Phenylketonuria (PKU)
Overview
Phenylketonuria (fen-ul-key-toe-NU-ree-uh), also called PKU, is a rare inherited disorder that causes an amino acid called phenylalanine to build up in the body. PKU is caused by a change in the phenylalanine hydroxylase (PAH) gene. This gene helps create the enzyme needed to break down phenylalanine.
Without the enzyme necessary to break down phenylalanine, a dangerous buildup can develop when a person with PKU eats foods that contain protein or eats aspartame, an artificial sweetener. This can eventually lead to serious health problems.
For the rest of their lives, people with PKU — babies, children and adults — need to follow a diet that limits phenylalanine, which is found mostly in foods that contain protein. Newer medications may allow some people with PKU to eat a diet that has a higher or an unrestricted amount of phenylalanine.
Babies in the United States and many other countries are screened for PKU soon after birth. Although there is no cure for PKU, recognizing PKU and starting treatment right away can help prevent limitations in areas of thinking, understanding and communicating (intellectual disability) and major health problems.
Symptoms
Newborns with PKU initially don't have any symptoms. However, without treatment, babies usually develop signs of PKU within a few months.
Signs and symptoms of untreated PKU can be mild or severe and may include:
- A musty odor in the breath, skin or urine, caused by too much phenylalanine in the body
- Nervous system (neurological) problems that may include seizures
- Skin rashes, such as eczema
- Lighter skin, hair and eye color than family members, because phenylalanine can't transform into melanin — the pigment responsible for hair and skin tone
- Unusually small head size (microcephaly)
- Hyperactivity
- Intellectual disability
- Delayed development
- Behavioral, emotional and social problems
- Mental health disorders
Severity varies
The severity of PKU depends on the type.
- Classic PKU. The most severe form of the disorder is called classic PKU. The enzyme needed to break down phenylalanine is missing or severely reduced. This results in high levels of phenylalanine that can cause severe brain damage.
- Less severe forms of PKU. In mild or moderate forms, the enzyme still has some function, so phenylalanine levels are not as high, resulting in a smaller risk of significant brain damage.
Regardless of the form, most infants, children and adults with the disorder still require a special PKU diet to prevent intellectual disability and other complications.
Pregnancy and PKU
Women who have PKU and become pregnant are at risk of another form of the condition called maternal PKU. If women don't follow the special PKU diet before and during pregnancy, blood phenylalanine levels can become high and harm the developing baby.
Even women with less severe forms of PKU may place their unborn children at risk by not following the PKU diet.
Babies born to women with high phenylalanine levels don't often inherit PKU. But a child can have serious problems if the level of phenylalanine is high in the mother's blood during pregnancy. At birth, the baby may have:
- Low birth weight
- Unusually small head
- Problems with the heart
In addition, maternal PKU can cause the child to have delayed development, intellectual disability and problems with behavior.
When to see a doctor
Talk to your health care provider in these situations:
- Newborns. If routine newborn screening tests show that your baby may have PKU, your child's health care provider will want to start dietary treatment right away to prevent long-term problems.
- Women of childbearing years. It's especially important for women with a history of PKU to see a health care provider and maintain the PKU diet before becoming pregnant and during pregnancy. This reduces the risk of high blood phenylalanine levels harming their unborn babies.
- Adults. People with PKU need to receive lifelong care. Adults with PKU who have stopped the PKU diet in their teens may benefit from a visit with their health care providers. Returning to the diet may improve mental functioning and behavior and prevent further damage to the central nervous system that can result from high phenylalanine levels.
Causes
A gene change (genetic mutation) causes PKU, which can be mild, moderate or severe. In a person with PKU, a change in the phenylalanine hydroxylase (PAH) gene causes a lack of or reduced amount of the enzyme that's needed to process phenylalanine, an amino acid.
A dangerous buildup of phenylalanine can develop when a person with PKU eats protein-rich foods, such as milk, cheese, nuts or meat, or grains such as bread and pasta, or aspartame, an artificial sweetener.
Inheritance
For a child to inherit PKU, both the mother and father must have and pass on the changed gene. This pattern of inheritance is called autosomal recessive.
It's possible for a parent to be a carrier — to have the changed gene that causes PKU, but not have the disease. If only one parent has the changed gene, there's no risk of passing PKU to a child, but it's possible for the child to be a carrier.
