Hives and angioedema
Overview
Hives — also known as urticaria (ur-tih-KAR-e-uh) — is a skin reaction that causes itchy welts that range in size from small spots to large blotches. Hives can be triggered by many situations and substances, including certain foods and medications.
Angioedema can arise with hives or alone. It causes swelling in the deeper layers of skin, often around the face and lips. Short-lived (acute) hives and angioedema are common. Most times, they are harmless, clear up within in a day and don't leave any lasting marks, even without treatment. Hives that last longer than six weeks are called chronic hives.
Hives and angioedema are usually treated with antihistamine medication. Angioedema can be life-threatening if swelling of the tongue or in the throat blocks the airway.
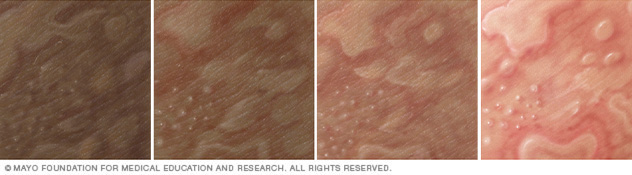
Illustration of hives on different skin colors. Hives can cause swollen, itchy welts. Hives is also called urticaria.
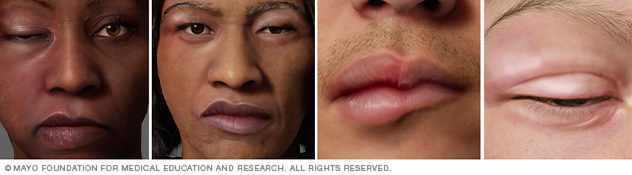
Illustration of angioedema on different skin colors. Angioedema causes swelling in the deeper layers of skin, often of the face and lips. It often goes away within a day.
Symptoms
Hives
The welts associated with hives can be:
- Skin-colored, reddish on white skin, or purplish on black and brown skin
- Itchy, ranging from mild to intense
- Round, oval or worm-shaped
- As small as a pea or as large as a dinner plate
Most hives appear quickly and go away within 24 hours. This is known as acute hives. Chronic hives can last for months or years.
Angioedema
Angioedema is a reaction similar to hives that affects deeper layers of the skin. It can appear with hives or alone. Signs and symptoms include:
- Welts that form in minutes to hours
- Swelling, especially around the eyes, cheeks or lips
- Mild pain and warmth in the affected areas
When to see a doctor
You can usually treat mild cases of hives or angioedema at home. See your health care provider if your symptoms continue for more than a few days.
If you think your hives or angioedema was caused by a known allergy to food or a medication, your symptoms may be an early sign of an anaphylactic reaction. Seek emergency care if you feel your tongue, lips, mouth or throat swelling or if you're having trouble breathing.
Causes
For most people who experience acute hives and angioedema, the exact cause can't be identified. The conditions are sometimes caused by:
- Foods. Many foods can trigger reactions in people with sensitivities. Shellfish, fish, peanuts, tree nuts, soy, eggs and milk are frequent offenders.
- Medications. Many medications may cause hives or angioedema, including penicillins, aspirin, ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve) and blood pressure medications.
- Airborne allergens. Pollen and other allergens that you breathe in can trigger hives, sometimes accompanied by upper and lower respiratory tract symptoms.
- Insect bites and infections. Other causes of acute hives and angioedema are insect bites and infections.
Risk factors
Hives and angioedema are common. You may be at increased risk of hives and angioedema if you:
- Have had hives or angioedema before
- Have had other allergic reactions
- Have a family history of hives, angioedema or hereditary angioedema
Complications
Severe angioedema can be life-threatening if swelling of the tongue or in the throat blocks the airway.
Prevention
To lower your likelihood of experiencing hives or angioedema, take the following precautions:
- Avoid known triggers. If you know what has triggered your hives, try to avoid that substance.
- Bathe and change your clothes. If pollen or animal contact has triggered your hives in the past, take a bath or shower and change your clothes if you're exposed to pollen or animals.
Diagnosis
To diagnose hives or angioedema, your doctor will likely look at your welts or areas of swelling and ask about your medical history. You may also need blood tests or an allergy skin test.
Treatment
If your symptoms are mild, you may not need treatment. Hives and angioedema often clear up on their own. But treatment can offer relief from intense itching, serious discomfort or symptoms that persist.
