Pneumonia
Overview
Pneumonia is an infection that inflames the air sacs in one or both lungs. The air sacs may fill with fluid or pus (purulent material), causing cough with phlegm or pus, fever, chills, and difficulty breathing. A variety of organisms, including bacteria, viruses and fungi, can cause pneumonia.
Pneumonia can range in seriousness from mild to life-threatening. It is most serious for infants and young children, people older than age 65, and people with health problems or weakened immune systems.
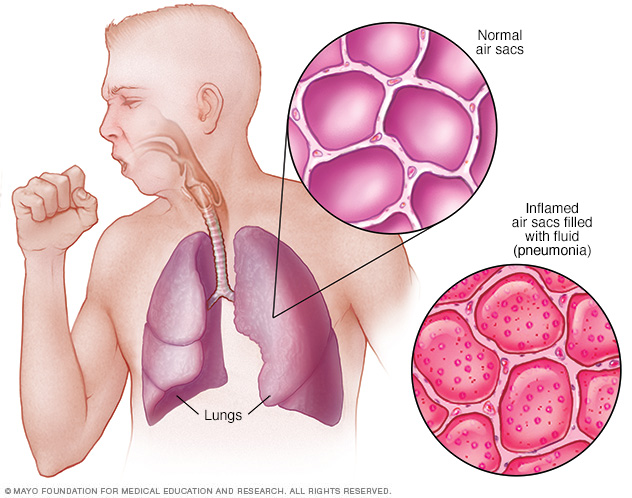
Most pneumonia occurs when a breakdown in your body's natural defenses allows germs to invade and multiply within your lungs. To destroy the attacking organisms, white blood cells rapidly accumulate. Along with bacteria and fungi, they fill the air sacs within your lungs (alveoli). Breathing may be labored. A classic sign of bacterial pneumonia is a cough that produces thick, blood-tinged or yellowish-greenish sputum with pus.
Symptoms
The signs and symptoms of pneumonia vary from mild to severe, depending on factors such as the type of germ causing the infection, and your age and overall health. Mild signs and symptoms often are similar to those of a cold or flu, but they last longer.
Signs and symptoms of pneumonia may include:
- Chest pain when you breathe or cough
- Confusion or changes in mental awareness (in adults age 65 and older)
- Cough, which may produce phlegm
- Fatigue
- Fever, sweating and shaking chills
- Lower than normal body temperature (in adults older than age 65 and people with weak immune systems)
- Nausea, vomiting or diarrhea
- Shortness of breath
Newborns and infants may not show any sign of the infection. Or they may vomit, have a fever and cough, appear restless or tired and without energy, or have difficulty breathing and eating.
When to see a doctor
See your doctor if you have difficulty breathing, chest pain, persistent fever of 102 F (39 C) or higher, or persistent cough, especially if you're coughing up pus.
It's especially important that people in these high-risk groups see a doctor:
- Adults older than age 65
- Children younger than age 2 with signs and symptoms
- People with an underlying health condition or weakened immune system
- People receiving chemotherapy or taking medication that suppresses the immune system
For some older adults and people with heart failure or chronic lung problems, pneumonia can quickly become a life-threatening condition.
Causes
Many germs can cause pneumonia. The most common are bacteria and viruses in the air we breathe. Your body usually prevents these germs from infecting your lungs. But sometimes these germs can overpower your immune system, even if your health is generally good.
Pneumonia is classified according to the types of germs that cause it and where you got the infection.
Community-acquired pneumonia
Community-acquired pneumonia is the most common type of pneumonia. It occurs outside of hospitals or other health care facilities. It may be caused by:
- Bacteria. The most common cause of bacterial pneumonia in the U.S. is Streptococcus pneumoniae. This type of pneumonia can occur on its own or after you've had a cold or the flu. It may affect one part (lobe) of the lung, a condition called lobar pneumonia.
- Bacteria-like organisms. Mycoplasma pneumoniae also can cause pneumonia. It typically produces milder symptoms than do other types of pneumonia. Walking pneumonia is an informal name given to this type of pneumonia, which typically isn't severe enough to require bed rest.
- Fungi. This type of pneumonia is most common in people with chronic health problems or weakened immune systems, and in people who have inhaled large doses of the organisms. The fungi that cause it can be found in soil or bird droppings and vary depending upon geographic location.
- Viruses, including COVID-19. Some of the viruses that cause colds and the flu can cause pneumonia. Viruses are the most common cause of pneumonia in children younger than 5 years. Viral pneumonia is usually mild. But in some cases it can become very serious. Coronavirus 2019 (COVID-19) may cause pneumonia, which can become severe.
