Squamous cell carcinoma of the skin
Overview
Squamous cell carcinoma of the skin is a type of cancer that starts as a growth of cells on the skin. It starts in cells called squamous cells. The squamous cells make up the middle and outer layers of the skin. Squamous cell carcinoma is a common type of skin cancer.
Squamous cell carcinoma of the skin is usually not life-threatening. But if it's not treated, squamous cell carcinoma of the skin can grow large or spread to other parts of the body. The growth of the cancer can cause serious complications.
Most squamous cell carcinomas of the skin are caused by too much ultraviolet (UV) radiation. UV radiation comes either from sunlight or from tanning beds or lamps. Protecting your skin from UV light can help reduce the risk of squamous cell carcinoma of the skin and other forms of skin cancer.
Squamous cell carcinomas can be anywhere on the skin. In people who sunburn easily, the cancer is usually found on areas of skin that have had a lot of sun. In people with Black and brown skin, squamous cell carcinomas are more likely to be on skin that isn't exposed to sun, such as the genitals.
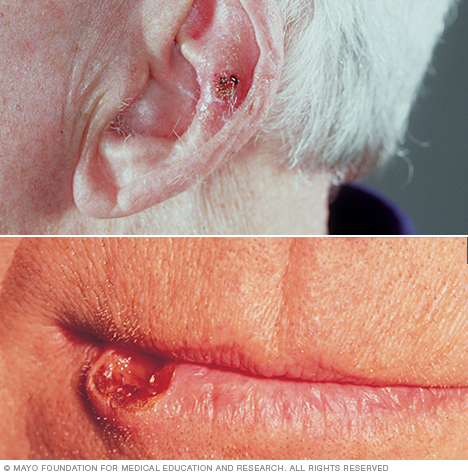
Sun-exposed areas such as the lips and ears are especially likely to develop squamous cell carcinoma of the skin.
Symptoms
Squamous cell carcinoma of the skin most often occurs on sun-exposed skin. This includes the scalp, the backs of the hands, the ears or the lips. But it can occur anywhere on the body. It can even occur inside the mouth, on the bottoms of the feet or on the genitals. When squamous cell carcinoma of the skin happens in people with Black and brown skin, it tends to happen in places that aren't exposed to the sun.
Symptoms of squamous cell carcinoma of the skin include:
- A firm bump on the skin, called a nodule. The nodule might be the same color as the skin, or it might look different. It can look pink, red, black or brown, depending on skin color.
- A flat sore with a scaly crust.
- A new sore or raised area on an old scar or sore.
- A rough, scaly patch on the lip that may become an open sore.
- A sore or rough patch inside the mouth.
- A raised patch or wartlike sore on or in the anus or on the genitals.
When to see a doctor
Make an appointment with a health care professional for a sore or scab that doesn't heal in about two months or a flat patch of scaly skin that won't go away.
Causes
Squamous cell carcinoma of the skin occurs when the squamous cells in the skin get changes in their DNA. Cells' DNA holds the instructions that tell cells what to do. The changes tell the squamous cells to multiply quickly. The cells continue living when healthy cells would die as part of their natural life cycle.
This causes too many cells. The cells can invade and destroy healthy body tissue. In time, the cells can break away and spread to other parts of the body.
Ultraviolet (UV) radiation causes most of the DNA changes in skin cells. UV radiation can come from sunlight, tanning lamps and tanning beds.
But skin cancers also can grow on skin that's not usually in sunlight. This means that other factors might add to the risk of skin cancer. One such factor might be having a condition that weakens the immune system.
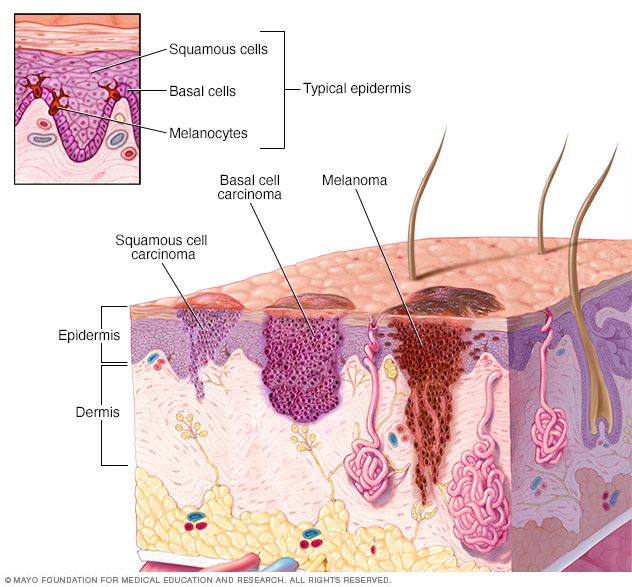
Skin cancer begins in the cells that make up the outer layer of the skin, called the epidermis. One type of skin cancer called basal cell carcinoma begins in the basal cells. Basal cells make skin cells that keep pushing older cells toward the surface. As new cells move up, they become squamous cells. Skin cancer that starts in the squamous cells is called squamous cell carcinoma of the skin. Melanoma, another type of skin cancer, comes from the pigment cells, called melanocytes.
