Stomach cancer
Overview
Stomach cancer, which is also called gastric cancer, is a growth of cells that starts in the stomach. The stomach is in the upper middle part of the belly, just below the ribs. The stomach helps to break down and digest food.
Stomach cancer can happen in any part of the stomach. In most of the world, stomach cancers happen in the main part of the stomach. This part is called the stomach body.
In the United States, stomach cancer is more likely to start by the gastroesophageal junction. This is the part where the long tube that carries food you swallow meets the stomach. The tube that carries food to the stomach is called the esophagus.
Where the cancer starts in the stomach is one factor health care providers think about when making a treatment plan. Other factors might include the cancer's stage and the type of cells involved. Treatment often includes surgery to remove the stomach cancer. Other treatments may be used before and after surgery.
Stomach cancer treatment is most likely to be successful if the cancer is only in the stomach. The prognosis for people with small stomach cancers is quite good. Many can expect to be cured. Most stomach cancers are found when the disease is advanced and a cure is less likely. Stomach cancer that grows through the stomach wall or spreads to other parts of the body is harder to cure.
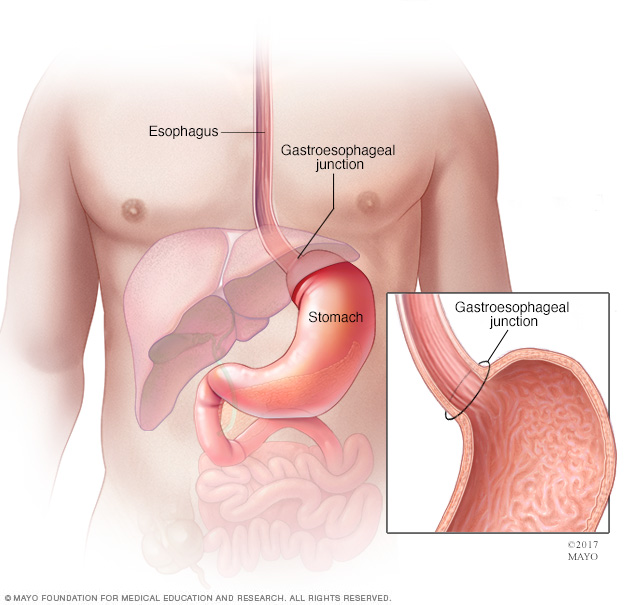
The stomach is a muscular sac in the middle of the upper abdomen that helps break down and digest food. Food you eat passes down your esophagus, through the gastroesophageal junction and into the stomach.
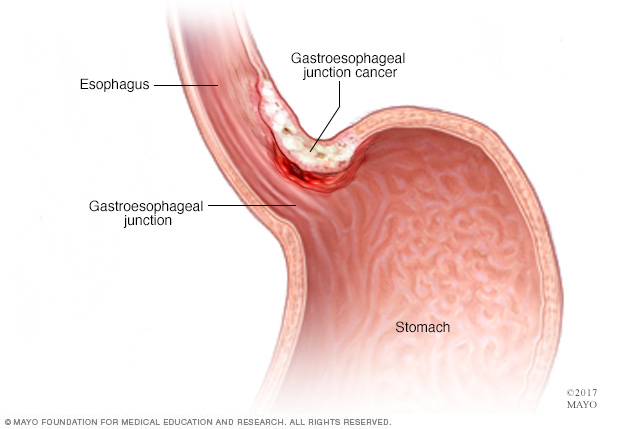
Cancer of the gastroesophageal junction develops in the area where the esophagus joins the top part of the stomach.