Most often, PKU is passed to children by two parents who are both carriers of the changed gene, but don't know it.
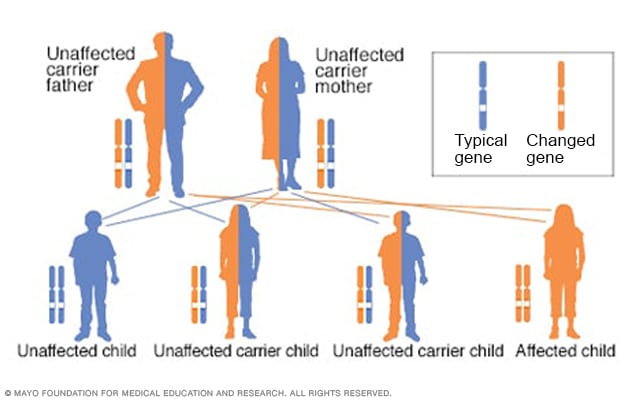
To have an autosomal recessive disorder, you inherit two changed genes, sometimes called mutations. You get one from each parent. Their health is rarely affected because they have only one changed gene. Two carriers have a 25% chance of having an unaffected child with two unaffected genes. They have a 50% chance of having an unaffected child who also is a carrier. They have a 25% chance of having an affected child with two changed genes.
Risk factors
Risk factors for inheriting PKU include:
- Having both parents with a gene change that causes PKU. Two parents must pass along a copy of the changed gene for their child to develop the condition.
- Being of a certain racial or ethnic descent. PKU affects people from most ethnic backgrounds worldwide. But in the United States, it's most common in people of European ancestry and much less common in people of African ancestry.
Complications
Untreated PKU can lead to complications in infants, children and adults with the disorder. When women with PKU have high blood phenylalanine levels during pregnancy, it can harm their unborn baby.
Untreated PKU can lead to:
- Irreversible brain damage and marked intellectual disability beginning within the first few months of life
- Neurological problems such as seizures and tremors
- Behavioral, emotional and social problems in older children and adults
- Major health and developmental problems
Prevention
If you have PKU and are considering getting pregnant:
- Follow a low-phenylalanine diet. Women with PKU can prevent harm to their developing baby by sticking to or returning to a low-phenylalanine diet before becoming pregnant. Nutritional supplements designed for people with PKU can ensure enough protein and nutrition during pregnancy. If you have PKU, talk to your health care provider before you start trying to conceive.
- Consider genetic counseling. If you have PKU, a close relative with PKU or a child with PKU, you may benefit from genetic counseling before becoming pregnant. A specialist in medical genetics (geneticist) can help you better understand how PKU is passed through your family. The specialist can also help determine your risk of having a child with PKU and assist with family planning.
Diagnosis
Newborn screening identifies almost all cases of phenylketonuria. All 50 states in the United States require newborns to be screened for PKU. Many other countries also routinely screen infants for PKU.
If you have PKU or a family history of it, your health care provider may recommend screening tests before pregnancy or birth. It's possible to identify PKU carriers through a blood test.
Testing your baby after birth
A PKU test is done a day or two after your baby's birth. For accurate results, the test is done after your baby is 24 hours old and after your baby has had some protein in the diet.
- A nurse or lab technician collects a few drops of blood from your baby's heel.
- A laboratory tests the blood sample for certain metabolic disorders, including PKU.
- If you don't deliver your baby in a hospital or are discharged soon after the birth, you may need to schedule a newborn screening with your health care provider.
If this test indicates that your baby may have PKU:
- Your baby may have additional tests to confirm the diagnosis, including more blood tests and urine tests
- You and your baby may have genetic testing to identify the gene change for PKU
Treatment
Starting treatment early and continuing treatment throughout life can help prevent intellectual disability and major health problems.
