Inflammatory breast cancer
Overview
Inflammatory breast cancer is a form of breast cancer that causes breast swelling and skin changes.
Inflammatory breast cancer happens when a growth of cells forms in the breast tissue. The cells break away from where they started to grow and travel to the lymphatic vessels in the skin. The cells can block the vessels and cause the skin on the breast to look swollen. This skin on the breast might look red or purple.
Inflammatory breast cancer is considered a locally advanced cancer. When a cancer is locally advanced, that means it has spread from where it started to nearby tissue and possibly to nearby lymph nodes.
Inflammatory breast cancer can easily be confused with a breast infection, which is a much more common cause of breast swelling and skin changes. Seek medical attention right away if you notice skin changes on your breast.
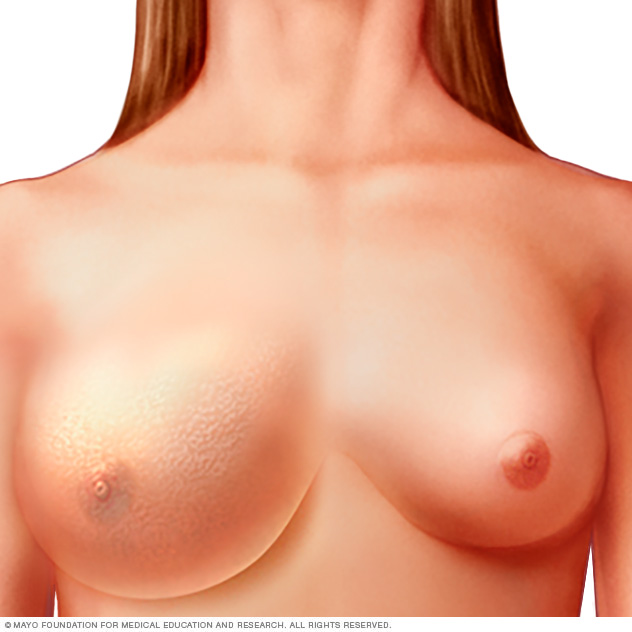
Inflammatory breast cancer often appears as an enlarged breast with thickened skin. The skin may look red, purple or bruised.
Symptoms
Inflammatory breast cancer doesn't commonly form a lump, as occurs with other forms of breast cancer. Instead, signs and symptoms of inflammatory breast cancer include:
- Fast change in the appearance of one breast, over the course of several weeks.
- Thickness, heaviness or swelling of one breast.
- Changes in skin color, giving the breast a red, purple, pink or bruised appearance.
- Unusual warmth of the affected breast.
- Dimpling or ridges on the skin of the affected breast, similar to an orange peel.
- Tenderness, pain or aching.
- Enlarged lymph nodes under the arm, above the collarbone or below the collarbone.
- Flattened nipple or nipple that turns inward on the affected breast.
For inflammatory breast cancer to be diagnosed, these symptoms must have been present for less than six months.
When to see a doctor
Make an appointment with a doctor or other healthcare professional if you have any symptoms that worry you.
Other, more common conditions have symptoms similar to those of inflammatory breast cancer. A breast injury or breast infection, called mastitis, may cause skin color changes, swelling and pain.
Inflammatory breast cancer can easily be confused with a breast infection, which is much more common. It's reasonable and common to first be treated with antibiotics for a week or more. If your symptoms respond to antibiotics, additional testing isn't necessary. But if the condition does not improve, your healthcare professional may consider more-serious causes of your symptoms, such as inflammatory breast cancer.
If you've been treated for a breast infection but your symptoms continue, contact your healthcare professional. You may have a mammogram or other test to evaluate your symptoms. The only way a healthcare professional can know whether your symptoms are caused by inflammatory breast cancer is to remove a sample of tissue for testing.
Causes
Inflammatory breast cancer happens when cells in the breast develop changes in their DNA. A cell's DNA holds the instructions that tell the cell what to do. In healthy cells, the DNA gives instructions to grow and multiply at a set rate. The instructions tell the cells to die at a set time. In cancer cells, the DNA changes give different instructions. The changes tell the cancer cells to make many more cells quickly. Cancer cells can keep living when healthy cells would die. This causes too many cells.
Most often the DNA changes happen in a cell in one of the tubes, called ducts, that can carry breast milk to the nipple. But the cancer also can begin with a cell in the glandular tissue, called lobules, where breast milk can be produced.
