Breast cysts
Overview
Breast cysts are fluid-filled sacs inside the breast. They are usually noncancerous (benign). You may have one or multiple breast cysts. A breast cyst often feels like a grape or a water-filled balloon, but sometimes a breast cyst feels firm.
Breast cysts don't require treatment unless a cyst is large and painful or uncomfortable. In that case, draining the fluid from a breast cyst can ease symptoms.
Although breast cysts can be found in women of any age, they're more common in women before menopause, typically under age 50. Breast cysts also commonly occur in postmenopausal women who take hormone therapy.
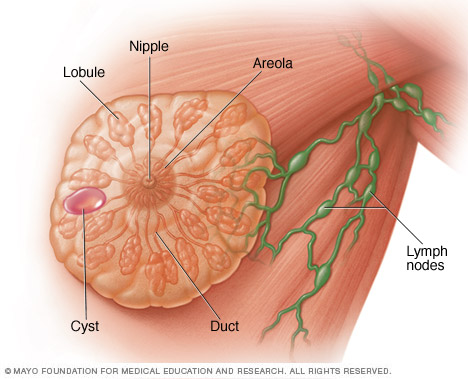
A breast cyst, an oval or round fluid-filled sac, may move slightly when you press on it.
Symptoms
Breast cysts may be found in one or both breasts. Signs and symptoms of a breast cyst include:
- A smooth, easily movable round or oval lump that may have smooth edges — which typically, though not always, indicates it's benign
- Nipple discharge that may be clear, yellow, straw colored or dark brown
- Breast pain or tenderness in the area of the breast lump
- An increase in breast lump size and breast tenderness just before your period
- A decrease in breast lump size and resolution of other symptoms after your period
Having breast cysts doesn't increase your risk of breast cancer. But having cysts may make it harder to find new breast lumps or other changes that might need evaluation by your doctor. Your breasts may feel lumpy and painful when you're menstruating, so it's important to be familiar with how your breasts feel throughout your menstrual cycle so that you'll know if something changes.
When to see a doctor
Normal breast tissue often feels lumpy or nodular. But if you feel a new breast lump that doesn't go away, gets bigger or persists after one or two menstrual cycles, see your doctor right away. Also see your doctor if you have new skin changes on one or both of your breasts.
Causes
Each of your breasts contains lobes of glandular tissue, arranged like petals of a daisy. The lobes are divided into smaller lobules that produce milk during pregnancy and breast-feeding. The supporting tissue that gives the breast its shape is made up of fatty tissue and fibrous connective tissue. Breast cysts develop as a result of fluid accumulation inside the glands in the breasts.
Breast cysts may be defined by their size:
- Microcysts may be seen during imaging tests, such as mammography or ultrasound, but are too small to feel.
- Macrocysts are large enough to be felt and can grow to about 1 to 2 inches (2.5 to 5 centimeters) in diameter.
Experts don't know exactly what causes breast cysts. They may develop as a result of hormonal changes from monthly menstruation.
Diagnosis
Diagnosis of a breast cyst usually includes a breast exam; imaging tests, such as a breast ultrasound or mammogram; and possibly fine-needle aspiration or a breast biopsy.
Breast exam
After discussing your symptoms and health history, your doctor will physically examine the breast lump and check for any other breast abnormalities. Because your doctor can't tell from a clinical breast exam alone whether a breast lump is a cyst, you'll need another test. This is usually either an imaging test or fine-needle aspiration.
Imaging tests
Needed tests may include:
- Mammography. Large cysts and clusters of small cysts can usually be seen with mammography. But microcysts can be difficult or impossible to see on a mammogram.
- Breast ultrasound. This test can help your doctor determine whether a breast lump is fluid filled or solid. A fluid-filled area usually indicates a breast cyst. A solid-appearing mass most likely is a noncancerous lump, such as a fibroadenoma, but solid lumps also could be breast cancer.
Your doctor may recommend a biopsy to further evaluate a mass that appears solid. If your doctor can easily feel a breast lump, he or she may skip imaging tests and perform fine-needle aspiration to drain the fluid and collapse the cyst.
Fine-needle aspiration
During a fine-needle aspiration, your doctor inserts a thin needle into the breast lump and attempts to withdraw (aspirate) fluid. Often, fine-needle aspiration is done using ultrasound to guide accurate placement of the needle. If fluid comes out and the breast lump goes away, your doctor can make a breast cyst diagnosis immediately.
- If the fluid is not bloody and has a straw-colored appearance and the breast lump disappears, you need no further testing or treatment.
- If the fluid appears bloody or the breast lump doesn't disappear, your doctor may send a sample of the fluid for lab testing and refer you to a breast surgeon or to a radiologist — a doctor trained to perform imaging exams and procedures — for follow-up.
- If no fluid is withdrawn, your doctor will likely recommend an imaging test, such as a diagnostic mammogram or ultrasound. The lack of fluid or a breast lump that doesn't disappear after aspiration suggests that the breast lump — or at least a portion of it — is solid. A sample of the tissue may be collected to check for cancer.
