Myocardial ischemia
Overview
Myocardial ischemia occurs when blood flow to your heart is reduced, preventing the heart muscle from receiving enough oxygen. The reduced blood flow is usually the result of a partial or complete blockage of your heart's arteries (coronary arteries).
Myocardial ischemia, also called cardiac ischemia, reduces the heart muscle's ability to pump blood. A sudden, severe blockage of one of the heart's artery can lead to a heart attack. Myocardial ischemia might also cause serious abnormal heart rhythms.
Treatment for myocardial ischemia involves improving blood flow to the heart muscle. Treatment may include medications, a procedure to open blocked arteries (angioplasty) or bypass surgery.
Making heart-healthy lifestyle choices is important in treating and preventing myocardial ischemia.
Symptoms
Some people who have myocardial ischemia don't have any signs or symptoms (silent ischemia).
When they do occur, the most common is chest pressure or pain, typically on the left side of the body (angina pectoris). Other signs and symptoms — which might be experienced more commonly by women, older people and people with diabetes — include:
- Neck or jaw pain
- Shoulder or arm pain
- A fast heartbeat
- Shortness of breath when you are physically active
- Nausea and vomiting
- Sweating
- Fatigue
When to see a doctor
Get emergency help if you have severe chest pain or chest pain that doesn't go away.
Causes
Myocardial ischemia occurs when the blood flow through one or more of your coronary arteries is decreased. The low blood flow decreases the amount of oxygen your heart muscle receives.
