Sick sinus syndrome
Overview
Sick sinus syndrome is a type of heart rhythm disorder. It affects the heart's natural pacemaker (sinus node), which controls the heartbeat. Sick sinus syndrome causes slow heartbeats, pauses (long periods between heartbeats) or irregular heartbeats (arrhythmias).
Sick sinus syndrome is relatively uncommon. The risk of developing it increases with age. Many people with sick sinus syndrome eventually need an implanted device called a pacemaker to keep the heart in a regular rhythm.
Sick sinus syndrome may also be called sinus node dysfunction or sinus node disease.
Symptoms
Most people with sick sinus syndrome have few or no symptoms. Symptoms may be mild or come and go — making them difficult to recognize at first.
Signs and symptoms of sick sinus syndrome may include:
- A sensation of rapid, fluttering heartbeats (palpitations)
- Chest pain or discomfort
- Confusion
- Dizziness or lightheadedness
- Fainting or near fainting
- Fatigue
- Shortness of breath
- Slower pulse (bradycardia)
When to see a doctor
Talk to your health care provider if you have any signs or symptoms of sick sinus syndrome. Many medical conditions can cause these problems. It's important to get a timely and accurate diagnosis.
If you have new or unexplained chest pain or think you're having a heart attack, call for emergency medical help immediately.
Causes
To understand the cause of sick sinus syndrome, it may be helpful to know how the heart typically beats.
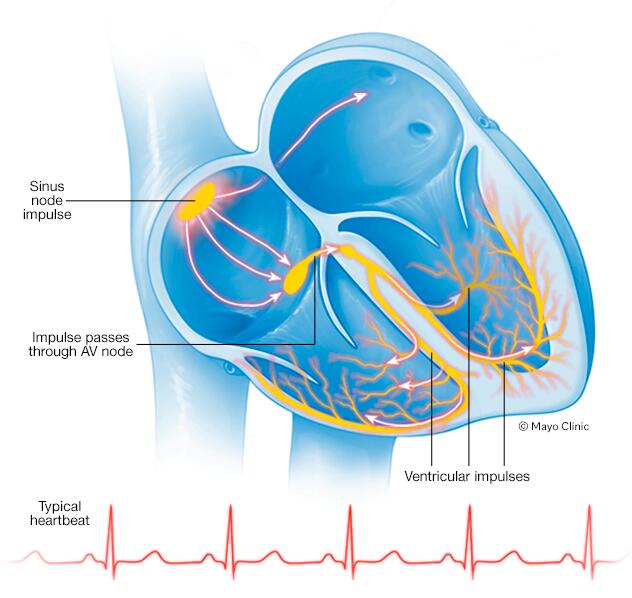
The heart is made up of four chambers — two upper (atria) and two lower (ventricles). The rhythm of the heart is typically controlled by the sinus node, an area of specialized cells in the right upper heart chamber (right atrium).
This natural pacemaker produces electrical signals that trigger each heartbeat. From the sinus node, electrical signals travel across the atria to the ventricles, causing them to contract and pump blood to the lungs and body.
Typically, the sinus node creates a steady pace of electrical impulses. The pace changes depending on activity, emotions and other factors.
In sick sinus syndrome, the electrical signals are irregularly paced. The heartbeat can be too fast, too slow, interrupted by long pauses — or an alternating combination of these rhythm issues. Sick sinus syndrome is relatively uncommon, but the risk of developing it increases with age.
Causes of sick sinus node syndrome can include:
- Age-related wear and tear of heart tissues
- Damage to the sinus node or scarring from heart surgery
- Heart disease
- Inflammatory diseases affecting the heart
- Medications to treat high blood pressure, including calcium channel blockers and beta blockers
- Medications to treat irregular heartbeats (arrhythmias)
- Some Alzheimer's disease medications
- Neuromuscular diseases, such as muscular dystrophy
- Obstructive sleep apnea
- Rare genetic changes
Features of sick sinus syndrome include:
- Sinus bradycardia. The sinus node produces a slow heartbeat.
