Syphilis
Overview
Syphilis is an infection caused by bacteria. Most often, it spreads through sexual contact. The disease starts as a sore that's often painless and typically appears on the genitals, rectum or mouth. Syphilis spreads from person to person through direct contact with these sores. It also can be passed to a baby during pregnancy and childbirth and sometimes through breastfeeding.
After the infection happens, syphilis bacteria can stay in the body for many years without causing symptoms. But the infection can become active again. Without treatment, syphilis can damage the heart, brain or other organs. It can become life-threatening.
Early syphilis can be cured, sometimes with a single shot of medicine called penicillin. That's why it's key to get a health care checkup as soon as you notice any symptoms of syphilis. All pregnant people should get tested for syphilis at their first prenatal checkup too.
Symptoms
Syphilis develops in stages. The symptoms vary with each stage. But the stages may overlap. And the symptoms don't always happen in the same order. You may be infected with syphilis bacteria without noticing any symptoms for years.
Primary syphilis
The first symptom of syphilis is a small sore called a chancre (SHANG-kur). The sore is often painless. It appears at the spot where the bacteria entered your body. Most people with syphilis develop only one chancre. Some people get more than one.
The chancre often forms about three weeks after you come in contact with syphilis bacteria. Many people who have syphilis don't notice the chancre. That's because it's usually painless. It also may be hidden within the vagina or rectum. The chancre heals on its own within 3 to 6 weeks.
Secondary syphilis
You may get a rash while the first chancre heals or a few weeks after it heals.
A rash caused by syphilis:
- Often is not itchy.
- May look rough, red or reddish-brown.
- Might be so faint that it's hard to see.
The rash often starts on the trunk of the body. That includes the chest, stomach area, pelvis and back. In time, it also could appear on the limbs, the palms of the hands and the soles of the feet.
Along with the rash, you may have symptoms such as:
- Wartlike sores in the mouth or genital area.
- Hair loss.
- Muscle aches.
- Fever.
- Sore throat.
- Tiredness, also called fatigue.
- Weight loss.
- Swollen lymph nodes.
Symptoms of secondary syphilis may go away on their own. But without treatment, they could come and go for months or years.
Latent syphilis
If you aren't treated for syphilis, the disease moves from the secondary stage to the latent stage. This also is called the hidden stage because you have no symptoms. The latent stage can last for years. Your symptoms may never come back. But without treatment, the disease might lead to major health problems, also called complications.
Tertiary syphilis
After the latent stage, up to 30% to 40% of people with syphilis who don't get treatment have complications known as tertiary syphilis. Another name for it is late syphilis.
The disease may damage the:
- Brain.
- Nerves.
- Eyes.
- Heart.
- Blood vessels.
- Liver.
- Bones and joints.
These problems may happen many years after the original, untreated infection.
Syphilis that spreads
At any stage, untreated syphilis can affect the brain, spinal cord, eyes and other body parts. This can cause serious or life-threatening health problems.
Congenital syphilis
Pregnant people who have syphilis can pass the disease to their babies. Unborn babies can become infected through the organ that provides nutrients and oxygen in the womb, called the placenta. Infection also can happen during birth.
Newborns with congenital syphilis might have no symptoms. But without fast treatment, some babies might get:
- Sores and rashes on the skin.
- Fever.
- A type of discolored skin and eyes, called jaundice.
- Not enough red blood cells, called anemia.
- Swollen spleen and liver.
- Sneezing or stuffed, drippy nose, called rhinitis.
- Bone changes.
Later symptoms may include deafness, teeth problems and saddle nose, a condition in which the bridge of the nose collapses.
Babies with syphilis also can be born too early. They may die in the womb before birth. Or they could die after birth.
When to see a doctor
Call a member of your health care team if you or your child has any symptoms of syphilis. These could include any unusual discharge, a sore or a rash, especially in the groin area.
Also get tested for syphilis if you:
- Have had sexual contact with someone who might have the disease.
- Have another sexually transmitted disease such as HIV.
- Are pregnant.
- Regularly have sex with more than one partner.
- Have unprotected sex, meaning sex without a condom.
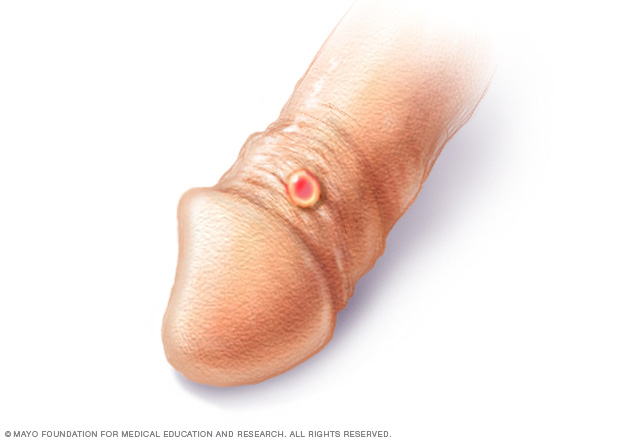
Primary syphilis causes painless sores (chancres) on the genitals, rectum, tongue or lips. The disease can be present with the appearance of a single chancre (shown here on a penis) or many.