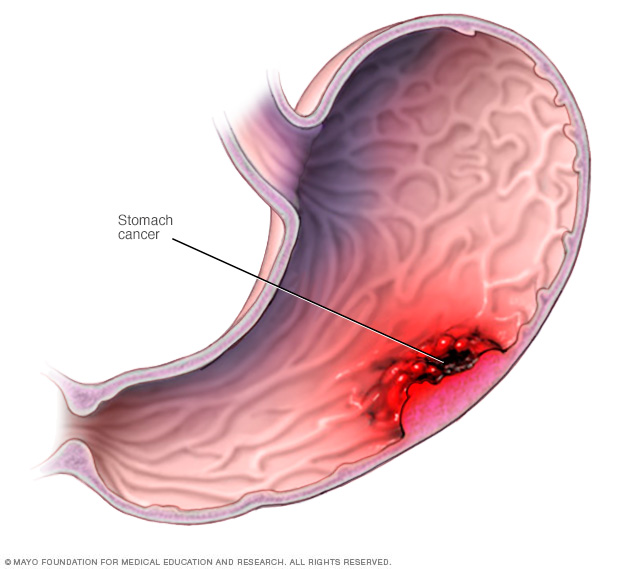
Stomach cancer most commonly begins in the cells that line the inside of the stomach.
Symptoms
Signs and symptoms of stomach cancer may include:
- Trouble swallowing
- Belly pain
- Feeling bloated after eating
- Feeling full after eating small amounts of food
- Not feeling hungry when you would expect to be hungry
- Heartburn
- Indigestion
- Nausea
- Vomiting
- Losing weight without trying
- Feeling very tired
- Stools that look black
Stomach cancer doesn't always cause symptoms in its early stages. When they happen, symptoms might include indigestion and pain in the upper part of the belly. Symptoms might not happen until the cancer is advanced. Later stages of stomach cancer might cause symptoms such as feeling very tired, losing weight without trying, vomiting blood and having black stools.
Stomach cancer that spreads to other parts of the body is called metastatic stomach cancer. It causes symptoms specific to where it spreads. For example, when cancer spreads to the lymph nodes it might cause lumps you can feel through the skin. Cancer that spreads to the liver might cause yellowing of the skin and whites of the eyes. If cancer spreads within the belly, it might cause fluid to fill the belly. The belly might look swollen.
When to see a doctor
If you have signs and symptoms that worry you, make an appointment with your health care provider. Many conditions can cause symptoms that are like the ones caused by stomach cancer. Your provider might test for those other causes first before testing for stomach cancer.
Causes
It's not clear what causes stomach cancer. Experts believe most stomach cancers start when something hurts the inside lining of the stomach. Examples include having an infection in the stomach, having long-standing acid reflux and eating a lot of salty foods. Not everyone with these risk factors gets stomach cancer, though. So more research is needed to find out exactly what causes it.
Stomach cancer begins when something hurts cells in the inner lining of the stomach. It causes the cells to develop changes in their DNA. A cell's DNA holds the instructions that tell a cell what to do. The changes tell the cells to multiply quickly. The cells can go on living when healthy cells would die as part of their natural lifecycle. This causes a lot of extra cells in the stomach. The cells can form a mass called a tumor.
Cancer cells in the stomach can invade and destroy healthy body tissue. They might start to grow deeper into the wall of the stomach. In time, cancer cells can break away and spread to other parts of the body. When cancer cells spread to another part of the body it's called metastasis.
Types of stomach cancer
The type of stomach cancer you have is based on the type of cell where your cancer began. Examples of stomach cancer types include:
- Adenocarcinoma. Adenocarcinoma stomach cancer starts in cells that produce mucus. This is the most common type of stomach cancer. Nearly all cancers that start in the stomach are adenocarcinoma stomach cancers.
- Gastrointestinal stromal tumors (GIST). GIST starts in special nerve cells that are found in the wall of the stomach and other digestive organs. GIST is a type of soft tissue sarcoma.
- Carcinoid tumors. Carcinoid tumors are cancers that start in the neuroendocrine cells. Neuroendocrine cells are found in many places in the body. They do some nerve cell functions and some of the work of cells that make hormones. Carcinoid tumors are a type of neuroendocrine tumor.
- Lymphoma. Lymphoma is a cancer that starts in immune system cells. The body's immune system fights germs. Lymphoma can sometimes start in the stomach if the body sends immune system cells to the stomach. This might happen if the body is trying to fight off an infection. Most lymphomas that start in the stomach are a type of non-Hodgkin's lymphoma.