The main treatments for PKU include:
- A lifetime diet with very limited intake of foods with phenylalanine
- Taking a PKU formula — a special nutritional supplement — for life to make sure that you get enough essential protein (without phenylalanine) and nutrients that are essential for growth and general health
- Medications, for certain people with PKU
A safe amount of phenylalanine differs for each person with PKU and can vary over time. In general, the idea is to consume only the amount of phenylalanine that's necessary for healthy growth and body processes, but no more. Your health care provider can determine a safe amount through:
- Regular review of food records and growth charts
- Frequent blood tests that monitor blood phenylalanine levels, especially during childhood growth spurts and pregnancy
- Other tests that assess growth, development and health
Your health care provider may refer you to a registered dietitian who can help you learn about the PKU diet, make adjustments to your diet when needed, and offer suggestions on ways to manage PKU diet challenges.
Which foods and products to avoid
Because the amount of phenylalanine that a person with PKU can safely eat is so low, it's important to avoid all high-protein foods, such as:
- Milk
- Eggs
- Cheese
- Nuts
- Soy products, such as soybeans, tofu, tempeh and milk
- Beans and peas
- Poultry, beef, pork and any other meat
- Fish
Potatoes, grains and other vegetables will likely be limited.
Children and adults also need to avoid certain other foods and beverages, including many diet sodas and other drinks that contain aspartame (NutraSweet, Equal). Aspartame is an artificial sweetener made with phenylalanine.
Some medications may contain aspartame and some vitamins or other supplements may contain amino acids or skim milk powder. Check with your pharmacist about the contents of nonprescription products and prescription medications.
Talk with your health care provider or registered dietitian to learn more about your specific dietary needs.
Formula for people with PKU
Because of the restricted diet, people with PKU need to get essential nutrients through a special nutritional supplement. The phenylalanine-free formula provides essential protein (amino acids) and other nutrients in a form that's safe for people with PKU.
Your health care provider and dietitian can help you find the right type of formula.
- Formula for babies and toddlers. Because regular infant formula and breast milk contain phenylalanine, babies with PKU instead need to have a phenylalanine-free infant formula. A dietitian can carefully calculate the amount of breast milk or regular formula to be added to the phenylalanine-free formula. The dietitian can also teach parents how to choose solid foods while not going over the child's daily phenylalanine allowance.
- Formula for older children and adults. Older children and adults continue to drink or eat a phenylalanine-free nutritional supplement (protein equivalent formula), as directed by a health care provider or dietitian. Your daily dose of formula is divided between your meals and snacks, instead of being eaten or drunk all at once. The formula for older children and adults is not the same as the one used for infants, but it also provides essential protein without phenylalanine. The formula is continued for life.
The need for a nutritional supplement, especially if you or your child doesn't find it appealing, and the limited food choices can make the PKU diet challenging. But making a firm commitment to this lifestyle change is the only way to prevent the serious health problems that people with PKU can develop.
PKU medication
The Food and Drug Administration (FDA) approved the drug sapropterin (Kuvan) for the treatment of PKU. The drug may be used in combination with a PKU diet. Some people with PKU who are taking the medication may not need to follow a PKU diet. But the drug doesn't work for everyone with PKU.
The FDA also approved a novel enzyme therapy, pegvaliase-pqpz (Palynziq), for adults with PKU when current therapy does not adequately reduce the level of phenylalanine. But because of frequent side effects, which can be severe, this treatment is only available as part of a restricted program under the supervision of certified health care providers.
Lifestyle and home remedies
Strategies to help manage PKU include keeping track of foods eaten, measuring correctly, and being creative. Like anything, the more these strategies are practiced, the greater the comfort and confidence you can develop.
Keep track and measure correctly
If you or your child is following a low-phenylalanine diet, you'll need to keep records of the food eaten every day.
To be as accurate as possible, measure food portions using standard measuring cups and spoons and a kitchen scale that reads in grams. The food amounts are compared with a food list or are used to calculate the amount of phenylalanine eaten every day. Each meal and snack includes the appropriately divided portion of your daily PKU formula.
Food diaries, computer programs and smartphone apps are available that list the amount of phenylalanine in baby foods, solid foods, PKU formulas, and common baking and cooking ingredients.
Meal planning or meal rotations of known foods may help reduce some of the daily tracking.
Be creative
Talk with your dietitian to find out how you can be creative with foods to help you stay on track. For example, use seasonings and a variety of cooking methods to transform lower phenylalanine vegetables into a whole menu of different dishes. Herbs and flavorings low in phenylalanine can have lots of flavor. Just remember to measure and count every ingredient and adjust recipes to your specific diet.
