Moyamoya disease
Overview
Moyamoya disease is a rare blood vessel disorder in which the carotid artery in the skull becomes blocked or narrowed. The carotid artery is a major artery that brings blood to the brain. When it's blocked, blood flow to the brain is reduced. Tiny blood vessels then develop at the base of the brain in an attempt to supply the brain with blood.
The condition may cause a ministroke, known as a transient ischemic attack, or a stroke. It also can cause bleeding in the brain. Moyamoya disease can affect how well the brain functions and can cause cognitive and developmental delays or disability.
Moyamoya disease most commonly affects children. However, adults may have the condition as well. Moyamoya disease is found all over the world. But it's more common in East Asian countries, especially Korea, Japan and China. This may be due to certain genetic factors in those populations.

In moyamoya disease, arteries to your brain become narrow and may even close, leading to reduced delivery of oxygen-rich blood to your brain. This lack of blood flow to the brain can cause a stroke and other symptoms.
Symptoms
Moyamoya disease may occur at any age. But symptoms are most common in children between ages 5 and 10 and in adults between ages 30 and 50. Spotting symptoms early is very important to prevent complications such as a stroke.
Moyamoya disease causes different symptoms in adults and children. In children, the first symptom is usually a stroke or recurrent transient ischemic attack (TIA). Adults may experience these symptoms, as well. But adults also may experience bleeding in the brain, known as a hemorrhagic stroke. The bleeding occurs because of the way blood vessels in the brain formed.
Symptoms of moyamoya disease related to reduced blood flow to the brain include:
- Headache.
- Seizures.
- Weakness, numbness or paralysis in your face, arm or leg. This is typically on one side of your body.
- Vision problems.
- Trouble speaking or understanding others, known as aphasia.
- Cognitive or developmental delays.
- Involuntary movements.
These symptoms can be triggered by exercise, crying, coughing, straining or a fever.
When to see a doctor
Seek immediate medical attention if you notice any symptoms of a stroke or ministroke, even if they seem to come and go or disappear.
Think "FAST" and do the following:
- Face. Ask the person to smile. Does one side of the face droop?
- Arms. Ask the person to raise both arms. Does one arm drift downward? Or is one arm unable to rise up?
- Speech. Ask the person to repeat a simple phrase. Is the person's speech slurred or strange?
- Time. If you observe any of these signs, call 911 or emergency medical help immediately.
Call 911 or your local emergency number right away. Don't wait to see if symptoms go away. Every minute counts. The longer a stroke goes untreated, the greater the potential for brain damage and disability.
If you're with someone you suspect is having a stroke, watch the person carefully while waiting for emergency assistance.
See your health care provider if you have any of the symptoms of moyamoya disease. Early detection and treatment can help prevent a stroke and serious complications.
Causes
The exact cause of moyamoya disease is unknown. Moyamoya disease is most commonly seen in Japan, Korea and China. But it also occurs in other parts of the world. Researchers believe the greater prevalence in these Asian countries strongly suggests a genetic factor in some populations.
Sometimes changes to the blood vessels, known as vascular changes, can occur that mimic moyamoya disease. These changes may have different causes and symptoms. This is known as moyamoya syndrome.
Moyamoya syndrome is also associated with certain conditions, such as Down syndrome, sickle cell anemia, neurofibromatosis type 1 and hyperthyroidism.
Risk factors
Though the cause of moyamoya disease is unknown, certain factors may increase your risk of having the condition. They include:
- Asian heritage. Although moyamoya disease is found all over the world, it's more common in East Asian countries, especially Korea, Japan and China. This may be due to certain genetic factors in those populations. This same higher prevalence has been documented among Asians living in Western countries.
- Family history of moyamoya disease. If you have a family member with moyamoya disease, your risk of having the condition is 30 to 40 times higher than that of the general population. This strongly suggests a genetic component.
- Medical conditions. Moyamoya syndrome sometimes occurs in association with other disorders, including neurofibromatosis type 1, sickle cell disease and Down syndrome, among many others.
- Being female. Females have a slightly higher incidence of moyamoya disease.
- Being young. Though adults can have moyamoya disease, children younger than 15 years old are most commonly affected.
Complications
Most complications from moyamoya disease are associated with the effects of strokes. They include seizures, paralysis and vision problems. Other complications include speech problems, movement disorders and developmental delays. Moyamoya disease can cause serious and permanent damage to the brain.