In inflammatory breast cancer, the cancer cells break away from where they started. They travel to the lymphatic vessels in the breast skin. The cells grow to clog the vessels. The blockage in the lymphatic vessels causes skin color changes, swelling and dimpled skin. This skin is a classic sign of inflammatory breast cancer.
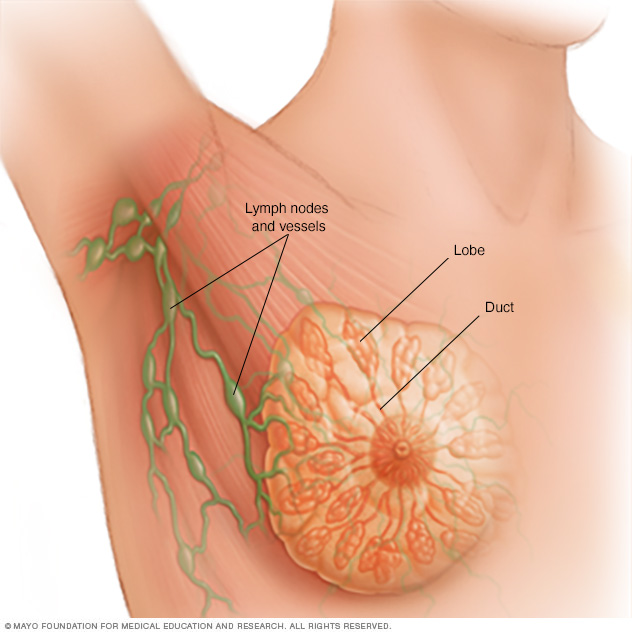
Each breast contains 15 to 20 lobes of glandular tissue, arranged like the petals of a daisy. The lobes are further divided into smaller lobules that produce milk for breastfeeding. Small tubes, called ducts, conduct the milk to a reservoir that lies just beneath the nipple.
Risk factors
Factors that increase the risk of inflammatory breast cancer include:
Being female
Women are much more likely than men to get breast cancer, including inflammatory breast cancer. Everyone is born with some breast tissue, so anyone can get breast cancer.
Being younger
Inflammatory breast cancer is more frequently diagnosed in people in their 40s and 50s.
Being Black
Black people have a higher risk of inflammatory breast cancer than do white people.
Being obese
People who are obese have a greater risk of inflammatory breast cancer.
Prevention
Making changes in your daily life may help lower your risk of breast cancer. Try to:
Ask about breast cancer screening
Talk with your doctor or other healthcare professional about when to begin breast cancer screening. Ask about the benefits and risks of screening. Together, you can decide what breast cancer screening tests are right for you.
Become familiar with your breasts through breast self-exam for breast awareness
You may choose to become familiar with your breasts by occasionally inspecting them during a breast self-exam for breast awareness. If you find a new change, lumps or other unusual signs in your breasts, tell a healthcare professional right away.
Breast awareness can't prevent breast cancer. But it may help you to better understand the look and feel of your breasts. This might make it more likely that you'll notice if something changes.
Drink alcohol in moderation, if at all
If you choose to drink, limit the amount of alcohol you drink to no more than one drink a day. For breast cancer prevention, there is no safe amount of alcohol. So if you're very concerned about your breast cancer risk, you may choose to not drink alcohol.
Exercise most days of the week
Aim for at least 30 minutes of exercise on most days of the week. If you haven't been active lately, ask your healthcare professional whether exercising is OK and start slowly.
Limit hormone therapy during menopause
Combination hormone therapy may increase the risk of breast cancer. Talk with a healthcare professional about the benefits and risks of hormone therapy.
Some people have symptoms during menopause that cause discomfort. These people may decide that the risks of hormone therapy are acceptable to get relief. To reduce the risk of breast cancer, use the lowest dose of hormone therapy possible for the shortest amount of time.
Maintain a healthy weight
If your weight is healthy, work to maintain that weight. If you need to lose weight, ask a healthcare professional about healthy ways to lower your weight. Eat fewer calories and slowly increase the amount you exercise.
Diagnosis
Inflammatory breast cancer is a clinical diagnosis that often starts with a discussion of your health history and an exam of the breast. Other tests include imaging tests and removing some cells for testing.
