Thoracic outlet syndrome
Overview
Thoracic outlet syndrome (TOS) is a group of conditions in which there's pressure on blood vessels or nerves in the area between the neck and shoulder. This space is known as the thoracic outlet. Compression of the blood vessels and nerves can cause shoulder and neck pain. It also can cause numbness in the fingers.
Common causes of thoracic outlet syndrome include trauma from a car accident, repetitive injuries from a job or sport, and pregnancy. Differences in anatomy, such as having an extra or irregular rib, also can cause TOS. Sometimes the cause of thoracic outlet syndrome is not known.
Treatment often involves physical therapy and pain relief. Most people improve with these treatments. For some, surgery may be recommended.
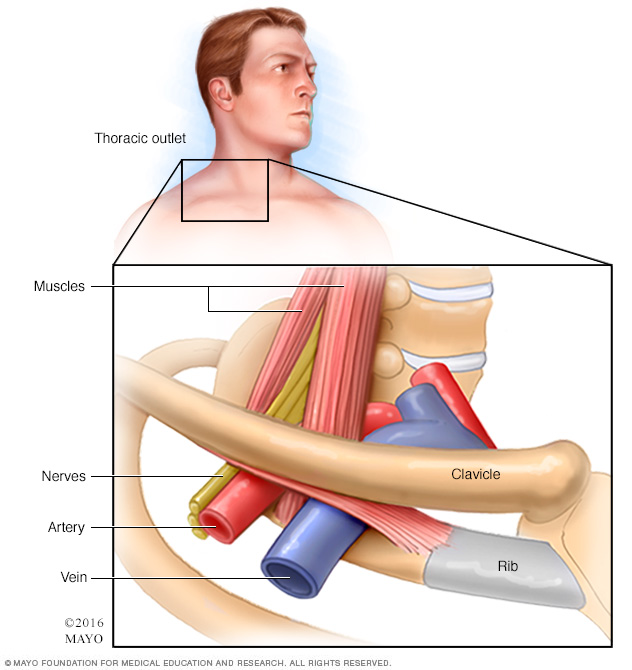
The thoracic outlet is the space between the collarbone, known as the clavicle, and the first rib. This narrow passageway is crowded with blood vessels, nerves and muscles.
Symptoms
There are three types of thoracic outlet syndrome:
- Neurogenic thoracic outlet syndrome. This is the most common type of thoracic outlet syndrome. In this type, a group of nerves called the brachial plexus is compressed. The nerves of the brachial plexus come from the spinal cord. The nerves control muscle movements and feeling in the shoulder, arm and hand.
- Venous thoracic outlet syndrome. This type of thoracic outlet syndrome occurs when one or more of the veins under the collarbone are compressed and damaged. This can result in blood clots.
- Arterial thoracic outlet syndrome. This is the least common type of TOS. It occurs when one of the arteries under the collarbone is compressed. The compression may cause injury to the artery resulting in a bulge, known as an aneurysm, or blood clot formation.
Thoracic outlet syndrome symptoms can vary depending on the type. When nerves are compressed, symptoms of neurogenic thoracic outlet syndrome include:
- Numbness or tingling in the arm or fingers.
- Pain or aches in the neck, shoulder, arm or hand.
- Arm fatigue with activity.
- A weakening grip.
Symptoms of venous thoracic outlet syndrome can include:
- A change in the color of the hand or one or more fingers.
- Hand or arm pain and swelling.
Symptoms of arterial thoracic outlet syndrome can include:
- A pulsating lump near the collarbone.
- Cold fingers, hands or arms.
- Hand and arm pain.
- A change in color in one or more of the fingers or the entire hand.
- Weak or no pulse in the affected arm.
When to see a doctor
See your healthcare professional if you regularly experience any of the symptoms of thoracic outlet syndrome.
Causes
Thoracic outlet syndrome is often caused by compression of the nerves or blood vessels in the thoracic outlet, the area between the neck and shoulder. The cause of the compression varies and can include:
- Differences in anatomy. Some people are born with an extra rib in the neck found above the first rib. The extra rib, known as a cervical rib, can compress nerves or blood vessels. There also may be a tight fibrous band connecting the spine to the rib that causes compression.
- Poor posture. Drooping your shoulders or holding your head in a forward position can cause compression in the thoracic outlet area.
- Trauma. A traumatic event, such as a car accident, can cause internal changes that then compress the nerves in the thoracic outlet. The onset of symptoms related to a traumatic accident often is delayed.
Risk factors
There are several factors that seem to increase the risk of thoracic outlet syndrome, including:
- Sex. Women are more than three times more likely to be diagnosed with thoracic outlet syndrome than are men.
- Age. Thoracic outlet syndrome may occur at any age but is most commonly diagnosed in adults between the ages of 20 and 50.
