TMJ disorders
Overview
The temporomandibular (tem-puh-roe-man-DIB-u-lur) joint (TMJ) acts like a sliding hinge, connecting your jawbone to your skull. You have one joint on each side of your jaw. TMJ disorders — a type of temporomandibular disorder or TMD — can cause pain in your jaw joint and in the muscles that control jaw movement.
The exact cause of a person's TMJ disorder is often difficult to determine. Your pain may be due to a combination of factors, such as genetics, arthritis or jaw injury. Some people who have jaw pain also tend to clench or grind their teeth (bruxism), although many people habitually clench or grind their teeth and never develop TMJ disorders.
In most cases, the pain and discomfort associated with TMJ disorders is temporary and can be relieved with self-managed care or nonsurgical treatments. Surgery is typically a last resort after conservative measures have failed, but some people with TMJ disorders may benefit from surgical treatments.
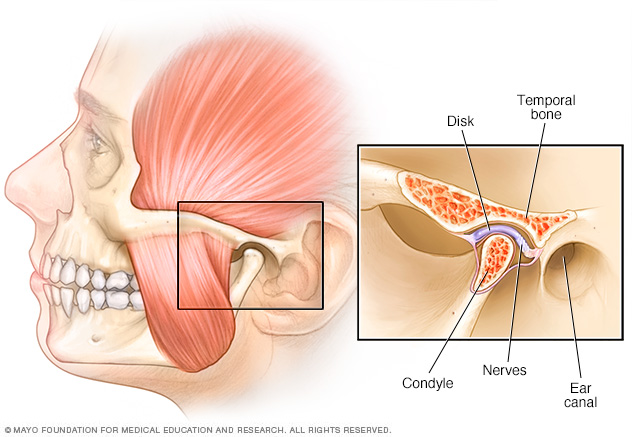
TMJ disorders affect the temporomandibular joint, located on each side of your head in front of your ears. A soft cartilage disk acts as a cushion between the bones of the joint, so the joint can move smoothly.
Symptoms
Signs and symptoms of TMJ disorders may include:
- Pain or tenderness of your jaw
- Pain in one or both of the temporomandibular joints
- Aching pain in and around your ear
- Difficulty chewing or pain while chewing
- Aching facial pain
- Locking of the joint, making it difficult to open or close your mouth
TMJ disorders can also cause a clicking sound or grating sensation when you open your mouth or chew. But if there's no pain or limitation of movement associated with your jaw clicking, you probably don't need treatment for a TMJ disorder.
When to see a doctor
Seek medical attention if you have persistent pain or tenderness in your jaw, or if you can't open or close your jaw completely. Your doctor, your dentist or a TMJ specialist can discuss possible causes and treatments for your problem.
Causes
The temporomandibular joint combines a hinge action with sliding motions. The parts of the bones that interact in the joint are covered with cartilage and are separated by a small shock-absorbing disk, which normally keeps the movement smooth.
Painful TMJ disorders can occur if:
- The disk erodes or moves out of its proper alignment
- The joint's cartilage is damaged by arthritis
- The joint is damaged by a blow or other impact
In many cases, however, the cause of TMJ disorders isn't clear.
Risk factors
Factors that may increase the risk of developing TMJ disorders include:
- Various types of arthritis, such as rheumatoid arthritis and osteoarthritis
- Jaw injury
- Long-term (chronic) grinding or clenching of teeth
- Certain connective tissue diseases that cause problems that may affect the temporomandibular joint
Diagnosis
Your doctor or dentist will discuss your symptoms and examine your jaw. He or she will probably:
- Listen to and feel your jaw when you open and close your mouth
- Observe the range of motion in your jaw
- Press on areas around your jaw to identify sites of pain or discomfort
If your doctor or dentist suspects a problem, you may need:
- Dental X-rays to examine your teeth and jaw
- CT scan to provide detailed images of the bones involved in the joint
- MRI to reveal problems with the joint's disk or surrounding soft tissue
TMJ arthroscopy is sometimes used in the diagnosis of a TMJ disorder. During TMJ arthroscopy, your doctor inserts a small thin tube (cannula) into the joint space, and a small camera (arthroscope) is then inserted to view the area and to help determine a diagnosis.
Treatment
In some cases, the symptoms of TMJ disorders may go away without treatment. If your symptoms persist, your doctor may recommend a variety of treatment options, often more than one to be done at the same time.
Medications
Along with other nonsurgical treatments, these medication options may help relieve the pain associated with TMJ disorders:
- Pain relievers and anti-inflammatories. If over-the-counter pain medications aren't enough to relieve TMJ pain, your doctor or dentist may prescribe stronger pain relievers for a limited time, such as prescription strength ibuprofen.
- Tricyclic antidepressants. These medications, such as amitriptyline, are used mostly for depression, but in low doses, they're sometimes used for pain relief, bruxism control and sleeplessness.
- Muscle relaxants. These types of drugs are sometimes used for a few days or weeks to help relieve pain caused by TMJ disorders created by muscle spasms.
Therapies
Nondrug therapies for TMJ disorders include:
- Oral splints or mouth guards (occlusal appliances). Often, people with jaw pain will benefit from wearing a soft or firm device inserted over their teeth, but the reasons why these devices are beneficial are not well-understood.
