Uveitis
Overview
Uveitis is a form of eye inflammation. It affects the middle layer of tissue in the eye wall (uvea).
Uveitis (u-vee-I-tis) warning signs often come on suddenly and get worse quickly. They include eye redness, pain and blurred vision. The condition can affect one or both eyes, and it can affect people of all ages, even children.
Possible causes of uveitis are infection, injury, or an autoimmune or inflammatory disease. Many times a cause can't be identified.
Uveitis can be serious, leading to permanent vision loss. Early diagnosis and treatment are important to prevent complications and preserve your vision.
Symptoms
The signs, symptoms and characteristics of uveitis may include:
- Eye redness.
- Eye pain.
- Light sensitivity.
- Blurred vision.
- Dark, floating spots in your field of vision (floaters).
- Decreased vision.
Symptoms may occur suddenly and get worse quickly, though in some cases, they develop gradually. They may affect one or both eyes. Occasionally, there are no symptoms, and signs of uveitis are observed on a routine eye exam.
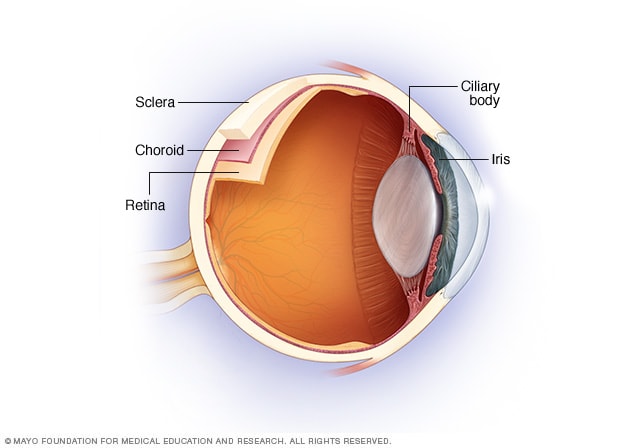
The uvea is the middle layer of tissue in the wall of the eye. It consists of the iris, the ciliary body and the choroid. When you look at your eye in the mirror, you will see the white part of the eye (sclera) and the colored part of the eye (iris).
The iris is located inside the front of the eye. The ciliary body is a structure behind the iris. The choroid is a layer of blood vessels between the retina and the sclera. The retina lines the inside of the back of the eye, like wallpaper. The inside of the back of the eye is filled with a gel-like liquid called vitreous.
The type of uveitis you have depends on which part or parts of the eye are inflamed:
- Anterior uveitis affects the inside of the front of your eye (between the cornea and the iris) and the ciliary body. It is also called iritis and is the most common type of uveitis.
- Intermediate uveitis affects the retina and blood vessels just behind the lens (pars plana) as well as the gel in the center of the eye (vitreous).
- Posterior uveitis affects a layer on the inside of the back of your eye, either the retina or the choroid.
- Panuveitis occurs when all layers of the uvea are inflamed, from the front to the back of your eye.
When to seek medical advice
Contact your doctor if you think you have the warning signs of uveitis. He or she may refer you to an eye specialist (ophthalmologist). If you're having significant eye pain and unexpected vision problems, seek immediate medical attention.
Causes
In about half of all cases, the specific cause of uveitis isn't clear, and the disorder may be considered an autoimmune disease that only affects the eye or eyes. If a cause can be determined, it may be one of the following:
- An autoimmune or inflammatory disorder that affects other parts of the body, such as sarcoidosis, systemic lupus erythematosus or Crohn's disease.
- Ankylosing spondylitis, a type of inflammatory disease that can cause some of the bones in the spine to fuse, leading to back pain. Uveitis is one of the most common complications of ankylosing spondylitis.
- An infection, such as cat-scratch disease, herpes zoster, syphilis, toxoplasmosis or tuberculosis.
- Medication side effect.
- Eye injury or surgery.
- Very rarely, a cancer that affects the eye, such as lymphoma.
Risk factors
People with changes in certain genes may be more likely to develop uveitis. Cigarette smoking has been associated with more difficult to control uveitis.
Complications
Left untreated, uveitis can cause complications, including:
- Retinal swelling (macular edema).
- Retinal scarring.
- Glaucoma.
- Cataracts.
- Optic nerve damage.
- Retinal detachment.
- Permanent vision loss.
Diagnosis
When you visit an eye specialist (ophthalmologist), they will likely conduct a complete eye exam and gather a thorough health history. The eye examination usually involves the following:
- Assessment of vision (with your glasses if you normally wear them) and the response of your pupils to light.
- Tonometry. A tonometry exam measures the pressure inside your eye (intraocular pressure). Numbing eyedrops may be used for this test.
- A slit-lamp examination. A slit lamp is a microscope that magnifies and illuminates the front of your eye with an intense line of light. This evaluation is necessary to identify microscopic inflammatory cells in the front of the eye.
- Ophthalmoscopy. Also known as funduscopy, this exam involves widening (dilating) the pupil with eye drops and shining a bright light into the eye to examine the back of the eye.
Your doctor also may recommend:
- Color photography of the inside of the eye (retina).
