Polycystic kidney disease
Overview
Polycystic kidney disease (PKD) is an inherited disorder in which clusters of cysts develop primarily within your kidneys, causing your kidneys to enlarge and lose function over time. Cysts are noncancerous round sacs containing fluid. The cysts vary in size, and they can grow very large. Having many cysts or large cysts can damage your kidneys.
Polycystic kidney disease can also cause cysts to develop in your liver and elsewhere in your body. The disease can cause serious complications, including high blood pressure and kidney failure.
PKD varies greatly in its severity, and some complications are preventable. Lifestyle changes and treatments might help reduce damage to your kidneys from complications.
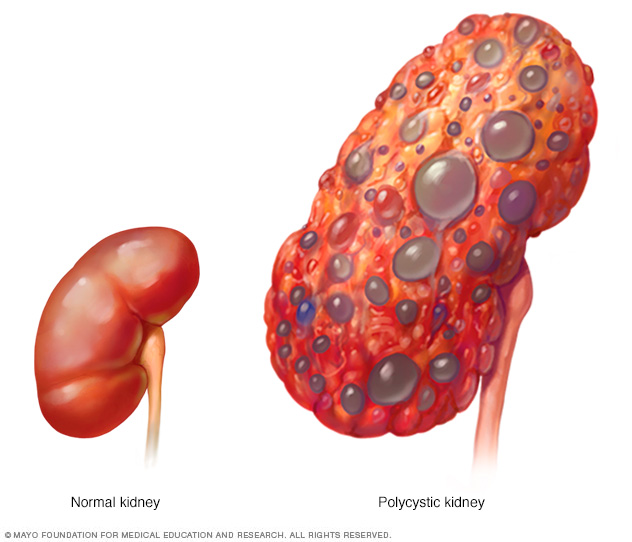
A healthy kidney (left) eliminates waste from the blood and maintains the body's chemical balance. With polycystic kidney disease (right), fluid-filled sacs called cysts develop in the kidneys. The kidneys grow larger and gradually lose the ability to function as they should.
Symptoms
Polycystic kidney disease symptoms can include:
- High blood pressure
- Back or side pain
- Blood in your urine
- A feeling of fullness in your abdomen
- Increased size of your abdomen due to enlarged kidneys
- Headaches
- Kidney stones
- Kidney failure
- Urinary tract or kidney infections
When to see a doctor
It's not uncommon for people to have polycystic kidney disease for years without knowing it.
If you develop some of the signs and symptoms of polycystic kidney disease, see your doctor. If you have a first-degree relative — parent, sibling or child — with polycystic kidney disease, see your doctor to discuss screening for this disorder.
Causes
Abnormal genes cause polycystic kidney disease, which means that in most cases, the disease runs in families. Sometimes, a genetic mutation occurs on its own (spontaneous), so that neither parent has a copy of the mutated gene.
The two main types of polycystic kidney disease, caused by different genetic flaws, are:
-
Autosomal dominant polycystic kidney disease (ADPKD). Signs and symptoms of ADPKD often develop between the ages of 30 and 40. In the past, this type was called adult polycystic kidney disease, but children can develop the disorder.
Only one parent needs to have the disease for it to pass to the children. If one parent has ADPKD, each child has a 50% chance of getting the disease. This form accounts for most of the cases of polycystic kidney disease.
-
Autosomal recessive polycystic kidney disease (ARPKD). This type is far less common than is ADPKD. The signs and symptoms often appear shortly after birth. Sometimes, symptoms don't appear until later in childhood or during adolescence.
Both parents must have abnormal genes to pass on this form of the disease. If both parents carry a gene for this disorder, each child has a 25% chance of getting the disease.
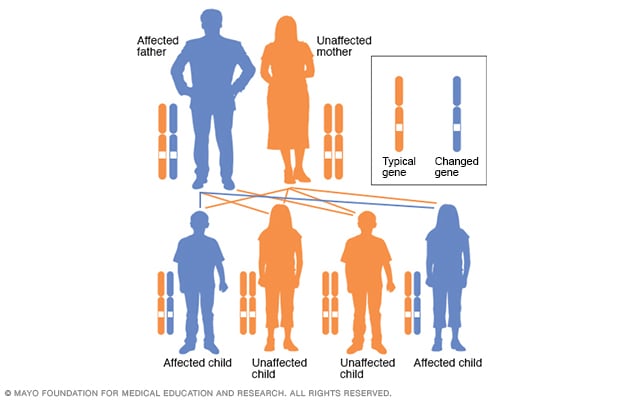
In an autosomal dominant disorder, the changed gene is a dominant gene. It's located on one of the nonsex chromosomes, called autosomes. Only one changed gene is needed to be affected by this type of condition. A person with an autosomal dominant condition — in this example, the father — has a 50 percent chance of having an affected child with one changed gene. The person has a 50 percent chance of having an unaffected child.