Hospital-acquired pneumonia
Some people catch pneumonia during a hospital stay for another illness. Hospital-acquired pneumonia can be serious because the bacteria causing it may be more resistant to antibiotics and because the people who get it are already sick. People who are on breathing machines (ventilators), often used in intensive care units, are at higher risk of this type of pneumonia.
Health care-acquired pneumonia
Health care-acquired pneumonia is a bacterial infection that occurs in people who live in long-term care facilities or who receive care in outpatient clinics, including kidney dialysis centers. Like hospital-acquired pneumonia, health care-acquired pneumonia can be caused by bacteria that are more resistant to antibiotics.
Aspiration pneumonia
Aspiration pneumonia occurs when you inhale food, drink, vomit or saliva into your lungs. Aspiration is more likely if something disturbs your normal gag reflex, such as a brain injury or swallowing problem, or excessive use of alcohol or drugs.
Risk factors
Pneumonia can affect anyone. But the two age groups at highest risk are:
- Children who are 2 years old or younger
- People who are age 65 or older
Other risk factors include:
- Being hospitalized. You're at greater risk of pneumonia if you're in a hospital intensive care unit, especially if you're on a machine that helps you breathe (a ventilator).
- Chronic disease. You're more likely to get pneumonia if you have asthma, chronic obstructive pulmonary disease (COPD) or heart disease.
- Smoking. Smoking damages your body's natural defenses against the bacteria and viruses that cause pneumonia.
- Weakened or suppressed immune system. People who have HIV/AIDS, who've had an organ transplant, or who receive chemotherapy or long-term steroids are at risk.
Complications
Even with treatment, some people with pneumonia, especially those in high-risk groups, may experience complications, including:
- Bacteria in the bloodstream (bacteremia). Bacteria that enter the bloodstream from your lungs can spread the infection to other organs, potentially causing organ failure.
- Difficulty breathing. If your pneumonia is severe or you have chronic underlying lung diseases, you may have trouble breathing in enough oxygen. You may need to be hospitalized and use a breathing machine (ventilator) while your lung heals.
- Fluid accumulation around the lungs (pleural effusion). Pneumonia may cause fluid to build up in the thin space between layers of tissue that line the lungs and chest cavity (pleura). If the fluid becomes infected, you may need to have it drained through a chest tube or removed with surgery.
- Lung abscess. An abscess occurs if pus forms in a cavity in the lung. An abscess is usually treated with antibiotics. Sometimes, surgery or drainage with a long needle or tube placed into the abscess is needed to remove the pus.
Prevention
To help prevent pneumonia:
- Get vaccinated. Vaccines are available to prevent some types of pneumonia and the flu. Talk with your doctor about getting these shots. The vaccination guidelines have changed over time so make sure to review your vaccination status with your doctor even if you recall previously receiving a pneumonia vaccine.
- Make sure children get vaccinated. Doctors recommend a different pneumonia vaccine for children younger than age 2 and for children ages 2 to 5 years who are at particular risk of pneumococcal disease. Children who attend a group child care center should also get the vaccine. Doctors also recommend flu shots for children older than 6 months.
- Practice good hygiene. To protect yourself against respiratory infections that sometimes lead to pneumonia, wash your hands regularly or use an alcohol-based hand sanitizer.
- Don't smoke. Smoking damages your lungs' natural defenses against respiratory infections.
- Keep your immune system strong. Get enough sleep, exercise regularly and eat a healthy diet.
Diagnosis
Your doctor will start by asking about your medical history and doing a physical exam, including listening to your lungs with a stethoscope to check for abnormal bubbling or crackling sounds that suggest pneumonia.
If pneumonia is suspected, your doctor may recommend the following tests:
- Blood tests. Blood tests are used to confirm an infection and to try to identify the type of organism causing the infection. However, precise identification isn't always possible.
- Chest X-ray. This helps your doctor diagnose pneumonia and determine the extent and location of the infection. However, it can't tell your doctor what kind of germ is causing the pneumonia.
- Pulse oximetry. This measures the oxygen level in your blood. Pneumonia can prevent your lungs from moving enough oxygen into your bloodstream.
- Sputum test. A sample of fluid from your lungs (sputum) is taken after a deep cough and analyzed to help pinpoint the cause of the infection.
Your doctor might order additional tests if you're older than age 65, are in the hospital, or have serious symptoms or health conditions. These may include:
- CT scan. If your pneumonia isn't clearing as quickly as expected, your doctor may recommend a chest CT scan to obtain a more detailed image of your lungs.
- Pleural fluid culture. A fluid sample is taken by putting a needle between your ribs from the pleural area and analyzed to help determine the type of infection.
