Infant reflux
Overview
Infant reflux is when a baby spits up liquid or food. It happens when stomach contents move back up from a baby's stomach into the esophagus. The esophagus is the muscular tube that connects the mouth to the stomach.
Reflux happens in healthy infants many times a day. As long as your baby is healthy, content and growing well, reflux is not a cause for concern. Sometimes called gastroesophageal reflux (GER), the condition becomes less common as a baby gets older. It's unusual for infant reflux to continue after age 18 months.
In rare cases, infant reflux leads to weight loss or growth that lags behind other children of the same age and sex. These symptoms may indicate a medical problem. These medical problems may include an allergy, a blockage in the digestive system or gastroesophageal reflux disease (GERD). GERD is a more serious form of GER that causes serious health issues.
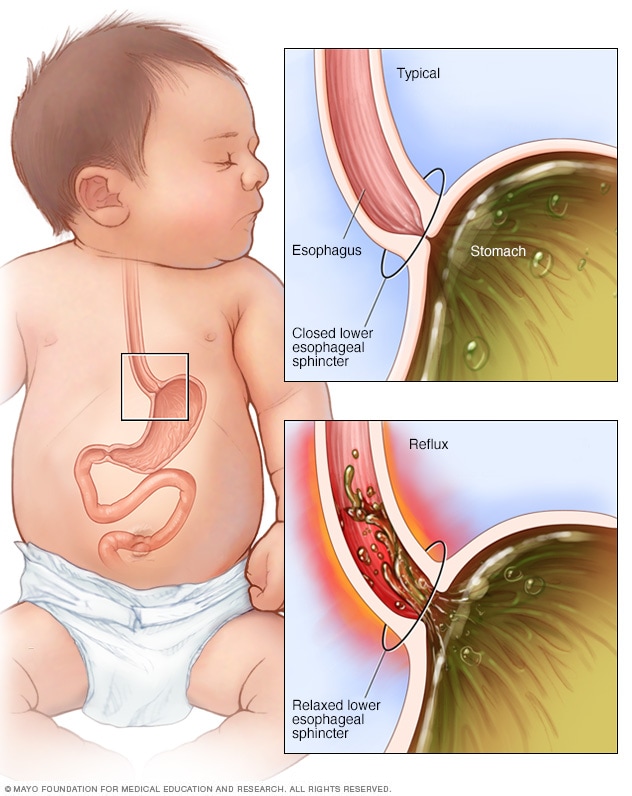
If the muscle between the esophagus and the stomach relaxes when the stomach is full, food might flow up the baby's esophagus. This muscle is called the lower esophageal sphincter.
Symptoms
In most cases, infant reflux isn't a cause for concern. It's unusual for stomach contents to have enough acid to irritate the throat or esophagus and cause symptoms.
When to see a doctor
See your baby's health care provider if your baby:
- Isn't gaining weight.
- Consistently spits up forcefully, causing stomach contents to shoot out of the mouth. This is called projectile vomiting.
- Spits up green or yellow fluid.
- Spits up blood or stomach contents that look like coffee grounds.
- Refuses to feed or eat.
- Has blood in the stool.
- Has difficulty breathing or a cough that won't go away.
- Begins spitting up at age 6 months or older.
- Is unusually irritable after eating.
- Doesn't have much energy.
Some of these symptoms may indicate serious but treatable conditions. These include GERD or a blockage in the digestive tract.
Causes
In infants, the ring of muscle between the esophagus and the stomach is not yet fully developed. This muscle is called the lower esophageal sphincter (LES). When the LES is not fully developed, it allows stomach contents to flow back up into the esophagus. Over time, the LES typically matures. It opens when your baby swallows and remains tightly closed at other times, keeping stomach contents where they belong.
Some factors that contribute to infant reflux are common in babies and often can't be avoided. These include lying flat most of the time and being fed an almost completely liquid diet.
Sometimes, infant reflux can be caused by more-serious conditions, such as:
- GERD. The reflux has enough acid to irritate and damage the lining of the esophagus.
- Pyloric stenosis. A muscular valve allows food to leave the stomach and enter the small intestine as part of digestion. In pyloric stenosis, the valve thickens and becomes larger than it should. The thickened valve then traps food in the stomach and blocks it from entering the small intestine.
- Food intolerance. A protein in cow's milk is the most common trigger.
- Eosinophilic esophagitis. A certain type of white blood cell builds up and injures the lining of the esophagus. This white blood cell is called an eosinophil.
- Sandifer syndrome. This causes irregular tilting and rotation of the head, and movements that resemble seizures. It's a rarely seen consequence of GERD.