- Sinus arrest. Signals from the sinus node pause, causing skipped beats.
- Sinoatrial exit block. Signals to the upper heart chambers are slowed or blocked, causing pauses or skipped beats.
- Chronotropic incompetence. The heart rate is within regular range at rest but doesn't increase as much as it should with physical activity.
- Tachycardia-bradycardia syndrome. The heart rate alternates between unusually slow and fast rhythms, often with a long pause between heartbeats.
Risk factors
Sick sinus syndrome can occur at any age. It's most common in people in their 70s or older. Common heart disease risk factors might increase the risk of sick sinus syndrome. Risk factors for heart disease include:
- High blood pressure
- High cholesterol
- Excess body weight
- Lack of exercise
Complications
Complications of sick sinus syndrome include:
- Atrial fibrillation, a type of irregular heartbeat (arrhythmia)
- Heart failure
- Stroke
- Cardiac arrest
Diagnosis
To diagnose sick sinus syndrome, a health care provider performs a physical exam and asks about symptoms and medical history.
Symptoms of sick sinus syndrome — such as dizziness, shortness of breath and fainting — only occur when the heart is beating irregularly. You may not have symptoms at the time of the appointment.
To determine whether symptoms are related to problems with the sinus node and heart function, a health care provider may use the following tests:
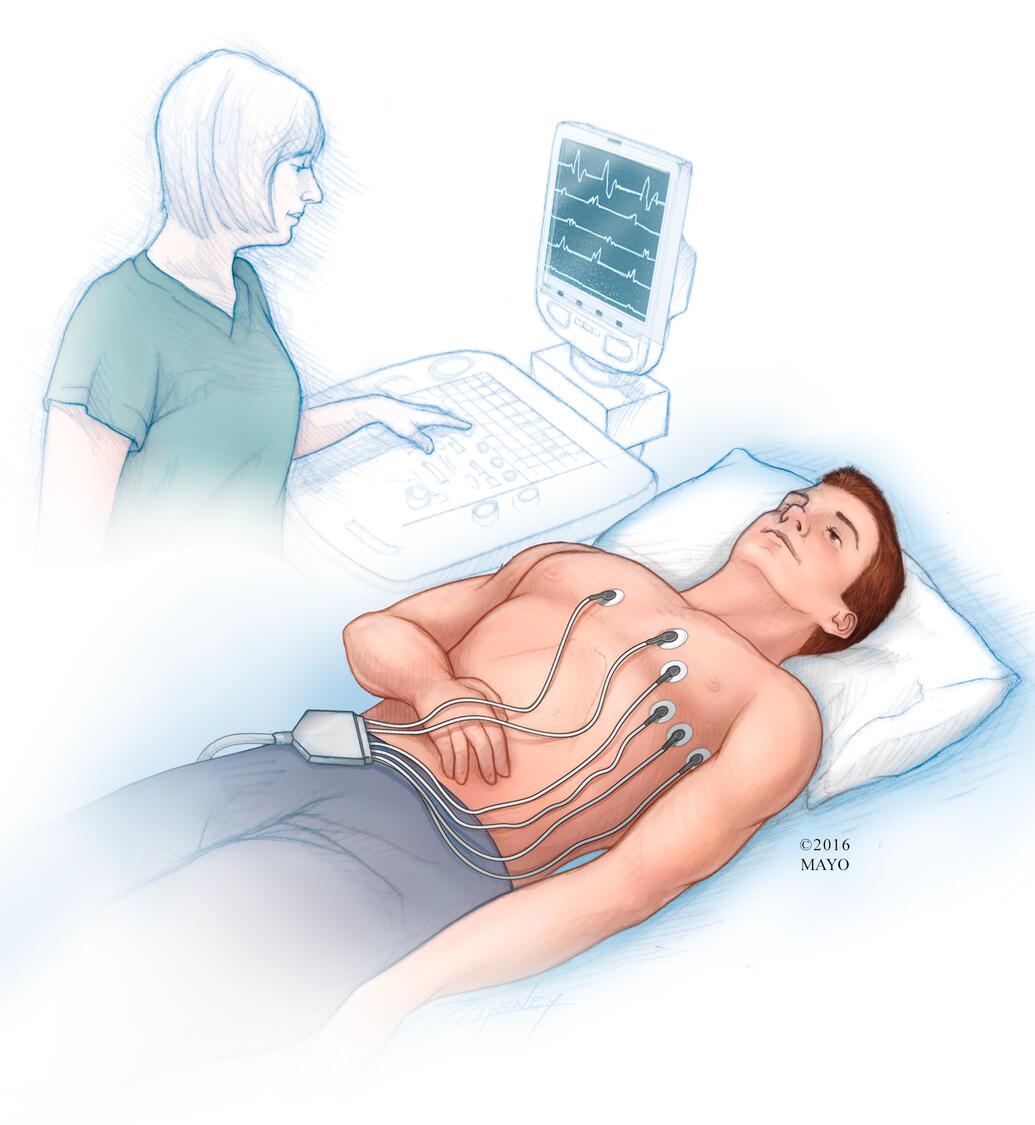