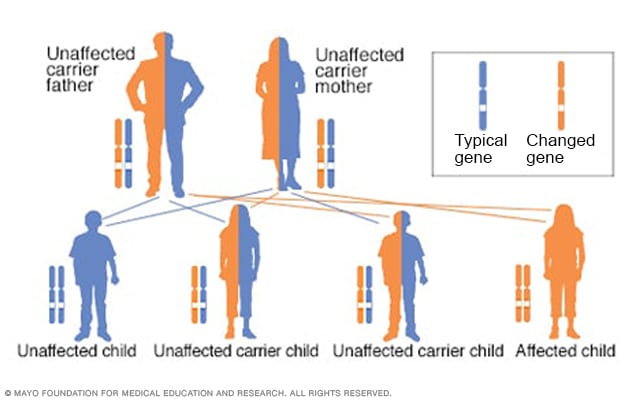
To have an autosomal recessive disorder, you inherit two changed genes, sometimes called mutations. You get one from each parent. Their health is rarely affected because they have only one changed gene. Two carriers have a 25% chance of having an unaffected child with two unaffected genes. They have a 50% chance of having an unaffected child who also is a carrier. They have a 25% chance of having an affected child with two changed genes.
Complications
Complications associated with polycystic kidney disease include:
- High blood pressure. Elevated blood pressure is a common complication of polycystic kidney disease. Untreated, high blood pressure can cause further damage to your kidneys and increase your risk of heart disease and strokes.
-
Loss of kidney function. Progressive loss of kidney function is one of the most serious complications of polycystic kidney disease. Nearly half of those with the disease have kidney failure by age 60.
PKD can interfere with the ability of your kidneys to keep wastes from building to toxic levels, a condition called uremia. As the disease worsens, end-stage kidney (renal) disease may result, necessitating ongoing kidney dialysis or a transplant to prolong your life.
- Chronic pain. Pain is a common symptom for people with polycystic kidney disease. It often occurs in your side or back. The pain can also be associated with a urinary tract infection, a kidney stone or a malignancy.
- Growth of cysts in the liver. The likelihood of developing liver cysts for someone with polycystic kidney disease increases with age. While both men and women develop cysts, women often develop larger cysts. Female hormones and multiple pregnancies might contribute to liver cyst development.
- Development of an aneurysm in the brain. A balloon-like bulge in a blood vessel (aneurysm) in your brain can cause bleeding (hemorrhage) if it ruptures. People with polycystic kidney disease have a higher risk of aneurysms. People with a family history of aneurysms seem to be at highest risk. Ask your doctor if screening is needed in your case. If screening reveals that you don't have an aneurysm, your doctor may recommend repeating the screening exam in a few years or after several years as a follow-up. The timing of repeat screening depends on your risk.
- Pregnancy complications. Pregnancy is successful for most women with polycystic kidney disease. In some cases, however, women may develop a life-threatening disorder called preeclampsia. Those most at risk have high blood pressure or a decline in kidney function before they become pregnant.
- Heart valve abnormalities. As many as 1 in 4 adults with polycystic kidney disease develops mitral valve prolapse. When this happens, the heart valve no longer closes properly, which allows blood to leak backward.
- Colon problems. Weaknesses and pouches or sacs in the wall of the colon (diverticulosis) may develop in people with polycystic kidney disease.
Prevention
If you have polycystic kidney disease and you're considering having children, a genetic counselor can help you assess your risk of passing the disease to your offspring.
Keeping your kidneys as healthy as possible may help prevent some of the complications of this disease. One of the most important ways you can protect your kidneys is by managing your blood pressure.
Here are some tips for keeping your blood pressure in check:
- Take the blood pressure medications prescribed by your doctor as directed.
- Eat a low-salt diet containing plenty of fruits, vegetables and whole grains.
- Maintain a healthy weight. Ask your doctor what the right weight is for you.
- If you smoke, quit.
- Exercise regularly. Aim for at least 30 minutes of moderate physical activity most days of the week.
- Limit alcohol use.
Diagnosis
For polycystic kidney disease, certain tests can detect the size and number of kidney cysts you have and evaluate the amount of healthy kidney tissue, including:
- Ultrasound. During an ultrasound, a wandlike device called a transducer is placed on your body. It emits sound waves that are reflected back to the transducer — like sonar. A computer translates the reflected sound waves into images of your kidneys.
- CT scan. As you lie on a movable table, you're guided into a big, doughnut-shaped device that projects thin X-ray beams through your body. Your doctor is able to see cross-sectional images of your kidneys.
- MRI scan. As you lie inside a large cylinder, magnetic fields and radio waves generate cross-sectional views of your kidneys.
Treatment
The severity of polycystic kidney disease varies from person to person — even among members of the same family. Often, people with PKD reach end-stage kidney disease between ages 55 to 65. But some people with PKD have a mild disease and might never progress to end-stage kidney disease.