Tests and procedures used to diagnose inflammatory breast cancer include:
- A physical exam. Your healthcare professional examines your breast to look for changes in skin color, swelling and other signs of inflammatory breast cancer.
- Imaging tests. Imaging tests make pictures of the body. Your healthcare professional may recommend a breast X-ray, called a mammogram, or a breast ultrasound to look for signs of cancer in your breast. Additional imaging tests, such as an MRI, may be recommended in certain situations.
- Removing a sample of tissue for testing. A biopsy is a procedure to remove a sample of tissue for testing in a lab. The tissue might be removed using a needle that is put through the skin and into the suspected cancer cells. A skin biopsy also may be helpful. This type of biopsy removes a sample of skin cells. The sample is tested in a lab to see if it is cancer.
Tests to determine the extent of the cancer
If you're diagnosed with inflammatory breast cancer, you may have other tests to see if the cancer has spread. These tests help your healthcare team find out the extent of your cancer, also called the stage. Cancer staging tests often involve imaging tests. The tests might look for signs of cancer in your lymph nodes or in other parts of your body. Your healthcare team uses the cancer staging test results to help create your treatment plan.
Imaging tests may include MRI, CT, bone scans and a positron emission tomography scan, which also is called a PET scan. Not every test is right for every person. Talk with your healthcare professional about which tests are best for you.
The stages of breast cancer range from 0 to 4. The lower numbers mean the cancer is small and hasn't spread from where it started. As the cancer grows, its stage gets higher. Because inflammatory breast cancer is aggressive and grows quickly, the stages usually range from 3 to 4. By stage 4, the cancer has spread to other areas of the body, such as the organs and bones.
Treatment
Inflammatory breast cancer treatment begins with chemotherapy. If the cancer hasn't spread to other areas of the body, treatment continues with surgery and radiation therapy. If the cancer has spread to other areas of the body, your healthcare team may recommend other medicines in addition to chemotherapy. These treatments can slow the growth of the cancer.
Chemotherapy
Chemotherapy treats cancer with strong medicines. You may receive chemotherapy medicines through a vein, in pill form or both.
Chemotherapy is used before surgery for inflammatory breast cancer. This pre-surgical treatment, called neoadjuvant therapy, aims to shrink the cancer before surgery. Neoadjuvant chemotherapy increases the chance that surgery will be successful.
If your cancer has a high risk of returning or spreading to another part of your body, your healthcare professional may recommend additional chemotherapy after you've completed other treatments. Additional chemotherapy decreases the chance that the cancer will recur.
Surgery
After chemotherapy, you may have a procedure to remove the affected breast and some of the nearby lymph nodes. The operation usually includes:
- Surgery to remove the breast, called mastectomy. A total mastectomy removes all of the breast tissue. This includes the lobules, ducts, fatty tissue and some skin, including the nipple and areola.
- Surgery to remove the nearby lymph nodes, called axillary dissection. The surgeon removes the lymph nodes under the arm and near the affected breast.
Talk with your healthcare team about your options for breast reconstruction. Surgery to reconstruct the breast is often delayed until after you complete all of your breast cancer treatments.
Radiation therapy
Radiation therapy treats cancer with powerful energy beams. The energy can come from X-rays, protons or other sources. During radiation therapy, you lie on a table while a machine moves around you. The machine directs radiation to precise points on your body.
For inflammatory breast cancer, radiation therapy is used after surgery to kill any cancer cells that might remain. The radiation is aimed at your chest, armpit and shoulder.
Targeted therapy
Targeted therapy for cancer is a treatment that uses medicines that attack specific chemicals in the cancer cells. By blocking these chemicals, targeted treatments can cause cancer cells to die.
For example, several targeted therapy medicines focus on a protein that some breast cancer cells make too much of. This protein is called human epidermal growth factor receptor 2, also called HER2. The protein helps breast cancer cells grow and survive. By targeting cells that make too much HER2, the medicines can damage cancer cells while sparing healthy cells.
If your inflammatory breast cancer cells test positive for HER2, your healthcare team might recommend combining targeted therapy with your initial chemotherapy treatment. After surgery, targeted therapy can be combined with hormone therapy.
For cancer that spreads to other parts of the body, targeted therapy medicines that focus on other changes within cancer cells are available. Your cancer cells may be tested to see which targeted therapies might be helpful for you.
