Eisenmenger syndrome
Overview
Eisenmenger (I-sun-meng-ur) syndrome is a long-term complication of an unrepaired heart problem present at birth (congenital heart defect). Eisenmenger syndrome is life-threatening.
In Eisenmenger syndrome, there is irregular blood flow in the heart and lungs. This causes the blood vessels in the lungs to become stiff and narrow. Blood pressure rises in the lungs' arteries (pulmonary arterial hypertension). Eisenmenger syndrome permanently damages the blood vessels in the lungs.
Early diagnosis and repair of congenital heart defects usually prevents Eisenmenger syndrome. If it does develop, treatment involves regular medical visits and medications to improve symptoms.
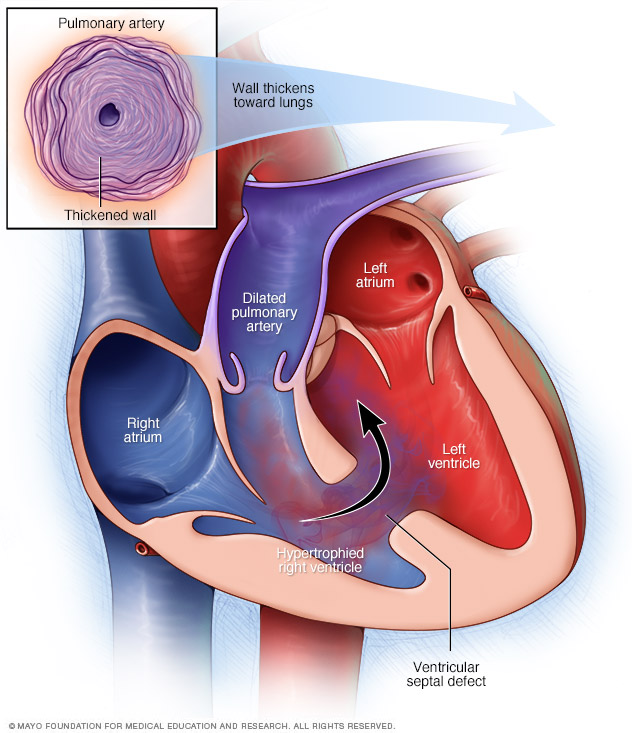
Eisenmenger syndrome is most often a complication of having a hole between two chambers of the heart. Here, a hole between the heart's main pumping chambers (ventricular septal defect) causes more blood to flow to the lungs' arteries. Eventually this causes these blood vessels to stiffen and narrow, increasing pressure in the lungs' arteries. The high pressure causes the walls of the right lower heart chamber (right ventricle) to thicken (hypertrophy).
Symptoms
Symptoms of Eisenmenger syndrome include:
- Blue or gray skin color due to low oxygen levels (cyanosis)
- Chest pain or tightness
- Coughing up blood
- Dizziness or fainting
- Easily tiring and shortness of breath with activity
- Headaches
- Large, rounded fingernails or toenails (clubbing)
- Numbness or tingling in fingers or toes
- Shortness of breath while at rest
- Skipped or racing heartbeats (palpitations)
When to see a doctor
If you have any symptoms of Eisenmenger syndrome, see your health care provider. Make an appointment even if you have never been diagnosed with a heart problem. Symptoms such as shortness of breath or chest pain require medical attention.
Causes
Eisenmenger syndrome is usually caused by an unrepaired hole (shunt) between the main blood vessels or chambers of the heart. A shunt is a heart problem present at birth (congenital heart defect).
To understand how Eisenmenger syndrome affects the heart and lungs, it's helpful to know how the heart typically works.
How the heart works
The heart is divided into chambers — two upper chambers (atria) and two lower chambers (ventricles).
- The right side of the heart moves blood to the lungs through blood vessels (pulmonary arteries).
- In the lungs, blood picks up oxygen and then returns to the left side of the heart through the pulmonary veins.
- The left side of the heart then pumps the blood through the aorta and out to the rest of the body.
Heart valves control the flow of blood into and out of the chambers of the heart. These valves open to allow blood to move to the next chamber or to one of the arteries, and then close to keep blood from flowing backward.
How Eisenmenger syndrome develops
Heart problems present at birth (congenital heart defects) that can cause Eisenmenger syndrome include:
- Ventricular septal defect. This is the most common cause of Eisenmenger syndrome. There is a hole (shunt) in the wall of tissue that divides the right and left sides of the heart's main pumping chambers (ventricles).
