Low blood pressure (hypotension)
Overview
Low blood pressure is a condition in which the force of the blood pushing against the artery walls is too low. It's also called hypotension.
Blood pressure is measured in millimeters of mercury (mm Hg). In general, low blood pressure is a reading lower than 90/60 mm Hg.
What's considered low blood pressure for one person might be OK for someone else though. Low blood pressure might cause no symptoms that you notice. Or it might cause dizziness and fainting. Sometimes, low blood pressure can be life-threatening.
The causes of low blood pressure include dehydration and other serious medical conditions. It's important to find out what's causing low blood pressure so that it can be treated, if needed.
Types
Types of low blood pressure include:
- Orthostatic hypotension, also called postural hypotension. This is a sudden drop in blood pressure when standing up after sitting or lying down. Causes include dehydration, long-term bed rest, pregnancy, certain medical conditions and some medicines. This type of low blood pressure is common in older adults.
- Postprandial hypotension. This drop in blood pressure occurs 1 to 2 hours after eating. It's most likely to affect older adults, especially those with high blood pressure. The risk also is higher for older adults with Parkinson's disease or other conditions that affect the part of the nervous system that controls automatic functions such as breathing and heart rate. This is called the autonomic nervous system. Certain lifestyle changes might help ease symptoms of postprandial hypotension. Eat small, low-carbohydrate meals, drink more water, and stay away from alcohol.
- Neurally mediated hypotension. This is a blood pressure drop that happens after standing for long amounts of time. This type of low blood pressure mostly affects young adults and children. It might result from communication trouble between the heart and the brain.
- Multiple system atrophy with orthostatic hypotension. This rare condition affects the autonomic nervous system. Multiple system atrophy with orthostatic hypotension is linked with having very high blood pressure while lying down. It also used to be called Shy-Drager syndrome.
Symptoms
Low blood pressure symptoms can include:
- Blurred or fading vision.
- Dizzy or lightheaded feelings.
- Fainting.
- Fatigue.
- Trouble concentrating.
- Upset stomach.
For some people, low blood pressure may be a symptom of an underlying health condition. That's especially so when blood pressure drops suddenly or when low blood pressure occurs with symptoms.
A sudden fall in blood pressure can be dangerous. A change of just 20 mm Hg can make you feel dizzy or faint. For example, those symptoms could happen after a drop in systolic pressure from 110 mm Hg to 90 mm Hg. And big drops can be life-threatening. These can happen for reasons such as serious bleeding, serious infections or allergic reactions.
Extreme low blood pressure can lead to a condition known as shock. Symptoms of shock include:
- Confusion, especially in older people.
- Cold, clammy skin.
- Decrease in skin color, also called pallor.
- Rapid, shallow breathing.
- Weak and rapid pulse.
When to see a doctor
If you have symptoms of extreme low blood pressure or shock, call 911 or your local emergency number.
Most healthcare professionals consider blood pressure to be too low only if it causes symptoms. Minor dizzy or lightheaded feelings from time to time can be caused by many things. Causes could include spending too much time in the sun or in a hot tub. It's important to see a healthcare professional to find out the cause of your symptoms.
If you often have low blood pressure readings but feel fine, you might not need treatment. Instead, your healthcare professional tracks your health during routine checkups. It can help to keep a record of your symptoms, when they occur and what you're doing at the time.
Causes
Low blood pressure has various causes. Some health conditions and the use of certain medicines can cause it. Other factors affect blood pressure as well.
Blood pressure is determined by the amount of blood the heart pumps and the amount of resistance to blood flow in the arteries. A blood pressure reading has two numbers:
- Top number, called systolic pressure. The top number is the pressure in the arteries when the heart beats.
- Bottom number, called diastolic pressure. The bottom number is the pressure in the arteries when the heart rests between beats.
The American Heart Association classifies healthy blood pressure as normal. Normal blood pressure usually is lower than 120/80 mm Hg.
Blood pressure varies throughout the day. It depends on:
- Body position.
- Breathing.
- Food and drink.
- Medicines.
- Physical condition.
- Stress.
- Time of day.
Blood pressure usually is lowest at night and rises sharply on waking.
Conditions that can cause low blood pressure
Medical conditions that can cause low blood pressure include:
- Pregnancy. Changes during pregnancy cause blood vessels to expand fast. The changes may cause blood pressure to drop. Low blood pressure is common in the first 24 weeks of pregnancy. After a person gives birth, blood pressure usually returns to the level that it was before pregnancy.
- Heart and heart valve conditions. A heart attack, heart failure, heart valve disease and a slow heart rate called bradycardia can cause low blood pressure.
- Hormone-related diseases, also called endocrine conditions. Conditions such as Addison's disease that affect certain glands that make key hormones may cause blood pressure to drop. Low blood sugar, also called hypoglycemia, may lower blood pressure too. So might diabetes.
- Dehydration. When the body doesn't have enough water, the amount of blood in the body declines. This can cause blood pressure to drop. Fever, vomiting, severe diarrhea, overuse of diuretic medicines and strenuous exercise can lead to dehydration.
