Bursitis
Overview
Bursitis (bur-SY-tis) is a painful condition that affects the small, fluid-filled sacs — called bursae (bur-SEE) — that cushion the bones, tendons and muscles near your joints. Bursitis occurs when bursae become inflamed.
The most common locations for bursitis are in the shoulder, elbow and hip. But you can also have bursitis by your knee, heel and the base of your big toe. Bursitis often occurs near joints that perform frequent repetitive motion.
Treatment typically involves resting the affected joint and protecting it from further trauma. In most cases, bursitis pain goes away within a few weeks with proper treatment, but recurrent flare-ups of bursitis are common.
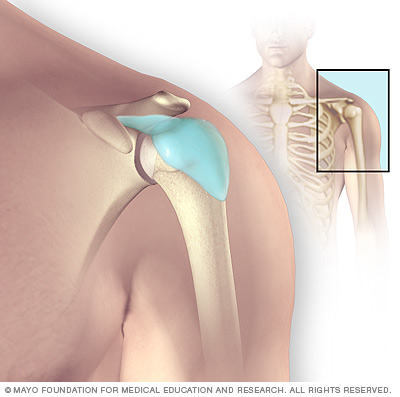
Bursae are small fluid-filled sacs that reduce friction between moving parts in your body's joints. Shoulder bursitis is inflammation or irritation of a bursa (shown in blue) in your shoulder.
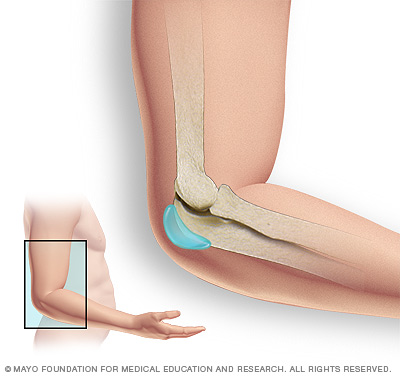
Bursae are small fluid-filled sacs that reduce friction between moving parts in your body's joints. Elbow bursitis is inflammation or irritation of the bursa (shown in blue) in your elbow.
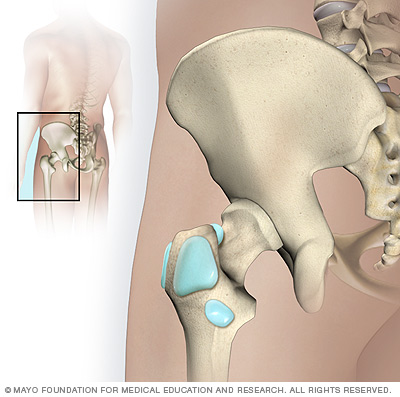
Bursae are small fluid-filled sacs that reduce friction between moving parts in your body's joints. Hip bursitis is inflammation or irritation of one or more of the bursae (shown in blue) in your hip.
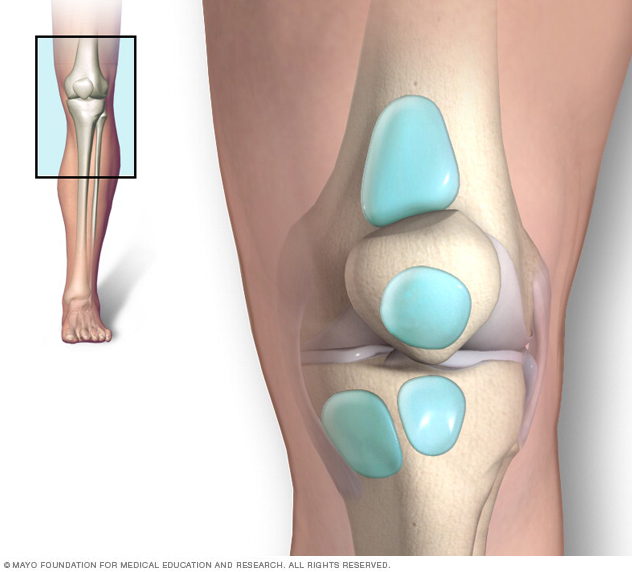
Bursae are small fluid-filled sacs, shown in blue. They lessen friction between moving parts in the body's joints. Knee bursitis is swelling, also called inflammation, of one or more of the bursae in the knee.
Symptoms
If you have bursitis, the affected joint might:
- Feel achy or stiff
- Hurt more when you move it or press on it
- Look swollen and red
When to see a doctor
Consult your doctor if you have:
- Disabling joint pain
- Sudden inability to move a joint
- Excessive swelling, redness, bruising or a rash in the affected area
- Sharp or shooting pain, especially when you exercise or exert yourself
- A fever
Causes
The most common causes of bursitis are repetitive motions or positions that put pressure on the bursae around a joint. Examples include:
- Throwing a baseball or lifting something over your head repeatedly
- Leaning on your elbows for long periods
- Extensive kneeling for tasks such as laying carpet or scrubbing floors
Other causes include injury or trauma to the affected area, inflammatory arthritis such as rheumatoid arthritis, gout and infection.