Myocardial ischemia can develop slowly as arteries become blocked over time. Or it can occur quickly when an artery becomes blocked suddenly.
Conditions that can cause myocardial ischemia include:
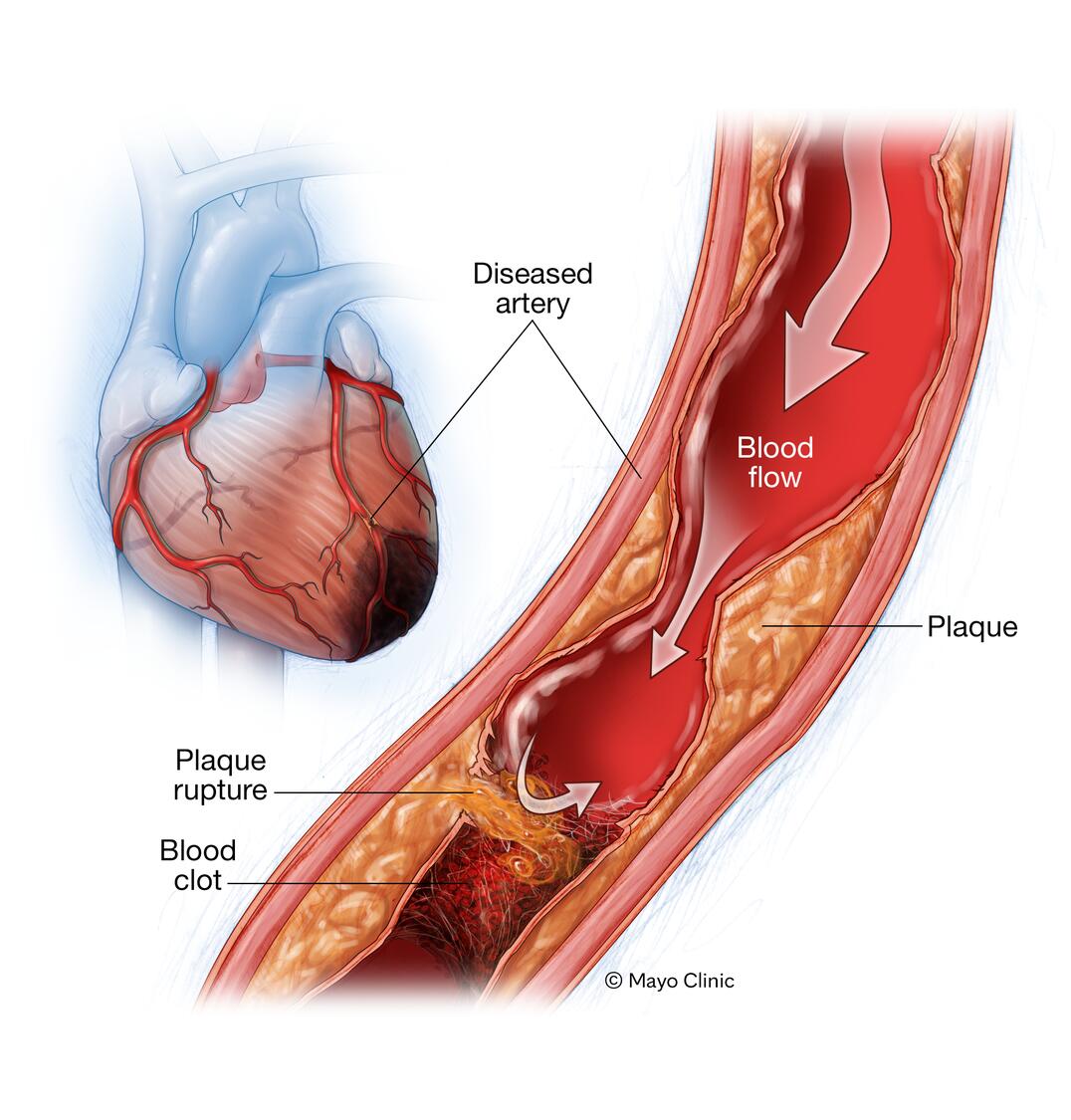
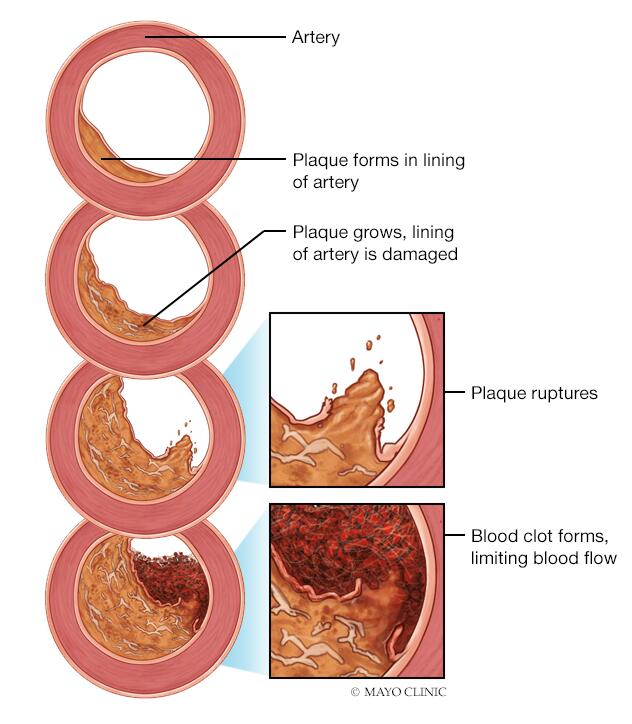
- Coronary artery disease (atherosclerosis). Plaques made up mostly of cholesterol build up on your artery walls and restrict blood flow. Atherosclerosis is the most common cause of myocardial ischemia.
- Blood clot. The plaques that develop in atherosclerosis can rupture, causing a blood clot. The clot might block an artery and lead to sudden, severe myocardial ischemia, resulting in a heart attack. Rarely, a blood clot might travel to the coronary artery from elsewhere in the body.
- Coronary artery spasm. This temporary tightening of the muscles in the artery wall can briefly decrease or even prevent blood flow to part of the heart muscle. Coronary artery spasm is an uncommon cause of myocardial ischemia.
Chest pain associated with myocardial ischemia can be triggered by:
- Physical exertion
- Emotional stress
- Cold temperatures
- Cocaine use
- Eating a heavy or large meal
- Sexual intercourse
Risk factors
Factors that can increase your risk of developing myocardial ischemia include:
- Tobacco. Smoking and long-term exposure to secondhand smoke can damage the inside walls of arteries. The damage can allow deposits of cholesterol and other substances to collect and slow blood flow in the coronary arteries. Smoking causes the coronary arteries to spasm and may also increase the risk of blood clots.
