Bradycardia
Overview
Bradycardia (brad-e-KAHR-dee-uh) is a slow heart rate. The hearts of adults at rest usually beat between 60 and 100 times a minute. If you have bradycardia, your heart beats fewer than 60 times a minute.
Bradycardia can be a serious problem if the heart rate is very slow and the heart can't pump enough oxygen-rich blood to the body. If this happens, you may feel dizzy, very tired or weak, and short of breath. Sometimes bradycardia doesn't cause symptoms or complications.
A slow heart rate isn't always a concern. For example, a resting heart rate between 40 and 60 beats a minute is quite common during sleep and in some people, particularly healthy young adults and trained athletes.
If bradycardia is severe, an implanted pacemaker may be needed to help the heart maintain an appropriate rate.
Symptoms
A slower than typical heartbeat (bradycardia) can prevent the brain and other organs from getting enough oxygen, possibly causing these signs and symptoms:
- Chest pain
- Confusion or memory problems
- Dizziness or lightheadedness
- Easily tiring during physical activity
- Fatigue
- Fainting (syncope) or near-fainting
- Shortness of breath
When to see a doctor
Many things can cause signs and symptoms of bradycardia. It's important to get a prompt, accurate diagnosis and appropriate care. See your health care provider if you are concerned about a slow heart rate.
If you faint, have difficulty breathing or have chest pain lasting more than a few minutes, call 911 or emergency medical services.
Causes
Bradycardia can be caused by:
- Heart tissue damage related to aging
- Damage to heart tissues from heart disease or heart attack
- A heart condition present at birth (congenital heart defect)
- Inflammation of heart tissue (myocarditis)
- A complication of heart surgery
- An underactive thyroid gland (hypothyroidism)
- Imbalance of chemicals in the blood, such as potassium or calcium
- Repeated pauses in breathing during sleep (obstructive sleep apnea)
- Inflammatory disease, such as rheumatic fever or lupus
- Certain medications, including sedatives, opioids, and drugs used to treat heart rhythm disorders, high blood pressure and certain mental health disorders
To better understand the causes of bradycardia, it may be helpful to know how the heart typically beats.
The typical heart has four chambers — two upper chambers (atria) and two lower chambers (ventricles). Within the upper right chamber of the heart (right atrium) is a group of cells called the sinus node. The sinus node is the heart's natural pacemaker. It produces the signal that starts each heartbeat.
Bradycardia occurs when these signals slow down or are blocked.
Sinus node problems
Bradycardia often starts in the area of the heart called the sinus node. In some people, sinus node problems cause alternating slow and fast heart rates (bradycardia-tachycardia syndrome).
Heart block (atrioventricular block)
Bradycardia can also occur if the heart's electrical signals don't move correctly from the upper chambers (atria) to the lower chambers (ventricles). If this occurs, the condition is called heart block, or atrioventricular block.
Heart blocks fall into three main groups.
- First-degree heart block. In the mildest form, all electrical signals from the atria reach the ventricles, but the signal is slowed. First-degree heart block rarely causes symptoms and usually needs no treatment if there's no other problem in electrical signaling.
- Second-degree heart block. Not all electrical signals reach the ventricles. Some beats are dropped, resulting in a slower and sometimes irregular heart rhythm.
- Third-degree (complete) heart block. None of the electrical signals from the atria reaches the ventricles. When this happens, the ventricles will usually beat on their own but at a very slow rate.

In a typical heart rhythm, a tiny cluster of cells at the sinus node sends out an electrical signal. The signal then travels through the atria to the atrioventricular (AV) node and then passes into the ventricles, causing them to contract and pump out blood.
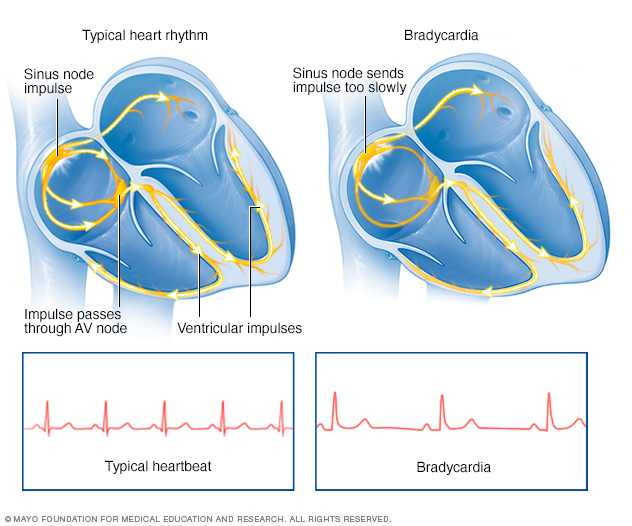
Bradycardia, shown on the right, is a slower than typical heart rhythm that often starts in the area of the heart called the sinus node. A typical heart rhythm is shown in the image on the left.
Risk factors
Bradycardia is often associated with damage to heart tissue from some type of heart disease. Anything that increases the risk of heart problems can increase the risk of bradycardia. Risk factors for heart disease include:
- Older age
- High blood pressure
- Smoking
- Heavy alcohol use
- Illegal drug use
- Stress and anxiety
Healthy-lifestyle changes or medical treatment may help lower the risk of heart disease.
Complications
Possible complications of bradycardia can include:
- Frequent fainting
- Inability of the heart to pump enough blood (heart failure)
- Sudden cardiac arrest or sudden death
Prevention
Bradycardia can be caused by certain medications, particularly if they are taken at high doses, so it's important to take all medications as directed. Although bradycardia is not typically preventable, health care providers recommend strategies to reduce the risk of developing heart disease. Take the following heart-healthy steps:
- Get regular exercise. Your health care provider may give you recommendations about how much and what type of exercise is best for you.