Risk factors
Factors that increase the risk of stomach cancer include:
- Ongoing problems with stomach acid backing up into the esophagus, which is called gastroesophageal reflux disease
- A diet high in salty and smoked foods
- A diet low in fruits and vegetables
- Infection in the stomach caused by a germ called Helicobacter pylori
- Swelling and irritation of the inside of the stomach, which is called gastritis
- Smoking
- Growths of noncancerous cells in the stomach, called polyps
- Family history of stomach cancer
- Family history of genetic syndromes that increase the risk of stomach cancer and other cancers, such as hereditary diffuse gastric cancer, Lynch syndrome, juvenile polyposis syndrome, Peutz-Jeghers syndrome and familial adenomatous polyposis
Prevention
To lower the risk of stomach cancer, you can:
- Eat plenty of fruits and vegetables. Try to include fruits and vegetables in your diet each day. Choose a variety of colorful fruits and vegetables.
- Reduce the amount of salty and smoked foods you eat. Protect your stomach by limiting these foods.
- Stop smoking. If you smoke, quit. If you don't smoke, don't start. Smoking increases your risk of stomach cancer and many other types of cancer. Quitting smoking can be very hard, so ask your health care provider for help.
- Tell your health care provider if stomach cancer runs in your family. People with a strong family history of stomach cancer might have stomach cancer screening. Screening tests can detect stomach cancer before it causes symptoms.
Diagnosis
Tests and procedures used to diagnose and detect stomach cancer include:
- Looking inside the stomach. To look for signs of cancer, your health care provider might use a tiny camera to see inside your stomach. This procedure is called upper endoscopy. A thin tube with a tiny camera on the end is passed down the throat and into the stomach.
- Taking a sample of tissue for testing. If something that looks like cancer is found in your stomach, it might be removed for testing. This is called a biopsy. It can be done during an upper endoscopy. Special tools are passed down the tube to get the tissue sample. The sample is sent to a lab for testing.
Determining the stage of stomach cancer
Once you're found to have stomach cancer, you might have other tests to see if the cancer has spread. This information is used to give the cancer a stage. The stage tells your provider how advanced your cancer is and about your prognosis. Tests and procedures used to find the stage of stomach cancer include:
-
Blood tests. A blood test can't diagnose stomach cancer. Blood tests can give your provider clues about your health. For example, tests to measure your liver health might show problems caused by stomach cancer that spreads to the liver.
Another type of blood test looks for pieces of cancer cells in the blood. This is called a circulating tumor DNA test. It's only used in certain situations for people with stomach cancer. For example, this test might be used if you have advanced cancer and can't have a biopsy. Collecting pieces of cells from the blood can give your health care team information to help plan your treatment.
-
Stomach ultrasound. Ultrasound is an imaging test that uses sound waves to make pictures. For stomach cancer, the pictures can show how far the cancer has grown into the stomach wall. To get the pictures, a thin tube with a camera on the tip goes down the throat and into the stomach. A special ultrasound tool is used to make pictures of the stomach.
Ultrasound might be used to look at lymph nodes near the stomach. The images can help guide a needle to collect tissue from the lymph nodes. The tissue is tested in a lab to look for cancer cells.
- Imaging tests. Imaging tests make pictures to help your care team look for signs that stomach cancer has spread. The pictures could show cancer cells in nearby lymph nodes or other parts of the body. Tests may include CT and positron emission tomography (PET).
- Surgery. Sometimes imaging tests don't give a clear picture of your cancer, so surgery is needed to see inside the body. Surgery can look for cancer that has spread, which is also called metastasized cancer. Surgery might help your health care team make sure there are no small bits of cancer on the liver or in the belly.
Other tests may be used in certain situations.
Your health care team uses the information from these tests to give your cancer a stage. The stages of stomach cancer are numbers from 0 to 4.
At stage 0, the cancer is small and only on the inside surface of the stomach. A stage 1 stomach cancer has grown into the inner layers of the stomach. In stage 2 and stage 3, the cancer grows deeper into the wall of the stomach. The cancer may have spread to nearby lymph nodes. At stage 4, the stomach cancer may have grown through the stomach and into nearby organs. Stage 4 includes cancers that have spread to other parts of the body. When cancer spreads, it's called metastatic cancer. When stomach cancer metastasizes, it often goes to the lymph nodes or the liver. It can also go to the lining around the organs in the belly, which is called the peritoneum.