- Optical coherence tomography (OCT) imaging. This test maps the retina and choroid to reveal swelling in these layers.
- Fluorescein angiography or indocyanine green angiography. These tests require placement of an intravenous (IV) catheter in a vein in your arm in order to give a dye. This dye will reach the blood vessels in the eyes and allow photographs of swollen blood vessels inside the eyes.
- Analysis of aqueous or vitreous fluid from the eye.
- Blood tests.
- Imaging tests, radiography, CT or MRI scans.
If the ophthalmologist thinks an underlying condition may be the cause of your uveitis, you may be referred to another doctor for a general medical examination and laboratory tests.
Sometimes, it's difficult to find a specific cause for uveitis. Even if a specific cause is not identified, uveitis can still be treated successfully. In the majority of cases, identifying a cause for the uveitis does not lead to a cure. It is still necessary to use some form of treatment to control the swelling.
Treatment
If uveitis is caused by an underlying condition, treatment may focus on that specific condition. Usually the treatment for uveitis is the same regardless of the cause, as long as the cause is not infectious. The goal of treatment is to reduce the swelling in your eye, as well as in other parts of the body, if present. In some cases, treatment may be necessary for months to years. Several treatment options are available.
Medications
- Drugs that reduce inflammation. Your doctor may first prescribe eye drops with an anti-inflammatory medication, such as a corticosteroid. Eye drops are usually not enough to treat inflammation beyond the front of the eye, so a corticosteroid injection in or around the eye or corticosteroid tablets (taken by mouth) may be necessary.
- Drugs that control spasms. Eye drops that widen (dilate) the pupil may be prescribed to control spasms in the iris and ciliary body, which can help relieve eye pain.
- Drugs that fight bacteria or viruses. If uveitis is caused by an infection, your doctor may prescribe antibiotics, antiviral medications or other medicines, with or without corticosteroids, to bring the infection under control.
- Drugs that affect the immune system or destroy cells. You may need immunosuppressive drugs if your uveitis affects both eyes, doesn't respond well to corticosteroids or becomes severe enough to threaten your vision.
Some of these medicines can have serious eye-related side effects, such as glaucoma and cataracts. Medicine by mouth or injection can have side effects in other parts of the body outside the eyes. You may need to visit your doctor frequently for follow-up examinations and blood tests.
Surgical or other procedures
- Vitrectomy. Surgery to remove some of the vitreous in your eye is rarely used to diagnose or manage the condition.
-
A medication-releasing implant. For people with difficult-to-treat posterior uveitis, a device that's implanted in the eye may be an option. This device slowly releases corticosteroid into the eye for months or years depending on the implant used.
If people have not had cataract surgery, this treatment usually causes cataracts to develop. Also, up to 30% of patients will require treatment or monitoring for elevated eye pressure or glaucoma.
The speed of your recovery depends in part on the type of uveitis you have and how bad your symptoms are. Uveitis that affects the back of your eye (posterior uveitis or panuveitis, including retinitis or choroiditis) tends to heal more slowly than uveitis in the front of the eye (anterior uveitis or iritis). Severe inflammation takes longer to clear up than mild inflammation does.
Uveitis can come back. Make an appointment with your doctor if any of your symptoms reappear or worsen.
Preparing for your appointment
Your symptoms may prompt you to make an appointment with your primary doctor. You may be referred to a doctor who specializes in disorders of the eyes, called an ophthalmologist.
Here's some information to help you get ready for your appointment and know what to expect from your doctor.
What you can do
- List your symptoms, including any that may seem unrelated to the reason for which you scheduled the appointment.
- List key personal information, including any major illnesses, traumas or recent life changes.
- Bring a list of all medications, vitamins or supplements that you're taking.
- Ask a family member or friend to come with you. Sometimes it can be difficult to remember all of the information provided during an appointment. Someone who accompanies you may remember something that you missed or forgot. Additionally, someone who comes with you can drive you to your appointment, especially if your symptoms make it difficult to see properly.
- List questions to ask your doctor.
Preparing a list of questions can help cover all of the points that are important to you. For uveitis, some basic questions to ask include:
- What's the most likely cause of my eye problems?
- What else might be causing my symptoms?
- What kinds of tests do I need? Do these tests require any special preparation?
- Is uveitis temporary or long lasting?
- Will I lose my sight?
- What treatments are available, and which do you recommend?
- What types of side effects can I expect from treatment?
- Is there anything I can do to prevent this from happening again?
- I have other health conditions. How can I best manage these conditions together?
- Do you have any brochures or material I can take home with me?
- What websites do you recommend?
What to expect from your doctor
Your doctor is likely to ask you a number of questions, such as:
- When did you first begin experiencing symptoms?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms? Have they gotten worse?
- Does anything seem to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
- Have you ever had uveitis before?
- Do you have any other medical problems?
- Do you have arthritis?
- Do you have back problems?
- Have you had any recent skin rashes?
- Have you had any ulcerated sores in your mouth or on your genitalia?
- Have you had a recent upper respiratory infection or cold symptoms?
Last Updated Mar 7, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use