Contact dermatitis
Overview
Contact dermatitis is an itchy rash caused by direct contact with a substance or an allergic reaction to it. The rash isn't contagious, but it can be very uncomfortable.
Many substances can cause this reaction, such as cosmetics, fragrances, jewelry and plants. The rash often shows up within days of exposure.
To treat contact dermatitis successfully, you need to identify and avoid the cause of your reaction. If you avoid the substance causing the reaction, the rash often clears up in 2 to 4 weeks. You can try soothing your skin with a cool, wet cloth and other self-care steps.
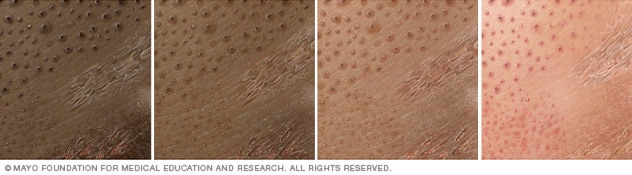
Illustration of contact dermatitis on different skin colors. Contact dermatitis can appear as an itchy rash.
Symptoms
Contact dermatitis shows up on skin that has been directly exposed to the substance causing the reaction. For example, the rash may show up along a leg that brushed against poison ivy. The rash can develop within minutes to hours of exposure, and it can last 2 to 4 weeks.
Signs and symptoms of contact dermatitis vary widely and may include:
- An itchy rash
- Leathery patches that are darker than usual (hyperpigmented), typically on brown or Black skin
- Dry, cracked, scaly skin, typically on white skin
- Bumps and blisters, sometimes with oozing and crusting
- Swelling, burning or tenderness
When to see a doctor
See your health care provider if:
- The rash is so itchy that you can't sleep or go about your day
- The rash is severe or widespread
- You're worried about how your rash looks
- The rash doesn't get better within three weeks
- The rash involves the eyes, mouth, face or genitals
Seek immediate medical care in the following situations:
- You think your skin is infected. Clues include fever and pus oozing from blisters.
- It's hard to breathe after inhaling burning weeds.
- Your eyes or nasal passages hurt after inhaling smoke from burning poison ivy.
- You think an ingested substance has damaged the lining of your mouth or digestive tract.
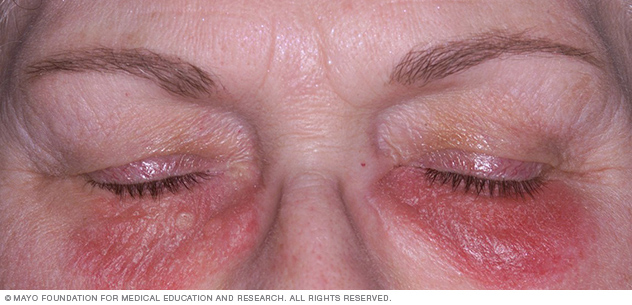
Contact dermatitis often affects skin directly exposed to an offending substance. Here, the rash is likely caused by cosmetics.
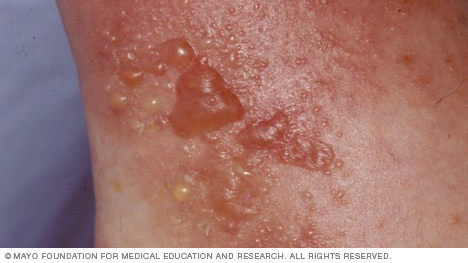
Here, the blisters are caused by contact with the oily substance in poison ivy (urushiol) that causes allergic reactions.
Causes
Contact dermatitis is caused by exposure to a substance that irritates your skin or triggers an allergic reaction. The substance could be one of thousands of known allergens and irritants. Often people have irritant and allergic reactions at the same time.
Irritant contact dermatitis is the most common type. This nonallergic skin reaction occurs when an irritant damages your skin's outer protective layer.
Some people react to strong irritants after a single exposure. Others may develop a rash after repeated exposures to even mild irritants, such as soap and water. And some people develop a tolerance to the substance over time.
Common irritants include:
- Solvents
- Rubber gloves
- Bleach and detergents
- Hair products
- Soap
- Airborne substances
- Plants
- Fertilizers and pesticides
Allergic contact dermatitis occurs when a substance to which you're sensitive (allergen) triggers an immune reaction in your skin. It often affects only the area that came into contact with the allergen. But it may be triggered by something that enters your body through foods, flavorings, medicine, or medical or dental procedures (systemic contact dermatitis).
