Pilonidal cyst
Overview
A pilonidal (pie-low-NIE-dul) cyst is an unusual pocket in the skin that usually contains hair and skin debris. The cyst is almost always near the tailbone at the top of the buttocks.
Pilonidal cysts usually occur when hair punctures the skin and then becomes embedded. If a pilonidal cyst becomes infected, it can be very painful. The cyst can be drained through a small cut in the skin. Sometimes, surgery is needed.
Pilonidal cysts are most common in young adult males, and the problem tends to recur. People who sit for long periods of time are at higher risk of developing pilonidal cysts.
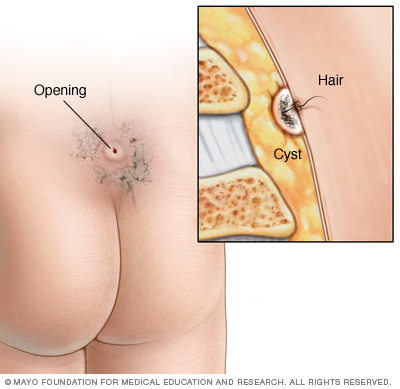
A pilonidal cyst is an unusual pocket in the skin that usually contains hair and skin debris. A pilonidal cyst is almost always near the tailbone at the top of the buttocks.
Symptoms
A pilonidal cyst may not cause symptoms. But if it's infected, the skin around the cyst may be swollen and painful. Symptoms of an infected pilonidal cyst include:
- A pit near the top of the buttocks crease.
- Pain.
- Inflamed, swollen skin.
- Pus or blood leaking from an opening in the skin.
- An odor from draining pus.
When to see a doctor
If you notice any symptoms of a pilonidal cyst, see your health care provider.
Causes
The cause of most pilonidal cysts is loose hairs that puncture the skin. Friction and pressure from rubbed skin, tight clothing, cycling or long periods of sitting can force hair into the skin.
The body creates a cyst around the hair to try to push it out. Most pilonidal cysts form on the tailbone. People who groom animals or cut hair can develop a cyst between their fingers.
Risk factors
Factors that might increase your risk of a pilonidal cyst include:
- Being a young adult white male.
- Being overweight.
- Having an inactive lifestyle.
- Sitting for long periods at a time.
- Having thick, stiff body hair.
Complications
Some people have pilonidal cysts that become infected again and again over a long time. Without treatment, these people may be at increased risk of a type of skin cancer called squamous cell carcinoma.
Prevention
To help prevent pilonidal cysts, try to:
- Wash regularly.
- Achieve or maintain a healthy weight.
- Avoid prolonged sitting.
If you've had pilonidal cysts in the past, you might want to regularly shave the affected area or use hair removal products to reduce the risk of a new cyst.
Diagnosis
Your health care provider may be able to diagnose a pilonidal cyst by asking about your symptoms, medical history and personal habits and by looking at the affected skin.
Treatment
A pilonidal cyst is usually treated in your health care provider's office. After numbing the area, your health care provider makes a small cut to drain the cysts. If the cyst returns, you may need surgery.
If you need surgery, your health care provider numbs the area and removes the cyst through an incision.
After removing the cyst, your health care provider might:
- Leave the wound open. In this option, the surgeon leaves the wound open and packs it with dressing. This allows the area to heal from the inside out. This takes longer but makes it less likely the cyst will come back.
- Close the wound with stitches. In this option, the surgeon closes the wound with stitches. This process results in a shorter healing time but has a greater risk of the cyst coming back.
Wound care is very important after surgery. Your health care provider will show you how to change dressings and explain what to expect during the healing process. You'll also be told when to call your health care provider. You may need to shave around the surgical site to prevent hairs from entering the wound.
Preparing for an appointment
You're likely to start by seeing your primary care provider. In some cases when you call to set up an appointment, you may be referred immediately to a surgeon or to a doctor who specializes in treating skin conditions, called a dermatologist.
What you can do
Before your appointment, you may want to write a list that answers the following questions:
- When did your symptoms begin?
- Have you experienced this problem before?
- Does anything improve your symptoms?
- What, if anything, appears to worsen your symptoms?
- What medications or supplements do you take regularly?
What to expect from your doctor
Your health care provider is likely to ask you a number of questions, including:
- Have you had a fever?
- Is the pain keeping you awake at night?
- What is your occupation? Do you sit all day?
Last Updated Dec 16, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