- Blood loss. Losing a lot of blood also reduces blood volume, leading to a severe drop in blood pressure. Causes of serious blood loss include injuries and internal bleeding.
- Severe infection. When an infection in the body enters the bloodstream, it can lead to a life-threatening drop in blood pressure called septic shock. Another name for an infection that happens when germs get into the blood and spread is septicemia.
- Severe allergic reaction, also called anaphylaxis. Symptoms of a severe allergic reaction include a sudden and large drop in blood pressure.
- Lack of nutrients in the diet. Low levels of vitamin B-12, folate and iron can keep the body from making enough red blood cells. A lack of healthy red blood cells is called anemia, and it can lead to low blood pressure.
Medications that can cause low blood pressure
Some medicines can cause low blood pressure, including:
- All blood pressure medicines. These include diuretics, alpha blockers and beta blockers. Examples of diuretics are furosemide (Lasix, Furoscix) and hydrochlorothiazide (Microzide). Alpha blockers include prazosin (Minipress). Some beta blockers are atenolol (Tenormin) and propranolol (Inderal LA, Innopran XL, others).
- Medicines for Parkinson's disease, such as pramipexole (Mirapex ER) and medicines that contain levodopa (Dhivy, Duopa, others).
- Certain types of depression medicine called tricyclic antidepressants, including doxepin (Silenor) and imipramine (Tofranil).
- Medicines for erectile dysfunction, including sildenafil (Revatio, Viagra) or tadalafil (Adcirca, Alyq, others), especially when taken with the heart medicine nitroglycerin (Nitrostat, Nitro-Dur, others).
Risk factors
Anyone can have low blood pressure. Risk factors for hypotension include:
- Age. Drops in blood pressure when standing up or after eating occur mainly in adults older than 65. Neurally mediated hypotension mainly affects children and younger adults.
- Medications. Certain medicines have the potential to cause low blood pressure. These include all medicines that treat high blood pressure.
- Certain diseases. Parkinson's disease, diabetes and some heart conditions can lead to low blood pressure.
- Alcohol or illegal drugs. Either of these may raise the risk of low blood pressure.
Complications
Complications of low blood pressure can include:
- Dizzy feeling.
- Weakness.
- Fainting.
- Injury from falls.
Severely low blood pressure can lower the body's oxygen levels, which can lead to heart and brain damage.
Diagnosis
To find out if you have low blood pressure, also called hypotension, your healthcare professional gives you a physical exam. You're also asked questions about your medical history. The exam includes checking your blood pressure.
You also can measure your blood pressure at home. Checking your blood pressure at home can help your healthcare professional diagnose high blood pressure earlier than usual. Ask a member of your healthcare team to:
- Help you pick a blood pressure monitor.
- Tell you how often to check your blood pressure.
- Explain what blood pressure numbers should prompt you to call the medical office right away.
If you get a home blood pressure reading at or just below 90/60 mm Hg, it's not always a cause for concern. Your healthcare professional might tell you that the reading is OK for you, especially if you have no symptoms.
Tests
Other tests may be done to find out the cause of low blood pressure.
- Blood tests. Blood tests can help find symptoms of other conditions that can lower blood pressure. These include low blood sugar, also called hypoglycemia; high blood sugar, also called hyperglycemia or diabetes; and a low red blood cell count, also called anemia.
- Electrocardiogram (ECG or EKG). This quick and painless test measures the electrical activity of the heart. During an ECG, sensors called electrodes are attached to the chest and sometimes to the arms or legs. Wires attached to the sensors connect to a machine that displays or prints out results. An ECG shows how fast or slow the heart is beating. It can be used to detect a current or previous heart attack.
- Tilt table test. A tilt table test can study how the body reacts to changes in position. The test involves lying on a table that's tilted to raise the upper part of the body. This mimics the movement from lying down to standing up. Straps hold the body in place. Heart rate and blood pressure are tracked during the test.
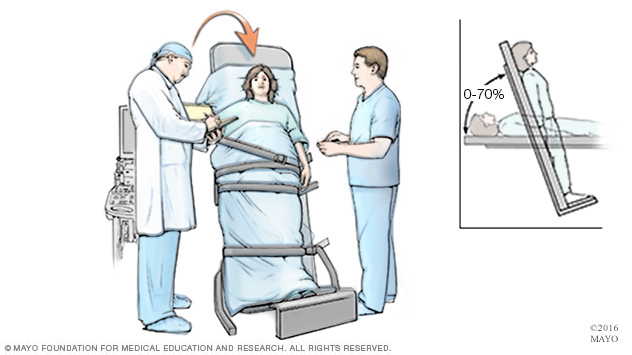
Someone having a tilt table test begins by lying flat on a table. Straps hold the person in place. After lying flat for a while, the table is tilted to a position that mimics standing. The healthcare professional watches how the heart and the nervous system that controls it respond to the changes in position.
Treatment
Low blood pressure without symptoms or with only mild symptoms rarely requires treatment.