Your health care team might give your cancer a new stage after your first treatment. There are separate staging systems for stomach cancer that can be used after surgery or after chemotherapy.
Understanding your prognosis
Your health care team uses your cancer's stage to understand your prognosis. The prognosis is how likely it is that the cancer will be cured. For stomach cancer, the prognosis for early-stage cancer is very good. As the stage gets higher, the chances of a cure get lower. Even when stomach cancer can't be cured, treatments may control the cancer to prolong your life and make you comfortable.
Things that can influence the prognosis for stomach cancer include:
- The type of cancer
- The cancer's stage
- Where the cancer is within the stomach
- Your overall health
- If the cancer is removed completely with surgery
- If the cancer responds to treatment with chemotherapy or radiation therapy
If you're concerned about your prognosis, talk about it with your provider. Ask about the seriousness of your cancer.
Detecting stomach cancer before it causes symptoms
Sometimes tests are used to look for stomach cancer in people who don't have symptoms. This is called stomach cancer screening. The goal of screening is to detect stomach cancer when it's small and more likely to be cured.
In the United States, stomach cancer screening tests are only for people with a high risk of stomach cancer. Your risk could be high if stomach cancer runs in your family. You could have a high risk if you have a genetic syndrome that can cause stomach cancer. Examples include hereditary diffuse gastric cancer, Lynch syndrome, juvenile polyposis syndrome, Peutz-Jeghers syndrome and familial adenomatous polyposis.
In other parts of the world where stomach cancer is much more common, tests to detect stomach cancer are used more widely.
Upper endoscopy is the most common test used to detect stomach cancer. Some countries use X-rays to detect stomach cancer.
Stomach cancer screening is an active area of cancer research. Scientists are studying blood tests and other ways to detect stomach cancer before it causes symptoms.
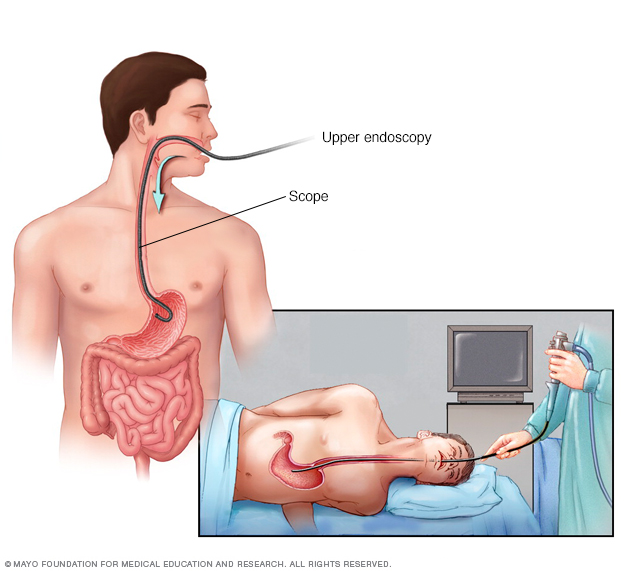
During an upper endoscopy, a healthcare professional inserts a thin, flexible tube equipped with a light and camera down the throat and into the esophagus. The tiny camera provides a view of the esophagus, stomach and the beginning of the small intestine, called the duodenum.
Treatment
Treatment options for stomach cancer depend on the cancer's location within the stomach and its stage. Your health care provider also thinks about your overall health and your preferences when making a treatment plan. Stomach cancer treatments include surgery, chemotherapy, radiation therapy, targeted therapy, immunotherapy and palliative care.
Surgery
The goal of surgery for stomach cancer, which is also called gastric cancer, is to remove all of the cancer. For small stomach cancers, surgery might be the first treatment. Other treatments might be used first if the stomach cancer grows deeper into the stomach wall or spreads to the lymph nodes.
Operations used to treat stomach cancer include:
- Removing small cancers from the stomach lining. Very small cancers can be cut away from the inside lining of the stomach. To remove the cancer, a tube is passed down the throat and into the stomach. Special cutting tools are passed through the tube to cut out the cancer. This procedure is called an endoscopic mucosal resection. It might be an option for treating stage 1 cancer that's growing on the inner lining of the stomach.