Risk factors
Factors that can increase the risk of squamous cell carcinoma of the skin include:
-
Having skin that sunburns easily. Anyone of any skin color can get squamous cell carcinoma of the skin. But it's more common in people who have low levels of melanin in their skin. Melanin is a substance that gives color to skin. It also helps protect the skin from damaging ultraviolet (UV) radiation. People with Black or brown skin have more melanin than people with white skin.
The risk of squamous cell carcinoma is highest in people who have blond or red hair, have light-colored eyes and freckle or sunburn easily.
- Being in the sun too much. UV radiation from the sun increases the risk of squamous cell carcinoma of the skin. Covering the skin with clothes or sunblock can help lower the risk.
- Using tanning beds. People who use indoor tanning beds have an increased risk of squamous cell carcinoma of the skin.
- Having a history of sunburns. Having had one or more sunburns that raised blisters as a child or teenager increases the risk of developing squamous cell carcinoma of the skin as an adult. Sunburns in adulthood also are a risk factor.
- Having a history of precancerous skin lesions. Some types of skin sores can turn into skin cancer. Examples are actinic keratosis or Bowen disease. Having one of these conditions increases the risk of squamous cell carcinoma.
- Having a history of skin cancer. People who've had squamous cell carcinoma of the skin once are much more likely to get it again.
- Having a weakened immune system. People with weakened immune systems have an increased risk of skin cancer. This includes people who have leukemia or lymphoma. And it includes those who take medicines to control the immune system, such as those who have had organ transplants.
- Having a rare genetic disorder. People with xeroderma pigmentosum, which causes great sensitivity to sunlight, have a greatly increased risk of developing skin cancer.
- Having human papillomavirus infection (HPV). This common infection that's passed through sexual contact increases the risk of squamous cell carcinoma of the skin.
- Having scars or long-lasting wounds on the skin. Squamous cell carcinoma of the skin can form in scars, burns and sores that don't heal.
Complications
Untreated squamous cell carcinoma of the skin can destroy nearby healthy tissue. It can spread to the lymph nodes or other organs. And it can be fatal, although this is not common.
The risk of squamous cell carcinoma of the skin spreading may be higher if the cancer:
- Grows very large or deep.
- Involves the mucous membranes, such as the lips.
- Occurs in a person with a weakened immune system. Examples of things that might cause a weakened immune system include having chronic leukemia or taking medicine to control the immune system after an organ transplant.
Prevention
Most squamous cell carcinomas of the skin can be prevented. To protect yourself:
- Stay out of the sun during the middle of the day. For much of North America, the sun's rays are strongest between about 10 a.m. and 3 p.m. Plan outdoor activities at other times of the day, even during winter or when the sky is cloudy. When outside, stay in shade as much as possible.
- Wear sunscreen year-round. Use a broad-spectrum sunscreen with an SPF of at least 30, even on cloudy days. Apply sunscreen generously. Apply again every two hours, or more often if you're swimming or sweating.
- Wear protective clothing. Wear dark, tightly woven clothes that cover arms and legs. Wear a wide-brimmed hat that shades your face and ears. Don't forget sunglasses. Look for those that block both types of UV radiation, UVA and UVB rays.
- Don't use tanning beds. The lights in tanning beds give off UV radiation. Using tanning beds increases the risk of skin cancer.
-
Check your skin often and report changes to your health care team. Look at your skin often for new growths. Look for changes in moles, freckles, bumps and birthmarks. Use mirrors to check your face, neck, ears and scalp.
Look at your chest and trunk and the tops and undersides of your arms and hands. Look at the front and back of your legs and your feet. Look at the bottom of the feet and the spaces between your toes. Also check your genital area and between your buttocks.
Diagnosis
Tests and procedures used to diagnose squamous cell carcinoma of the skin include:
- Physical exam. A member of your health care team asks about your health history and looks at your skin for signs of squamous cell carcinoma of the skin.
- Removing a sample of tissue for testing, called a biopsy. A biopsy is a procedure to remove a sample of tissue for testing in a lab. A member of your health care team uses a tool to cut away, shave off or punch out some or all of the area of skin that looks unusual. The sample is tested in a lab to see if it is cancer.