- Electrocardiogram (ECG or EKG). This simple test measures the electrical activity of the heart. Sensors (electrodes) are attached to the chest and legs. Wires attach the sensors to a computer, which displays or prints results. An ECG can tell how fast or slow the heart is beating. A health care provider can look for signal patterns to determine if sick sinus syndrome is present.
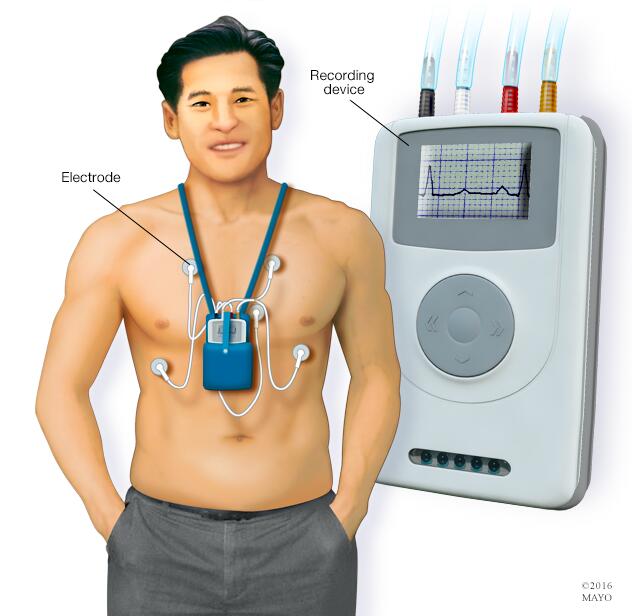
- Holter monitor. This portable ECG device can be worn for a day or more during daily activities. It automatically records the heart's activity for 24 to 72 hours. A person wearing a monitor might also keep a diary of symptoms.
- Event recorder. This portable ECG device is intended to be worn for up to 30 days or until you have an irregular heartbeat or symptoms. You typically press a button when symptoms occur.
- Other monitors. Some personal devices, such as smart watches, offer electrocardiogram monitoring. Ask your health care provider if this is an option for you.
- Implantable loop recorder. This small ECG device is implanted just under the skin of the chest. It's used for continuous, long-term monitoring of the heart's electrical activity, particularly for people who have infrequent symptoms.
Electrophysiologic (EP) testing
This test, also called an EP study, is rarely used to screen for sick sinus syndrome. However, it may be done to check the function of the sinus node and to evaluate other electrical properties of the heart.
During an EP study, thin, flexible wires tipped with electrodes are threaded through blood vessels to different areas within the heart. Once in place, the electrodes can map the spread of electrical signals through the heart.
