Rosacea
Overview
Rosacea (roe-ZAY-she-uh) is a common skin condition that causes flushing or long-term redness on your face. It also may cause enlarged blood vessels and small, pus-filled bumps. Some symptoms may flare for weeks to months and then go away for a while.
Rosacea can be mistaken for acne, dermatitis or other skin problems.
There's no cure for rosacea. But you may be able to control it with medicine, gentle skin care and avoiding things that cause flare-ups.
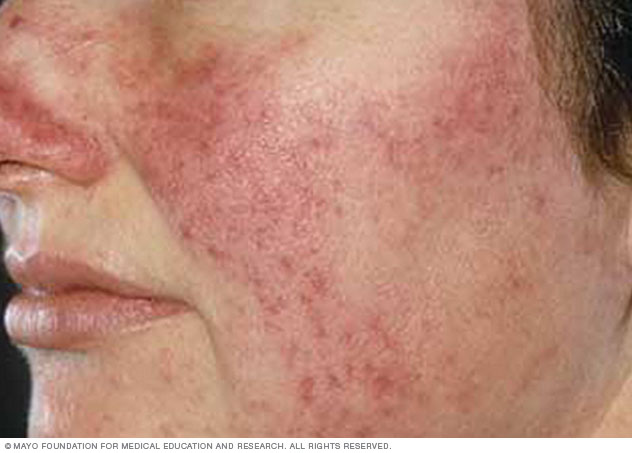
Changes typical of rosacea on white skin are red cheeks, nose and central face, with small red bumps or bumps with pus in them.
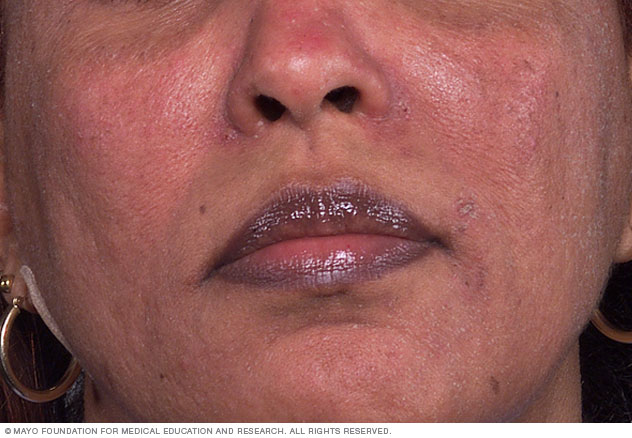
The flushing and redness of rosacea may be difficult to see on brown and Black skin. Watch for other symptoms of the condition.
Symptoms
Symptoms of rosacea include:
- Facial redness and flushing. Rosacea can make your face flush more easily. Over time, you may notice that your face stays red. Depending on skin color, redness may be subtle or look more pink or purple.
- Visible veins. Small blood vessels of the nose and cheeks break and become larger. These are also called spider veins. They may be subtle and hard to see, depending on skin color.
- Swollen bumps. Many people with rosacea develop pimples on the face that look like acne. These bumps sometimes contain pus. They also may appear on the chest and back.
- Burning sensation. The skin of the affected area may feel hot and tender.
- Eye problems. Many people with rosacea also have dry, irritated, swollen eyes and eyelids. This is known as ocular rosacea. Eye symptoms may show up before, after or at the same time as skin symptoms.
- Enlarged nose. Over time, rosacea can thicken the skin on the nose, causing the nose to look bigger. This condition also is called rhinophyma. It occurs more often in men than in women.
When to see a doctor
If you have ongoing symptoms of the face or eyes, see a healthcare professional for a diagnosis and treatment. Skin specialists also are called dermatologists.
