Periodontitis
Overview
Periodontitis (per-e-o-don-TIE-tis), also called gum disease, is a serious gum infection that damages the soft tissue around teeth. Without treatment, periodontitis can destroy the bone that supports your teeth. This can cause teeth to loosen or lead to tooth loss.
Periodontitis is common but can usually be prevented. It's often the result of not taking care of your mouth and teeth. To help prevent periodontitis or improve your chance of successful treatment, brush at least twice a day, floss daily and get regular dental checkups.
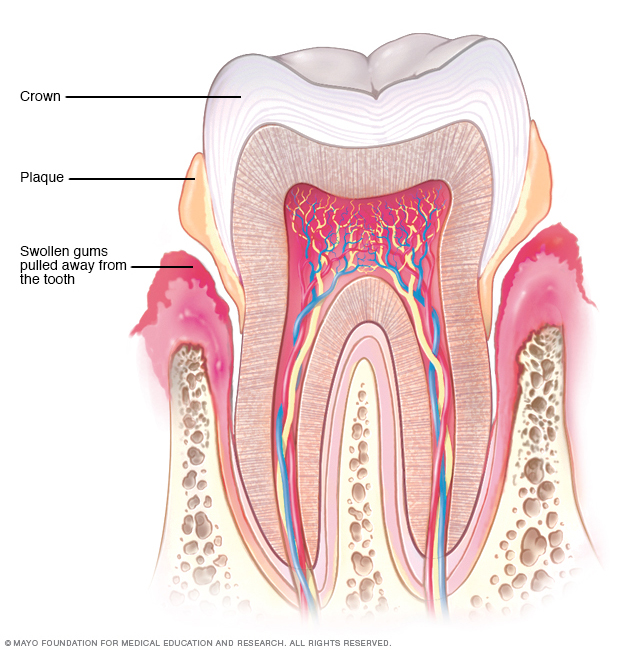
Periodontitis is a severe gum infection that can lead to tooth loss, bone loss and other serious health complications.
Symptoms
Healthy gums are firm and fit snugly around teeth. The color of healthy gums can vary. They may range from light pink in some people to dark pink and brown in others.
Symptoms of periodontitis can include:
- Swollen or puffy gums.
- Bright red, dark red or dark purple gums.
- Gums that feel tender when touched.
- Gums that bleed easily.
- A toothbrush that looks pink after brushing your teeth.
- Spitting out blood when brushing or flossing your teeth.
- Bad breath that won't go away.
- Pus between your teeth and gums.
- Loose teeth or loss of teeth.
- Painful chewing.
- New spaces that develop between your teeth that look like black triangles.
- Gums that pull away from your teeth, making your teeth look longer than usual, called receding gums.
- A change in the way your teeth fit together when you bite.
When to see a dentist
Follow your dentist's recommended schedule for regular checkups. If you notice any symptoms of periodontitis, make an appointment with your dentist as soon as possible. The sooner you get care, the better your chances of reversing damage from periodontitis.
Causes
In most cases, the development of periodontitis starts with plaque. Plaque is a sticky film mainly made up of bacteria. If not treated, here's how plaque can advance over time to periodontitis:
- Plaque forms on your teeth when starches and sugars in food interact with bacteria commonly found in your mouth. Brushing your teeth twice a day and flossing once a day removes plaque, but plaque quickly comes back.
- Plaque can harden under your gumline into tartar if it stays on your teeth. Tartar is more difficult to remove. You can't get rid of it by brushing and flossing — you need a professional dental cleaning to remove it. Because plaque and tartar are filled with bacteria, the longer they stay on your teeth, the more damage they can do.
- Plaque can cause gingivitis, the mildest form of gum disease. Gingivitis is irritation and swelling of the gum tissue around the base of your teeth. Gingiva is another word for gum tissue. Gingivitis can be reversed with professional treatment and good home oral care, but only if treated early before you have bone loss.
- Ongoing gum irritation and swelling, called inflammation, can cause periodontitis. Eventually this causes deep pockets to form between your gums and teeth. These pockets fill with plaque, tartar and bacteria and become deeper over time. If not treated, these deep infections cause a loss of tissue and bone. Eventually you may lose one or more teeth. Also, ongoing inflammation can put a strain on your immune system, causing other health problems.
Risk factors
Factors that can increase your risk of periodontitis include:
- Gingivitis.
- Poor oral health care habits.
- Smoking or chewing tobacco.
- Hormonal changes, such as those related to pregnancy or menopause.
- Recreational drug use, such as smoking marijuana or vaping.
- Obesity.
- Poor nutrition, including a low vitamin C level.
- Genetics.
- Certain medicines that cause dry mouth or gum changes.
- Conditions that lower immunity, such as leukemia, HIV/AIDS and cancer treatment.
- Certain diseases, such as diabetes, rheumatoid arthritis and Crohn's disease.
Complications
Periodontitis can cause tooth loss. The bacteria that cause periodontitis can enter your bloodstream through gum tissue, possibly affecting other parts of your body. For example, periodontitis is linked with respiratory disease, rheumatoid arthritis, coronary artery disease, preterm birth and low birth weight, and problems controlling blood sugar in diabetes.
Prevention
The best way to prevent periodontitis is to get into the habit of taking good care of your mouth and teeth. Start this routine at a young age and keep it throughout life.
- Good oral care. This means brushing your teeth for two minutes at least twice a day — in the morning and before going to bed — and flossing at least once a day. Flossing before you brush allows you to clean away the loosened food bits and bacteria. Good oral care keeps your teeth and gums clean and removes the bacteria that cause periodontal disease.