- Diabetes. Type 1 and type 2 diabetes are linked to an increased risk of myocardial ischemia, heart attack and other heart problems.
- High blood pressure. Over time, high blood pressure can accelerate atherosclerosis, resulting in damage to the coronary arteries.
- High blood cholesterol level. Cholesterol is a major part of the deposits that can narrow your coronary arteries. A high level of "bad" (low-density lipoprotein, or LDL) cholesterol in your blood may be due to an inherited condition or a diet high in saturated fats and cholesterol.
- High blood triglyceride level. Triglycerides, another type of blood fat, also may contribute to atherosclerosis.
- Obesity. Obesity is associated with diabetes, high blood pressure and high blood cholesterol levels.
- Waist circumference. A waist measurement of more than 35 inches (89 centimeters) for women and 40 inches (102 cm) in men increases the risk of high blood pressure, diabetes, and heart disease.
- Lack of physical activity. Not getting enough exercise contributes to obesity and is linked to higher cholesterol and triglyceride levels. People who get regular aerobic exercise have better heart health, which is associated with a lower risk of myocardial ischemia and heart attack. Exercise also reduces blood pressure.
Complications
Myocardial ischemia can lead to serious complications, including:
- Heart attack. If a coronary artery becomes completely blocked, the lack of blood and oxygen can lead to a heart attack that destroys part of the heart muscle. The damage can be serious and sometimes fatal.
- Irregular heart rhythm (arrhythmia). An abnormal heart rhythm can weaken your heart and may be life-threatening.
- Heart failure. Over time, repeated episodes of ischemia may lead to heart failure.
Prevention
The same lifestyle habits that can help treat myocardial ischemia can also help prevent it from developing in the first place. Leading a heart-healthy lifestyle can help keep your arteries strong, elastic and smooth, and allow for maximum blood flow.
Diagnosis
Your doctor will start by asking questions about your medical history and with a physical exam. After that, your doctor might recommend:
- Electrocardiogram (ECG). Electrodes attached to your skin record the electrical activity of your heart. Certain changes in your heart's electrical activity may be a sign of heart damage.
- Stress test. Your heart rhythm, blood pressure and breathing are monitored while you walk on a treadmill or ride a stationary bike. Exercise makes your heart pump harder and faster than usual, so a stress test can detect heart problems that might not be noticeable otherwise.
- Echocardiogram. Sound waves directed at your heart from a wand-like device held to your chest produce video images of your heart. An echocardiogram can help identify whether an area of your heart has been damaged and isn't pumping normally.
- Stress echocardiogram. A stress echocardiogram is similar to a regular echocardiogram, except the test is done after you exercise in the doctor's office on a treadmill or stationary bike.
- Nuclear stress test. Small amounts of radioactive material are injected into your bloodstream. While you exercise, your doctor can watch as it flows through your heart and lungs — allowing blood-flow problems to be identified.
- Coronary angiography. A dye is injected into the blood vessels of your heart. Then a series of X-ray images (angiograms) are taken, showing the dye's path. This test gives your doctor a detailed look at the inside of your blood vessels.
- Cardiac CT scan. This test can determine if you have a buildup of calcium in your coronary arteries — a sign of coronary atherosclerosis. The heart arteries can also be seen using CT scanning (coronary CT angiogram).
Treatment
The goal of myocardial ischemia treatment is to improve blood flow to the heart muscle. Depending on the severity of your condition, your doctor may recommend medications, surgery or both.
Medications
Medications to treat myocardial ischemia include:
- Aspirin. A daily aspirin or other blood thinner can reduce your risk of blood clots, which might help prevent blockage of your coronary arteries. Ask your doctor before starting to take aspirin because it might not be appropriate if you have a bleeding disorder or if you're already taking another blood thinner.
- Nitrates. These medications widen arteries, improving blood flow to and from your heart. Better blood flow means your heart doesn't have to work as hard.
- Beta blockers. These medications help relax your heart muscle, slow your heartbeat and decrease blood pressure so blood can flow to your heart more easily.
- Calcium channel blockers. These medications relax and widen blood vessels, increasing blood flow in your heart. Calcium channel blockers also slow your pulse and reduce the workload on your heart.
