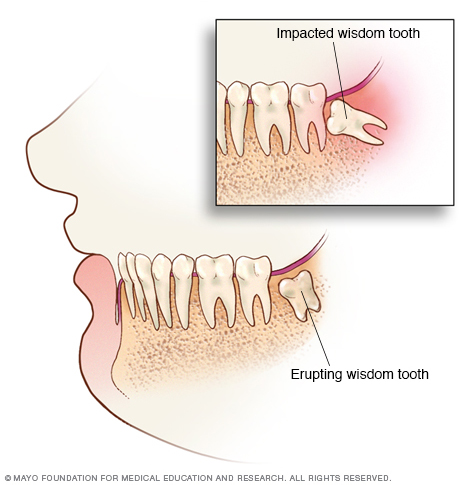
Wisdom teeth are the last of your teeth to appear (erupt) in the mouth. Sometimes a wisdom tooth becomes stuck below the surface of your gums and grows at an odd angle, possibly causing problems. This is called an impacted wisdom tooth.
Symptoms
Impacted wisdom teeth don't always cause symptoms. But when an impacted wisdom tooth becomes infected, damages other teeth or causes other dental problems, you may have some of these symptoms:
- Red or swollen gums.
- Tender or bleeding gums.
- Jaw pain.
- Swelling around the jaw.
- Bad breath.
- An unpleasant taste in your mouth.
- A hard time opening your mouth.
When to see a doctor
See your dentist if you have symptoms in the area behind your last molar that may be related to an impacted wisdom tooth.
Causes
Wisdom teeth become impacted because they don't have enough room to come in or develop in the usual way.
Wisdom teeth usually emerge sometime between the ages of 17 and 26. Some people have wisdom teeth that emerge behind the second molars without any problems and line up with the other teeth. But in many cases, the mouth is too crowded for proper development of third molars. These crowded third molars become impacted.
An impacted wisdom tooth may partially emerge so that some of the crown is visible. This is called a partially impacted wisdom tooth. If the tooth never breaks through the gums, it's called a fully impacted wisdom tooth.
Whether partially or fully impacted, the tooth may:
- Grow at an angle toward the next tooth, which is the second molar.
- Grow at an angle toward the back of the mouth.
- Grow at a right angle to the other teeth, as if the wisdom tooth is "lying down" within the jawbone.
- Grow straight up or down like other teeth but stay trapped within the jawbone.
Risk factors
Risk factors that can lead to impacted wisdom teeth include lack of space or a blockage that keeps the teeth from emerging properly.
Complications
Impacted wisdom teeth can cause several problems in the mouth, including:
- Damage to other teeth. If the wisdom tooth pushes against the second molar, it may damage the second molar or raise the risk of infection in that area. This pressure also can cause problems with crowding of the other teeth or require orthodontic treatment to straighten other teeth.
- Cysts. Wisdom teeth develop in sacs within the jawbone. The sacs can fill with fluid, forming cysts that can damage the jawbone, teeth and nerves. Rarely, a tumor develops. This type of tumor is usually noncancerous, also called benign. But tissue and bone may need to be taken out due to this problem.
- Decay. Partially impacted wisdom teeth appear to be at higher risk of getting cavities compared toother teeth. This is because the position of wisdom teeth when they are impacted makes them harder to clean. Also, food and bacteria can get trapped easily between the gum and a partially erupted tooth.
- Gum disease. It's hard to clean impacted, partially erupted wisdom teeth. So you're more likely to get a painful, inflammatory gum condition called pericoronitis (per-ih-kor-o-NI-tis) in those areas.
Prevention
You can't keep an impaction from occurring. But keeping regular six-month dental appointments for cleaning and checkups allows your dentist to watch the growth and emergence of your wisdom teeth. Regularly updated dental X-rays may show impacted wisdom teeth before any symptoms start.
Diagnosis
Your dentist or oral surgeon can look at your teeth and mouth to see if you have impacted wisdom teeth or another condition that could be causing your symptoms. Such exams typically include:
- Questions about your dental symptoms and general health.
- Checks of the condition of your teeth and gums.