People often become sensitized to allergens after many contacts with it over years. Once you develop an allergy to a substance, even a small amount of it can cause a reaction.
Common allergens include:
- Nickel, which is used in jewelry, buckles and many other items
- Medications, such as antibiotic creams
- Balsam of Peru, which is used in many products, such as perfumes, toothpastes, mouth rinses and flavorings
- Formaldehyde, which is in preservatives, cosmetics and other products
- Personal care products, such as body washes, hair dyes and cosmetics
- Plants such as poison ivy and mango, which contain a highly allergenic substance called urushiol
- Airborne allergens, such as ragweed pollen and spray insecticides
- Products that cause a reaction when you're in the sun (photoallergic contact dermatitis), such as some sunscreens and cosmetics
Children develop allergic contact dermatitis from the usual offenders and also from exposure to diapers, baby wipes, jewelry used in ear piercing, clothing with snaps or dyes, and so on.
Risk factors
The risk of contact dermatitis may be higher in people who have certain jobs and hobbies. Examples include:
- Agricultural workers
- Cleaners
- Construction workers
- Cooks and others who work with food
- Florists
- Hair stylists and cosmetologists
- Health care workers, including dental workers
- Machinists
- Mechanics
- Scuba divers or swimmers, due to the rubber in face masks or goggles
Complications
Contact dermatitis can lead to an infection if you repeatedly scratch the affected area, causing it to become wet and oozing. This creates a good place for bacteria or fungi to grow and may cause an infection.
Prevention
You can take the following steps to help prevent contact dermatitis:
- Avoid irritants and allergens. Try to identify and avoid the cause of your rash. For ear and body piercings, use jewelry made of hypoallergenic material, such as surgical steel or gold.
- Wash your skin. For poison ivy, poison oak or poison sumac, you might be able to remove most of the rash-causing substance if you wash your skin right away after coming into contact with it. Use a mild, fragrance-free soap and warm water. Rinse completely. Also wash any clothing or other items that may have come into contact with a plant allergen, such as poison ivy.
- Wear protective clothing or gloves. Face masks, goggles, gloves and other protective items can shield you from irritating substances, including household cleansers.
- Apply an iron-on patch to cover metal fasteners next to your skin. This can help you avoid a reaction to jean snaps, for example.
- Apply a barrier cream or gel. These products can provide a protective layer for your skin. For example, a nonprescription skin cream containing bentoquatam (Ivy Block) may prevent or lessen your skin's reaction to poison ivy.
- Use moisturizer. Regularly applying moisturizing lotions can help restore your skin's outermost layer and keep your skin supple.
- Take care around pets. Allergens from plants, such as poison ivy, can cling to pets and then be spread to people. Bathe your pet if you think it got into poison ivy or something similar.
Diagnosis
Your health care provider may be able to diagnose contact dermatitis by talking to you about your signs and symptoms. You might be asked questions to help identify the cause of your condition and uncover clues about the trigger substance. And you'll likely undergo a skin exam to assess the rash.
Your health care provider may suggest a patch test to identify the cause of your rash. In this test, small amounts of potential allergens are put on sticky patches. Then the patches are placed on your skin. They stay on your skin for 2 to 3 days. During this time, you'll need to keep your back dry. Then your health care provider checks for skin reactions under the patches and determines whether further testing is needed.
This test can be useful if the cause of your rash isn't apparent or if your rash recurs often. But the redness indicating a reaction can be hard to see on brown or Black skin, which may lead to a missed diagnosis.