Treating polycystic kidney disease involves dealing with the following signs, symptoms and complications in their early stages:
-
Kidney cyst growth. Tolvaptan therapy may be recommended for adults at risk of rapidly progressive ADPKD. Tolvaptan (Jynarque, Samsca) is a pill that you take by mouth that works to slow the rate of kidney cyst growth and the decline in how well your kidneys work.
There's a risk of serious liver injury when taking tolvaptan, and it can interact with other medicines you take. It's best to see a doctor who specializes in kidney health (nephrologist) when taking tolvaptan, so that you can be monitored for side effects and possible complications.
-
High blood pressure. Controlling high blood pressure can delay the progression of the disease and slow further kidney damage. Combining a low-sodium, low-fat diet that's moderate in protein and calorie content with not smoking, increasing exercise and reducing stress may help control high blood pressure.
However, medications are usually needed to control high blood pressure. Medications called angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers (ARBs) are often used to control high blood pressure.
- Declining kidney function. To help your kidneys stay as healthy as possible for as long as possible, experts recommend maintaining a normal body weight (body mass index). Drinking water and fluids throughout the day may help slow the growth of kidney cysts, which in turn could slow down a decline in kidney function. Following a low-salt diet and eating less protein might allow kidney cysts to respond better to the increase in fluids.
- Pain. You might be able to control the pain of polycystic kidney disease with over-the-counter medications containing acetaminophen. For some people, however, the pain is more severe and constant. Your doctor might recommend a procedure using a needle to draw out cyst fluid and inject a medication (sclerosing agent) to shrink kidney cysts. Or you may need surgery to remove cysts if they're large enough to cause pressure and pain.
- Bladder or kidney infections. Prompt treatment of infections with antibiotics is necessary to prevent kidney damage. Your doctor may investigate whether you have a simple bladder infection or a more complicated cyst or kidney infection. For more complicated infections, you may need to take a longer course of antibiotics.
- Blood in the urine. You'll need to drink lots of fluids, preferably plain water, as soon as you notice blood in your urine to dilute the urine. Dilution might help prevent obstructive clots from forming in your urinary tract. In most cases, the bleeding will stop on its own. If it doesn't, it's important to contact your doctor.
- Kidney failure. If your kidneys lose their ability to remove waste products and extra fluids from your blood, you'll eventually need either dialysis or a kidney transplant. Seeing your doctor regularly for monitoring of PKD allows for the best timing of a kidney transplant. You may be able to have a preemptive kidney transplant, which means you wouldn't need to start dialysis but would have the transplant instead.
-
Aneurysms. If you have polycystic kidney disease and a family history of ruptured brain (intracranial) aneurysms, your doctor may recommend regular screening for intracranial aneurysms.
If an aneurysm is discovered, surgical clipping of the aneurysm to reduce the risk of bleeding may be an option, depending on its size. Nonsurgical treatment of small aneurysms may involve controlling high blood pressure and high blood cholesterol, as well as quitting smoking.
Early treatment offers the best chance of slowing polycystic kidney disease progression.
Coping and support
As with other chronic illnesses, having polycystic kidney disease might feel overwhelming. The support of friends and family is important in dealing with a chronic illness. In addition, a counselor, psychologist, psychiatrist or clergy member may be able to help.
You might also consider joining a support group. Although not for everyone, support groups can provide helpful information about treatments and coping. And being with people who understand what you're going through might make you feel less alone.
Ask your doctor about support groups in your community.
Preparing for an appointment
You're likely to start by seeing your primary care provider. However, you might be referred to a doctor who specializes in kidney health (nephrologist). You may benefit from starting a specialized treatment early on in the course of the disease, even if blood tests show that you still have normal kidney function.
Here's some information to help you get ready for your appointment.
What you can do
When you make the appointment, ask if there's anything you need to do in advance, such as fasting before having a specific test. Make a list of:
- Your symptoms, including any that seem unrelated to the reason for which you scheduled the appointment, and when they began
- All medications, vitamins and other supplements you take, including dosages
- Your and your family's medical history, particularly kidney diseases
- Questions to ask your doctor
Take a family member or friend along, if possible, to help you remember the information you receive.
For polycystic kidney disease, questions to ask your doctor include:
- What's the most likely cause of my symptoms?
- Are there other possible causes for my symptoms?
- What tests do I need?
- Is this condition temporary or chronic?
- What's the best course of action?
- What alternatives are there to the approach you're suggesting?
- I have other health conditions. How can I best manage them together?
- Do I need to restrict my diet or activities?
- Are there brochures or other printed material that I can take? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your doctor is likely to ask you questions, such as:
- Have your symptoms been continuous or occasional?
- Does anything seem to improve or worsen your symptoms?
- Do you know what your blood pressure normally is?
- Has your kidney function been measured?
Last Updated Jan 25, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




