Microscopic colitis
Overview
Microscopic colitis is swelling and irritation, called inflammation, of the large intestine. This large intestine is also called the colon. Microscopic colitis causes symptoms of watery diarrhea.
The condition gets its name from needing to look at colon tissue under a microscope to diagnose it. The tissue appears typical on exam with a colonoscopy or flexible sigmoidoscopy.
There are two subtypes of microscopic colitis:
- Collagenous colitis, in which a thick layer of protein called collagen grows in colon tissue.
- Lymphocytic colitis, in which white blood cells called lymphocytes increase in colon tissue.
Researchers believe collagenous (kuh-LAYJ-uh-nus) colitis and lymphocytic colitis may be forms of the same condition. Symptoms, testing and treatment are the same for both subtypes.
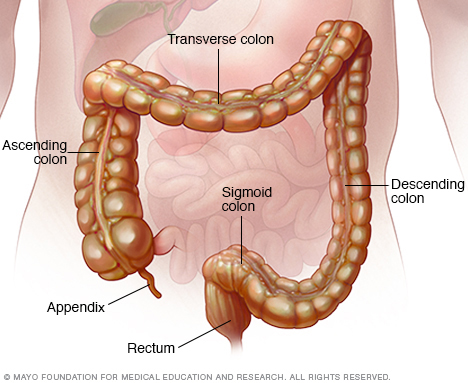
The colon is a long tube-like organ in the abdomen. It's the largest part of the large intestine. The colon carries waste to be expelled from the body. The rectum makes up the last several inches of the colon.
Symptoms
Symptoms of microscopic colitis include:
- Watery diarrhea.
- Belly pain, cramps or bloating.
- Weight loss.
- Nausea.
- Not being able to control bowel movements, called fecal incontinence.
- The body not having enough water, called dehydration.
The symptoms of microscopic colitis can come and go. At times, symptoms improve on their own.
When to see a doctor
If you have watery diarrhea that lasts more than a few days, contact your healthcare professional to diagnose and treat your condition.
Causes
It's not clear what causes the swelling and irritation, called inflammation, of the colon found in microscopic colitis. Researchers believe that the causes may include:
- Medicines that can inflame the lining of the colon.
- Bile acid not absorbed as it should be that inflames the lining of the colon.
- Bacteria that make toxins or viruses that interact with the lining of the colon.
- Autoimmune disease linked to microscopic colitis, such as rheumatoid arthritis, celiac disease or psoriasis. Autoimmune disease happens when the body's immune system attacks healthy tissues.
Risk factors
Risk factors for microscopic colitis include:
- Age. Microscopic colitis is most common in people older than age 50.
- Sex. Women are more likely to have microscopic colitis than are men. Some studies suggest a link between post-menopausal hormone therapy and microscopic colitis.
- Autoimmune disease. People with microscopic colitis sometimes also have an autoimmune disorder, such as celiac disease, thyroid disease, rheumatoid arthritis, type 1 diabetes or psoriasis.
- Genetic link. Research suggests that there may be a link between microscopic colitis and a family history of irritable bowel syndrome.
- Smoking. Recent research studies have shown a link between tobacco smoking and microscopic colitis, mostly in people ages 16 to 44.
Some research studies show a link between using certain medicines that may increase the risk of microscopic colitis. But not all studies agree.
Medicines that may be linked to the condition include:
- Pain relievers, such as aspirin, ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve).
- Proton pump inhibitors including lansoprazole (Prevacid), esomeprazole (Nexium), pantoprazole (Protonix), rabeprazole (Aciphex), omeprazole (Prilosec) and dexlansoprazole (Dexilant).
- Selective serotonin reuptake inhibitors (SSRIs) such as sertraline (Zoloft).
- Acarbose.
- Flutamide.
- Ranitidine.
- Carbamazepine (Carbatrol, Tegretol, others).
- Clozapine (Clozaril, Versacloz).
- Entacapone (Comtan).
- Paroxetine (Paxil).
- Simvastatin (Flolipid, Zocor).
- Topiramate (Topamax, Qsymia, others).
Complications
There are minimal complications for most people once microscopic colitis is successfully treated. The condition does not increase the risk of colon cancer.
Diagnosis
A complete medical history, physical exam and testing can help tell whether other conditions, such as celiac disease, may be causing diarrhea. Your healthcare professional also will ask about medicines you take.
