Shellfish allergy
Overview
Shellfish allergy is an atypical response by the body's immune system to proteins in certain marine animals. Marine animals in the shellfish category include crustaceans and mollusks. Examples are shrimp, crabs, lobster, squid, oysters, scallops and snails.
Shellfish is a common food allergy. Some people with shellfish allergy react to all shellfish, while others react to only certain kinds. Reactions range from mild symptoms — such as hives or a stuffy nose — to severe and even life-threatening.
If you think you have shellfish allergy, talk to your health care provider. Tests can help confirm the allergy so you can take steps to avoid future reactions.
Symptoms
Shellfish allergy symptoms generally start within minutes to an hour after eating or having contact with shellfish. They may include:
- Hives
- Itchy, irritated skin
- Nasal stuffiness (congestion)
- Swelling of the lips, face, tongue and throat, or other parts of the body
- Wheezing or trouble breathing
- Coughing and choking or a tight feeling in the throat
- Belly (abdominal) pain, diarrhea, nausea or vomiting
- Dizziness, lightheadedness or fainting
Anaphylaxis
Allergies can cause a severe, potentially life-threatening allergic reaction known as anaphylaxis. It can occur within seconds to minutes after exposure to something you're allergic to — and worsens quickly.
An anaphylactic reaction to shellfish is a medical emergency. Anaphylaxis requires immediate treatment with an epinephrine (adrenaline) injection and a follow-up trip to the emergency room. If anaphylaxis isn't treated right away, it can be fatal.
Anaphylaxis causes the immune system to release a flood of chemicals that can cause you to go into shock. Signs and symptoms of anaphylaxis include:
- A swollen throat or tongue or a tightness in the throat (airway constriction) that makes it difficult for you to breathe
- Coughing, choking or wheezing with trouble breathing
- Shock, with a severe drop in your blood pressure and a rapid or weak pulse
- Severe skin rash, hives, itching or swelling
- Nausea, vomiting or diarrhea
- Dizziness, lightheadedness or fainting
When to see a doctor
Seek emergency treatment if you develop signs or symptoms of anaphylaxis.
See a health care provider or allergy specialist if you have food allergy symptoms shortly after eating.
Causes
All food allergies are caused by an immune system overreaction. Your immune system identifies a harmless substance as being harmful. This substance is called an allergen. In shellfish allergy, your immune system mistakenly identifies a certain protein in shellfish as harmful. Your immune system is how your body protects itself, so it produces immunoglobulin E (IgE) antibodies to protect against this allergen. The next time you come in contact with the shellfish protein, these antibodies signal your immune system to release chemicals such as histamine into your bloodstream. This causes a reaction that leads to the symptoms of an allergic reaction.
Types of shellfish
There are several types of shellfish, each containing different proteins:
- Crustaceans include crabs, lobster, crayfish, shrimp and prawn
- Mollusks include squid, octopus, mussels, snails, clams, oysters, abalone and scallops
An allergy to crustaceans is the most common type. Some people are allergic to only one type of shellfish but can eat others. Other people with shellfish allergy must avoid all shellfish.
An allergy to fish — such as salmon, tuna or catfish — is a different seafood allergy from an allergy to shellfish. Some people who are allergic to shellfish may still be able to eat fish, or they could be allergic to both. Your health care provider can help you determine what is safe to eat.
Risk factors
You're at increased risk of developing shellfish allergy if allergies of any type are common in your family.
Though people of any age can develop shellfish allergy, it's more common in adults. In fact, shellfish allergy is the most common food allergy in adults. Among adults, shellfish allergy is more common in women. Among children, shellfish allergy is more common in boys.
Complications
In severe cases, shellfish allergy can lead to anaphylaxis, a dangerous allergic reaction that can be life-threatening.
When you have shellfish allergy, you may be at increased risk of anaphylaxis if you have:
- Asthma
- Allergic reactions to very small amounts of shellfish (extreme sensitivity)
- History of food-induced anaphylaxis
- Strong family history of allergy
Anaphylaxis is treated with an emergency injection of epinephrine (adrenaline). If you are at risk of having a severe allergic reaction to shellfish, you always should carry injectable epinephrine (Auvi-Q, EpiPen, others).
Prevention
If you have shellfish allergy, the only way to avoid an allergic reaction is to avoid all shellfish and products that contain shellfish. Even trace amounts of shellfish can cause a severe reaction in some people.
Avoiding shellfish
- Be cautious when dining out. When dining at restaurants, always check to make sure that the pan, oil or utensils used for shellfish aren't also used to prepare other foods, creating cross-contamination. It might be necessary to avoid eating at seafood restaurants, where there's a high risk of cross-contamination.