Causes
The cause of syphilis is a bacterium called Treponema pallidum. The most common way syphilis spreads is through contact with an infected person's sore during vaginal, oral or anal sex.
The bacteria enter the body through minor cuts or scrapes in the skin or in the moist inner lining of some body parts.
Syphilis is contagious during its primary and secondary stages. Sometimes it's also contagious in the early latent period, which happens within a year of getting infected.
Less often, syphilis can spread by kissing or touching an active sore on the lips, tongue, mouth, breasts or genitals. It also can be passed to babies during pregnancy and childbirth and sometimes through breastfeeding.
Syphilis can't be spread through casual contact with objects that an infected person has touched.
So you can't catch it by using the same toilet, bathtub, clothing, eating utensils, doorknobs, swimming pools or hot tubs.
Once cured, syphilis doesn't come back on its own. But you can become infected again if you have contact with someone's syphilis sore.
Risk factors
The risk of catching syphilis is higher if you:
- Have unprotected sex.
- Have sex with more than one partner.
- Live with HIV, the virus that causes AIDS if untreated.
The chances of getting syphilis also are higher for men who have sex with men. The higher risk may be linked, in part, with less access to health care and less use of condoms among this group. Another risk factor for some people in this group includes recent sex with partners found through social media apps.
Complications
Without treatment, syphilis can lead to damage throughout the body. Syphilis also raises the risk of HIV infection and can cause problems during pregnancy. Treatment can help prevent damage. But it can't repair or reverse damage that's already happened.
Small bumps or tumors
Rarely in the late stage of syphilis, bumps called gummas can form on the skin, bones, liver or any other organ. Most often, gummas go away after treatment with medicine called antibiotics.
Neurological problems
Syphilis can cause many problems with the brain, its covering or the spinal cord. These issues include:
- Headache.
- Stroke.
- Meningitis, a disease that inflames the protective layers of tissue around the brain and spinal cord.
- Confusion, personality changes or trouble focusing.
- Symptoms that mimic dementia, such as loss of memory, judgment and decision-making skills.
- Not being able to move certain body parts, called paralysis.
- Trouble getting or keeping an erection, called erectile dysfunction.
- Bladder problems.
Eye problems
Disease that spreads to the eye is called ocular syphilis. It can cause:
- Eye pain or redness.
- Vision changes.
- Blindness.
Ear problems
Disease that spreads to the ear is called otosyphilis. Symptoms can include:
- Hearing loss.
- Ringing in the ears, called tinnitus.
- Feeling like you or the world around you is spinning, called vertigo.
Heart and blood vessel problems
These may include bulging and swelling of the aorta — the body's major artery — and other blood vessels. Syphilis also may damage heart valves.
HIV infection
Syphilis sores on the genitals raise the risk of catching or spreading HIV through sex. A syphilis sore can bleed easily. This provides an easy way for HIV to enter the bloodstream during sex.
Pregnancy and childbirth complications
If you're pregnant, you could pass syphilis to your unborn baby. Congenital syphilis greatly raises the risk of miscarriage, stillbirth or your newborn's death within a few days after birth.
Prevention
There is no vaccine for syphilis. To help prevent the spread of syphilis, follow these tips:
- Have safe sex or no sex. The only certain way to avoid contact with syphilis bacteria is not to have sex. This is called abstinence. If a person is sexually active, safer sex means a long-term relationship in which you and your partner have sex only with each other, and neither of you is infected. Before you have sex with someone new, you should both get tested for syphilis and other sexually transmitted infections (STIs).
- Use a latex condom. Condoms can lower your risk of getting or spreading syphilis. But condoms work only if they cover an infected person's syphilis sores. Other types of birth control do not lower your risk of syphilis.
- Be careful with alcohol and stay away from street drugs. Drinking too much alcohol or taking drugs can get in the way of your judgment. Either can lead to unsafe sex.
- Do not douche. It can remove some of the healthy bacteria that's usually in the vagina. And that might raise your risk of getting STIs.
- Breastfeed with caution. Syphilis can pass from a parent to a baby during breastfeeding if sores are on one or both breasts. This can happen when the baby or pumping equipment touches a sore. To keep that from happening, pump or hand-express breastmilk from the breast with sores. Do so until the sores heal. If your pump touches a sore, get rid of the milk you just pumped.
Partner notification and preventive treatment
If tests show that you have syphilis, your sex partners need to know so that they can get tested. This includes your current partners and any others you've had over the last three months to 1 year. If they're infected, they can then get treatment.
After you learn you have syphilis, your local health department may contact you. A department employee talks with you about private ways to let your partners know that they've been exposed to syphilis. You can ask the department to do this for you without revealing your identity to your partners.