- Atrioventricular canal defect. This is a large hole in the center of the heart where the walls between the upper chambers (atria) and lower chambers (ventricles) meet. Some of the valves in the heart also may not work properly.
- Atrial septal defect. This is a hole in the wall of tissue that divides the right and left sides of the upper chambers of the heart (atria).
- Patent ductus arteriosus. This is an opening between the pulmonary artery that carries oxygen-poor blood to the lungs and the artery that carries oxygen-rich blood to the rest of the body (aorta).
In any of these heart problems, blood flows in a way it usually doesn't. As a result, pressure rises in the pulmonary artery. Over time, the increased pressure damages the smaller blood vessels in the lungs. The damaged blood vessel walls make it difficult to pump blood to the lungs.
In Eisenmenger syndrome, there's increased blood pressure in the side of the heart that has oxygen-poor blood (blue blood). The blue blood goes through the hole (shunt) in the heart or blood vessels. Oxygen-rich and oxygen-poor blood now mix. This causes low blood oxygen levels.
Risk factors
A family history of congenital heart defects increases the risk of similar heart problems in a baby. If you've been diagnosed with Eisenmenger syndrome, talk to your health care provider about screening other family members for congenital heart defects.
Complications
Eisenmenger syndrome is a life-threatening condition. The outlook for people diagnosed with Eisenmenger syndrome depends on the specific cause and if there are other medical conditions.
Without proper treatment and monitoring, complications of Eisenmenger syndrome may include:
- Low blood oxygen levels. The reversed blood flow through the heart reduces oxygen to the body's tissues and organs. Without prompt treatment, the oxygen levels worsen over time.
- Irregular heart rhythms (arrhythmias). Eisenmenger syndrome causes the heart walls to get bigger and thicker. It also causes oxygen levels to lower. These changes may cause irregular heart rhythms. Some arrhythmias increase the risk of blood clots that can cause heart attacks or strokes.
- Sudden cardiac arrest. This is the sudden loss of heart activity due to an irregular heart rhythm. If not treated immediately, sudden cardiac arrest can quickly lead to death. Survival is possible with fast, appropriate medical care.
- Heart failure. The increased pressure in the heart can cause the heart muscle to weaken. It becomes harder for the heart to pump blood.
- Bleeding in the lungs. Eisenmenger syndrome can cause life-threatening bleeding in the lungs and airways. This can cause you to cough up blood and further lower your blood oxygen levels. Bleeding can also occur in other parts of the body.
- Stroke. If a blood clot travels from the right to left side of the heart, the clot may block a blood vessel in the brain, leading to a stroke.
- Kidney problems. Low oxygen levels in the blood may lead to problems with the kidneys.
- Gout. Eisenmenger syndrome can increase the risk of a type of arthritis called gout. Gout causes sudden, severe attacks of pain and swelling in one or more joints, usually the big toe.
- Heart infection. People with Eisenmenger syndrome have a higher risk of a heart infection called endocarditis.
- Pregnancy risks. During pregnancy, the heart and lungs have to work harder to support the growing baby. Because of this, pregnancy with Eisenmenger syndrome poses a high risk of death for both you and the baby. If you have Eisenmenger syndrome, talk to your care provider about your specific pregnancy risks.
Diagnosis
To diagnose Eisenmenger syndrome, your health care provider does a physical exam and asks medical history questions.
Tests to diagnose Eisenmenger syndrome may include:
- Blood tests. A complete blood cell count is often done. The red blood cell count may be high in Eisenmenger syndrome. Blood tests are also done to check kidney and liver function and iron level.
- Electrocardiogram (ECG). This quick and painless test measures the electrical activity of the heart. During an ECG, sensors (electrodes) are attached to the chest and sometimes to the arms or legs. Wires connect the sensors to a machine, which displays or prints results. An ECG can show how fast or slow the heart is beating.
- Chest X-ray. A chest X-ray helps show the condition of the heart and lungs.
- Echocardiogram. An ultrasound of the heart is called an echocardiogram. This test uses sound waves to create detailed images of the heart in motion. An echocardiogram shows blood flow through the heart.
- Computerized tomography (CT) scan. A CT scan uses X-rays to create cross-sectional images of specific parts of the body. This test may be done to get more details about the lungs and lung arteries. Dye (contrast) may be given by IV for this test. The dye helps blood vessels show up more clearly on the images. CT scan images provide more-detailed information than plain X-rays do.
- Magnetic resonance imaging (MRI) scan of the lungs. This test uses magnetic fields and radio waves to create detailed images of the blood vessels in the lungs.