Tests
To help confirm a diagnosis of microscopic colitis, you may have one or more of the following tests and procedures:
-
Colonoscopy and biopsies. This exam allows your healthcare professional to view your entire colon using a thin, flexible, lighted tube with an attached camera, called a colonoscope. The camera sends pictures of your rectum and entire colon to a monitor. This lets your healthcare professional see the intestinal lining.
The healthcare professional also can put instruments through the tube to take a tissue sample, called a biopsy, to study under a microscope.
-
Flexible sigmoidoscopy. This procedure is like a colonoscopy. But rather than showing the entire colon, a flexible sigmoidoscopy allows your healthcare professional to see the inside of the rectum and most of the sigmoid colon. This is about the last 1 to 2 feet (30 to 60 centimeters) of the large intestine.
The healthcare professional uses a slender, lighted tube, called a sigmoidoscope, to look at the intestinal lining. A tissue sample is taken through the scope during the exam to look for microscopic colitis.
Intestinal tissues often appear typical in microscopic colitis. So a colon tissue sample, called a biopsy, taken during a colonoscopy or flexible sigmoidoscopy is needed to confirm a diagnosis.
In both subtypes of microscopic colitis, cells in colon tissue can be seen under the microscope to make a diagnosis.
Other testing
Besides a colonoscopy or flexible sigmoidoscopy, you may have one or more of these tests to rule out other causes for your symptoms.
- Stool sample study to help rule out infection as the cause of the diarrhea.
- Blood test to look for signs of anemia or celiac disease.
- Upper endoscopy with biopsy to rule out celiac disease. Healthcare professionals use a long, thin tube with a camera on the end to look at the upper digestive tract. They may remove a tissue sample, called a biopsy, for study in a lab.
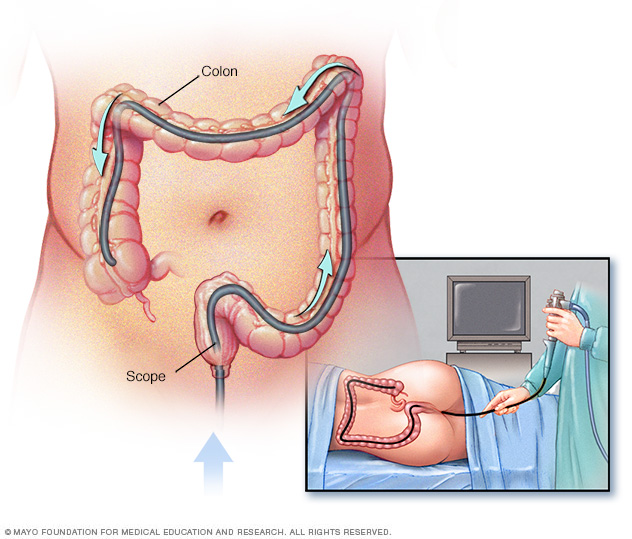
During a colonoscopy, the healthcare professional puts a colonoscope into the rectum to check the entire colon.
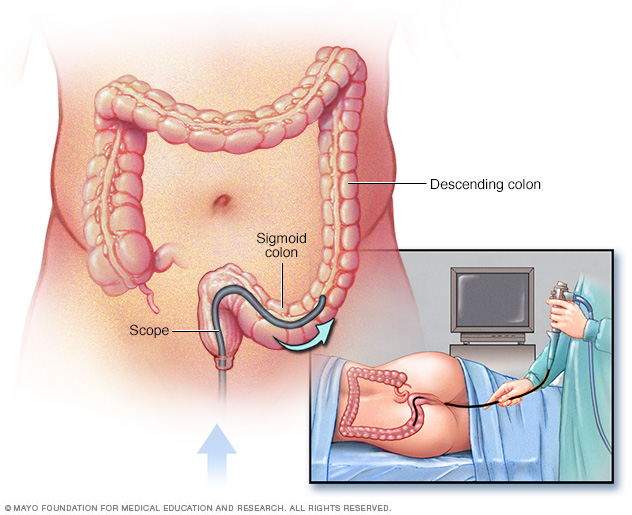
During a flexible sigmoidoscopy exam, the healthcare professional puts a sigmoidoscope into the rectum to check the lower colon.
Treatment
Microscopic colitis may get better on its own. But when symptoms are severe or don't go away, you may need treatment to relieve them. Healthcare professionals most often start with the simplest treatments that are least likely to cause side effects.
