Indigestion
Overview
Indigestion — also called dyspepsia or an upset stomach — is discomfort in your upper abdomen. Indigestion describes certain symptoms, such as belly pain and a feeling of fullness soon after you start eating, rather than a specific disease. Indigestion can also be a symptom of other digestive disorders.
Although indigestion is common, each person may experience indigestion in a slightly different way. Symptoms of indigestion may be felt occasionally or as often as daily.
Indigestion may often be relieved with lifestyle changes and medicines.
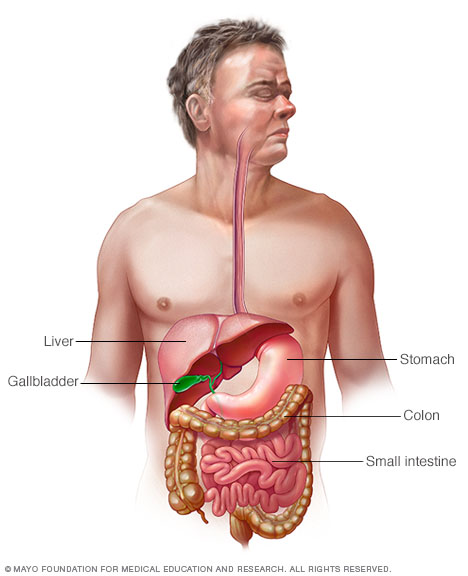
The major organs in your digestive system are the liver, stomach, gallbladder, colon and small intestine.
Symptoms
If you have indigestion, you may have:
- Early fullness during a meal. You haven't eaten much of your meal, but you already feel full and may not be able to finish eating.
- Uncomfortable fullness after a meal. The feeling of fullness lasts longer than it should.
- Discomfort in the upper abdomen. You feel a mild to severe pain in the area between the bottom of your breastbone and your bellybutton.
- Burning in the upper abdomen. You feel an uncomfortable heat or burning sensation between the bottom of your breastbone and your bellybutton.
- Bloating in the upper abdomen. You feel an uncomfortable sensation of tightness in your upper abdomen.
- Nausea. You feel as if you want to vomit.
Less frequent symptoms include vomiting and belching.
Sometimes people with indigestion also experience heartburn. Heartburn is a pain or burning feeling in the center of your chest that may radiate into your neck or back during or after eating.
When to see a doctor
Mild indigestion is usually nothing to worry about. Consult your health care provider if discomfort lasts for more than two weeks.
Contact your provider right away if pain is severe or accompanied by:
- Unintentional weight loss or loss of appetite.
- Repeated vomiting or vomiting with blood.
- Black, tarry stools.
- Trouble swallowing that gets worse.
- Fatigue or weakness, which may be signs of anemia.
Seek immediate medical attention if you have:
- Shortness of breath, sweating or chest pain radiating to the jaw, neck or arm.
- Chest pain when you're active or stressed.
Causes
Indigestion has many possible causes. Often, indigestion is related to lifestyle and may be triggered by food, drink or medicine. Common causes of indigestion include:
- Overeating or eating too quickly.
- Fatty, greasy or spicy foods.
- Too much caffeine, alcohol, chocolate or carbonated beverages.
- Smoking.
- Anxiety.
- Certain antibiotics, pain relievers and iron supplements.
A condition known as functional or nonulcer dyspepsia, which is related to irritable bowel syndrome, is a very common cause of indigestion.
Sometimes indigestion is caused by other conditions, including:
- Inflammation of the stomach, called gastritis.
- Peptic ulcers.
- Celiac disease.
- Gallstones.
- Constipation.
- Pancreas inflammation, called pancreatitis.
- Stomach cancer.
- Intestinal blockage.
- Reduced blood flow in the intestine, called intestinal ischemia.
- Diabetes.
- Thyroid disease.
- Pregnancy.
Complications
Although indigestion doesn't usually have serious complications, it can affect your quality of life by making you feel uncomfortable and causing you to eat less. You might miss work or school because of your symptoms.
Diagnosis
Your health care provider is likely to start with a health history and a thorough physical exam. Those evaluations may be enough if your indigestion is mild and you're not experiencing certain symptoms, such as weight loss and repeated vomiting.
But if your indigestion began suddenly, and you are experiencing severe symptoms or are older than age 55, your provider may recommend:
- Laboratory tests, to check for anemia or other metabolic disorders.
- Breath and stool tests, to check for Helicobacter pylori (H. pylori), the bacterium associated with peptic ulcers, which can cause indigestion.