- Eat a healthy diet. Choose a healthy, low-fat, low-salt, low-sugar diet that's rich in fruits, vegetables and whole grains.
- Maintain a healthy weight. Being overweight increases the risk of developing heart disease.
- Keep blood pressure and cholesterol under control. Make lifestyle changes and take medications as prescribed to manage high blood pressure, diabetes and high cholesterol.
- Don't smoke. If you need help quitting, talk to your health care provider about strategies or programs to help.
- If you drink, do so in moderation. If you choose to drink alcohol, do so in moderation. For healthy adults, that means up to one drink a day for women and up to two drinks a day for men. If you can't control your alcohol use, talk to a health care provider about a program to quit drinking and manage other behaviors related to alcohol abuse.
- Manage stress. Intense emotions may affect heart rate. Some ways to relieve stress are getting regular exercise, joining a support group and trying relaxation techniques, such as yoga.
- Go to scheduled checkups. Have regular physical exams and report signs or symptoms to your health care provider.
Monitor and treat existing heart disease
If you already have heart disease, there are steps you can take to lower your risk of developing bradycardia or another heart rhythm disorder:
- Follow the plan. Be sure you understand your treatment plan. Take all medications as prescribed.
- Report changes immediately. If your symptoms change or worsen or you develop new symptoms, tell your health care provider immediately.
Diagnosis
To diagnose bradycardia, a health care provider will usually perform a physical exam and listen to your heart with a stethoscope. He or she may ask you questions about your symptoms and medical history.
Your health care provider may recommend tests to check your heart rate and see if you have a heart problem that can cause bradycardia. Blood tests may be done to check for other conditions that can cause slow heartbeats, such as an infection, an underactive thyroid (hypothyroidism) or an electrolyte imbalance.
Tests
An electrocardiogram (ECG or EKG) is the main test used to diagnose bradycardia. An ECG measures the electrical activity of the heart. Sticky patches (electrodes) are placed on the chest and sometimes the arms and legs. Wires connect the electrodes to a computer, which displays the results. An ECG can show if the heart is beating too slow, too fast or not at all.
Because an ECG can't detect bradycardia unless the slow heartbeat occurs during the test, your health care provider might recommend a portable ECG device. Portable ECG devices include:
- Holter monitor. Carried in a pocket or worn on a belt or shoulder strap, this device records the heart's activity continuously for 24 hours or longer.
- Event recorder. This device is similar to a Holter monitor, but it records only at certain times for a few minutes at a time. It's worn longer than a Holter monitor, typically 30 days. You generally push a button when you feel symptoms. Some devices automatically record when an irregular heart rhythm is detected.
An ECG may be done with other tests to understand how bradycardia affects you. These tests include:
- Tilt table test. This test may help your health care provider better understand how your bradycardia causes fainting spells. As you lie flat on a special table, the table is tilted as if you were standing up. A tilt test is done to see if a change in position causes fainting.
- Stress exercise test. An ECG may be done to monitor your heart's activity while you ride on a stationary bicycle or walk on a treadmill. If you have difficulty exercising, a drug may be given to stimulate the heart in a way that's similar to exercise.
A sleep study may be recommended if your health care provider thinks that repeated pauses in breathing during sleep (obstructive sleep apnea) are causing bradycardia.
Treatment
Treatment for bradycardia depends on the severity of symptoms and the cause of the slow heart rate. If you don't have symptoms, treatment might not be necessary.
Bradycardia treatment may include lifestyle changes, medication changes or an implanted device called a pacemaker. If an underlying health problem, such as thyroid disease or sleep apnea, is causing the slow heart rate, treatment of that condition might correct bradycardia.
Medications
Many medications, including those used to treat other heart conditions, can cause bradycardia. Always let your health care provider know about all the medications you take, including those bought without a prescription.
If a medication you're taking is causing bradycardia, your health care provider may recommend a lower dosage or a different medication.
Surgery or other procedures
When other treatments aren't possible and bradycardia symptoms are severe, a device called a pacemaker is necessary to control the heart rhythm. Pacemakers work only when needed. When the heart beats too slowly, the pacemaker sends electrical signals to the heart to speed up the beat.
Having a pacemaker implanted requires a surgical procedure. One or more wires are inserted into a major vein under or near the collarbone and guided to the heart using X-rays as a guide. One end of each wire is secured at the appropriate area in the heart, while the other end is attached to a device (pulse generator) implanted under the skin beneath the collarbone.
A leadless pacemaker is smaller and typically requires a less invasive surgery to implant the device.
Preparing for an appointment
Whether you start by seeing your primary care provider or get emergency care, you'll likely be referred to a doctor trained in heart conditions (cardiologist) for diagnosis and treatment.
What you can do
If possible, write down the following information and take it with you to your health care provider's appointment:
- Your symptoms, including those that seem unrelated to your heart, and when they began
- Important personal information, including major stresses or recent life changes and your medical history
- Medications, including vitamins and other supplements you take, including doses
- Questions to ask your health care provider
If possible, take along a family member or friend to help you remember the information you receive.
For bradycardia, basic questions to ask your health care provider include:
- What is likely causing my slow heart rate?
- What tests do I need?
- What's the most appropriate treatment?
- What are the possible complications?
- How will my heart be monitored?
- How often will I need follow-up appointments?
- How will other conditions I have or medications I take affect my heart problem?
- Do I need to restrict my activities?
- Are there brochures or other printed material I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your health care provider is likely to ask you questions, such as:
- Have you had fainting spells?
- Does anything, such as exercise, worsen your symptoms?
- Do you smoke?
- Are you being treated for heart disease, high blood pressure, high cholesterol or other conditions that can affect your heart?
Last Updated May 7, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