- Physical therapy. Along with exercises to stretch and strengthen jaw muscles, treatments might include ultrasound, moist heat and ice.
- Counseling. Education and counseling can help you understand the factors and behaviors that may aggravate your pain, so you can avoid them. Examples include teeth clenching or grinding, leaning on your chin, or biting fingernails.
Surgical or other procedures
When other methods don't help, your doctor might suggest procedures such as:
- Arthrocentesis. Arthrocentesis (ahr-throe-sen-TEE-sis) is a minimally invasive procedure that involves the insertion of small needles into the joint so that fluid can be irrigated through the joint to remove debris and inflammatory byproducts.
- Injections. In some people, corticosteroid injections into the joint may be helpful. Infrequently, injecting botulinum toxin type A (Botox, others) into the jaw muscles used for chewing may relieve pain associated with TMJ disorders.
- TMJ arthroscopy. In some cases, arthroscopic surgery can be as effective for treating various types of TMJ disorders as open-joint surgery. A small thin tube (cannula) is placed into the joint space, an arthroscope is then inserted and small surgical instruments are used for surgery. TMJ arthroscopy has fewer risks and complications than open-joint surgery does, but it has some limitations as well.
- Modified condylotomy. Modified condylotomy (kon-dih-LOT-uh-mee) addresses the TMJ indirectly, with surgery on the mandible, but not in the joint itself. It may be helpful for treatment of pain and if locking is experienced.
- Open-joint surgery. If your jaw pain does not resolve with more-conservative treatments and it appears to be caused by a structural problem in the joint, your doctor or dentist may suggest open-joint surgery (arthrotomy) to repair or replace the joint. However, open-joint surgery involves more risks than other procedures do and should be considered very carefully, after discussing the pros and cons.
If your doctor recommends surgery or other procedures, be sure to discuss the potential benefits and risks, and ask what all your options are.
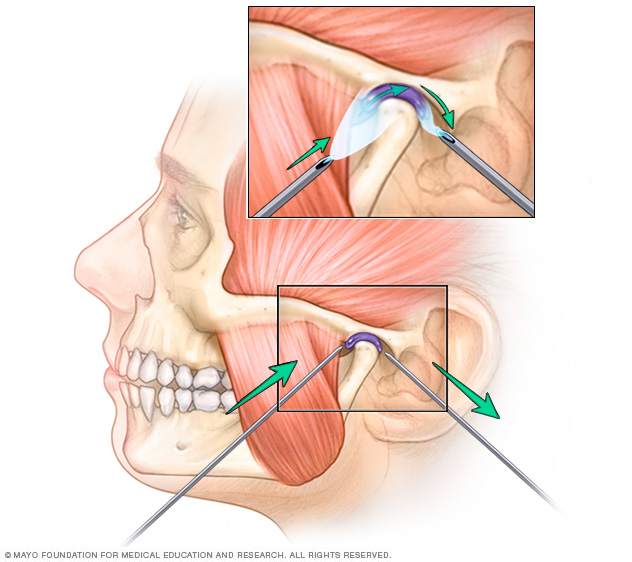
With arthrocentesis, tiny openings are inserted into the TMJ so that fluid can be flushed through the joint to remove debris.

With arthrocentesis, tiny openings are inserted into the TMJ so that fluid can be flushed through the joint to remove debris.
Lifestyle and home remedies
Becoming more aware of tension-related habits — clenching your jaw, grinding your teeth or chewing pencils — will help you reduce their frequency. The following tips may help you reduce symptoms of TMJ disorders:
- Avoid overuse of jaw muscles. Eat soft foods. Cut food into small pieces. Steer clear of sticky or chewy food. Avoid chewing gum.
- Stretching and massage. Your doctor, dentist or physical therapist may show you how to do exercises that stretch and strengthen your jaw muscles and how to massage the muscles yourself.
- Heat or cold. Applying warm, moist heat or ice to the side of your face may help alleviate pain.
Alternative medicine
Complementary and alternative medicine techniques may help manage the chronic pain often associated with TMJ disorders. Examples include:
- Acupuncture. A specialist trained in acupuncture treats chronic pain by inserting hair-thin needles at specific locations on your body.
- Relaxation techniques. Consciously slowing your breathing and taking deep, regular breaths can help relax tense muscles, which can reduce pain.
- Biofeedback. Electronic devices that monitor the tightness of specific muscles can help you practice effective relaxation techniques.
Preparing for an appointment
You'll probably first talk about your TMJ symptoms with your family doctor or dentist. If suggested treatments don't provide enough relief, you may be referred to a doctor who specializes in TMJ disorders.
What you can do
You may want to prepare a list that answers the following questions:
- When did your symptoms begin?
- Have you ever had this occur in the past?
- Has your level of stress increased recently?
- Do you have frequent headaches, neck aches or toothaches?
- What medications and supplements do you take regularly?
What to expect from your doctor or dentist
Your doctor may ask some of the following questions:
- Is your pain constant or do your symptoms come and go?
- Does any activity seem to trigger the pain?
- Does your jaw click or pop when you move it? Is that clicking painful?
- Is it difficult to open your mouth normally?
Your doctor or dentist will ask additional questions based on your responses, symptoms and needs. Preparing and anticipating questions will help you make the most of your time.
Last Updated Dec 28, 2018
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use