Mammary duct ectasia
Overview
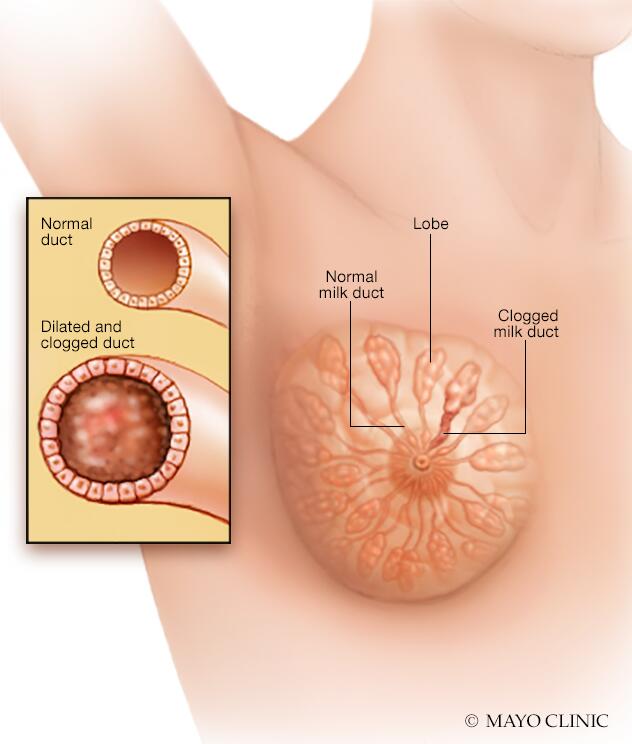
Mammary duct ectasia (ek-TAY-zhuh) occurs when one or more milk ducts beneath your nipple widens. The duct walls may thicken, and the duct may fill with fluid. The milk duct may become blocked or clogged with a thick, sticky substance. The condition often causes no symptoms, but some women may have nipple discharge, breast tenderness or inflammation of the clogged duct (periductal mastitis).
Mammary duct ectasia most often occurs in women during perimenopause — around age 45 to 55 years — but it can happen after menopause, too. The condition often improves without treatment. If symptoms persist, you may need antibiotics or possibly surgery to remove the affected milk duct.
Though it's normal to worry about any changes in your breasts, mammary duct ectasia and periductal mastitis aren't risk factors for breast cancer.
Symptoms
Mammary duct ectasia often doesn't cause any signs or symptoms, but some people experience:
- A dirty white, greenish or black nipple discharge from one or both nipples
- Tenderness in the nipple or surrounding breast tissue (areola)
- Redness of the nipple and areolar tissue
- A breast lump or thickening near the clogged duct
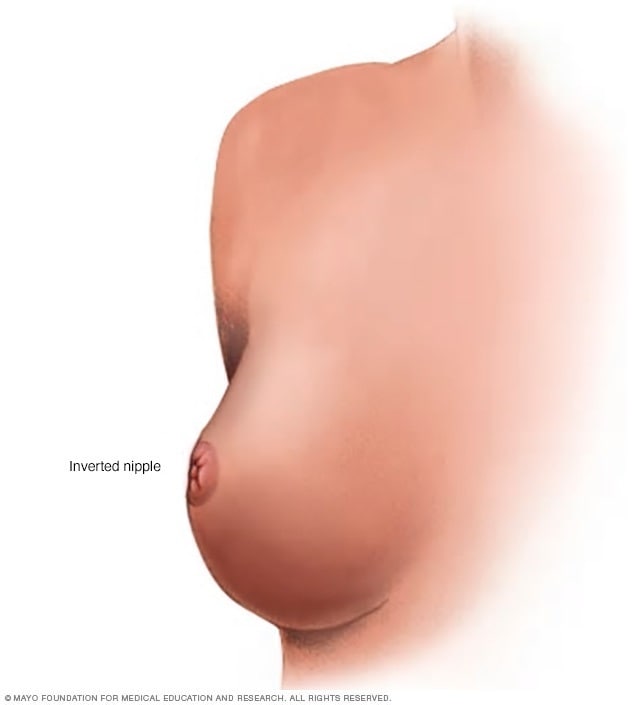
- A nipple that's turned inward (inverted)
A bacterial infection called mastitis also may develop in the affected milk duct, causing breast tenderness, inflammation in the area around the nipple (areola) and fever.
Signs and symptoms of mammary duct ectasia may improve on their own.
When to see a doctor
Make an appointment with your doctor if you notice changes in your breasts — such as a new breast lump, spontaneous nipple discharge, skin redness or inflammation, or an inverted nipple — that are persistent or that worry you.
Causes
Your breasts are made up of connective tissues that include a system of tiny passages that carry milk to the nipples (milk ducts). Mammary duct ectasia occurs when a milk duct beneath the nipple widens. The duct walls may thicken and fill with fluid, becoming blocked or clogged with a sticky substance. Inflammation may result.
Experts don't know exactly what causes mammary duct ectasia. Some speculate the cause to be associated with:
- Breast tissue changes due to aging. As you age, the composition of your breast tissue changes from mostly glandular to mostly fatty in a process called involution. These normal breast changes can sometimes lead to a blocked milk duct and the inflammation associated with mammary duct ectasia.