- Dental X-rays that can show impacted teeth as well as symptoms of damage to teeth or bone.
Treatment
If your impacted wisdom teeth are hard to treat or if you have medical conditions that may raise surgical risks, your dentist likely will ask you to see an oral surgeon. The oral surgeon can talk with you about the best course of action.
Managing wisdom teeth without symptoms
Dental specialists disagree about whether to remove impacted wisdom teeth that aren't causing symptoms. These are called asymptomatic wisdom teeth. Many dental specialists recommend removing asymptomatic wisdom teeth in the late teens to early twenties because the risk of complications is low and the procedure typically is safer and well tolerated by younger people.
Some dentists and oral surgeons recommend taking out wisdom teeth even if they aren't causing problems to prevent potential issues in the future. They say:
- Symptom-free wisdom teeth may not be free of disease.
- If there isn't enough space for the teeth to come in, it's often hard to get to them and clean them properly.
- Serious problems with wisdom teeth happen less often in younger adults.
- The procedure is harder with age and more likely to cause problems later.
Other dentists and oral surgeons recommend a more conservative approach. They note that:
- There isn't enough evidence to suggest that impacted wisdom teeth that aren't causing problems in young adulthood will cause problems later.
- The expense and risks of the procedure don't justify the expected benefit.
With a conservative approach, your dentist watches your teeth, looking for decay, gum disease or other problems. Your dentist may recommend taking out a tooth if problems arise.
Surgery to remove wisdom teeth
Impacted wisdom teeth that cause pain or other dental problems usually are taken out with surgery, also known as extraction. Extraction of a wisdom tooth usually is needed for:
- Infection or gum disease, also known as periodontal disease, involving the wisdom teeth.
- Tooth decay in partially erupted wisdom teeth.
- Cysts or tumors involving the wisdom teeth.
- Wisdom teeth that damage nearby teeth.
- Stopping future problems.
Extraction is done mostly as an outpatient procedure, so you'll likely go home the same day. The process includes:
- Sedation or anesthesia. You may have local anesthesia, which numbs your mouth. You also may have sedation anesthesia, which lowers your awareness. Or you may be under general anesthesia, which makes you go to sleep.
- Tooth removal. During an extraction, your dentist or oral surgeon makes a cut in your gums and takes out any bone that blocks access to the impacted tooth root. After taking out the tooth, the dentist or oral surgeon typically closes the wound.
Wisdom tooth extractions may cause some pain and bleeding, as well as swelling of the site or jaw. Some people have trouble opening their mouths wide for a short time due to swelling of the jaw muscles. You'll receive instructions on how to care for wounds and manage pain and swelling, such as taking pain medicine and using cold compresses to reduce swelling.
Much less commonly, some people may have:
- Painful dry socket, which is exposure of bone if a blood clot doesn't form or comes out of the socket after surgery.
- Infection in the socket from bacteria or trapped food particles.
- Damage to nearby teeth, nerves, jawbone or sinuses.
Coping and support
Needing to have a tooth taken out may cause you to feel worried or anxious, but delaying care can lead to serious and lasting problems. It's important to talk with your dentist about your concerns. It's common to be very nervous. This is nothing to be embarrassed about. Ask your dentist for ways to ease your anxiety and discomfort.
Many dentists offer ways to ease nervousness or anxiety, such as listening to music or watching videos. You may be able to bring along a supportive family member or friend. You also can learn relaxation techniques, such as deep breathing and imagery. If you have severe anxiety, you likely will be referred to an oral surgeon. An oral surgeon can provide medicines or sedative techniques that may reduce your level of anxiety and allow for the procedure to be completed more comfortably and safely.
Preparing for an appointment
If you're having symptoms or other dental problems that may suggest an impacted wisdom tooth, see your dentist as soon as possible. Your dentist may ask you these questions:
- What symptoms are you having?
- When did your symptoms begin?
- Does anything worsen symptoms, such as chewing toward the back of your mouth?
- Have you noticed any bleeding while brushing or flossing your teeth?
- How do you usually clean your teeth?
Last Updated Feb 1, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use