- Cholesterol-lowering medications. These medications decrease the primary material that deposits on the coronary arteries.
- Angiotensin-converting enzyme (ACE) inhibitors. These medications help relax blood vessels and lower blood pressure. Your doctor might recommend an ACE inhibitor if you have high blood pressure or diabetes in addition to myocardial ischemia. ACE inhibitors may also be used if you have heart failure or if your heart doesn't pump blood effectively.
- Ranolazine (Ranexa). This medication helps relax your coronary arteries to ease angina. Ranolazine may be prescribed with other angina medications, such as calcium channel blockers, beta blockers or nitrates.
Procedures to improve blood flow
Sometimes, more-aggressive treatment is needed to improve blood flow. Procedures that may help include:
- Angioplasty and stenting. A long, thin tube (catheter) is inserted into the narrowed part of your artery. A wire with a tiny balloon is threaded into the narrowed area and inflated to widen the artery. A small wire mesh coil (stent) is usually inserted to keep the artery open.
- Coronary artery bypass surgery. A surgeon uses a vessel from another part of your body to create a graft that allows blood to flow around the blocked or narrowed coronary artery. This type of open-heart surgery is usually used only for people who have several narrowed coronary arteries.
- Enhanced external counterpulsation. This noninvasive outpatient treatment might be recommended if other treatments haven't worked. Cuffs that have been wrapped around your legs are gently inflated with air then deflated. The resulting pressure on your blood vessels can improve blood flow to the heart.
Self care
Lifestyle changes are an important part of treatment. To follow a heart-healthy lifestyle:
- Quit smoking. Talk to your doctor about smoking cessation strategies. Also try to avoid secondhand smoke.
- Manage underlying health conditions. Treat diseases or conditions that can increase your risk of myocardial ischemia, such as diabetes, high blood pressure and high blood cholesterol.
- Eat a healthy diet. Limit saturated fat and eat lots of whole grains, fruits and vegetables. Know your cholesterol numbers and ask your doctor if you've reduced them to the recommended level.
- Exercise. Talk to your doctor about starting a safe exercise plan to improve blood flow to your heart.
- Maintain a healthy weight. If you're overweight, talk to your doctor about weight-loss options.
- Decrease stress. Practice healthy techniques for managing stress, such as muscle relaxation and deep breathing.
It's important to have regular medical checkups. Some of the main risk factors for myocardial ischemia — high cholesterol, high blood pressure and diabetes — have no symptoms in the early stages. Early detection and treatment can set the stage for a lifetime of better heart health.
Preparing for your appointment
If you are experiencing chest pain, you likely will be examined and treated in the emergency room.
If you don't have chest pain but are having other symptoms, or are concerned about your risk of myocardial ischemia, you might be referred to a heart specialist (cardiologist).
What you can do
- Be aware of any pre-appointment restrictions, such as fasting before a blood test.
- Write down your symptoms, including any that may seem unrelated to the reason why you scheduled the appointment.
- Make a list of all your medications, vitamins and supplements.
- Write down your key medical information, including other conditions.
- Write down key personal information, including any recent changes or stressors in your life.
- Write down questions to ask your doctor.
- Ask a relative or friend to accompany you, to help you remember what the doctor says.
Questions to ask your doctor
- What's the most likely cause of my symptoms?
- What tests do I need? Is there any special preparation for them?
- What kinds of treatments do I need?
- Should I make any lifestyle changes? What would be an appropriate diet and level of activity for me?
- How frequently should I be screened for heart disease?
- I have other health problems. How can I best manage these conditions together?
In addition to the questions that you've prepared to ask your doctor, don't hesitate to ask other questions during your appointment.
What to expect from your doctor
Your doctor is likely to ask you a number of questions. Being ready to answer them may leave time to go over points you want to spend more time on. You may be asked:
- What are your symptoms, and when did they begin?
- How severe are your symptoms? Are they occasional or continuous?
- Does anything improve or worsen your symptoms?
- Do you have a family history of heart disease, high blood pressure or high cholesterol?
- Do you or did you smoke?
Last Updated May 5, 2021
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use