- Endoscopy, to check for issues in your upper digestive tract, particularly in older people with symptoms that won't go away. A tissue sample, called a biopsy, may be taken for analysis.
- Imaging tests (X-ray or CT scan), to check for intestinal obstruction or another issue.
Treatment
Lifestyle changes may help ease indigestion. Your health care provider may recommend:
- Avoiding foods that trigger indigestion.
- Eating five or six small meals a day instead of three large meals.
- Reducing or eliminating the use of alcohol and caffeine.
- Avoiding certain pain relievers, such as aspirin, ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve).
- Finding alternatives for medicines that trigger indigestion.
- Controlling stress and anxiety.
If your indigestion won't go away, medicines may help. Nonprescription antacids are generally the first choice. Other options include:
- Proton pump inhibitors (PPIs), which can reduce stomach acid. PPIs may be recommended particularly if you experience heartburn along with indigestion.
- H-2-receptor blockers, which can also reduce stomach acid.
- Prokinetics, which may be helpful if your stomach empties slowly.
- Antibiotics, which can help if H. pylori bacteria are causing your indigestion.
- Antidepressants or anti-anxiety medicines, which may ease the discomfort from indigestion by decreasing your sensation of pain.
Lifestyle and home remedies
Mild indigestion can often be helped with lifestyle changes, including:
- Eating smaller, more-frequent meals. Chew your food slowly and thoroughly.
- Not eating certain foods. Fatty and spicy foods, processed foods, carbonated beverages, caffeine, alcohol, and smoking can trigger indigestion.
- Maintaining a healthy weight. Excess pounds put pressure on your abdomen, pushing up your stomach and causing acid to back up into your esophagus.
- Exercising regularly. Exercise helps you keep off extra weight and promotes better digestion.
- Managing stress. Create a calm environment at mealtime. Practice relaxation techniques, such as deep breathing, meditation or yoga. Spend time doing things you enjoy. Get plenty of sleep.
- Changing your medicines. With your health care provider's approval, stop or cut back on pain relievers or other medicines that may irritate your stomach lining. If that's not an option, be sure to take these medicines with food.
Alternative medicine
Alternative and complementary treatments have been used for many years to ease indigestion, although their effectiveness varies from person to person. These treatments include:
- Herbal therapies, including plain peppermint, or a combination of peppermint and caraway oils and the Japanese herbal formula rikkunshito.
- STW 5 (Iberogast), a liquid supplement containing extracts of nine herbs, may work by reducing the production of gastric acid.
- Acupuncture, which may work by blocking the pathways of nerves that carry sensations of pain to the brain.
- Psychological treatment, including behavior modification, relaxation techniques, cognitive behavioral therapy and hypnotherapy, is often very helpful.
Always check with your health care provider before taking any supplements to be sure you're taking a safe dose. This is also important to make sure the supplement won't react with any other medicines you're taking.
Preparing for an appointment
You're likely to start by seeing your primary health care provider, or you may be referred to a provider who specializes in digestive diseases, called a gastroenterologist. Here's some information to help you get ready for your appointment and know what to expect.
What you can do
- Be aware of any pre-appointment restrictions, such as not eating solid food on the day before your appointment.
- Write down your symptoms, including when they started and how they may have changed or worsened over time.
- Take a list of all your medicines, vitamins or supplements.
- Write down your key medical information, including other diagnosed conditions.
- Write down key personal information, including any recent changes or stressors in your life, as well as a detailed description of your typical daily diet.
- Write down questions to ask during your appointment.
Some basic questions to ask include:
- What's the most likely cause of my symptoms?
- Do you think my condition is temporary or chronic?
- What kinds of tests do I need?
- What treatments can help?
- Are there any dietary restrictions that I need to follow?
- Could any of my medications be causing my symptoms?
In addition to the questions that you've prepared, don't hesitate to ask questions during your appointment.
What to expect from your doctor
Be ready to answer questions your provider may ask:
- When did you first begin experiencing symptoms, and how severe are they?
- Have your symptoms been continuous or occasional?
- What, if anything, seems to improve or worsen your symptoms?
- What medications and pain relievers do you take?
- What do you eat and drink, including alcohol, in a typical day?
- How have you been feeling emotionally?
- Do you use tobacco? If so, do you smoke, chew or both?
- Are your symptoms better or worse on an empty stomach?
- Have you vomited blood or black material?
- Have you had any changes in your bowel habits, including stools turning black?
- Have you lost weight?
- Have you had nausea or vomiting or both?
Last Updated Feb 1, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



