Hiatal hernia
Overview
A hiatal hernia happens when the upper part of the stomach bulges through the large muscle that separates the abdomen and the chest. The muscle is called the diaphragm.
The diaphragm has a small opening called a hiatus. The tube used for swallowing food, called the esophagus, passes through the hiatus before connecting to the stomach. In a hiatal hernia, the stomach pushes up through that opening and into the chest.
A small hiatal hernia usually doesn't cause problems. You may never know you have one unless your healthcare team discovers it when checking for another condition.
But a large hiatal hernia can allow food and acid to back up into your esophagus. This can cause heartburn. Self-care measures or medicines can usually relieve these symptoms. A very large hiatal hernia might need surgery.
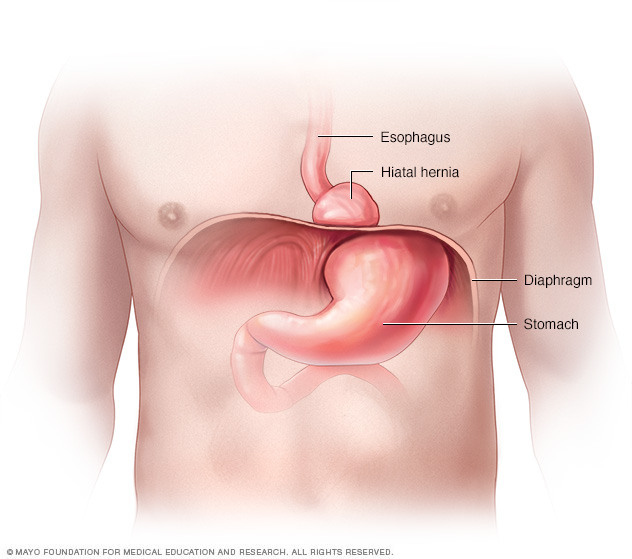
A hiatal hernia occurs when the upper part of the stomach bulges through the diaphragm into the chest cavity.
Symptoms
Most small hiatal hernias cause no symptoms. But larger hiatal hernias can cause:
- Heartburn.
- Backward flow of swallowed food or liquids into the mouth, called regurgitation.
- Backflow of stomach acid into the esophagus, called acid reflux.
- Trouble swallowing.
- Chest or abdominal pain.
- Feeling full soon after you eat.
- Shortness of breath.
- Vomiting of blood or passing of black stools, which could mean bleeding in the digestive tract.
When to see a doctor
Make an appointment with your doctor or other healthcare professional if you have any lasting symptoms that worry you.
Causes
A hiatal hernia occurs when weakened muscle tissue allows your stomach to bulge up through your diaphragm. It's not always clear why this happens. But a hiatal hernia might be caused by:
- Age-related changes in your diaphragm.
- Injury to the area, for example, after trauma or certain types of surgery.
- Being born with a very large hiatus.
- Constant and intense pressure on the surrounding muscles. This can happen while coughing, vomiting, straining during a bowel movement, exercising or lifting heavy objects.
Risk factors
Hiatal hernias are most common in people who are:
- Age 50 or older.
- Obese.
Diagnosis
A hiatal hernia is often discovered during a test or procedure to determine the cause of heartburn or pain in the chest or upper abdomen. These tests or procedures include:
- X-ray of your upper digestive system. X-rays are taken after you drink a chalky liquid that coats and fills the inside lining of your digestive tract. The coating allows your healthcare team to see an outline of your esophagus, stomach and upper intestine.
- A procedure to look at the esophagus and stomach, called an endoscopy. Endoscopy is a procedure to examine your digestive system with a long, thin tube with a tiny camera, called an endoscope. The endoscope is passed down your throat and looks at the inside of your esophagus and stomach and checks for inflammation.
- A test to measure muscle contractions of the esophagus, called an esophageal manometry. This test measures the rhythmic muscle contractions in your esophagus when you swallow. Esophageal manometry also measures the coordination and force used by the muscles of your esophagus.