- Removing part of the stomach. This procedure is called a subtotal gastrectomy. The surgeon removes the part of the stomach affected by cancer and some of the healthy tissue around it. It might be an option if your stomach cancer is located in the part of the stomach nearest the small intestine.
- Removing the entire stomach. This procedure is called a total gastrectomy. It involves removing all of the stomach and some surrounding tissue. The surgeon connects the esophagus to the small intestine to allow food to move through the digestive system. Total gastrectomy is a treatment for cancers in the part of the stomach that is closest to the esophagus.
- Removing lymph nodes to look for cancer. The surgeon may remove lymph nodes in your belly to test them for cancer.
- Surgery to relieve symptoms. An operation to remove part of the stomach may relieve symptoms of a growing cancer. This might be an option if the cancer is advanced and other treatments haven't helped.
Small stage 1 stomach cancers often can be cut away from the inner lining of the stomach. But if the cancer grows into the muscle layer of the stomach wall, this might not be an option. Some stage 1 cancers may need surgery to remove all of or some of the stomach.
For stage 2 and stage 3 stomach cancers, surgery might not be the first treatment. Chemotherapy and radiation therapy might be used first to shrink the cancer. This might make it easier to remove the cancer completely. Surgery often involves removing some or all of the stomach and also some lymph nodes.
If stage 4 stomach cancer grows through the stomach and into nearby organs, surgery might be an option. To remove all of the cancer, parts of the nearby organs might be removed, too. Other treatments might be used first to shrink the cancer. If a stage 4 cancer can't be removed completely, surgery might help control symptoms.
Chemotherapy
Chemotherapy is a drug treatment that uses chemicals to kill cancer cells. Types of chemotherapy include:
- Chemotherapy that travels through your whole body. The most common type of chemotherapy involves medicines that travel through your whole body, killing cancer cells. This is called systemic chemotherapy. The medicines can be given through a vein or taken in pill form.
- Chemotherapy that only goes in the belly. This type of chemotherapy is called hyperthermic intraperitoneal chemotherapy (HIPEC). HIPEC is done right after surgery. After the surgeon removes the stomach cancer, the chemotherapy medicines are put directly into the belly. The medicines are heated to make them more effective. The chemotherapy is left in place for a set amount of time and then drained.
Chemotherapy might not be needed for stage 1 stomach cancer. It might not be needed if surgery removed all of the cancer and there's a low risk of cancer coming back.
Chemotherapy is often used before surgery to treat stage 2 and stage 3 stomach cancers. Systemic chemotherapy might help shrink the cancer so that it's easier to remove. Giving chemotherapy before surgery is called neoadjuvant chemotherapy.
Systemic chemotherapy might be used after surgery if there's a risk that some cancer cells were left behind. This risk might be higher if the cancer grows deep into the stomach wall or spreads to the lymph nodes. Giving chemotherapy after surgery is called adjuvant chemotherapy.
Chemotherapy can be used alone or it can be combined with radiation therapy.
If surgery isn't an option, systemic chemotherapy might be recommended instead. It might be used if the cancer is too advanced or if you're not healthy enough to have surgery. Chemotherapy might help control cancer symptoms.
HIPEC is an experimental treatment that might be an option for stage 4 stomach cancer. It might be used if the cancer can't be removed completely because it extends through the stomach and into nearby organs. The surgeon might remove as much of the cancer as possible. Then HIPEC helps to kill any cancer cells that are left.
Radiation therapy
Radiation therapy uses high-powered beams of energy to kill cancer cells. The beams can come from X-rays, protons or other sources. During radiation therapy, you lie on a table while a machine gives the radiation treatment to precise points on your body.
Radiation therapy is often done at the same time as chemotherapy. Sometimes doctors call this chemoradiation.
Radiation therapy might not be needed for stage 1 stomach cancer. It might not be needed if surgery removed all of the cancer and there's a low risk that the cancer will come back.
Radiation is sometimes used before surgery to treat stage 2 and stage 3 stomach cancers. It can shrink the cancer so that it's easier to remove. Giving radiation before surgery is called neoadjuvant radiation.
