Myocarditis
Overview
Myocarditis is inflammation of the heart muscle, called the myocardium. The condition can reduce the heart's ability to pump blood. Myocarditis can cause chest pain, shortness of breath, and rapid or irregular heartbeats.
Infection with a virus is one cause of myocarditis. Sometimes myocarditis is caused by a medicine reaction or a condition that causes inflammation throughout the body.
Severe myocarditis weakens the heart so that the rest of the body doesn't get enough blood. Clots can form in the heart, leading to a stroke or heart attack.
Treatment for myocarditis may include medicines, procedures or surgeries.
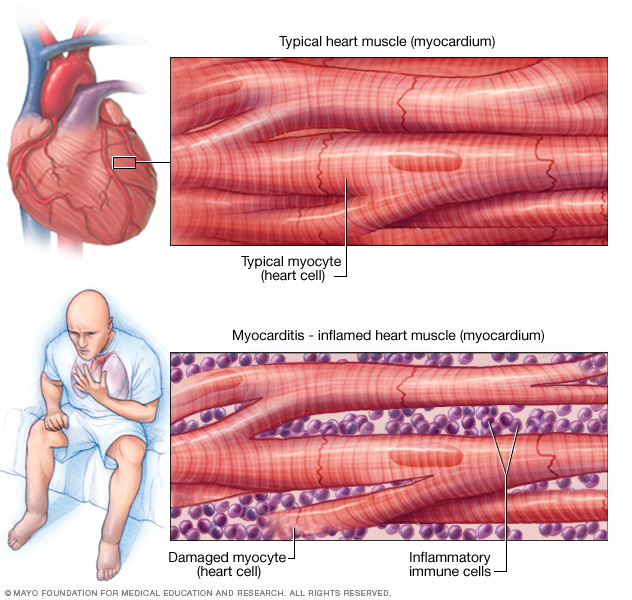
Myocarditis is inflammation of the heart muscle. This illustration shows typical heart muscle compared with damaged heart muscle due to inflammation.
Symptoms
Some people with early myocarditis don't have symptoms. Others have mild symptoms.
Common myocarditis symptoms include:
- Chest pain.
- Fatigue.
- Swelling of the legs, ankles and feet.
- Rapid or irregular heartbeats, called arrhythmias.
- Shortness of breath, at rest or during activity.
- Lightheadedness or feeling like you might faint.
- Flu-like symptoms such as headache, body aches, joint pain, fever or sore throat.
Sometimes, myocarditis symptoms are like symptoms of a heart attack. If you are having unexplained chest pain and shortness of breath, seek emergency medical help.
Myocarditis in children
When children get myocarditis, symptoms may include:
- Difficulty breathing.
- Rapid breathing.
- Chest pain.
- Rapid or irregular heartbeats, called arrhythmias.
- Fainting.
- Fever.
When to see a doctor
Contact a healthcare professional if you have symptoms of myocarditis. Symptoms of myocarditis can seem like a heart attack. Get emergency medical help if you have unexplained chest pain, rapid heartbeats or shortness of breath.
If you have severe symptoms, go to the emergency room or call for emergency medical help.
Causes
Infections can cause myocarditis.
-
Viruses. Many viruses have been linked to myocarditis, including the adenovirus, which causes the common cold; the COVID-19 virus; viruses that cause hepatitis B and C; parvovirus, which causes a mild rash, usually in children; and herpes simplex virus.
Gastrointestinal infections due to echoviruses, Epstein-Barr virus, which causes mononucleosis, and German measles, also called rubella, all can cause myocarditis. Myocarditis also can be caused by HIV, the virus that causes AIDS.
- Bacteria. Bacteria that can cause myocarditis include staphylococcus, streptococcus, and bacteria that cause diphtheria and Lyme disease.
- Parasites. Parasites that can cause myocarditis are Trypanosoma cruzi and toxoplasma. Some parasites are transmitted by insects and can cause a condition called Chagas disease. Chagas disease is much more common in Central and South America than in the United States.
- Fungi. A fungal infection may cause myocarditis, particularly in people with weakened immune systems. Fungal infections linked to myocarditis include yeast infections, such as candida; molds, such as aspergillus; and histoplasma, often found in bird droppings.