If you have any other health conditions, you may also need to consider those when you plan your diet. Talk with your health care provider or dietitian if you have any questions.
Coping and support
Living with PKU can be challenging. These strategies may help:
- Stay informed. Knowing the facts about PKU can help you take charge of the situation. Discuss any questions with your pediatrician, family health care provider, geneticist or dietitian. Read books and cookbooks specifically written for people with PKU.
- Learn from other families. Ask your health care provider about local or online support groups for people living with PKU. Talking with others who have mastered similar challenges can be helpful. The National PKU Alliance is an online support group for families and adults with PKU.
- Get help with menu planning. A registered dietitian with experience in PKU can help you devise delicious low-phenylalanine dinners. Your dietitian may also have great ideas for holiday meals and birthdays.
- Plan ahead when you eat out. A meal at the local restaurant gives you a break from the kitchen and can be fun for the whole family. Most places offer something that fits into the PKU diet. But you may want to call ahead and ask about the menu or bring food from home.
- Find sources of financial aid. Ask your health care provider or dietitian if there are programs or insurance plans that help cover the high costs of formula and low-protein foods. Also, see if your local school lunch program will make adjustments for special dietary needs.
- Don't focus on food. Making mealtime about family time can take some of the focus off food. Try family conversations or games while eating. Encourage children with PKU to focus on sports, music or favorite hobbies, not on just what they can and can't eat. Also consider creating holiday traditions that center on special projects and activities, not just food.
- Let your child help manage the diet as early as possible. Toddlers can make choices about which cereal, fruit or vegetable they'd like to eat and help measure out portions. They can also help themselves to pre-measured snacks. Older children can help with menu planning, pack their own lunches and keep their own food records.
- Make your grocery list and meals with the whole family in mind. A cupboard full of restricted foods can be tempting to a child or adult with PKU, so try to focus on foods that everyone can eat. Serve stir-fried vegetables that are lower in protein. If the other family members wish, they can add peas, corn, meat and rice. Or set up a salad bar with low-protein and moderate-protein options. You can also serve the whole family a delicious low-phenylalanine soup or curry.
- Be prepared for potlucks, picnics and car trips. Plan ahead, so there's always a PKU-friendly food option. Pack snacks of fresh fruits or lower protein crackers. Take fruit kebabs or vegetable skewers to a cookout, and make a low-phenylalanine salad for the neighborhood potluck. Other parents, friends and family members will likely make adjustments and be helpful if you explain the dietary restrictions.
- Talk to teachers and other staff in your child's school. Your child's teachers and cafeteria staff can be a big help with the PKU diet if you take the time to explain its importance and how it works. By working with your child's teachers, you can also plan ahead for special school events and parties so that your child always has a treat to eat.
Preparing for an appointment
Phenylketonuria is generally diagnosed through newborn screening. Once your child is diagnosed with PKU, you'll likely be referred to a medical center or specialty clinic with a specialist who treats PKU and a dietitian with expertise in the PKU diet.
Here's some information to help you get ready for your appointment and know what to expect.
What you can do
Before your appointment:
- Ask a family member or friend to go to the appointment with you — sometimes it can be difficult to remember all of the information provided during an appointment.
- Make a list of questions to ask your health care provider and dietitian to help you make the most of your time together.
Some questions to ask may include:
- How did my child get PKU?
- How can we manage PKU?
- Are there any medications to treat this disorder?
- What foods are completely off-limits?
- What is the recommended diet?
- Will my child have to stay on this special diet for life?
- What kind of formula will my child need? Can my child have breast milk?
- Are there any other supplements needed?
- What happens if my child eats a food that he or she is not supposed to eat?
- If I have another child, will that child have PKU?
- Are there brochures or other printed material that I can have? What websites do you recommend?
What to expect from your doctor
Your health care provider is likely to ask you several questions. For example:
- Has your child had any symptoms that concern you?
- Do you have any questions about your child's diet?
- Are you having any difficulty following the diet?
- Has the growth and development of your child been typical of other children the same age?
- Have you ever had genetic testing?
- Do any other relatives have PKU?
Your health care provider will ask additional questions based on your responses, symptoms and needs. Preparing and anticipating questions will help you make the most of your appointment time.
Last Updated May 13, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