-
Read labels. Cross-contamination can occur in stores where other food is processed or displayed near shellfish and during manufacturing. Shellfish may be in fish stock or seafood flavoring. Read food labels carefully.
Shellfish is not usually a hidden ingredient. Companies are required to label any product that contains crustacean shellfish or certain other foods that often cause allergic reactions. However, these regulations don't apply to mollusks.
- Keep your distance. You may need to completely avoid places where shellfish are prepared or processed. Some people react after touching shellfish or inhaling steam from cooking shellfish.
Be prepared
If you have shellfish allergy, talk with your health care provider about carrying emergency epinephrine and how to use it.
Consider wearing a medical alert bracelet or necklace that lets others know you have a food allergy.
Iodine or radiocontrast dye
One thing you don't need to worry about is if you'll also be allergic to iodine or radiocontrast material that's used in some imaging tests. Even though shellfish contain small amounts of iodine, shellfish allergy is unrelated to the reactions some people have to radiocontrast material or iodine.
Diagnosis
To find out if you have shellfish allergy, your health care provider will ask about your symptoms and do a physical exam to find or rule out other medical problems.
A history of allergic reactions shortly after exposure to shellfish can be a sign of shellfish allergy. But the symptoms could also be caused by something else, such as food poisoning.
Allergy testing is the only sure way to tell what's causing your symptoms, so your provider may recommend one or both of these tests:
- Skin prick test. Small amounts of the proteins found in shellfish are pricked into skin on your arm or upper back. You're then watched for an allergic reaction. If you're allergic, you'll develop a raised bump (hive) at the test site on your skin. This typically takes about 15 to 20 minutes. Allergy specialists usually are best equipped to perform allergy skin tests.
- Blood test. A blood sample is sent to a lab to measure your immune system's response to a specific allergen. This test measures your immune system's response to shellfish proteins by measuring the amount of allergy-causing antibodies in your bloodstream, known as immunoglobulin E (IgE) antibodies.
Medically supervised food challenges can be performed if the diagnosis still isn't clear after allergy testing.
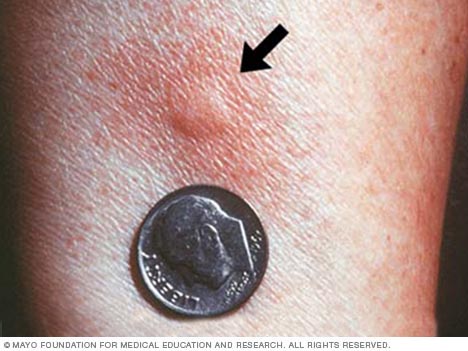
A small area of swelling with surrounding redness is typical of a positive allergy skin test.
Treatment
The only sure way to prevent an allergic reaction to shellfish is to avoid shellfish. But despite your best efforts, you may come into contact with shellfish.
If you have a severe allergic reaction to shellfish (anaphylaxis), you'll likely need an emergency injection of epinephrine (adrenaline). If you're at risk of anaphylaxis to shellfish, your health care provider can give you a prescription in advance and explain how and when to give the injection. Regularly check the expiration date on the packaging to make sure it's current.
Carry injectable epinephrine (Auvi-Q, EpiPen, others) with you at all times. Epinephrine is typically given at the first sign of an allergic reaction. A second dose may be needed if symptoms recur. After you use epinephrine, seek emergency medical care, even if you start to feel better.
Preparing for an appointment
You're likely to start by seeing your family health care provider. Or you may be referred directly to an allergy specialist.
What you can do
Prepare for your appointment by making a list of:
- Symptoms, including any that may seem unrelated to an allergy
- Family history of allergies and asthma, including specific types of allergies if you know them
- Medications, vitamins, herbs or other supplements you're taking, and the dosages
- Questions to ask your health care provider
Questions related to shellfish allergy include:
- Are my symptoms most likely due to an allergy?
- Will I need any allergy tests?
- Should I see an allergist?
- Do I need to carry epinephrine?
- Are there brochures or other educational materials I can have? What websites do you recommend?
Don't hesitate to ask other questions, as well.
What to expect from your doctor
Your health care provider may ask you questions, such as:
- What symptoms are you having? How severe are they?
- When did you notice your symptoms?
- Have you reacted to shellfish in the past?
- What kind of shellfish did you eat?
- How soon after eating shellfish did your symptoms occur?
- What other foods did you eat during your meal? Don't forget sauces, beverages and side dishes.
- Did others who dined with you have similar symptoms?
- Is there a history of allergy in your family?
- Do you have other allergies, such as hay fever?
- Do you have asthma or eczema (atopic dermatitis)?
What you can do in the meantime
Avoid eating or touching any type of shellfish while waiting for your appointment.
Last Updated Jul 2, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use