Radiation therapy might be used after surgery if the cancer can't be removed completely. Giving radiation after surgery is called adjuvant radiation.
Radiation can help relieve stomach cancer symptoms if the cancer is advanced or surgery isn't possible.
Targeted therapy
Targeted treatments use medicines that attack specific chemicals present within cancer cells. By blocking these chemicals, targeted treatments can cause cancer cells to die.
Your cancer cells are tested to see if targeted therapy is likely to work for you.
For stomach cancer, targeted therapy is often used with systemic chemotherapy. Targeted therapy is typically used for advanced stomach cancer. This might include stage 4 stomach cancer and cancer that comes back after treatment.
Immunotherapy
Immunotherapy is a treatment with medicine that helps your body's immune system to kill cancer cells. Your immune system fights off diseases by attacking germs and other cells that shouldn't be in your body. Cancer cells survive by hiding from the immune system. Immunotherapy helps the immune system cells find and kill the cancer cells.
Immunotherapy is sometimes used to treat advanced cancer. This might include stage 4 stomach cancer or cancer that comes back after treatment.
Palliative care
Palliative care is a special type of health care that helps you feel better when you have a serious illness. If you have cancer, palliative care can help relieve pain and other symptoms. Palliative care is done by a team of health care providers. This can include doctors, nurses and other specially trained professionals. Their goal is to improve the quality of life for you and your family.
Palliative care specialists work with you, your family and your care team to help you feel better. They provide an extra layer of support while you have cancer treatment. You can have palliative care at the same time as strong cancer treatments, such as surgery, chemotherapy or radiation therapy.
When palliative care is used along with all of the other appropriate treatments, people with cancer may feel better and live longer.
Coping and support
A cancer diagnosis can be overwhelming and frightening. It may take time to adjust to the initial shock of your diagnosis. In time you'll find ways to cope. Until then, it might help to:
- Learn enough to make decisions about your care. Ask your health care provider to write down the details of your cancer. This can include the type, the stage and your treatment options. Use those details to find more information about stomach cancer. Learn about the benefits and risks of each treatment option.
- Connect with other cancer survivors. Ask your provider about support groups in your area. Or go online and connect with cancer survivors on message boards, such as those run by the American Cancer Society.
- Stay active. Being diagnosed with cancer doesn't mean you have to stop doing the things you enjoy or normally do. For the most part, if you feel well enough to do something, go ahead and do it.
Preparing for an appointment
Start by seeing your usual health care provider if you have any symptoms that worry you. If your provider thinks that you may have a stomach problem, you may be referred to a specialist. This might be a doctor who diagnoses and treats problems in the digestive system. This doctor is called a gastroenterologist.
Once stomach cancer is diagnosed, you may be referred to other specialists. This might be a cancer doctor, which is also called an oncologist, or a surgeon who specializes in operating on the digestive tract.
It's a good idea to be prepared for your appointment. Here's some information to help you get ready, and what to expect from your doctor.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down any symptoms you're experiencing, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Write down key personal information, including any major stresses or recent life changes.
- Make a list of all medications, vitamins or supplements that you're taking.
- Note what seems to improve or worsen your signs and symptoms. Keep track of which foods, medications or other factors influence your signs and symptoms.
- Consider taking a family member or friend along. Sometimes it can be hard to absorb all the information provided during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your doctor.
Your time with your health care provider is limited, so prepare a list of questions. List your questions from most important to least important in case time runs out. For stomach cancer, some basic questions to ask include:
- What type of stomach cancer do I have?
- How advanced is my stomach cancer?
- What other kinds of tests do I need?
- What are my treatment options?
- How successful are the treatments?
- What are the benefits and risks of each option?
- Is there one option you feel is best for me?
- How will treatment affect my life? Can I continue to work?
- Should I seek a second opinion? What will that cost, and will my insurance cover it?
- Are there brochures or other printed material that I can take with me? What websites do you recommend?
In addition to the questions that you've prepared, don't hesitate to ask other questions you think of during your appointment.
What to expect from your doctor
Your provider is likely to ask you questions. Being ready to answer them may allow more time later to cover other points you want to address. Your provider may ask:
- When did you first begin experiencing symptoms?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Last Updated Jun 19, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