- Regular dental visits. See your dentist regularly for cleanings, usually every 6 to 12 months. If you have risk factors that increase your chance of developing periodontitis — such as having dry mouth, taking certain medicines or smoking — you may need professional cleaning more often.
Diagnosis
To tell whether you have periodontitis and how severe it is, your dentist may:
- Review your medical history to identify any factors that could be linked to your symptoms. Examples include smoking or taking certain medicines that cause dry mouth.
- Examine your mouth to look for plaque and tartar buildup and check for easy bleeding.
- Measure how deep the pockets are between your gums and teeth by placing a tiny ruler called a dental probe between your teeth and gumline. Pockets are measured at several places in your upper and lower gums. In a healthy mouth, the pocket depth is usually between 1 and 3 millimeters (mm). Pockets deeper than 4 mm may indicate periodontitis. Pockets deeper than 5 mm cannot be cleaned well with routine care.
- Take dental X-rays to check for bone loss in areas where your dentist sees deeper pockets.
Your dentist may assign a stage and a grade to periodontitis based on how severe the disease is, the complexity of treatment, your risk factors and your health. Then a treatment plan is made.
Treatment
Treatment may be done by a dentist or a periodontist. A periodontist is a dentist who specializes in gum disease. A dental hygienist may work with your dentist or periodontist as part of your treatment plan. The goal of treatment is to thoroughly clean the pockets around teeth and prevent damage to surrounding gum tissue and bone. You have the best chance for successful treatment when you also have a daily routine of good oral care, manage health conditions that may impact dental health and stop tobacco use.
Nonsurgical treatments
If periodontitis isn't advanced, treatment may involve less invasive procedures, including:
- Scaling. Scaling removes tartar and bacteria from your tooth surfaces and below your gumline. It may be done using instruments, a laser or an ultrasonic device.
- Root planing. Root planing smooths the root surfaces. This helps prevent further buildup of tartar and bacteria. It also helps your gums attach to your teeth again.
- Antibiotics. Topical or oral antibiotics can help control bacterial infection. Topical antibiotics can include antibiotic mouth rinses or putting gel containing an antibiotic into gum pockets. Sometimes oral antibiotics are needed to get of bacteria that cause infections.
Surgical treatments
If you have advanced periodontitis, you may need dental surgery, such as:
- Flap surgery, also called pocket reduction surgery. Your periodontist makes cuts in your gums to carefully fold back the tissue. This exposes the tooth roots for more effective scaling and root planing. Because periodontitis often causes bone loss, the underlying bone may be reshaped before the gum tissue is stitched back in place. After you heal, it's easier to clean the areas around your teeth and maintain healthy gum tissue.
- Soft tissue grafts. When you lose gum tissue, your gumline gets lower, exposing some of your tooth roots. You may need to have some of the damaged tissue reinforced. This is usually done by removing a small amount of tissue from the roof of your mouth or using tissue from another donor source and attaching it to the affected site. This can help reduce further gum loss, cover exposed roots and give your teeth a better appearance.
- Bone grafting. This procedure is performed when periodontitis destroys the bone around your tooth root. The graft may be made from small bits of your own bone, or the bone may be made of artificial material or donated. The bone graft helps prevent tooth loss by holding your tooth in place. It also serves as a platform for the regrowth of natural bone.
- Guided tissue regeneration. This allows the regrowth of bone that was destroyed by bacteria. In one approach, your dentist places a special type of fabric between existing bone and your tooth. The material prevents unwanted tissue from growing into the healing area, allowing bone to grow back instead.
- Tissue-stimulating proteins. Another approach involves applying a special gel to a diseased tooth root. This gel contains the same proteins found in developing tooth enamel and stimulates the growth of healthy bone and tissue.
Lifestyle and home remedies
Try these measures to reduce or prevent periodontitis:
- Brush your teeth twice a day or, better yet, after every meal or snack.
- Use a soft toothbrush and replace it at least every three months.
- Consider using an electric toothbrush, which may be more effective at removing plaque and tartar.
- Floss every day. If it's hard to use standard dental floss, try a floss holder. Other options include interdental brushes, water flossers or interdental cleaning aids designed to clean between your teeth. Talk with your dentist or dental hygienist about what would work best for you.
- Use a mouth rinse to help reduce plaque between your teeth, if recommended by your dentist.
- Get regular professional dental cleanings on a schedule recommended by your dentist.
- Don't smoke or chew tobacco.
Preparing for an appointment
You may start by seeing your general dentist. Depending on how severe your periodontitis is, your dentist may refer you to a specialist in the treatment of periodontal disease called a periodontist.
Here's some information to help you get ready for your appointment.
What you can do
Before your appointment, make a list of:
- Any symptoms you're experiencing, including any that may not seem related to the reason for your appointment.
- Key personal information, such as any medical conditions you may have.
- All medicines you take, including over-the-counter medicines, vitamins, herbs or other supplements, and the doses.
- Questions to ask your dentist.
Questions to ask your dentist may include:
- What's likely causing my symptoms?
- What kinds of tests, if any, do I need?
- What's the best plan of action?
- Will my dental insurance cover the treatments you're recommending?
- What are other options to the approach you're suggesting?
- Are there any restrictions that I need to follow?
- What steps can I take at home to keep my gums and teeth healthy?
- Are there any brochures or other printed material that I can have?
- What websites do you recommend?
Feel free to ask other questions during your appointment.
What to expect from your dentist
Your dentist may ask you questions, such as:
- When did you first start having symptoms?
- Do you have symptoms all the time or do they come and go?
- How often do you brush your teeth?
- Do you use dental floss? How often?
- How often do you see a dentist?
- What medical conditions do you have?
- What medicines do you take?
- Do you use tobacco products?
Preparing for questions will help you make the most of your time with the dentist.
Last Updated Feb 24, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use