Muscle cramp
Overview
A muscle cramp is a sudden, unexpected tightening of one or more muscles. Sometimes called a charley horse, a muscle cramp can be very painful. Exercising or working hard, especially in heat, can lead to muscle cramps. Some medicines and illnesses also might cause muscle cramps.
Muscle cramps aren't usually harmful. Self-care measures can treat most muscle cramps.
Symptoms
Muscle cramps occur mostly in leg muscles, most often in the calf. Cramps usually last for seconds to minutes. After the cramp eases, the area might be sore for hours or days.
When to see a doctor
Muscle cramps usually go away on their own. They don't usually need medical care. However, see a health care provider for cramps that:
- Cause severe discomfort.
- Have leg swelling, redness or skin changes.
- Come with muscle weakness.
- Happen often.
- Don't get better with self-care.
Causes
A muscle cramp can happen after working a muscle too hard or straining it, losing body fluids through sweat or simply holding a position for a long time. Often, however, the cause isn't known.
Most muscle cramps are harmless. But some might be related to a medical concern, such as:
- Not enough blood flow. A narrowing of the arteries that bring blood to the legs can cause a cramping pain in the legs and feet during exercise. These cramps usually go away soon after exercise stops.
- Nerve compression. Pressure on the nerves in the spine also can cause cramping pain in the legs. The pain usually gets worse with walking. Walking bent slightly forward, such as when pushing a shopping cart, might ease cramping.
- Not enough minerals. Too little potassium, calcium or magnesium in the diet can cause leg cramps. Medicines often prescribed for high blood pressure can cause increased urination, which may drain the body of these minerals.
Risk factors
Factors that might increase the risk of muscle cramps include:
- Age. Older people lose muscle mass. Then the muscles can't work as hard and can get stressed more easily.
- Poor conditioning. Not being in shape for an activity causes muscles to tire more easily.
- Extreme sweating. Athletes who get tired and sweat a lot while playing sports in warm weather often get muscle cramps.
- Pregnancy. Muscle cramps are common during pregnancy.
- Medical issues. Having diabetes or illnesses that involve nerves, liver or thyroid can increase the risk of muscle cramps.
- Weight. Being overweight can increase the risk of muscle cramps.
Prevention
These steps might help prevent cramps:
- Drink plenty of liquids every day. Muscles need fluids to work well. During activity, drink liquids regularly. Keep drinking water or other liquids without caffeine or alcohol after the activity.
- Stretch your muscles. Stretch gently before and after using any muscle for a time. To avoid getting leg cramps at night, stretch before bedtime. Light exercise, such as riding a stationary bicycle for a few minutes before bedtime, also may help prevent cramps while you sleep.
Treatment
Self-care measures usually can treat muscle cramps. A health care provider can show you stretching exercises that can reduce the chances of getting muscle cramps. Drinking plenty of fluids can also help prevent muscle cramps.
If you keep getting cramps that wake you from sleep, a care provider might prescribe medicine to relax muscles or help you sleep.
Lifestyle and home remedies
If you have a cramp, these actions might help:
-
Stretch and massage. Stretch the cramped muscle and gently rub it. For a calf cramp, keep the leg straight while pulling the top of your foot on the side that's cramped toward your face. Also try standing with your weight on your cramped leg and pressing down firmly. This helps ease a cramp in the back of the thigh too.
For a front thigh cramp, try pulling the foot on that leg up toward your buttock. Hold on to a chair to steady yourself.
- Apply heat or cold. Use a warm towel or heating pad on tense or tight muscles. Taking a warm bath or directing the stream of a hot shower onto the cramped muscle also can help. Rubbing the sore muscle with ice also might relieve pain.
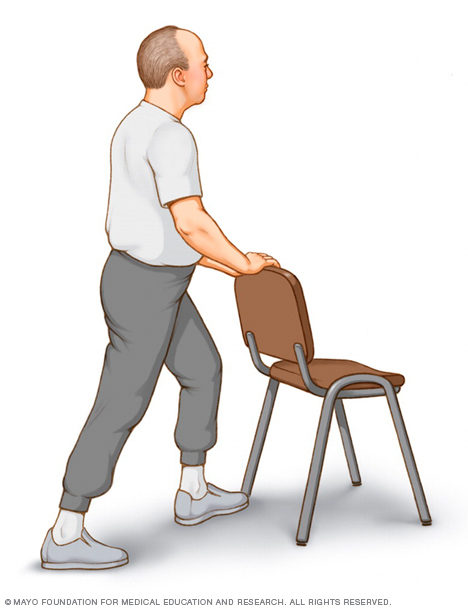
While holding on to a chair, keep one leg back with your knee straight and your heel flat on the floor. Slowly bend your elbows and front knee and move your hips forward until you feel a stretch in your calf. Hold this position for 30 to 60 seconds. Switch leg positions and repeat with your other leg.
Alternative medicine
Taking vitamin B complex and other vitamins might help manage leg cramps. Talk to your health care provider about what to take.
Preparing for an appointment
See a health care provider if you have muscle cramps often that are severe and not getting better with self-care.
Here's some information to help you get ready for your appointment.
What you can do
Make a list of:
- Your symptoms, including any that seem unrelated to the reason for your appointment, and when they began.
- Key personal information, including major stresses, recent life changes and family medical history.
- All medicines, vitamins and supplements you take, including doses.
- Questions to ask your provider.
For muscle cramps, questions to ask your provider might include:
- What's likely causing my cramps?
- Are there other possible causes?
- What tests do I need?
- What can I do about the cramping?
Ask any other questions you have.
What to expect from your doctor
Your provider is likely to ask you questions, including:
- How often do you get cramps and how bad are they?
- What, if anything, do you do before you get a cramp? Do cramps usually happen after exercise?
- Do you get cramps while resting?
- Does stretching help your cramps?
- Do you have other symptoms, such as muscle weakness or numbness?
- Have you noticed changes in your urine after exercise?
Last Updated Mar 7, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use