Complications
Complications from this condition stem from the type of thoracic outlet syndrome. If you have swelling or a painful discoloration in the arm, it is important to seek urgent medical attention. You may need treatment for blood clots or an aneurysm.
For neurogenic TOS, repetitive nerve compression can result in long-term injury resulting in chronic pain or disability. Neurogenic TOS can be confused for other joint or muscle injuries. If symptoms don't improve, it is important to seek medical attention for an evaluation and testing.
Prevention
If you're at risk of thoracic outlet compression, avoid repetitive movements and lifting heavy objects. If you're overweight, losing weight may help you prevent or relieve symptoms of thoracic outlet syndrome.
Even if you don't have symptoms of thoracic outlet syndrome, avoid carrying heavy bags over your shoulder. This can increase pressure on the thoracic outlet. Stretch daily, and do exercises that keep your shoulder muscles strong and flexible.
Daily stretches focusing on the chest, neck and shoulders can help improve shoulder muscle strength and prevent thoracic outlet syndrome.
Diagnosis
Diagnosing thoracic outlet syndrome can be challenging. Symptoms can vary greatly among people. Your healthcare professional may review your symptoms and medical history and conduct a physical exam. You also may need imaging and other types of tests.
Physical exam. Your healthcare professional does a physical exam to look for signs of thoracic outlet syndrome. These may include a depression in your shoulder or a bony area above the collarbone. Your healthcare professional also may look for swelling or a change in color in your arm. You may need to have your pulse and your range of motion checked.
Your health professional may reproduce your symptoms by asking you to move or lift your arms or turn your head. Knowing which positions and movements trigger your symptoms can help identify thoracic outlet syndrome.
- Medical history. Tell your healthcare professional about your medical history and symptoms. You also may be asked about your job duties and physical activities.
Imaging and nerve study tests
To confirm the diagnosis of thoracic outlet syndrome, you may need one or more of the following tests:
- Ultrasound. An ultrasound uses sound waves to create images of your body. It's often the first imaging test used to help diagnose thoracic outlet syndrome. This test may be used to see if you have venous or arterial thoracic outlet syndrome or other vascular conditions.
- X-ray. An X-ray can reveal an extra rib, known as a cervical rib. X-rays also can help to rule out other conditions that could be causing your symptoms.
- Computerized tomography (CT) scan. A CT scan uses X-rays to get cross-sectional images of your body. A dye may be injected into a vein to view the blood vessels in greater detail, known as CT angiography. A CT scan may identify the location and cause of blood vessel compression.
- Magnetic resonance imaging (MRI). An MRI uses radio waves and magnetic fields to create a detailed view of your body. An MRI may be helpful to determine the location and cause of blood vessel compression. Sometimes dye is injected to better see the blood vessels. An MRI may reveal differences in anatomy, such as a fibrous band connecting your spine to your rib or a cervical rib. These differences in anatomy may be the cause of your symptoms. A healthcare professional may place your head, shoulders and neck in different positions. This may allow for a better view of the blood vessels in your arm.
Arteriography and venography. In these tests, a thin, flexible tube called a catheter is inserted through a small cut, often in your groin. During arteriography, the catheter moves through your major arteries. During venography, the catheter moves through your veins. The catheter is threaded to the affected blood vessels. Then a dye is injected to show X-ray images of your arteries or veins.
Healthcare professionals can check to see if you have a compressed vein or artery. If a vein or artery has a clot, doctors can deliver medications through the catheter to dissolve the clot.
- Electromyography (EMG). During an EMG, a needle electrode is inserted through your skin into various muscles. The test checks the electrical activity of your muscles when they contract and when they're at rest. This test can determine if you have nerve damage.
Treatment
A conservative approach to treatment may be effective for most people, especially if your condition is diagnosed early. Treatment may include:
- Physical therapy. If you have neurogenic thoracic outlet syndrome, physical therapy is the first line of treatment. The exercises strengthen and stretch your shoulder muscles to open the thoracic outlet. This improves your range of motion and posture. These exercises, done over time, may take the pressure off the blood vessels and nerves in the thoracic outlet.
- Medicines. You may be prescribed anti-inflammatory medicines, pain medicines or muscle relaxants. The medicines reduce swelling, reduce pain and encourage muscle relaxation. If there is a blood clot, you may need a blood-thinning medicine.
- Clot-dissolving medicines. If you have venous or arterial thoracic outlet syndrome and have blood clots, you may be given a medicine to dissolve the clots. The medicine, known as thrombolytics, goes into your veins or arteries to dissolve blood clots. After you're given thrombolytics, your healthcare professional may prescribe medicines to prevent blood clots, known as anticoagulants.
- Injections. Injections of a local anesthetic, onabotulinumtoxinA (Botox) or a steroid medicine may be used to treat neurogenic thoracic outlet syndrome. The injections can help reduce pain.
