Lactose intolerance
Overview
People with lactose intolerance are unable to fully digest the sugar (lactose) in milk. As a result, they have diarrhea, gas and bloating after eating or drinking dairy products. The condition, which is also called lactose malabsorption, is usually harmless, but its symptoms can be uncomfortable.
Too little of an enzyme produced in your small intestine (lactase) is usually responsible for lactose intolerance. You can have low levels of lactase and still be able to digest milk products. But if your levels are too low you become lactose intolerant, leading to symptoms after you eat or drink dairy.
Most people with lactose intolerance can manage the condition without having to give up all dairy foods.
Symptoms
The signs and symptoms of lactose intolerance usually begin from 30 minutes to two hours after eating or drinking foods that contain lactose. Common signs and symptoms include:
- Diarrhea
- Nausea, and sometimes, vomiting
- Stomach cramps
- Bloating
- Gas
When to see a doctor
Make an appointment with your doctor if you frequently have symptoms of lactose intolerance after eating dairy foods, particularly if you're worried about getting enough calcium.
Causes
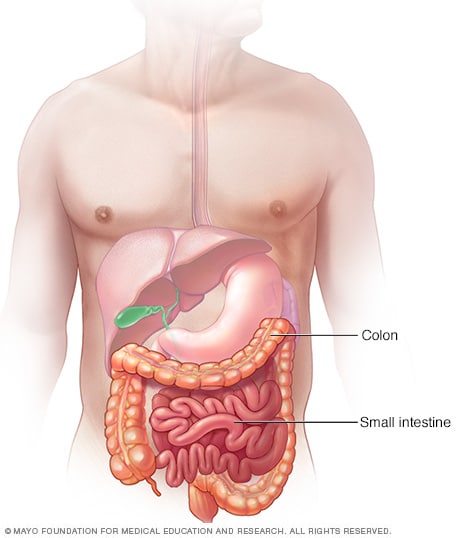
Lactose intolerance occurs when your small intestine doesn't produce enough of an enzyme (lactase) to digest milk sugar (lactose).
Normally, lactase turns milk sugar into two simple sugars — glucose and galactose — which are absorbed into the bloodstream through the intestinal lining.
If you're lactase deficient, lactose in your food moves into the colon instead of being processed and absorbed. In the colon, normal bacteria interact with undigested lactose, causing the signs and symptoms of lactose intolerance.
There are three types of lactose intolerance. Different factors cause the lactase deficiency underlying each type.
Primary lactose intolerance
People who develop primary lactose intolerance — the most common type — start life producing enough lactase. Infants, who get all their nutrition from milk, need lactase.
As children replace milk with other foods, the amount of lactase they produce normally drops, but usually remains high enough to digest the amount of dairy in a typical adult diet. In primary lactose intolerance, lactase production falls off sharply by adulthood, making milk products difficult to digest.
Secondary lactose intolerance
This form of lactose intolerance occurs when your small intestine decreases lactase production after an illness, injury or surgery involving your small intestine. Diseases associated with secondary lactose intolerance include intestinal infection, celiac disease, bacterial overgrowth and Crohn's disease.
Treatment of the underlying disorder might restore lactase levels and improve signs and symptoms, though it can take time.
Congenital or developmental lactose intolerance
It's possible, but rare, for babies to be born with lactose intolerance caused by a lack of lactase. This disorder is passed from generation to generation in a pattern of inheritance called autosomal recessive, meaning that both the mother and the father must pass on the same gene variant for a child to be affected. Premature infants can also have lactose intolerance because of an insufficient lactase level.
Risk factors
Factors that can make you or your child more prone to lactose intolerance include:
- Increasing age. Lactose intolerance usually appears in adulthood. The condition is uncommon in babies and young children.
- Ethnicity. Lactose intolerance is most common in people of African, Asian, Hispanic and American Indian descent.
- Premature birth. Infants born prematurely might have reduced levels of lactase because the small intestine doesn't develop lactase-producing cells until late in the third trimester.
- Diseases affecting the small intestine. Small intestine problems that can cause lactose intolerance include bacterial overgrowth, celiac disease and Crohn's disease.
- Certain cancer treatments. If you've had radiation therapy for cancer in your stomach or you have intestinal complications from chemotherapy, your risk of developing lactose intolerance increases.
Diagnosis
Your doctor might suspect lactose intolerance based on your symptoms and your response to reducing the amount of dairy foods in your diet. Your doctor can confirm the diagnosis by conducting one or more of the following tests:
- Hydrogen breath test. After you drink a liquid that contains high levels of lactose, your doctor measures the amount of hydrogen in your breath at regular intervals. Breathing out too much hydrogen indicates that you aren't fully digesting and absorbing lactose.