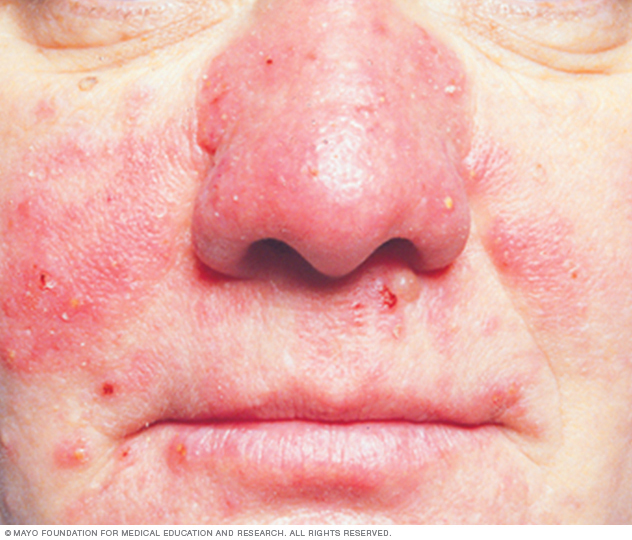
Over time, rosacea can thicken the skin on the nose, causing it to look bigger. This condition is called rhinophyma. It occurs more often in men than in women.
Causes
The cause of rosacea is not known. It could be due to genetics, an overactive immune system or things in your daily life. Rosacea is not caused by poor hygiene, and you can't catch it from other people.
Flare-ups might be brought on by:
- Sun or wind.
- Hot drinks.
- Spicy foods.
- Alcohol.
- Very hot and cold temperatures.
- Emotional stress.
- Exercise.
- Drugs that dilate blood vessels, including some blood pressure medicines.
- Some cosmetic, skin and hair care products.
Risk factors
Anyone can develop rosacea. But you may be more likely to develop it if you:
- Have skin that burns easily in the sun.
- Are between the ages of 30 to 50 years.
- Have a history of smoking.
- Have a family member with rosacea.
Diagnosis
To determine whether you have rosacea, a doctor or other healthcare professional examines your skin and asks about your symptoms. You may have tests to rule out other conditions, such as psoriasis or lupus. Some symptoms of rosacea may be harder to see on brown and Black skin. These include spider veins and flushing. So it's important to pay attention to other symptoms, such as swelling, bumps, facial stinging and dry-looking skin.
If your symptoms involve your eyes, you may see an eye doctor, also called an ophthalmologist, for other tests.
Treatment
If your symptoms don't improve with the self-care tips below, talk with a member of your healthcare team about a prescription gel or cream. This kind of medicine may help ease symptoms. For more serious rosacea, you might need prescription pills. Laser treatment may be used to reduce flushing and enlarged blood vessels in the face.
How long you need treatment depends on the type of rosacea you have and how serious your symptoms are. Even if your skin calms with treatment, the symptoms often return.
Medicines
Several medicines are used to help control rosacea symptoms. The type of medicine you are prescribed depends on your symptoms. For example, some medicines or treatments work better for flushing, and some medicines work better for pimples and bumps. You may need to try one or more medicines to find a treatment that works for you.
Medicines for rosacea include:
-
Gels or other products applied to the skin. For the flushing of mild to moderate rosacea, you may try a medicated cream or gel that you apply to the affected skin. Examples are brimonidine (Mirvaso) and oxymetazoline (Rhofade), which reduce flushing by constricting blood vessels. You may see results within 12 hours after use. The effect on the blood vessels is temporary. Overuse might lead to worse flushing. So rather than using it every day, you might use it only before important events.
Brimonidine and oxymetazoline often aren't covered by insurance.
Other prescription topical products help control the pimples of mild rosacea. Examples are azelaic acid (Azelex, Finacea), metronidazole (Metrogel, Noritate, others) and ivermectin (Soolantra). With azelaic acid and metronidazole, you may not see results for 2 to 6 weeks. Ivermectin may take even longer to improve skin. But the results tend to last longer than they do for metronidazole. Sometimes, using two or more of these products leads to the best results.
- Antibiotic medicine taken by mouth. For more serious rosacea with bumps and pimples, you may be prescribed an oral antibiotic pill such as doxycycline (Oracea, others).
- Acne medicine taken by mouth. For severe rosacea that doesn't respond to other medicine, you may be prescribed isotretinoin (Amnesteem, Claravis, others). It's a powerful oral acne medicine that also helps clear up the bumps of rosacea. This medicine is not to be taken during pregnancy as it can cause birth defects.