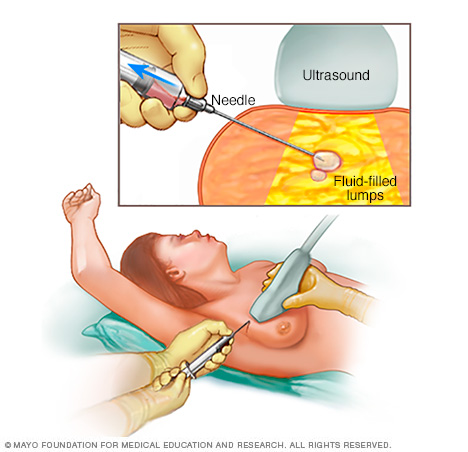
During fine-needle aspiration, a special needle is inserted into a breast lump, and any fluid is removed (aspirated). Ultrasound — a procedure that uses sound waves to create images of your breast on a monitor — might be used to help place the needle.
Treatment
No treatment is necessary for simple breast cysts — those that are fluid filled and don't cause any symptoms — that are confirmed on breast ultrasound or after a fine-needle aspiration. Many cysts will disappear with no treatment. If a cyst persists, feels firmer or you notice skin changes on the skin over the cyst, follow up with your doctor.
Fine-needle aspiration
Fine-needle aspiration may be used to diagnose and treat a breast cyst if all the fluid can be removed from the cyst during the procedure, and then your breast lump disappears and your symptoms resolve.
For some breast cysts, however, you may need to have fluid drained more than once. Recurrent or new cysts are common. If a breast cyst persists through two to three menstrual cycles and grows larger, see your doctor for further evaluation.
Hormone use
Using birth control pills (oral contraceptives) to regulate your menstrual cycles may help reduce the recurrence of breast cysts. But because of possible significant side effects, birth control pills or other hormone therapy, such as tamoxifen, is usually recommended only for women with severe symptoms. Discontinuing hormone therapy after menopause may also help prevent breast cysts.
Surgery
Surgery to remove a breast cyst is necessary only in unusual circumstances. Surgery may be considered if an uncomfortable breast cyst recurs month after month or if a breast cyst contains blood-tinged fluid or shows other worrisome signs.
Lifestyle and home remedies
To minimize discomfort associated with breast cysts, you might try these measures:
- Wear a supportive bra. Supporting your breasts with a bra that fits well may help relieve some discomfort.
- Apply a compress. Either a warm compress or an ice pack can help relieve pain.
- Avoid caffeine. Studies haven't shown a link between caffeine and breast cysts. However, some women find symptom relief after eliminating caffeine from their diets. Consider reducing or eliminating caffeine — in beverages, as well as in foods such as chocolate — to see if your symptoms improve.
- Consider trying over-the-counter pain medications if your doctor recommends them. Some types of breast pain may be eased by the use of acetaminophen (Tylenol, others) or nonsteroidal anti-inflammatory drugs, such as ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve, others).
Alternative medicine
Talk with your doctor about any vitamins, herbal remedies or other dietary supplements that you're taking or thinking of taking. There is no evidence that any of these products help breast cyst symptoms, and they may cause side effects.
Preparing for an appointment
You'll likely see your primary care provider to evaluate new breast lumps or changes in your breasts. You may be referred to a breast-health specialist based on a clinical breast exam or findings on an imaging test.
What you can do
The first evaluation focuses on your medical history. You'll discuss your symptoms, their relation to your menstrual cycle and any other relevant information. To prepare for this discussion, make lists that include:
- All of your symptoms, even if they seem unrelated to the reason you scheduled the appointment
- Key personal information, including major stresses or recent life changes
- All medications, vitamins, herbal remedies and supplements that you regularly take
- Questions to ask your doctor, from most important to least important to be sure you cover the points you're most concerned about
Basic questions to ask your doctor include:
- What might be causing my symptoms?
- Does having cysts increase my risk of breast cancer?
- What kinds of tests do I need?
- Will I need treatment? If so, what treatments are available?
- Are there any restrictions I'll need to follow?
- Are there any printed materials that I can take home? What websites do you recommend?
Don't hesitate to ask questions anytime you don't understand something.
What to expect from your doctor
Be prepared to answer questions that your doctor may ask, such as:
- When did you first notice the breast cyst or lump?
- Have you noticed a change in the size of the breast cyst or lump?
- What symptoms have you experienced, and how long have you had them?
- Do your symptoms occur in one or both breasts?
- Have any symptoms changed over time?
- Do you have breast pain? If so, how severe is it?
- Do you have nipple discharge? If so, does it occur in one or both breasts?
- How does your menstrual cycle affect the breast cyst or lump?
- When was your last mammogram?
- Do you have a family history of breast cysts or lumps?
- Have you previously had a breast cyst or lump, a breast biopsy or breast cancer?
Last Updated Jan 9, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