- Lactose tolerance test. Two hours after drinking a liquid that contains high levels of lactose, you'll undergo blood tests to measure the amount of glucose in your bloodstream. If your glucose level doesn't rise, it means your body isn't properly digesting and absorbing the lactose-filled drink.
Treatment
In people with lactose intolerance caused by an underlying condition, treating the condition might restore the body's ability to digest lactose, although that process can take months. For other causes, you might avoid the discomfort of lactose intolerance by following a low-lactose diet.
To lower the amount of lactose in your diet:
- Limit milk and other dairy products
- Include small servings of dairy products in your regular meals
- Eat and drink lactose-reduced ice cream and milk
- Add a liquid or powder lactase enzyme to milk to break down the lactose
Self care
With some trial and error, you might be able to predict your body's response to foods containing lactose and figure out how much you can eat or drink without discomfort. Few people have such severe lactose intolerance that they have to cut out all milk products and be wary of nondairy foods or medications that contain lactose.
Maintain good nutrition
Reducing the dairy products doesn't mean you can't get enough calcium. Calcium is found in many other foods, such as:
- Broccoli and leafy green vegetables
- Calcium-fortified products, such as cereals and juices
- Canned salmon or sardines
- Milk substitutes, such as soy milk and rice milk
- Oranges
- Almonds, Brazil nuts and dried beans
Also make sure you get enough vitamin D, which is typically supplied in fortified milk. Eggs, liver and yogurt also contain vitamin D, and your body makes vitamin D when you spend time in the sun.
Even without restricting dairy foods, though, many adults don't get enough vitamin D. Talk to your doctor about taking vitamin D and calcium supplements to be sure.
Limit dairy products
Most people with lactose intolerance can enjoy some milk products without symptoms. You might tolerate low-fat milk products, such as skim milk, better than whole-milk products. It also might be possible to increase your tolerance to dairy products by gradually introducing them into your diet.
Ways to change your diet to minimize symptoms of lactose intolerance include:
- Choosing smaller servings of dairy. Sip small servings of milk — up to 4 ounces (118 milliliters) at a time. The smaller the serving, the less likely it is to cause gastrointestinal problems.
- Saving milk for mealtimes. Drink milk with other foods. This slows the digestive process and may lessen symptoms of lactose intolerance.
-
Experimenting with an assortment of dairy products. Not all dairy products have the same amount of lactose. For example, hard cheeses, such as Swiss or cheddar, have small amounts of lactose and generally cause no symptoms.
Ice cream and milk contain the most lactose, but the high fat content in ice cream might allow you to eat it without symptoms. You might tolerate cultured milk products such as yogurt because the bacteria used in the culturing process naturally produce the enzyme that breaks down lactose.
- Buying lactose-reduced or lactose-free products. You can find these products at most supermarkets in the dairy section.
- Using lactase enzyme tablets or drops. Over-the-counter tablets or drops containing the lactase enzyme (Lactaid, others) might help you digest dairy products. You can take tablets just before a meal or snack. Or the drops can be added to a carton of milk. These products don't help everyone who has lactose intolerance.
Alternative medicine
Probiotics
Probiotics are living organisms present in your intestines that help maintain a healthy digestive system. Probiotics are also available as active or "live" cultures in some yogurts and as supplements in capsule form.
They are sometimes used for gastrointestinal conditions, such as diarrhea and irritable bowel syndrome. They might also help your body digest lactose. Probiotics are generally considered safe and might be worth a try if other methods don't help.
Preparing for your appointment
Start by seeing your family doctor if you have signs or symptoms that suggest you may have lactose intolerance. Here's some information to help you get ready.
What you can do
When you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
Make a list of:
- Your symptoms, including any that may seem unrelated to the reason for which you scheduled the appointment, and when they occur
- All medications, vitamins or other supplements you take, including doses
- Questions to ask your doctor
Questions for your doctor about lactose intolerance might include:
- Are there other possible causes for my symptoms besides lactose intolerance?
- What tests do I need?
- What are my treatment options?
- Must I stop eating all dairy products?
- How can I be certain that I'm getting enough calcium in my diet?
- Should I see a dietitian?
- I have these other health conditions. How can I best manage these conditions together?
- Are there brochures or other printed material that I can have? What websites do you recommend?
What you can do in the meantime
Keep track of your daily servings of dairy foods, including milk, ice cream, yogurt and cottage cheese, and when you have them and what you eat with them. Also let your doctor know which dairy foods, in what amounts, give you symptoms. This information can help your doctor make a diagnosis.
If you think you may have lactose intolerance, try cutting dairy products from your diet for a few days to see if your symptoms ease. Let your doctor know if your symptoms got better on the days you didn't have dairy products.
Last Updated Mar 5, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