Diet and stopping certain medicines
Treatment usually begins with changes to your diet and medicines that may help relieve diarrhea. Your healthcare professional might suggest that you:
- Eat a low-fat, low-fiber diet. Foods that have less fat and are low in fiber may help relieve diarrhea in the short term. But this diet may not help with microscopic colitis in the long term.
- Limit dairy products, gluten, caffeine and sugar. These foods may make your symptoms worse.
- Stop taking any medicines that might be a cause of your symptoms. You might have to switch to another medicine to treat a condition.
Medications
If you keep having symptoms, your healthcare professional may suggest:
- Anti-diarrheal medicines such as loperamide (Imodium) or bismuth subsalicylate (Pepto-Bismol).
- Steroids such as budesonide (Entocort EC, Ortikos, others).
- Medicines that block bile acids, such as cholestyramine/aspartame or cholestyramine (Locholest, Prevalite), or colestipol (Colestid).
- Medicines that suppress the immune system to help reduce swelling and irritation in the colon, such as mercaptopurine (Purinethol) and azathioprine (Azasan, Imuran).
- Biologic medicines, such as infliximab (Remicade), adalimumab (Humira) or vedolizumab (Entyvio). These can reduce swelling and irritation in the colon.
Surgery
Very rarely, when the symptoms of microscopic colitis are severe and medicines don't work, your healthcare professional may suggest surgery to remove all or part of your colon.
Lifestyle and home remedies
Changes to your diet may help relieve the diarrhea of microscopic colitis. Try to:
- Drink plenty of fluids. Water is best, but fluids with added sodium and potassium, called electrolytes, may help as well. Try drinking broth or watered-down fruit juice. Don't drink beverages that are high in sugar or sorbitol or contain alcohol or caffeine, such as coffee, tea and colas. These can make symptoms worse.
- Choose soft, easy-to-digest foods. These include applesauce, bananas, melons and rice. Don't eat high-fiber foods such as beans and nuts. Eat only well-cooked vegetables. If you think your symptoms are getting better, slowly add high-fiber foods back to your diet. Talk to your healthcare professional about how long to continue this type of diet.
- Eat several small meals rather than a few large meals. Spacing meals throughout the day may ease diarrhea.
- Avoid irritating foods. Stay away from spicy, fatty or fried foods and any other foods that make your symptoms worse.
Preparing for an appointment
Here's some information to help you get ready for your appointment.
What you can do
- Be aware of anything you shouldn't do before your appointment. This might include eating solid food on the day before your appointment.
- Write down your symptoms, including when they started and how they have changed or worsened over time.
- Make a list of all your medicines, vitamins or supplements, including doses.
- Write down your key medical information, including other conditions you have. Also note if you have been in a hospital in the last few months.
- Write down key personal information, including any recent changes or stressors in your life. Include details of your daily diet, including whether you usually use caffeine and alcohol.
- Write down questions to ask your healthcare professional.
Questions to ask your doctor
Some basic questions to ask your healthcare professional include:
- What is the most likely cause of my condition?
- Do you think my condition will go away or last?
- What kinds of tests do I need?
- What treatments can help?
- Are there any other medical problems I might have that are linked to microscopic colitis?
- If I need surgery, what will my recovery be like?
- Are there foods and drinks I need to avoid? Would changing my diet help?
Don't hesitate to ask questions anytime you don't understand something.
What to expect from your doctor
Your healthcare professional is likely to ask you:
- When did your symptoms begin?
- Have your symptoms been ongoing, or do they come and go?
- How many loose bowel movements are you having each day?
- How severe are your other symptoms, such as abdominal cramping and nausea?
- Has there been blood in your stools?
- Have you lost any weight?
- Have you traveled recently?
- Is anyone else sick at home with diarrhea?
- Have you been to a hospital or taken antibiotics in the last few months?
- Does anything make your diarrhea worse, such as certain foods?
- What medicines are you taking? Did you start taking any in the weeks before your diarrhea began?
- What do you eat in a typical day?
- Do you use caffeine or alcohol? How much?
- Do you have celiac disease? If so, are you eating a gluten-free diet?
- Do you have diabetes or thyroid disease?
- What, if anything, seems to improve your symptoms?
- What, if anything, seems to worsen your symptoms?
What you can do in the meantime
You may find some relief from diarrhea by making changes to your diet:
- Eat bland, low-fat foods.
- Don't have dairy products, spicy foods, caffeine and alcohol.
Last Updated Jan 16, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