Treatment
The goals of sick sinus treatment are to reduce or eliminate symptoms and to manage any other contributing health conditions.
Treatment of sick sinus syndrome may include:
- Regular checkups
- Medications
- Catheter procedures
- Surgery to implant a device to maintain a regular heartbeat (pacemaker)
If you don't have symptoms, your health care provider may simply recommend regular health checkups to monitor your condition. Most people with symptoms need to have a procedure to implant a device to maintain a regular heartbeat (pacemaker).
Medications
Some medications, including those used to treat high blood pressure or heart disease, may interfere with sinus node function. Your health care provider will likely review the medications you take and may adjust them or prescribe different ones.
Medications may be needed to prevent or to slow down fast heartbeats.
Blood-thinners (anticoagulants), such as warfarin (Jantoven), dabigatran (Pradaxa) or others, may be prescribed if sick sinus syndrome is associated with atrial fibrillation or other irregular heart rhythms linked to stroke.
Surgeries or other procedures
Most people with sick sinus syndrome eventually need a permanent device to control the heart rhythm (pacemaker). A pacemaker is a small, battery-powered device that's implanted under the skin near the collarbone during a minor surgical procedure. The pacemaker stimulates (paces) the heart as needed to keep it beating regularly.
If sick sinus syndrome symptoms are mild or infrequent, the decision to use a pacemaker will depend on the results of electrocardiograms (ECGs), your overall health and the risk of more-serious problems.
The type of pacemaker you need depends on the type of irregular heart rhythm you have. Types of pacemakers include:
- Single chamber pacemaker. This type usually carries electrical signals to the right lower heart chamber (ventricle) of the heart.
- Dual chamber pacemaker. This type paces the right lower heart chamber (ventricle) and the right upper heart chamber (atrium) separately. Most people with sick sinus syndrome benefit from dual-chamber pacemakers.
- Biventricular pacemaker. Biventricular pacing, also called cardiac resynchronization therapy, is for people who have heart failure and heartbeat problems. This type of pacemaker stimulates both lower heart chambers (the right and left ventricles) to make the heart beat more efficiently.
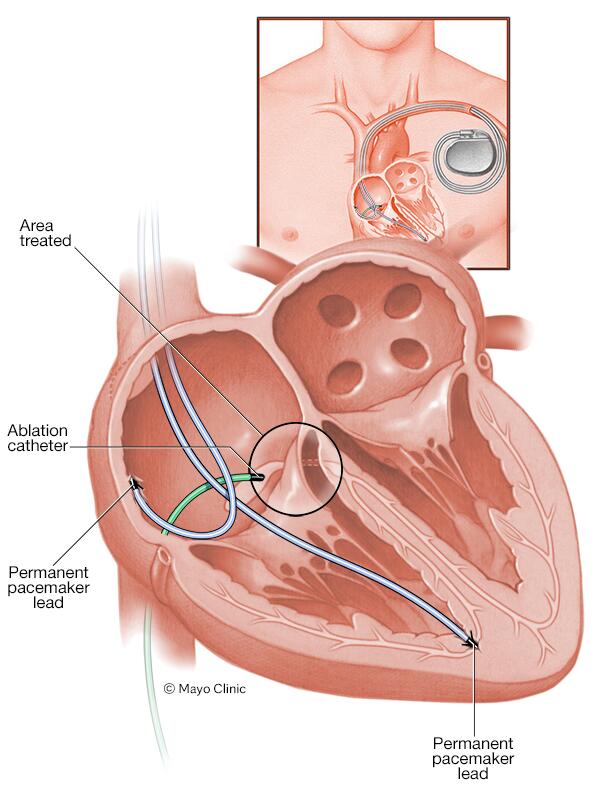
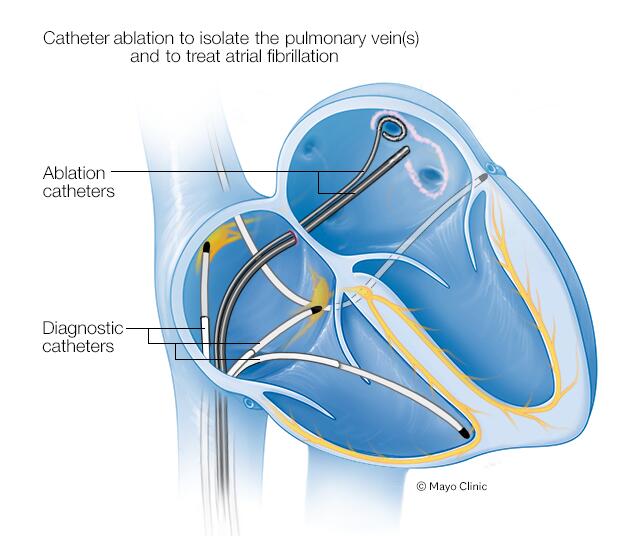
If your heart rate is still irregular after getting a pacemaker, you may need medications or a catheter-based procedure called cardiac ablation to correct or control it. Cardiac ablation uses heat or cold energy to create tiny scars in the heart to block faulty signals and restore a regular heartbeat. It's most often done using thin, flexible tubes called catheters inserted through the veins or arteries. Less commonly, ablation is performed during cardiac surgery. A type of cardiac ablation called AV node ablation is often used to control fast heart rhythms in people with pacemakers.