Surgical options
Your healthcare professional may recommend surgery if conservative treatments haven't been effective. Or you might consider surgery if you experience ongoing or worsening symptoms.
A surgeon trained in chest surgery, known as a thoracic surgeon, or blood vessel surgery, known as a vascular surgeon, typically does the procedure.
Thoracic outlet syndrome surgery has risks of complications, such as injury to the nerves, known as the brachial plexus. Also, surgery may not relieve your symptoms or only partially relieve your symptoms, and symptoms may come back.
Surgery to treat thoracic outlet syndrome, called thoracic outlet decompression, may be done using several different approaches. These approaches involve removing a muscle and a part of the first rib to relieve compression. You also may need surgery to repair damaged blood vessels.
In venous or arterial thoracic outlet syndrome, your surgeon may deliver medicines to dissolve blood clots prior to thoracic outlet decompression. Or you may need a procedure to remove a clot from the vein or artery or to repair the vein or artery. The procedure is done before thoracic outlet decompression.
If you have arterial thoracic outlet syndrome, your surgeon may need to replace the damaged artery. This is done with a section of an artery from another part of your body, known as a graft. Or an artificial graft may be used. This procedure may be done at the same time as a procedure to have the first rib removed.
Lifestyle and home remedies
If you're diagnosed with thoracic outlet syndrome, a physical therapist may instruct you to do exercises at home. The exercises can strengthen and support the muscles surrounding your thoracic outlet.
In general, to avoid unnecessary stress on your shoulders and muscles surrounding the thoracic outlet:
- Maintain good posture.
- Take frequent breaks at work to move and stretch.
- Maintain a healthy weight.
- Create a work area that allows you to keep good posture and doesn't make symptoms worse.
- Gently massage your shoulders and thoracic outlet.
- Apply a heating pad to the area.
- Practice relaxation exercises such as deep breathing, meditation and stretching.
Coping and support
Symptoms associated with thoracic outlet syndrome can be caused by a number of other conditions. This can make it hard to diagnose. Many people experience thoracic outlet syndrome symptoms for years before they are diagnosed with the condition. Discuss your concerns with your healthcare professional if your symptoms persist and a diagnosis hasn't been made.
Preparing for an appointment
You're likely to start by seeing your healthcare professional. Or you may be referred to a doctor trained in blood vessel conditions or in blood vessel surgery, known as a vascular surgeon.
Here's some information to help you prepare for your appointment.
What you can do
- Be aware of any pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do before you arrive at the office.
- Write down any symptoms you're experiencing, including any that seem unrelated to the reason for which you scheduled the appointment. Be as specific and detailed as possible in describing your symptoms, including what part of your body is affected and how the discomfort makes you feel.
- Write down key personal information, including any physical traumas you've experienced, such as a car accident or work-related injury. Include the information even if the injuries occurred years ago. Also note any repetitive physical activities that you do now or have done in the past. This may include activities at work, in sports, and for hobbies and other recreational activities.
- List your key medical information, including other conditions for which you're receiving treatment. Also include the names of any prescription and nonprescription medicines or supplements that you're taking.
- Take a family member or friend along, if possible. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your healthcare professional.
Preparing a list of questions helps you make the most of your time. For thoracic outlet syndrome, some basic questions to ask include:
- What's the most likely cause of my symptoms?
- What kinds of tests do I need?
- What treatments are available, and which treatment do you recommend for me?
- How likely are nonsurgical treatments to improve my symptoms?
- If conservative treatments aren't effective, is surgery an option?
- Is there anything I can do to prevent a recurrence of this problem?
- Will I need to change my job?
- Do I need to limit or give up other activities that may be causing my symptoms?
- If you're recommending weight loss, how much weight do I need to lose to notice an improvement in my symptoms?
- I have other health conditions. How can I best manage them with this condition?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend visiting?
Don't hesitate to ask any other questions you have.
What to expect from your doctor
It's likely you'll be asked several questions, such as:
- When did you first notice your symptoms?
- How would you describe your symptoms?
- Have your symptoms changed over time?
- Where does your pain seem to start and where does it go from there?
- Does the pain or numbness worsen when you lift your arms overhead?
- Does anything else seem to worsen or improve your symptoms?
- What activities do you perform on your job?
- Do you or did you play sports?
- What are your hobbies or most frequent recreational activities?
- Have you been diagnosed or treated for any other medical conditions? When?
- Have you noticed a lack of color or a change in color in one or more of your fingers or your entire hand? Have you noticed other changes to the area?
What you can do in the meantime
While you're waiting for your appointment, try taking a nonsteroidal anti-inflammatory drug (NSAID), such as ibuprofen (Advil, Motrin IB, others). Your discomfort also may be improved if you maintain good posture and avoid using repetitive movements and lifting heavy objects.
Last Updated Jun 4, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use