Laser treatment
Laser treatment can help improve the look of enlarged blood vessels. It also can help the long-term redness of rosacea. And it often works better than a cream or a pill for this symptom. Because the laser targets visible veining, this method is most effective on skin that isn't tanned, brown or Black.
Talk with a member of your healthcare team about the risks and benefits of laser treatment. Common side effects include redness, bruising and mild swelling for a few days following the treatment. Rare side effects include blistering and scarring. Icing and gentle skin care help while you heal. On brown or Black skin, laser treatment might cause long-term or permanent changes to the color of the treated skin.
The full effect of the treatment might not be seen for weeks. Repeat treatments may be needed to keep the improved look of your skin.
Laser treatment for rosacea is sometimes considered a cosmetic procedure. Such procedures often aren't covered by insurance. However, nowadays some insurances do cover the procedure. Check with your insurance company directly to see if they cover laser treatment for rosacea.
Lifestyle and home remedies
These self-care tips may help you calm your skin and prevent flare-ups:
- Identify and avoid things that make your symptoms worse. Notice what tends to cause flare-ups for you and avoid those things.
-
Protect your face. Use a broad-spectrum sunscreen or moisturizer containing sunscreen with an SPF of at least 30, even on cloudy days. Apply sunscreen generously. Reapply every two hours, or more often if you're swimming or sweating.
People with rosacea might benefit from selecting sunscreens that contain titanium dioxide, zinc or both. These are called mineral-based sunscreens or physical sunscreens. Examples include Eucerin Sensitive Mineral Zinc Oxide Protection, La Roche-Posay Tinted Mineral, and others. Or look for products with silicone, such as dimethicone, or cyclomethicone.
Apply sunscreen after you put on any medicine for your face and before applying makeup, if you use it.
Take other steps to protect your face, such as wearing a hat and avoiding midday sun. In cold, windy weather, wear a scarf or ski mask.
-
Treat your skin gently. Don't rub or touch your face too much. Use a nonsoap cleanser two times a day and moisturize. Some face creams may help reduce redness. Products made for the face that contain azelaic acid, dicarboxylic or niacinamide may help with rosacea symptoms. These products are available without a prescription.
Choose fragrance-free products, and avoid those that contain skin irritants such as alcohol, camphor, urea and menthol.
- Reduce facial symptoms with makeup. Some makeup products may help reduce the facial flushing common with rosacea. For example, green-tinted makeup can help cover up the red color. Avoid alcohol-based gels and thin lotions.
Alternative medicine
Gently massaging your face daily may help ease symptoms of rosacea. Using your fingers, make little circles starting on the center of the face and working to the ears. Do this for a few minutes.
If stress seems to make your symptoms worse, try stress management methods. Examples are deep breathing and meditating.
Coping and support
Rosacea can be distressing. You might feel embarrassed or anxious about how your face looks and become withdrawn or self-conscious. Or you may be upset by other people's reactions. It may help to talk with a counselor about these feelings. It also might help to find a rosacea support group, either in person or online. You may find comfort in connecting with others facing the same types of issues.
Preparing for an appointment
You're likely to start by seeing a member of your primary care team. Or you may be referred to a skin disease specialist, called a dermatologist. If your condition affects your eyes, you may be referred to an eye specialist, called an ophthalmologist.
It's a good idea to prepare for your appointment. Here's some information to help you.
What you can do
Preparing a list of questions helps you make the most of your appointment time. For rosacea, some basic questions are:
- What might be causing the symptoms?
- Do I need tests to confirm the diagnosis?
- What is the best treatment?
- Will this condition go away or is it long term?
- Is there a generic version of the medicine you're prescribing?
- I have other medical problems. How can I manage them together?
- Can I wait to see if the condition clears up on its own?
- What other treatments are there?
- What skin care routine do you suggest for me?
Ask any other questions that come up during your appointment.
What to expect from your doctor
Prepare to answer questions like these:
- When did you first notice your symptoms?
- How often do you have these symptoms?
- Have your symptoms been nonstop or do they come and go?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to bring on or worsen your symptoms?
Last Updated Oct 17, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