If low blood pressure causes symptoms, the treatment depends on the cause. For instance, if medicine causes low blood pressure, your healthcare professional may recommend changing or stopping the medicine. Or the dose of medicine might be lowered. Don't change or stop taking your medicine without first talking to your healthcare professional.
If the cause of low blood pressure isn't clear or if no treatment exists, the goal is to raise blood pressure and relieve symptoms. Depending on your age, health and the type of low blood pressure you have, there are various ways to do this:
- Use more salt. Experts usually recommend limiting table salt and foods high in sodium. That's because salt and sodium can raise blood pressure, sometimes by a lot. For people with low blood pressure, though, that can be a good thing. But too much salt or sodium can lead to heart failure, especially in older adults. So it's important to check with a healthcare professional before eating more salt or high-sodium foods.
- Drink more water. Fluids increase blood volume and help prevent dehydration, both of which are important in treating hypotension.
- Wear compression stockings. Also called support stockings, these elastic stockings are often used to relieve the pain and swelling of varicose veins. They improve blood flow from the legs to the heart. Some people have an easier time using compression belts around the stomach area than they do using compression stockings. The compression belts are called abdominal binders.
Medicines. Various medicines can treat low blood pressure that occurs when standing up, also called orthostatic hypotension. For example, the drug fludrocortisone boosts blood volume. It's often used to treat orthostatic hypotension.
If you have long-term orthostatic hypotension, midodrine (Orvaten) may be prescribed to raise standing blood pressure levels. This medicine lessens the ability of the blood vessels to expand, which raises blood pressure.
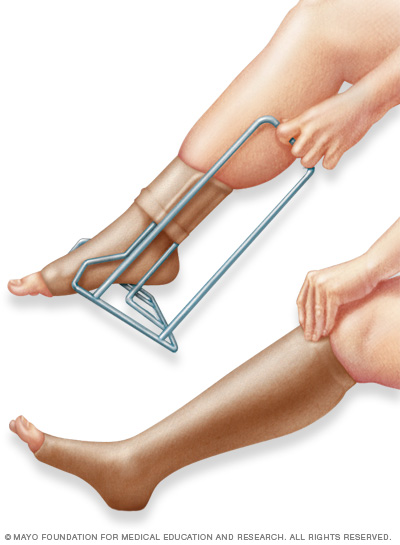
Compression stockings, also called support stockings, press on the legs, improving blood flow. A stocking butler may help with putting on the stockings.
Lifestyle and home remedies
Depending on the reason for low blood pressure, the following lifestyle and home remedies might help ease or prevent symptoms:
- Drink more water, less alcohol. Alcohol is dehydrating and can lower blood pressure, even in moderation. Water boosts the amount of blood in the body and prevents dehydration.
Pay attention to body positions. Gently move from lying flat or squatting to a standing position. Don't sit with legs crossed.
If symptoms of low blood pressure begin while standing, cross the thighs like a pair of scissors and squeeze. Or put one foot on a ledge or chair and lean as far forward as you can. These moves encourage blood flow from the legs to the heart.
Eat small, low-carb meals. To help prevent blood pressure from dropping sharply after meals, eat small meals several times a day. Limit high-carbohydrate foods such as potatoes, rice, pasta and bread.
A healthcare professional also might recommend drinking one or two strong cups of caffeinated coffee or tea with breakfast. Caffeine can cause dehydration, though, so be sure to drink plenty of water and other fluids without caffeine.
- Exercise regularly. As a general goal, work up to at least 150 minutes of moderate aerobic exercise a week. For example, you could aim to get about 30 minutes of activity most days. Also, aim to do strength-training exercises at least twice a week. But try not to exercise in hot, humid conditions.
Preparing for an appointment
You don't have to take any special steps to prepare to have your blood pressure checked. Don't stop taking medicines you think might affect your blood pressure without a healthcare professional's advice.
Here's some information to help you get ready for your appointment.
What you can do
Make a list of:
- Symptoms. Include any that do not seem related to low blood pressure, and when they occur.
- Blood pressure readings. If you track your blood pressure at home, keep a log of your blood pressure readings. Note multiple readings at different times of day. Also note when you have symptoms and whether they happened when your blood pressure was low.
- Important personal information. Include any family history of low blood pressure and major stresses or recent life changes.
- All medicines, vitamins or other supplements you use. Include the doses you take.
- Questions to ask your healthcare professional.
For low blood pressure, basic questions to ask your healthcare professional include:
- What is likely causing my symptoms or condition?
- What are other possible causes?
- What tests will I need?
- What's the most appropriate treatment?
- How often should I be screened for low blood pressure?
- I have other health conditions. How can I best manage them together?
- Are there restrictions I need to follow?
- Should I see a specialist?
- Are there brochures or other printed materials I can have? What websites do you recommend?
Feel free to ask other questions.
What to expect from your doctor
Your healthcare professional is likely to ask you questions, including:
- Do you always have symptoms of low blood pressure, or do they come and go?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to make your symptoms worse?
- Do you have a family history of heart disease?
Last Updated Jun 13, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use