Myocarditis also may be caused by:
- Certain medicines or illegal drugs. These include medicines used to treat cancer; antibiotics, such as penicillin and sulfonamide drugs; some anti-seizure medicines; and cocaine. When these cause myocarditis, it's called drug-induced myocarditis.
- Chemicals or radiation. Exposure to carbon monoxide and radiation can sometimes cause myocarditis.
- Other health conditions. Conditions that may cause myocarditis include lupus, Wegener's granulomatosis, giant cell arteritis and Takayasu's arteritis.
Often, the cause of myocarditis isn't found.
Complications
Usually, myocarditis goes away without complications. However, severe myocarditis can permanently damage the heart muscle.
Possible complications of myocarditis may include:
- Heart failure. Untreated, myocarditis can damage the heart muscle so that it can't pump blood well. People with myocarditis-related heart failure may need a ventricular assist device or a heart transplant.
- Heart attack or stroke. If the heart muscle is damaged and can't pump blood, the blood that collects in the heart can form clots. A heart attack can occur if a clot blocks one of the heart arteries. A stroke can happen if a blood clot in the heart travels to an artery leading to the brain.
- Rapid or irregular heartbeats, called arrhythmias. Damage to the heart muscle can change how the heart beats. Certain arrhythmias increase the risk of stroke.
- Sudden cardiac death. Certain serious irregular heartbeats can cause the heart to suddenly stop beating, a condition called sudden cardiac arrest. If it leads to death it's called sudden cardiac death.
Prevention
There's no specific prevention for myocarditis. However, taking these steps to prevent infections might help:
- Stay away from people who are sick. Stay away from people with symptoms of the flu or other respiratory illness until they are better. If you're sick with symptoms of a viral infection, try to avoid passing the germs to others.
- Wash your hands regularly. Frequent hand-washing is one of the best ways to not get sick and spread germs.
- Avoid risky behaviors. To reduce the chances of getting an HIV-related myocardial infection, practice safe sex and don't use illegal drugs.
- Get recommended vaccines. Stay up to date on recommended vaccines, including those that protect against COVID-19, influenza and rubella — diseases that can cause myocarditis. Rarely, the COVID-19 vaccine can cause myocarditis and inflammation of the outer heart lining, called pericarditis, particularly in males ages 12 to 29. Talk with your healthcare team about the benefits and risks of vaccines.
Diagnosis
Early diagnosis of myocarditis is important to preventing long-term heart damage. To diagnose myocarditis, a healthcare professional examines you and listens to your heart with a stethoscope.
Blood and imaging tests may be done to check your heart health. Imaging tests can help confirm myocarditis and determine its severity.
Tests
Tests to diagnose myocarditis include:
- Blood tests. Blood tests are usually done to check for a heart attack, inflammation and infection. A cardiac enzyme test can check for proteins related to heart muscle damage. Antibody blood tests may help learn if you had an infection linked to myocarditis.
- Electrocardiogram (ECG or EKG). This quick and painless test shows how the heart is beating. Your healthcare professional can look for signal patterns on an ECG to learn if you have irregular heartbeats.
- Chest X-ray. A chest X-ray shows the size and shape of the heart and lungs. A chest X-ray can tell if there's fluid in or around the heart that might be related to heart failure.
- Heart MRI, also called a cardiac MRI. This test uses magnetic fields and radio waves to create detailed images of the heart. A cardiac MRI shows the heart's size, shape and structure. It can help diagnose myocarditis.
- Echocardiogram. Sound waves create moving images of the beating heart. An echocardiogram can show the heart's size and how well blood flows through the heart and heart valves. An echocardiogram can see if there's fluid around the heart.
- Cardiac catheterization and heart muscle biopsy. A doctor places a thin, flexible tube called a catheter into a blood vessel in the arm or groin. It's guided to an artery in the heart. Dye flows through the catheter to help the heart arteries show up more clearly on X-rays. A tiny sample of heart muscle tissue may be taken during this test. This is called a biopsy. The sample is sent to a lab to be checked for signs of myocarditis or an infection.
Treatment
Often, myocarditis gets better on its own or with treatment. Myocarditis treatment focuses on the cause and the symptoms, such as heart failure.