- Smoking. Cigarette smoking may be associated with widening of milk ducts, which can lead to inflammation and, possibly, mammary duct ectasia.
- Nipple inversion. A newly inverted nipple may obstruct milk ducts, causing inflammation and infection. A nipple that's newly inverted could also be a sign of a more serious underlying condition, such as cancer.
Complications
Complications of mammary duct ectasia are usually minor and often more bothersome than serious. These may include:
- Nipple discharge. Nipple discharge caused by mammary duct ectasia can be frustrating. Fluid leaking from your nipples can cause embarrassing wetness and staining on your clothes.
- Breast discomfort. Mammary duct ectasia can cause redness, swelling and tenderness around your nipples.
- Infection. An inflammatory infection (periductal mastitis) may develop in the affected milk duct, sometimes causing pain in or around the nipple, a general feeling of illness or a fever. Persistent redness and worsening pain could be a sign of a bacterial infection and can lead to an abscess — a collection of pus in your breast tissue — which may require a procedure to drain it.
- Concern about breast cancer. When you notice a change in your breast, you may worry that it's a sign of breast cancer, especially if you develop a hard lump around the nipple or areola. Having a history of mammary duct ectasia doesn't increase your risk of breast cancer. Still, it's important to see your doctor promptly anytime you notice breast changes.
Diagnosis
Based on information you provide to your doctor and the results of a physical exam, you might need additional tests, including:
- Diagnostic ultrasound of the nipple and areola. An ultrasound uses sound waves to make images of breast tissue. It allows your doctor to evaluate the milk ducts beneath your nipple. A diagnostic ultrasound lets your doctor focus on an area of suspicion.
- Diagnostic mammography. Mammography provides X-ray images of your breast and can help your doctor evaluate your breast tissue. A diagnostic mammogram provides more-detailed views of a specific area of your breast than a screening mammogram does.
Treatment
Mammary duct ectasia doesn't always require treatment. If your symptoms are bothersome, however, treatment options may include:
- Antibiotics. Your doctor may prescribe an antibiotic for 10 to 14 days to treat an infection caused by mammary duct ectasia. Even if your symptoms greatly improve or disappear completely after starting the antibiotic, it's important to take all your medication as prescribed.
- Pain medication. You could try a mild pain reliever, such as acetaminophen (Tylenol, others) or ibuprofen (Advil, Motrin IB, others), as needed for breast discomfort. Follow your doctor's recommendation on which pain reliever is best for you.
- Surgery. If an abscess has developed and antibiotics and self-care don't work, the affected milk duct may be surgically removed. This procedure is done through a tiny incision at the edge of the colored tissue around your nipple (areola). Surgery rarely is needed for mammary duct ectasia.
Self care
To relieve discomfort associated with mammary duct ectasia, you might try these self-care measures:
- Apply warm compresses. A warm compress applied to your nipple and surrounding area may soothe painful breast tissue.
- Use breast pads for nipple discharge. Using breast pads or nursing pads can keep fluid from leaking through your clothing. These pads are available at drugstores and many retail stores that sell baby care products.
- Wear a support bra. Choose bras with good support to minimize breast discomfort. A well-fitting bra can also help keep a breast pad in place to absorb nipple discharge.
- Sleep on the opposite side. Avoid sleeping on the same side of your body as your affected breast to help prevent swelling and further discomfort.
- Stop smoking. Smoking may make it harder to treat an infection, and ongoing smoking may result in recurrent infections or an abscess.
Preparing for your appointment
For evaluation of a new breast lump or changes in your breast, you're likely to start by seeing your primary care doctor. In some cases, based on a clinical breast exam or findings on the mammogram or ultrasound, you may be referred to a breast health specialist.
What you can do
The initial evaluation focuses on your medical history and the signs and symptoms you're experiencing, including how they're related to your menstrual cycle. To prepare for this discussion with your doctor:
- Take note of all your symptoms, even if they seem unrelated to the reason for which you scheduled the appointment.
- Review key personal information, including major stresses or recent life changes.
- Make a list of all medications, vitamins and supplements that you regularly take.
- Write down questions to ask your doctor, to make sure you remember everything you want to ask.
For mammary duct ectasia, here are some questions you might ask your doctor:
- What's causing my symptoms?
- Will this condition resolve itself, or will I need treatment?
- What treatment approach do you recommend?
- Is there an over-the-counter medication I can take for pain relief?
- What self-care measures can I try?
- Do you have printed information I can take home with me? What websites do you recommend?
What to expect from your doctor
Your doctor may ask you a number of questions, such as:
- How long have you experienced symptoms?
- Have your symptoms changed over time?
- Do you experience breast pain? How severe?
- Do you have nipple discharge? How would you describe the color, consistency and amount?
- Do your symptoms occur in one or both breasts?
- Have you had a fever?
- When was your last mammogram?
- Have you ever been diagnosed with a precancerous breast condition?
- Have you ever had a breast biopsy or been diagnosed with a benign breast condition?
- Has your mother, a sister or anyone else in your family had breast cancer?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Last Updated Jun 18, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