Hormone therapy
Hormone therapy is used to treat breast cancers that use the body's hormones to grow. Healthcare professionals refer to these cancers as estrogen receptor positive, also called ER positive, and progesterone receptor positive, also called PR positive.
Hormone therapy can be used after surgery or other treatments to decrease the chance of the cancer returning. If the cancer has already spread, hormone therapy may shrink and control it.
Treatments that can be used in hormone therapy include:
- Medicines that block hormones from attaching to cancer cells, called selective estrogen receptor modulators.
- Medicines that stop the body from making estrogen after menopause, called aromatase inhibitors.
- Surgery or medicines that stop the ovaries from making hormones.
Immunotherapy
Immunotherapy for cancer is a treatment with medicine that helps the body's immune system kill cancer cells. The immune system fights off diseases by attacking germs and other cells that shouldn't be in the body. Cancer cells survive by hiding from the immune system. Immunotherapy helps the immune system cells find and kill the cancer cells.
Immunotherapy might be an option if your cancer has spread to other areas of the body and is triple negative. Triple negative means that the cancer cells don't have receptors for HER2 or the hormones estrogen or progesterone. Your healthcare professional may test your cancer cells to see if they're likely to respond to immunotherapy.
Palliative care
Palliative care is a special type of healthcare that helps people with serious illnesses feel better. If you have cancer, palliative care can help relieve pain and other symptoms. A team of healthcare professionals gives palliative care. This can include doctors, nurses and other specially trained professionals. Their goal is to improve the quality of life for you and your family.
Palliative care specialists work with you, your family and your care team to help you feel better. They provide an extra layer of support while you have cancer treatment. You can have palliative care at the same time as strong cancer treatments, such as surgery, chemotherapy or radiation therapy.
When palliative care is used along with other treatments, people with cancer may feel better and live longer.
Coping and support
Inflammatory breast cancer progresses rapidly. Sometimes this means you need to start treatment before you've had time to think everything through. With time, you'll find what helps you cope with the uncertainty and distress of a cancer diagnosis. Until then, you may find that it helps to:
Learn enough about inflammatory breast cancer to make decisions about your care
Ask your healthcare team about your cancer, including your test results, treatment options and, if you like, your prognosis. As you learn more about inflammatory breast cancer, you may become more confident in making treatment decisions.
Keep friends and family close
Keeping your close relationships strong can help you deal with inflammatory breast cancer. Friends and family can provide the practical support you may need, such as helping take care of your home if you're in the hospital. And they can serve as emotional support when you feel overwhelmed by having cancer.
Find someone to talk with
Find someone who is willing to listen to you talk about your hopes and fears. This may be a friend or family member. The concern and understanding of a counselor, medical social worker, clergy member or cancer support group also may be helpful.
Ask your healthcare team about support groups in your area. Other sources of information include the National Cancer Institute and the American Cancer Society.
Preparing for an appointment
Make an appointment with a doctor or other healthcare professional if you have any symptoms that worry you.
If you're diagnosed with inflammatory breast cancer, you'll be referred to a doctor who specializes in treating cancer, called an oncologist.
Because appointments can be brief, it's a good idea to be prepared. Here's some information to help you get ready.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down symptoms you're experiencing, including any that may not seem related to the reason for which you scheduled the appointment.
- Write down key personal information, including major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements you're taking and the doses.
- Take a family member or friend along. Sometimes it can be very hard to remember all the information provided during an appointment. Someone who goes with you may remember something that you missed or forgot.
- Write down questions to ask your healthcare team.
Your time with your healthcare team is limited, so preparing a list of questions can help you make the most of your time together. List your questions from most important to least important in case time runs out. For inflammatory breast cancer, some basic questions to ask include:
- Do I have inflammatory breast cancer?
- Has my inflammatory breast cancer spread beyond my breast?
- Do I need more tests?
- Can I have a copy of my pathology report?
- What are my treatment options?
- What are the potential risks of each treatment option?
- Can any treatments cure my inflammatory breast cancer?
- Is there one treatment you believe is best for me?
- If you had a friend or family member in my situation, what would you recommend?
- How much time can I take to choose a treatment?
- How will cancer treatment affect my daily life?
- Should I see a specialist? What will that cost, and will my insurance cover it?
- Are there brochures or other printed material that I can take with me? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Be prepared to answer questions, such as:
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Last Updated Mar 12, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