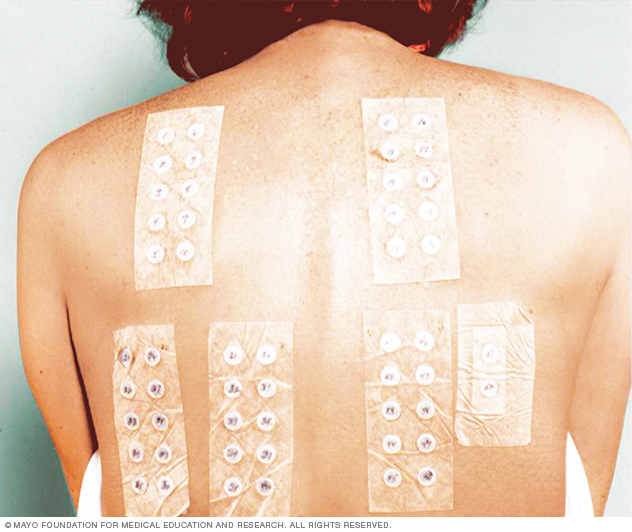
Patch testing can be helpful in determining if you're allergic to a specific substance. Small amounts of different substances are placed on your skin under a sticky coating. After 2 to 3 days, your health care provider checks for a skin reaction under the patches.
Treatment
If home care steps don't ease your signs and symptoms, your health care provider may prescribe medications. Examples include:
- Steroid creams or ointments. These are applied to the skin to help soothe the rash. You might apply prescription topical steroids, such as clobetasol 0.05% or triamcinolone 0.1%. Talk with your health care provider about how many times a day to apply it and for how many weeks.
- Pills. In severe cases, your health care provider may prescribe pills you take by mouth (oral medications) to reduce swelling, relieve itching or fight a bacterial infection.
Lifestyle and home remedies
To help reduce itching and soothe inflamed skin, try these self-care approaches:
- Avoid the irritant or allergen. The key to this is identifying what's causing your rash and staying away from it. Your health care provider may give you a list of products that typically contain the substance that affects you. Also ask for a list of products that are free of the substance that affects you.
- Apply an anti-itch cream or ointment. Put on the itchy area 1% hydrocortisone cream or ointment (Cortizone 10, others). This is a nonprescription product that you can buy at a drugstore. Use it 1 to 2 times a day for a few days. Or try calamine lotion. Whatever product you use, try cooling it in the refrigerator before applying.
- Take an anti-itch drug. An oral antihistamine, such as diphenhydramine (Advil PM, Benadryl, others), which may also help you sleep better. A nonprescription antihistamine that won't make you so drowsy is loratadine (Alavert, Claritin, others).
- Apply cool, wet compresses. Place a cool, wet cloth over the rash for 15 to 30 minutes several times a day.
- Protect your skin. Avoid scratching. Trim your nails. If you can't keep from scratching an itchy area, cover it with a dressing. Leave blisters alone. While your skin heals, stay out of the sun or use other sun protection measures.
- Soak in a soothing cool bath. Soak the affected area in cool water for 20 minutes. Sprinkle the water an oatmeal-based bath product (Aveeno).
- Protect your hands. Rinse and dry hands well and gently after washing. Use moisturizers throughout the day — on top of any medicated cream you're using. And choose gloves based on what you're protecting your hands from. For example, plastic gloves lined with cotton are good if your hands are often wet.
Preparing for an appointment
You're likely to start by seeing your primary care provider, who might then refer you to a doctor who specializes in skin disorders (dermatologist).
Because appointments can be brief, it's a good idea to be well prepared for your appointment.
What you can do
- List your signs and symptoms, including when they began and how long they've lasted.
- Avoid any substances that you think may have caused the rash.
- Make notes about any new products you've started using and any substances that regularly come in contact with your affected skin areas.
- Make a list of all the medications and supplements you take. Even better, take along the original bottles and a list of the dosages and directions. Include any creams or lotions you're using.
- List questions to ask your health care provider.
For contact dermatitis, some basic questions you could ask include:
- What might be causing my signs and symptoms?
- Are tests needed to confirm the diagnosis?
- What treatments are available, and which do you recommend?
- Is this condition temporary or chronic?
- Can I wait to see if the condition goes away on its own?
- Will scratching spread the rash?
- Will popping the blisters spread the rash?
- What skin care routines do you recommend to improve my condition?
- How can I prevent this in the future?
What to expect from your doctor
Your health care provider is likely to ask you questions such as the following:
- When did you begin noticing symptoms?
- How often do you have symptoms?
- Have your symptoms been continuous or occasional? Do they get better over the weekend or during vacation?
- Does anything seem to make your symptoms better or worse?
- Have you started using any new soaps, lotions, cosmetics or household products?
- Does your work or a hobby involve using products that often come in contact with your skin?
Last Updated May 2, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