Treatment
Most squamous cell carcinomas of the skin can be removed with minor surgery. Some are removed with a medicine applied to the skin. The treatment depends on where the cancer is, how large it is, how fast it's growing and what you prefer.
Treatments for very small skin cancers
If the skin cancer is small, not deep into the skin, called superficial, and has a low risk of spreading, less-invasive treatment choices include:
- Curettage and electrodessication. This treatment involves removing the top of the skin cancer with a scraping tool called a curet. Then an electric needle is used to sear the base of the cancer.
- Laser therapy. This treatment uses an intense beam of light to destroy growths. There's usually little damage to nearby tissue. And there's a reduced risk of bleeding, swelling and scarring.
- Freezing. This treatment, called cryosurgery, involves freezing cancer cells with liquid nitrogen. Freezing might be done after using a scraping tool, called a curet, to remove the surface of the skin cancer.
- Photodynamic therapy. During photodynamic therapy, a liquid medicine that makes the cancer cells sensitive to light is applied to the skin. Later, a light that destroys the skin cancer cells is shined on the area. This treatment might be used with surgery or other treatments.
Treatments for larger skin cancers
More-invasive treatments might be recommended for larger squamous cell carcinomas and those that go deeper into the skin. Options might include:
- Simple excision. This involves cutting out the cancer and a margin of healthy skin around it. Sometimes more skin around the tumor is removed, called a wide excision.
- Mohs surgery. Mohs surgery involves removing the cancer layer by layer and looking at each layer under the microscope until no cancer cells are left. This allows the surgeon to remove the whole growth without taking too much of the healthy skin around it.
- Radiation therapy. Radiation therapy uses powerful energy beams to kill cancer cells. Radiation therapy is sometimes used after surgery when there is an increased risk that the cancer might return. It also might be an option for people who can't have or don't want surgery.
Treatments for skin cancer that spreads past the skin
When squamous cell carcinoma spreads to other parts of the body, medicines might be recommended, including:
- Chemotherapy. Chemotherapy uses strong medicines to kill cancer cells. If squamous cell carcinoma spreads to the lymph nodes or other parts of the body, chemotherapy can be used alone or with other treatments, such as targeted therapy and radiation therapy.
- Targeted therapy. Targeted therapy uses medicines that attack specific chemicals in the cancer cells. By blocking these chemicals, targeted treatments can cause cancer cells to die. Targeted therapy is usually used with chemotherapy.
-
Immunotherapy. Immunotherapy is a treatment with medicine that helps the body's immune system kill cancer cells. The immune system fights off diseases by attacking germs and other cells that shouldn't be in the body. Cancer cells survive by hiding from the immune system. Immunotherapy helps the immune system cells find and kill the cancer cells.
For squamous cell carcinoma of the skin, immunotherapy might be considered when the cancer is advanced and other treatments aren't an option.
Preparing for an appointment
If you have a skin sore that concerns you, make an appointment with a doctor or other health care professional. You may be referred to a doctor who specializes in the diagnosis and treatment of skin conditions, called a dermatologist.
If you've already had skin cancer, you have an increased risk of a second cancer. Talk with your dermatologist about how often to have a skin exam to look for signs of another skin cancer.
Here's some information to help you get ready for your appointment.
What you can do
Ask a family member or friend to go with you to the appointment to help you remember the information you get.
Make a list of:
- Your medical history, including other conditions for which you've been treated.
- All your medications, vitamins and natural remedies you take, including doses.
- Questions to ask your health care team.
Some basic questions to ask about squamous cell carcinoma of the skin include:
- Do I have skin cancer? What kind?
- Is this type of cancer likely to spread?
- Has my cancer spread?
- What treatment do you recommend?
- What are the possible side effects of this treatment?
- Will I have a scar after treatment?
- Is this cancer likely to come back?
- Am I at risk of other types of skin cancer?
- What can I do to prevent skin cancer?
- How often will I need follow-up visits after treatment?
- Are there brochures or other printed material that I can have? What websites do you recommend?
What to expect from your doctor
Be prepared to answer some basic questions, such as:
- How long have you had this skin growth?
- Has it grown much since you found it?
- Does the growth or sore cause discomfort?
- Do you have any other growths or sores that concern you?
- Have you had skin cancer before?
- How much were you in the sun as a child?
- Have you ever used tanning beds?
- How much are you in the sun now?
- What do you do to stay safe in the sun?
- Have you ever taken medicines that suppress your immune system?
- Do you or did you smoke? How much?
Last Updated Aug 11, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