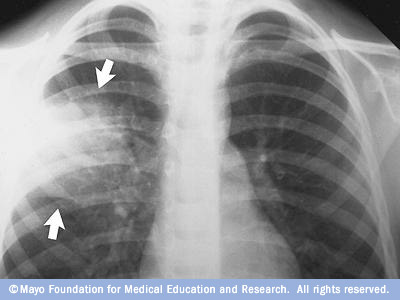
This chest X-ray shows an area of lung inflammation indicating the presence of pneumonia.
Treatment
Treatment for pneumonia involves curing the infection and preventing complications. People who have community-acquired pneumonia usually can be treated at home with medication. Although most symptoms ease in a few days or weeks, the feeling of tiredness can persist for a month or more.
Specific treatments depend on the type and severity of your pneumonia, your age and your overall health. The options include:
- Antibiotics. These medicines are used to treat bacterial pneumonia. It may take time to identify the type of bacteria causing your pneumonia and to choose the best antibiotic to treat it. If your symptoms don't improve, your doctor may recommend a different antibiotic.
- Cough medicine. This medicine may be used to calm your cough so that you can rest. Because coughing helps loosen and move fluid from your lungs, it's a good idea not to eliminate your cough completely. In addition, you should know that very few studies have looked at whether over-the-counter cough medicines lessen coughing caused by pneumonia. If you want to try a cough suppressant, use the lowest dose that helps you rest.
- Fever reducers/pain relievers. You may take these as needed for fever and discomfort. These include drugs such as aspirin, ibuprofen (Advil, Motrin IB, others) and acetaminophen (Tylenol, others).
Hospitalization
You may need to be hospitalized if:
- You are older than age 65
- You are confused about time, people or places
- Your kidney function has declined
- Your systolic blood pressure is below 90 millimeters of mercury (mm Hg) or your diastolic blood pressure is 60 mm Hg or below
- Your breathing is rapid (30 breaths or more a minute)
- You need breathing assistance
- Your temperature is below normal
- Your heart rate is below 50 or above 100
You may be admitted to the intensive care unit if you need to be placed on a breathing machine (ventilator) or if your symptoms are severe.
Children may be hospitalized if:
- They are younger than age 2 months
- They are lethargic or excessively sleepy
- They have trouble breathing
- They have low blood oxygen levels
- They appear dehydrated
Lifestyle and home remedies
These tips can help you recover more quickly and decrease your risk of complications:
- Get plenty of rest. Don't go back to school or work until after your temperature returns to normal and you stop coughing up mucus. Even when you start to feel better, be careful not to overdo it. Because pneumonia can recur, it's better not to jump back into your routine until you are fully recovered. Ask your doctor if you're not sure.
- Stay hydrated. Drink plenty of fluids, especially water, to help loosen mucus in your lungs.
- Take your medicine as prescribed. Take the entire course of any medications your doctor prescribed for you. If you stop taking medication too soon, your lungs may continue to harbor bacteria that can multiply and cause your pneumonia to recur.
Preparing for an appointment
You may start by seeing a primary care doctor or an emergency care doctor, or you may be referred to a doctor who specializes in infectious diseases or in lung disease (pulmonologist).
Here's some information to help you get ready for your appointment and know what to expect.
What you can do
- Keep a record of any symptoms, including your temperature.
- Write down key medical information, including recent hospitalizations and any medical conditions you have.
- Write down key personal information, including exposure to any chemicals or toxins, or any recent travel.
- Make a list of all medications, vitamins and supplements that you're taking, especially an antibiotic left over from a previous infection, as this can lead to a drug-resistant pneumonia.
- Bring a family member or friend along, if possible, to help you remember questions to ask and what your doctor said.
- Write down questions to ask the doctor.
Some basic questions to ask the doctor include:
- What is likely causing my symptoms?
- What kinds of tests do I need?
- What treatment do you recommend?
- Will I need to be hospitalized?
- I have other health conditions. How will my pneumonia affect them?
- Are there any restrictions that I need to follow?
Don't hesitate to ask other questions.
What to expect from the doctor
Be ready to answer questions your doctor may ask:
- When did you first start having symptoms?
- Have you had pneumonia before? If so, in which lung?
- Have your symptoms been continuous or occasional? How severe are they?
- What, if anything, seems to improve or worsen your symptoms?
- Have you traveled or been exposed to chemicals or toxic substances?
- Have you been exposed to sick people at home, school or work?
- Do you smoke? Or have you ever smoked?
- How much alcohol do you consume in a week?
- Have you had flu or pneumonia vaccines?
What you can do in the meantime
To avoid making your condition worse:
- Don't smoke or be around smoke
- Drink plenty of fluids and get plenty of rest
Last Updated Jun 13, 2020
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use