Risk factors
Anyone can develop bursitis, but certain factors can increase your risk:
- Age. Bursitis becomes more common with aging.
- Occupations or hobbies. If your work or hobby requires repetitive motion or pressure on particular bursae, your risk of developing bursitis increases. Examples include carpet laying, tile setting, gardening, painting and playing a musical instrument.
- Other medical conditions. Certain systemic diseases and conditions — such as rheumatoid arthritis, gout and diabetes — increase your risk of developing bursitis. Being overweight can increase your risk of developing hip and knee bursitis.
Prevention
While not all types of bursitis can be prevented, you can reduce your risk and the severity of flare-ups by changing the way you do certain tasks. Examples include:
- Using kneeling pads. Use some type of padding to reduce the pressure on your knees if your job or hobby requires a lot of kneeling.
- Lifting properly. Bend your knees when you lift. Failing to do so puts extra stress on the bursae in your hips.
- Wheeling heavy loads. Carrying heavy loads puts stress on the bursae in your shoulders. Use a dolly or a wheeled cart instead.
- Taking frequent breaks. Alternate repetitive tasks with rest or other activities.
- Maintaining a healthy weight. Being overweight places more stress on your joints.
- Exercising. Strengthening your muscles can help protect your affected joint.
- Warming up and stretching before strenuous activities to protect your joints from injury.
Diagnosis
Doctors can often diagnose bursitis based on a medical history and physical exam. Testing, if needed, might include:
- Imaging tests. X-ray images can't positively establish the diagnosis of bursitis, but they can help to exclude other causes of your discomfort. Ultrasound or MRI might be used if your bursitis can't easily be diagnosed by a physical exam alone.
- Lab tests. Your doctor might order blood tests or an analysis of fluid from the inflamed bursa to pinpoint the cause of your joint inflammation and pain.
Treatment
Bursitis generally gets better on its own. Conservative measures, such as rest, ice and taking a pain reliever, can relieve discomfort. If conservative measures don't work, you might require:
- Medication. If the inflammation in your bursa is caused by an infection, your doctor might prescribe an antibiotic.
- Therapy. Physical therapy or exercises can strengthen the muscles in the affected area to ease pain and prevent recurrence.
- Injections. A corticosteroid drug injected into the bursa can relieve pain and inflammation in your shoulder or hip. This treatment generally works quickly and, in many cases, one injection is all you need.
- Assistive device. Temporary use of a walking cane or other device will help relieve pressure on the affected area.
- Surgery. Sometimes an inflamed bursa must be surgically drained, but only rarely is surgical removal of the affected bursa necessary.
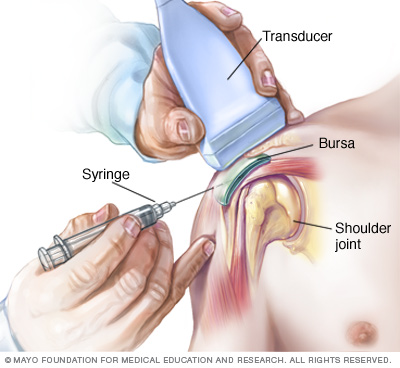
Injection of a corticosteroid medication into your bursa can relieve the pain and inflammation of bursitis. In some cases, your doctor might use ultrasound to guide the injection into the affected bursa. The ultrasound's hand-held transducer provides a live-action display your doctor can view on a monitor during the procedure.
Lifestyle and home remedies
Measures you can take to relieve the pain of bursitis include:
- Rest and don't overuse the affected area.
- Apply ice to reduce swelling for the first 48 hours after symptoms occur.
- Apply dry or moist heat, such as a heating pad or taking a warm bath.
- Take an over-the-counter medication, such as ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve, others), to relieve pain and reduce inflammation. Some are available in a form you apply to the skin.
- Cushion your knees if you sleep on your side by placing a small pillow between your legs.
Preparing for an appointment
You'll likely start by seeing your family doctor, who might refer you to a doctor who specializes in joint disorders (rheumatologist).
What you can do
Make a list that includes:
- Detailed descriptions of your symptoms and when they began
- Information about your medical history and your family's
- All medications and dietary supplements you take, including doses
- Questions to ask the doctor
For bursitis, questions to ask your doctor include:
- What is the most likely cause of my symptoms?
- What are other possible causes?
- What tests will I need?
- What treatment approach do you recommend?
- I have other medical problems. How best can I manage them together?
- Will I need to limit my activities?
- Do you have brochures or other printed material I can take? What websites do you recommend?
What to expect from your doctor
During the physical exam, your doctor will press on various spots around your affected joint to try to determine whether a specific bursa is causing your pain.
Your doctor may also ask you questions, such as:
- Did your pain come on suddenly or gradually?
- What kind of work do you do?
- What are your hobbies or recreational activities?
- Does your pain occur or worsen during certain activities, such as kneeling or climbing stairs?
- Have you recently fallen or had another injury?
- What treatments have you tried?
- What effect did those treatments have?
Last Updated Aug 25, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