Self care
It's important to take steps to lower the risk of heart disease. Try these heart-healthy strategies:
- Eat a healthy diet. Choose generous portions of nonstarchy vegetables, fruits and whole grains and modest portions of fish, lean meats, poultry and dairy.
- Exercise and maintain a healthy weight. Being overweight increases the risk of developing heart disease. Unless your provider tells you otherwise, aim for at least 30 minutes of moderate physical activity every day. Ask your health care provider what your goal weight should be.
- Keep blood pressure and cholesterol under control. Make lifestyle changes and take medications as prescribed to manage high blood pressure or high cholesterol.
- Don't smoke. If you smoke and can't quit on your own, talk to your health care provider about ways or programs to help break a smoking habit.
- If you drink, do so in moderation. For some conditions it's recommended that you completely avoid alcohol. Ask your health care provider for advice specific to your condition. If you can't control your alcohol use, talk to your provider about a program to quit drinking and manage other behaviors related to alcohol use.
- Don't use illegal drugs. Talk to your provider about a program if you need help quitting.
- Control stress. Getting more exercise, practicing mindfulness and connecting with others in support groups are some ways to reduce stress.
- Go to scheduled checkups. Have regular physical exams and report any signs or symptoms to your health care provider.
Preparing for your appointment
Call your health care provider if you have symptoms of sick sinus syndrome. You might be referred to a doctor trained in diagnosing and treating heart conditions (cardiologist).
Be prepared to answer questions about your medical history and symptoms. Write down your answers to help you remember details.
Questions your provider may ask about symptoms include:
- Do your symptoms include feeling lightheaded or dizzy?
- Have you ever fainted?
- Do you have rapid, fluttering or pounding heartbeats?
- Do you feel pressure, heaviness, tightness or pain in your chest?
- Does exercise or activity worsen your symptoms?
- Does anything improve your symptoms?
- How often have you had symptoms?
- How long have the symptoms lasted?
Other questions may include the following:
- Have you been diagnosed with high blood pressure, high cholesterol, diabetes or a heart condition?
- What medications do you take and what dosage? Who is the prescribing doctor?
- Why were the prescription drugs prescribed?
- Have you been taking the medication as prescribed?
- Have you recently stopped, started or changed medications?
- What over-the-counter medications, herbal remedies or supplements do you take?
Write down any questions you have for your provider. You might bring a friend or relative to write down information during the appointment.
What you can do in the meantime
If exercise makes your symptoms worse, avoid exercise until you see your provider.
Last Updated Apr 30, 2022
© 2024 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use