- Cardiac catheterization. A long, thin flexible tube (catheter) is inserted in a blood vessel, usually in the groin or wrist, and guided to the heart. Dye flows through the catheter to the arteries. The dye helps the arteries show up more clearly on X-ray images and video. During this test, the provider may measure blood pressure in the blood vessels and heart's chambers. Cardiac catheterization can also help show the size of any holes in the heart and blood flow in the area.
- Walking test. This six-minute walking test is done to see how well you can tolerate a mild level of exercise.
Treatment
The goals of Eisenmenger syndrome treatment are to control symptoms, improve quality of life and prevent serious complications.
If you are diagnosed with Eisenmenger syndrome, you'll be referred to a heart specialist (cardiologist). Regular health checkups — at least once a year — are an important part of Eisenmenger syndrome treatment. It's helpful to find a cardiologist who has experience treating people who have congenital heart defects.
Medications
Medications are the main treatment for Eisenmenger syndrome. They can't cure the condition, but they can help improve your quality of life. You need regular medical checkups when taking medications. Your provider checks for any changes in blood pressure, pulse rate and fluid levels.
Medications for Eisenmenger syndrome include:
- Heart rhythm drugs. These medications, called anti-arrhythmics, help control the heart rhythm and prevent irregular heartbeats.
- Iron supplements. Your health care provider may prescribe these if your iron level is too low. Don't start taking iron supplements without talking to your provider first.
- Aspirin or blood-thinning medications. If you have had a stroke, blood clot or certain types of irregular heart rhythms, your health care provider may recommend aspirin or a blood thinner such as warfarin (Jantoven). These medications can increase the risk of bleeding. Never take them unless your provider tells you to do so. Ask your provider if other pain medications, such as ibuprofen (Advil, Motrin IB, others), are safe for you.
- Drugs for pulmonary arterial hypertension. A medication called bosentan (Tracleer) may be used to increase the supply of blood to the lungs. If you take bosentan, you'll need monthly liver tests because the drug can damage the liver.
- Sildenafil and tadalafil. Sildenafil (Revatio, Viagra) and tadalafil (Cialis, Adcirca, others) are sometimes used to treat high blood pressure in the pulmonary arteries caused by Eisenmenger syndrome. These drugs open the blood vessels in the lungs so blood flows more easily.
- Antibiotics. Certain dental and medical procedures may allow bacteria to enter the bloodstream. Depending on your condition, you may need to take antibiotics before having such procedures. Antibiotics can help prevent a heart infection (endocarditis). If you have any type of congenital heart disease, talk to your dentist and other care providers about your risks and whether you need preventive antibiotics.
Surgeries or other procedures
Health care providers don't recommend surgery to repair the hole (shunt) in the heart once Eisenmenger syndrome has developed.
Surgeries or procedures that may be done to treat symptoms or complications of Eisenmenger include:
- Blood withdrawal (phlebotomy). If your red blood cell count becomes too high and is causing symptoms such as headaches, difficulty concentrating or vision problems, your provider may recommend this procedure. Phlebotomy should not be done routinely and should only be done after talking with a congenital heart disease expert. You should receive IV fluids when having this procedure to help replace the lost fluids.
- Transplant. Some people who have Eisenmenger syndrome may need surgery to replace the heart or lungs if other treatments don't work.
If you need a procedure or surgery for Eisenmenger, consider getting care at a medical center with providers who have experience in congenital heart diseases.
Lifestyle and home remedies
If you're diagnosed with Eisenmenger syndrome, proper treatment and precautions can help improve quality of life. Try these strategies:
- Avoid dehydration. Ask your provider how much fluid you need each day. You may need to drink more fluids when you are sick or when you are in a heated room or on an airplane.
- Ask about exercise restrictions. If you have Eisenmenger syndrome, you shouldn't do strenuous exercise or sports. But you may be able to do less intense physical activities. Talk to your health care provider about what type of physical activity is best for you.
- Avoid high altitudes. Because of the low oxygen levels at high altitudes, people with Eisenmenger syndrome should not spend a lot of time at high altitudes. The American College of Cardiology and the American Heart Association say to avoid exposure to altitudes of 5,000 feet (1,524 meters) or higher above sea level. Discuss travel by airplane or to high altitudes with your care provider for specific recommendations.
- Avoid situations that can greatly lower blood pressure. These include sitting in a hot tub or sauna or taking long hot baths or showers. Such activities lower blood pressure and may cause fainting or even death. If you have Eisenmenger syndrome, also avoid activities that cause prolonged straining, such as lifting heavy objects or weights.