Medications
Treatments for hives and angioedema may include prescription drugs:
- Anti-itch drugs. The standard treatment for hives and angioedema is antihistamines that don't make you drowsy. These medications reduce itching, swelling and other allergy symptoms. They're available in nonprescription and prescription formulations.
- Drugs that suppress the immune system. If antihistamines are not effective, your doctor might prescribe a drug that can calm an overactive immune system.
- Drugs for hereditary angioedema. If you have the type of angioedema that runs in families, you may take medication to relieve symptoms and keep the levels of certain proteins in your blood at levels that do not cause symptoms.
- Anti-inflammatory drugs. For severe hives or angioedema, doctors may prescribe a short course of an oral corticosteroid drug — such as prednisone — to reduce swelling, inflammation and itching.
Emergency situations
For a severe attack of hives or angioedema, you may need a trip to the emergency room and an emergency injection of epinephrine — a type of adrenaline. If you have had a serious attack or your attacks recur despite treatment, your doctor may have you carry a penlike device that will allow you to self-inject epinephrine in emergencies.
Lifestyle and home remedies
If you're experiencing mild hives or angioedema, these tips may help relieve your symptoms:
- Avoid triggers. These can include foods, medications, pollen, pet dander, latex and insect stings. If you think a medication caused your rash, stop using it and contact your primary care provider. Some studies suggest that stress or fatigue can trigger hives.
- Use an anti-itch drug available without a prescription. A nonprescription oral antihistamine, such as loratadine (Alavert, Claritin, others), cetirizine (Zyrtec Allergy, others) or diphenhydramine (Benadryl Allergy, others), may help relieve itching. Consider whether you might prefer a type that doesn't cause drowsiness. Ask your pharmacist about options.
- Apply cold. Covering the affected area with a cold washcloth or rubbing an ice cube over it for a few minutes can help soothe the skin and prevent scratching.
- Take a comfortably cool bath. Find relief from itching in a cool shower or bath. Some people may also benefit from bathing in cool water sprinkled with baking soda or oatmeal powder (Aveeno, others), but this isn't a solution for long-term control of chronic itching.
- Wear loose, smooth-textured cotton clothing. Avoid wearing clothing that's rough, tight, scratchy or made from wool.
- Protect your skin from the sun. Apply sunscreen liberally about a half hour before going outdoors. When outdoors, seek shade to help relieve discomfort.
Preparing for an appointment
You're likely to start by seeing your primary care doctor. In some cases when you call to set up an appointment, you may be referred immediately to a skin disease specialist (dermatologist) or to an allergy specialist.
What you can do
Here are some tips to help you get ready for your appointment.
- List your signs and symptoms, when they occurred, and how long they lasted.
- List any medications you're taking, including vitamins, herbs and supplements. Even better, take the original bottles and a list of the doses and directions.
- List questions to ask your doctor.
For hives and angioedema, questions you may want to ask include:
- What is likely causing my symptoms?
- Do I need any tests to confirm the diagnosis?
- What are other possible causes for my symptoms?
- Is my condition likely temporary or chronic?
- What is the best course of action?
- What are the alternatives to the primary approach that you're suggesting?
- Do I need prescription medication, or can I use nonprescription medications to treat the condition?
- What results can I expect?
- Can I wait to see if the condition goes away on its own?
What to expect from your doctor
Your doctor is likely to ask you a number of questions, such as:
- When did you first begin experiencing symptoms?
- What did your skin reaction look like when it first appeared?
- Have your symptoms changed over time?
- Have you noticed anything that makes your symptoms worse or better?
- Do your skin lesions mainly itch, or do they burn or sting?
- Do your skin lesions go away completely without leaving a bruise or a mark?
- Do you have any known allergies?
- Have you ever had a similar skin reaction before?
- Have you tried a new food for the first time, changed laundry products or adopted a new pet?
- What prescriptions, nonprescription medications and supplements are you taking?
- Have you started taking any new medications or started a new course of a medication you've taken before?
- Has your overall health changed recently? Have you had any fevers or have you lost weight?
- Has anyone else in your family ever had this kind of skin reaction? Do other family members have any known allergies?
- What at-home treatments have you used?
Last Updated Oct 27, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