Or you can contact your partners along with a department employee or simply tell your partners yourself. This free service is called partner notification. It can help limit the spread of syphilis. The practice also steers those at risk toward counseling and the right treatment.
And since you can get syphilis more than once, partner notification lowers your risk of getting infected again.
Screening tests for pregnant people
You can be infected with syphilis and not know it. And the disease can have deadly effects on unborn babies. For this reason, health officials recommend that all pregnant people be tested for the disease.
Diagnosis
Tests
Your health care team can find syphilis by testing samples of:
- Blood. Blood tests can confirm the presence of proteins called antibodies. The immune system makes these to fight infections. The antibodies to the bacteria that causes syphilis stay in the body for years. So blood tests can be used to find a current or past infection.
- Fluid from a sore. A laboratory can study this fluid under a microscope to confirm that syphilis caused the sore.
- Fluid that surrounds the brain and spinal cord. Another name for this is cerebrospinal fluid. If your care team thinks that you have nervous system problems from syphilis, they might recommend testing this fluid. A needle is used to take a sample of cerebrospinal fluid from between two of the bones in the back. This procedure is called a lumbar puncture.
Remember, your local health department may offer partner services. These help you notify your sexual partners that they may be infected. Your partners can be tested and treated, limiting the spread of syphilis.
Treatment
Medications
Syphilis is simple to cure when it's found and treated in its early stages. The preferred treatment at all stages is penicillin. This antibiotic medicine can kill the bacteria that causes syphilis.
If you're allergic to penicillin, your health care team may suggest another antibiotic. Or they may recommend a process that safely helps your body get used to penicillin over time.
The recommended treatment for primary, secondary or early-stage latent syphilis is a single shot of penicillin. If you've had syphilis for longer than a year, you may need additional doses.
Penicillin is the only recommended treatment for pregnant people with syphilis. Those who are allergic to penicillin can follow a process that may allow them to take the medicine. The procedure is called penicillin desensitization.
It's done by a specialist called an allergist or an immunologist. It involves taking tiny amounts of penicillin every 15 to 20 minutes over about 4 hours.
Even if you're treated for syphilis during your pregnancy, your newborn should be tested for congenital syphilis. A baby infected with the syphilis bacterium receives antibiotic treatment.
The first day you receive treatment, you may have what's known as the Jarisch-Herxheimer reaction. Symptoms include a fever, chills, nausea, achy pain and a headache. Most often, this reaction doesn't last more than one day.
Treatment follow-up
After you're treated for syphilis, your health care team likely will ask you to:
- Have regular blood tests and exams to make sure the penicillin treatment is working. The follow-up tests you need depend on the stage of syphilis you have.
- Do not have sexual contact with new partners until the treatment is finished. Blood tests should show that the infection has been cured, and any sores should be gone.
- Tell your sex partners so they can be tested and get treatment if needed.
- Get tested for HIV.
Coping and support
Finding out you have syphilis can be upsetting. You might get angry if you feel you've been betrayed by a partner. Or you might feel shame if you think you've infected others.
Hold off placing any blame. Don't assume that your partner has been unfaithful to you. One or both of you may have been infected by a past partner.
Preparing for an appointment
Many people don't feel comfortable sharing the details of their sexual experiences. But it's important to have a private talk with your health care team about this information, so you can get the right care.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, ask if there's anything you need to do in advance.
- Write down any symptoms you have. Include any that may not seem related to the reason for which you made the appointment.
- Make a list of all medicines, vitamins or supplements you take. Include the amounts you take, also called the doses.
- Write down questions to ask your health care team.
Some basic questions to ask include:
- What's the medical name of the infection I have?
- How does it spread?
- Will it keep me from having children?
- If I get pregnant, could I give it to my baby?
- Is it possible to catch this again?
- Could I have caught this from someone I had sex with only once?
- Could I give this to someone by having sex with that person just once?
- How long have I had it?
- I have other health conditions. How can I best manage them together?
- Should I stop sexual activity while I'm being treated?
- Does my partner have to be treated?
What to expect from your doctor
Give your health care team a complete report of your symptoms and sexual history. This helps the team figure out how to best care for you. Here are some of the things you may be asked:
- What symptoms made you decide to come in? How long have you had these symptoms?
- With whom do you have sex?
- Do you currently have one sex partner or more than one?
- How long have you been with your current partner or partners?
- Have you ever injected yourself with drugs?
- Have you ever had sex with someone who has injected drugs?
- What do you do to protect yourself from sexually transmitted infections (STIs)?
- What do you do to prevent pregnancy?
- Has a doctor or nurse ever told you that you have chlamydia, herpes, gonorrhea, syphilis or HIV?
- Have you ever been treated for genital discharge, genital sores, painful urination or an infection of your sex organs?
- How many sex partners have you had in the past year? In the past two months?
- When was your most recent sexual encounter?
What you can do in the meantime
If you think you might have syphilis, it's best to not have any sexual contact until you've talked with your health care team. If you have sexual activity before you see your care team, follow safe sex practices such as using a condom.
Last Updated Oct 7, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use