Myocarditis treatment may include:
- Medicine.
- Medical devices.
- Surgery.
Medications
People with mild myocarditis may only need rest and medicine. If myocarditis is severe, medicines may be given through an IV at a hospital to quickly improve the heart's ability to pump blood.
Medicine to treat myocarditis may include:
- Corticosteroids. These medicines may be used to treat some rare types of viral myocarditis, such as giant cell and eosinophilic myocarditis.
- Medicines to prevent blood clots. If myocarditis is causing severe heart failure or irregular heartbeats, medicine may be given to reduce the risk of blood clots in the heart.
- Heart medicines. Medicines may be used to remove extra fluid from the body and reduce the strain on the heart. Some types of medicines that may be used to treat myocarditis symptoms are diuretics, beta blockers, angiotensin-converting enzyme (ACE) inhibitors or angiotensin 2 receptor blockers (ARBs).
- Medicines to treat chronic conditions. Sometimes another health condition, such as lupus, causes myocarditis. Treating this underlying condition may help reduce heart muscle inflammation.
Some people with myocarditis take medicines for just a few months and then get better completely. Others may have long-term heart damage that needs lifelong medicine. It's important to have regular health checkups after myocarditis to check for possible complications.
Therapies
A treatment called extracorporeal membrane oxygenation (ECMO) may be used to help the heart to recover or while waiting for other treatments, such as a heart transplant.
An ECMO machine works like the lungs. It removes carbon dioxide and adds oxygen to the blood. If you have severe heart failure, this device can send oxygen to your body. During ECMO, blood is removed from the body through tubes, passed through the machine and then returned to the body.
Surgeries and procedures
Severe myocarditis needs aggressive treatment. Treatment may include:
- Ventricular assist device (VAD). A VAD helps pump blood from the lower chambers of the heart to the rest of the body. It's a treatment for a weakened heart or heart failure. Open-heart surgery is usually needed to place the device in the body. The device may be used to help the heart work while waiting for other treatments, such as a heart transplant.
- Intra-aortic balloon pump (IABP). This device helps increase blood flow and reduce the strain on the heart. It's placed in the body's main artery, called the aorta. A doctor inserts a thin tube called a catheter into a blood vessel in the leg and guides it to the aorta. A balloon attached to the end of the catheter inflates and deflates as the heart beats and relaxes.
- Heart transplant. An urgent heart transplant may be needed for those who have very severe myocarditis.
Lifestyle and home remedies
Rest and reducing the strain on the heart are important parts of myocarditis recovery.
If you have or had myocarditis, ask your healthcare professional which type and amount of physical activity is safe for you. If you have myocarditis, you should avoid competitive sports for at least 3 to 6 months.
Preparing for an appointment
If you have symptoms of myocarditis, make an appointment for a health checkup. If symptoms are severe, you may first be seen in an emergency setting. You usually are sent to a doctor trained in heart diseases, called a cardiologist. You also may see a doctor trained in infectious disease.
What you can do
Here's some information to help you get ready for your appointment. Write down the following details:
- Your symptoms, including any that might seem unrelated to myocarditis, and when they began.
- Important personal information, including recent illnesses and any symptoms, recent travel locations, and your and your family's medical history.
- All medicines, vitamins and supplements you take. Include those bought without a prescription. Also include the doses.
- Questions to ask your healthcare team.
For myocarditis, basic questions to ask your healthcare team include:
- What's the most likely cause of my symptoms?
- What are other possible causes?
- What tests do I need?
- How is myocarditis treated?
- What side effects can I expect from treatment?
- Are there alternatives to the primary treatment that you're suggesting?
- I have other health conditions. How can I best manage these conditions together?
- Do I need to change my activities or diet?
- Are there brochures or other printed material I can have? What websites do you recommend?
Don't hesitate to ask other questions. Take a family member or friend along to your appointment, if possible, to help you remember the information you receive.
What to expect from your doctor
Your healthcare team is likely to ask many questions, including:
- Have you recently been sick or have you recovered from another illness?
- Have you recently traveled out of the country?
- What, if anything, makes symptoms better?
- What, if anything, makes your symptoms worse?
Last Updated Jun 4, 2024
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use