Diagnosis
Moyamoya disease is usually diagnosed by a neurologist who specializes in the condition. The specialist will review your symptoms and your family and medical history. The specialist also will likely perform a physical exam. Several tests are generally needed to diagnose moyamoya disease and any underlying conditions.
Tests may include:
-
Magnetic resonance imaging (MRI). An MRI uses powerful magnets and radio waves to create detailed images of the brain. A health care provider may inject a dye into a blood vessel to view your arteries and veins and highlight blood circulation. This type of test is called a magnetic resonance angiogram.
Your neurologist may recommend a perfusion MRI if available. This type of imaging can measure the amount of blood passing through the vessels. It can show the extent of reduction of blood supply to the brain.
- Computerized tomography (CT) scan. A CT scan uses a series of X-rays to create a detailed image of your brain. A health care provider may inject a dye into a blood vessel to highlight blood flow in your arteries and veins. This is called a (CT angiogram). This test can't diagnose early stages of moyamoya disease. But it may be helpful in identifying problems with blood vessels.
- Cerebral angiogram. In a cerebral angiogram, a health care provider inserts a long, thin tube called a catheter into a blood vessel in your groin. The provider then guides it to your brain using X-ray imaging. The provider injects dye through the catheter into the blood vessels of your brain. The contrast conforms to the shape of the blood vessels to make them more visible under X-ray imaging.
- Positron emission tomography (PET) scan or single-photon emission computerized tomography (SPECT). In these tests, you're injected with a small amount of a safe radioactive material. PET provides visual images of brain activity. SPECT measures blood flow to regions of the brain.
- Electroencephalogram (EEG). An EEG monitors the electrical activity in your brain using small metal discs called electrodes attached to your scalp. Children with moyamoya disease often have EEG results that aren't typical.
- Transcranial Doppler ultrasound. In surgical transcranial Doppler ultrasound, sound waves are used to obtain images of your head and sometimes your neck. Specialists may use this test to evaluate blood flow in blood vessels in your neck.
If necessary, your neurologist may order other tests to rule out other conditions.
Treatment
Health care providers evaluate your condition and determine the most appropriate treatment. Treatment doesn't cure moyamoya disease. But treatment can be effective in preventing strokes.
The goal of treatment is to reduce your symptoms and improve brain blood flow. Treatment also aims to lower your risk of complications. Complications include ischemic stroke caused by a lack of blood flow, bleeding in your brain and death.
The prognosis for moyamoya disease depends on several factors, including:
- How early the disease was diagnosed.
- How much damage has occurred when you seek treatment.
- Whether or not you undergo treatment.
- Age.
Your treatment may include:
Medication
Medicines may be prescribed to manage symptoms, to reduce the risk of a stroke or to aid in seizure control. They include:
- Blood thinners. Blood thinners are typically recommended if you've been diagnosed with moyamoya disease and you have mild or no symptoms. Your health care provider may recommend that you take aspirin or another blood thinner to prevent strokes.
- Calcium channel blockers. Also known as calcium antagonists, this type of medicine may help manage headaches. They also may help reduce symptoms related to transient ischemic attacks. These drugs can help manage blood pressure, which is essential in people with moyamoya disease to prevent blood vessel damage.
- Anti-seizure medicines. These medicines could be helpful for those who have had seizures.
Moyamoya surgery types
Early surgical treatment can help slow progression of moyamoya disease. Your neurologist may recommend revascularization surgery if you develop symptoms or strokes. Surgery also may be recommended if tests show evidence of low blood flow to your brain.
In revascularization surgery, surgeons bypass blocked arteries. They do this by connecting blood vessels on the outside and inside of the skull to help restore blood flow to your brain. This may include direct or indirect revascularization procedures. Or it may include a combination of both.
-
Direct revascularization procedures. In direct revascularization surgery, surgeons stitch the scalp artery directly to a brain artery. This is also known as superficial temporal artery to middle cerebral artery bypass surgery. This procedure increases blood flow to your brain immediately.
Direct bypass surgery may be difficult to perform in children due to the size of the blood vessels to be attached. But it's the preferred option in adults. This intervention can be performed safely and effectively by an experienced surgical team that treat moyamoya patients on a daily basis.
-
Indirect revascularization procedures. In indirect revascularization, the goal is to lay over the brain surface blood-rich tissues to increase blood flow to your brain gradually over time. In high-volume surgical centers, indirect revascularization is almost always combined with direct revascularization in adult patients.
Types of indirect revascularization procedures include encephaloduroarteriosynangiosis (EDAS) or encephalomyosynangiosis (EMS), or a combination of both.