- Use medications and supplements with caution. Many supplements and medicines, including those bought without a prescription, can affect blood pressure. Some may increase the risk of bleeding or affect kidney function in those who have Eisenmenger syndrome. Talk to your health care provider before taking any supplements or medications.
- Get a flu shot. Avoiding respiratory infections is important for people with Eisenmenger syndrome. Experts recommend getting a flu shot every year and a pneumonia vaccination every five years.
- Avoid secondhand smoke and quit using tobacco products. Cigarette smoke and other tobacco products can increase the risk of complications. It's important to avoid illegal drugs too.
Birth control and pregnancy
If you have Eisenmenger syndrome, becoming pregnant poses serious health risks — and can be life-threatening — for you and the baby. It's critical that pregnancy be avoided if you have Eisenmenger syndrome.
Effective contraceptive methods include vasectomy, an intrauterine device (IUD) or a contraceptive hormonal implant such as Nexplanon. Tying of the fallopian tubes (tubal ligation) is a very effective form of contraception. But it's less often recommended due to the risks posed by having even minor surgery.
Birth control pills containing estrogen aren't recommended for those who have Eisenmenger syndrome. Estrogen increases the risk of developing blood clots that could potentially block an artery to the heart, brain or lungs. Using a barrier method alone, such as a condom or diaphragm, isn't recommended due to the risk of failure.
Coping and support
A diagnosis of Eisenmenger syndrome can be scary. Although treatments can help symptoms and improve prognosis, you may feel worried or anxious.
You may find that joining a support group is helpful. Some people find that talking with others who've been through similar situations brings comfort and encouragement. Ask your health care provider if there are any local support groups.
Children with a congenital heart defect or Eisenmenger syndrome may have emotional and physical difficulties that can affect home and school life. For example, a long recovery time from surgeries or procedures may lead to developmental delays. Talk to your health care provider about ways you can help your child. This may include support groups or a visit to a therapist or psychologist.
Preparing for an appointment
Eisenmenger syndrome is a complicated condition. There's often a lot to discuss at a medical appointment. So it's a good idea to be prepared. Here's some information to help you get ready for your appointment and know what to expect from your health care provider.
What you can do
- Make note of any previous heart treatments. Include medications, surgeries or procedures you've received for a heart problem.
- Be aware of any pre-appointment restrictions. When you make the appointment, ask whether there's anything you need to do in advance, such as fill out forms or restrict your diet. For example, some imaging tests require you to avoid food or drink for a period of time beforehand.
- Write down any symptoms, including any that may seem unrelated to Eisenmenger syndrome. Try to recall when they began. Be specific, such as days, weeks and months. Try to avoid vague terms such as "some time ago."
- Write down key personal information, including a family history of heart defects, pulmonary hypertension, lung disease, heart disease, stroke, high blood pressure or diabetes, and any major stresses or recent life changes.
- Make a list of all medications, vitamins and supplements that you're taking. Include dosages. Also, be sure to tell your health care provider if you've recently stopped taking any medications.
- Take a family member or friend along, if possible. Sometimes it can be difficult to remember all the information provided to you during an appointment. Someone who goes with you may remember something that you missed or forgot.
- Write down questions to ask your care provider.
Your time with your health care provider may be limited. Prepare a list of questions to help you make the most of your time together. List your questions from most important to least important in case time runs out. For Eisenmenger syndrome, some basic questions to ask your provider include:
- What are other possible causes for my symptoms?
- What kinds of tests do I need?
- What treatment do I need?
- What are the side effects of the treatment you're recommending?
- Do I need to avoid or limit exercise?
- How often do I need follow-up visits?
- I have other health conditions. How can I best manage them together?
- Can you recommend a specialist who has experience treating Eisenmenger syndrome?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend?
In addition to the questions you've prepared to ask your health care provider, don't hesitate to ask additional questions during your appointment.
What to expect from your doctor
Your health care provider is likely to ask you many questions. Being ready to answer them may save time to go over information you want to spend more time on. Your provider may ask the following questions:
- Have you ever been diagnosed with a heart problem or high blood pressure in the lungs? If so, what treatments did you have for your condition?
- Has one of your care providers ever said you had a heart murmur but didn't look for a cause? If so, when was this?
- When did your symptoms begin?
- Do you always have symptoms or do they come and go?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- Does anything make your symptoms worse?
Last Updated Aug 4, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