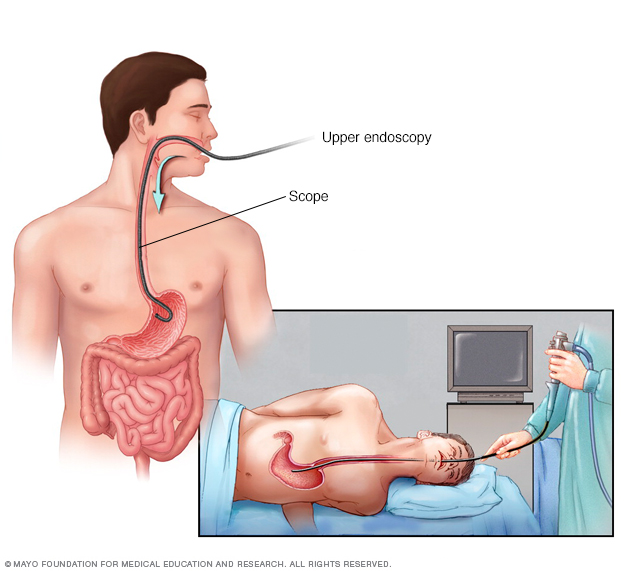
During an upper endoscopy, a healthcare professional inserts a thin, flexible tube equipped with a light and camera down the throat and into the esophagus. The tiny camera provides a view of the esophagus, stomach and the beginning of the small intestine, called the duodenum.
Treatment
Most people with a hiatal hernia don't experience any symptoms and won't need treatment. If you experience symptoms, such as frequent heartburn and acid reflux, you may need medicine or surgery.
Medicines
If you experience heartburn and acid reflux, your healthcare professional may recommend:
- Antacids that neutralize stomach acid. Antacids may provide quick relief. Overuse of some antacids can cause side effects, such as diarrhea or sometimes kidney problems.
- Medicines to reduce acid production. These medicines are known as H-2-receptor blockers. They include cimetidine (Tagamet HB), famotidine (Pepcid AC) and nizatidine (Axid AR). Stronger versions are available by prescription.
- Medicines that block acid production and heal the esophagus. These medicines are known as proton pump inhibitors. They are stronger acid blockers than H-2-receptor blockers and allow time for damaged esophageal tissue to heal. Proton pump inhibitors available without a prescription include lansoprazole (Prevacid 24HR) and omeprazole (Prilosec, Zegerid). Stronger versions are available in prescription form.
Surgery
Sometimes a hiatal hernia requires surgery. Surgery may help people who aren't helped by medicines to relieve heartburn and acid reflux. Surgery also may help people who have complications such as serious inflammation or narrowing of the esophagus.
Surgery to repair a hiatal hernia may involve pulling the stomach down into the abdomen and making the opening in the diaphragm smaller. Surgery also may involve reshaping the muscles of the lower esophagus. This helps keep the contents of the stomach from coming back up. Sometimes, hiatal hernia surgery is combined with weight-loss surgery, such as a sleeve gastrectomy.
Surgery may be performed using a single incision in the chest wall, called a thoracotomy. Surgery also may be performed using a technique called laparoscopy. In laparoscopic surgery, a surgeon inserts a tiny camera and special tools through several small incisions in the abdomen. The operation is then performed by a surgeon who views images from inside the body that are displayed on a video monitor.
Lifestyle and home remedies
Making a few lifestyle changes may help control the symptoms caused by a hiatal hernia. Try to:
- Eat several smaller meals throughout the day rather than a few large meals.
- Don't eat foods that trigger heartburn. These include fatty or fried foods, tomato sauce, alcohol, chocolate, mint, garlic, onion, and caffeine.
- Avoid lying down after a meal or eating late in the day.
- Maintain a healthy weight.
- Stop smoking.
- Elevate the head of your bed 8 inches (20 centimeters).
Preparing for an appointment
Make an appointment with a doctor or other healthcare professional if you have any symptoms that worry you.
If you've been diagnosed with a hiatal hernia and your problems persist after you make lifestyle changes and start medicine, you might be referred to a doctor who specializes in digestive diseases, called a gastroenterologist.
Because appointments can be brief, it's a good idea to be prepared. Here's some information to help you get ready.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down symptoms you're experiencing, including any that may not seem related to the reason for which you scheduled the appointment.
- Write down key personal information, including major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements you're taking and the doses.
- Take a family member or friend along. Sometimes it can be difficult to remember all the information provided during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your healthcare team.
Your time with your doctor or other healthcare professional is limited, so preparing a list of questions can help you make the most of your time together. List your questions from most important to least important in case time runs out. For hiatal hernia, some basic questions to ask include:
- What's likely causing my symptoms?
- Other than the most likely cause, what are other possible causes for my symptoms?
- What tests do I need?
- What's the best course of action?
- What are the alternatives to the primary approach you're suggesting?
- I have these other health conditions. How can I best manage them together?
- Are there restrictions I need to follow?
- Should I see a specialist?
- Are there brochures or other printed material I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Be prepared to answer questions, such as:
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- How serious are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Last Updated Dec 23, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