In EDAS, a surgeon separates a scalp artery over several inches.
The surgeon makes a small temporary opening on the skin to expose the artery. Then the surgeon makes an opening in your skull directly beneath the artery. The surgeon lays the intact scalp artery to the surface of your brain, which allows blood vessels from the artery to grow into your brain over time. The surgeon then replaces the bone and closes the opening in your skull.
In EMS, your surgeon separates a muscle in the temple region of your forehead and places it onto the surface of your brain through an opening in your skull. This helps restore blood flow.
Your surgeon may perform EMS with EDAS. In this procedure, your surgeon separates a muscle in the temple region of your forehead. The surgeon places it onto the surface of your brain after attaching the scalp artery to the surface of your brain. The muscle helps to hold the artery in place as blood vessels grow into your brain over time.
Possible surgery risks of revascularization procedures for moyamoya disease include changes in pressure in the blood vessels in the brain. This can cause symptoms such as headaches, bleeding and seizures. However, the benefits of surgery largely outweigh the risks.
Some people with moyamoya disease develop a bulge or ballooning of a blood vessel in the brain known as a brain aneurysm. If this occurs, surgery may be necessary to prevent or treat a ruptured brain aneurysm.
Therapy
To address the physical and mental effects of a stroke on you or your child, your health care provider may recommend an evaluation by a psychiatrist or therapist. Without surgery, moyamoya disease can cause cognitive decline due to narrowing blood vessels. A psychiatrist may look for signs of problems with thinking and reasoning skills. The psychiatrist also may monitor you or your child for signs that those problems are worsening.
Cognitive behavioral therapy can help address emotional issues related to having moyamoya disease, such as how to cope with fears and uncertainties about future strokes.
Physical and occupational therapy can help regain any lost physical function caused by a stroke.
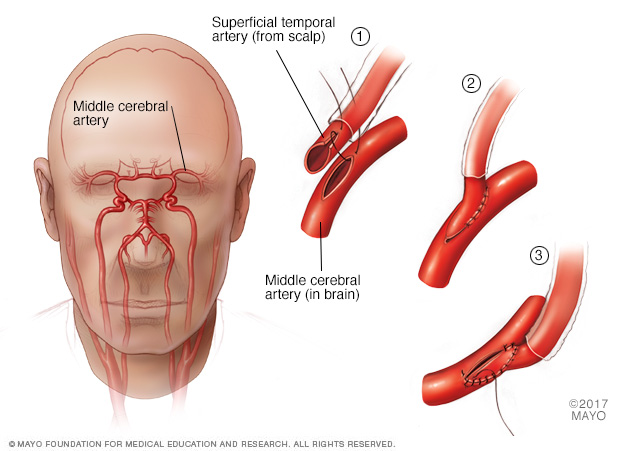
In a direct revascularization procedure, your surgeon connects a scalp artery, known as a superficial temporal artery, directly to the middle brain artery, known as a middle cerebral artery. This increases blood flow to the brain.
Preparing for an appointment
If you or your child has been diagnosed with moyamoya disease, you'll most likely be referred to a doctor who specializes in brain conditions, known as a neurologist.
What you can do
- Write down any symptoms you or your child has experienced. Include any that may seem unrelated to the reason you scheduled the appointment.
- Make a list of all medicines. Include vitamins and supplements you or your child is taking, along with the dosages. Write down the reasons any medicines were discontinued, whether because of side effects or lack of effectiveness.
- Ask a family member to come with you to the appointment. Sometimes it can be difficult to remember all the information provided during an appointment. Someone who goes with you may remember something you missed or forgot.
- Write down questions. Preparing a list of questions for your health care provider will help you make the most of your time together.
Some basic questions to ask include:
- What is likely causing my or my child's symptoms or condition?
- What kinds of tests are necessary? Do they require any special preparation?
- What treatments are available, and which do you recommend?
- What side effects can be expected from treatment?
- Is surgery a possibility?
- Are you prescribing medicine? If so, is there a generic alternative?
- My child has other medical problems. How can they be managed together?
- Will I or my child have any restrictions on physical activity?
- Are there brochures or other printed materials that I can take with me? What websites do you recommend?
- What makes a center of excellency for treatment of moyamoya patients?
What to expect from your doctor
Your health care provider is likely to ask you or your child a number of questions, such as:
- When did symptoms first occur?
- How often do the symptoms occur?
- Do certain activities trigger symptoms?
- Has anyone in your immediate family ever had moyamoya disease?
Last Updated Apr 18, 2023
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