Risk factors
Infant reflux is common. But some things make it more likely that a baby will experience infant reflux. These include:
- Premature birth
- Lung conditions, such as cystic fibrosis
- Conditions that affect the nervous system, such as cerebral palsy
- Previous surgery on the esophagus
Complications
Infant reflux usually resolves on its own. It rarely causes problems for babies.
If your baby has a more serious condition such as GERD, your baby's growth may lag behind that of other children. Some research indicates that babies who have frequent episodes of spitting up might be more likely to develop GERD later in childhood.
Diagnosis
Your baby's health care provider will start with a physical exam and ask you questions about your baby's symptoms. If your baby is healthy, growing as expected and seems content, then testing usually isn't needed. In some cases, however, your health care provider might recommend:
- Ultrasound. This imaging test can detect pyloric stenosis.
- Lab tests. Blood and urine tests can help identify or rule out possible causes of recurring vomiting and poor weight gain.
- Esophageal pH monitoring. To measure the acidity in your baby's esophagus, the doctor will insert a thin tube through the baby's nose or mouth and into the esophagus. The tube is attached to a device that monitors acidity. Your baby might need to stay in the hospital while being monitored.
- X-rays. These images can detect problems in the digestive tract, such as a blockage. Your baby may be given a contrast liquid from a bottle before the test. This liquid is usually barium.
- Upper endoscopy. The doctor passes a special tube that has a camera lens and a light through your baby's mouth into the esophagus, stomach and the upper part of the small intestine. This tube is called an endoscope. Tissue samples may be taken for analysis. For infants and children, endoscopy usually is done under general anesthesia. General anesthesia is a combination of medicines that causes a sleep-like state before surgery or other medical procedure.
Treatment
For most babies, making some changes to feeding will ease infant reflux until it resolves on its own.
Medications
Reflux medications aren't typically used to treat uncomplicated reflux in children. But your child’s health care provider may recommend an acid-blocking medication for several weeks or months. Acid-blocking medications include cimetidine (Tagamet HB), famotidine (Pepcid AC) and omeprazole magnesium (Prilosec). Your child's provider may recommend an acid-blocking medication if your baby:
- Has poor weight gain, and changes in feeding haven't worked
- Refuses to feed
- Has an inflamed esophagus
- Has chronic asthma
Surgery
In rare cases, your baby may need surgery. This is only done if your baby is not gaining enough weight or has trouble breathing because of reflux. During the surgery, the LES between the esophagus and the stomach is tightened. This prevents acid from flowing back up into the esophagus.
Lifestyle and home remedies
To minimize reflux:
- Feed your baby in an upright position. Then, hold your baby in a sitting position for 30 minutes after feeding. Gravity can help stomach contents stay where they belong. Be careful not to jostle or jiggle your baby while the food is settling.
- Try smaller, more frequent feedings. Feed your baby a little bit less than usual if you're bottle-feeding, or cut back a little on nursing time.
- Take time to burp your baby. Frequent burps during and after feeding can keep air from building up in your baby's stomach.
- Put baby to sleep on the back. Most babies should be placed on their backs to sleep, even if they have reflux.
Keep in mind that infant reflux is usually little cause for concern. Just keep plenty of burp cloths handy as you wait for your baby's reflux to stop.
Preparing for an appointment
You may start by seeing your primary care provider. Or you may be referred immediately to a specialist in children's digestive diseases, called a pediatric gastroenterologist.
What you can do
When you make the appointment, ask if there's anything you need to do in advance. Make a list of:
- Your baby's symptoms, including any that seem unrelated to the reason for your baby's appointment.
- Key personal information, including major stresses, recent life changes and family medical history
- All medications, vitamins or other supplements your baby takes, including the doses
- Questions to ask your baby's doctor.
- Caregivers and how they feed your baby
Take a family member or friend along, if possible, to help you remember the information you're given.
For infant reflux, some basic questions to ask your doctor include:
- What's likely causing my baby's symptoms?
- Other than the most likely cause, what are other possible causes for my baby's symptoms?
- What tests does my baby need?
- Is my baby's condition likely temporary or chronic?
- What's the best course of action?
- What are the alternatives to the primary approach you're suggesting?
- My baby has other health conditions. How can I best manage them together?
- Are there restrictions I need to follow for my baby?
- Should I take my baby to a specialist?
- Are there brochures or other printed material I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your doctor is likely to ask you questions, such as:
- When did your baby's symptoms begin?
- Have your baby's symptoms been continuous or occasional?
- How severe are your baby's symptoms?
- What, if anything, seems to improve your baby's condition?
- What, if anything, seems to worsen your baby's condition?
What you can do in the meantime
Avoid doing anything that seems to worsen your baby's symptoms.
Last Updated Jan 24, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





